Impact of stigma and stigma-focused interventions on screening and treatment outcomes in cancer patients
Elizabeth O Akin-Odanye1 and Anisah J Husman2
1Department of Clinical Psychology, University College Hospital, Queen Elizabeth Road, Oritamefa, Ibadan, Oyo State, 200212, Nigeria
2College of Health Professions and Sciences, University of Central Florida, 4000 Central Florida Blvd, Orlando, FL 32816, USA
Abstract
Background: Stigma is known to negatively influence cancer patients’ psychosocial behaviour and treatment outcomes. The aim of this study was to systematically review the current data on cancer-related stigma across different populations and identify effective interventions used to address it.
Methodology: The protocol, search, appraisal, synthesis, analysis and reporting framework was used for conducting this systematic literature review. CINAHL, PubMed, PsycINFO and Google Scholar databases were searched using the different combination of keywords that include ‘cancer stigma’. Articles publication period was set for 2010–2020. A total of 54 articles (31 quantitative, 19 qualitative, 2 mixed methods and 2 scoping reviews) that met inclusion criteria were reviewed out of the 958 articles initially identified. Quality assessment of included studies revealed the studies had varying levels of methodological quality. Extracted data were organised and narratively analysed.
Results: Cancer stigma was expressed across different segments of the society including amongst the elites and healthcare providers. Developing countries had higher rates of stigma reported and experience of stigma varied by cancer type. Cancer was consistently associated with imminent death in all studies reviewed. Cancer patients experiencing stigma were more inclined to conceal their diagnosis and to seek medical help later. Whilst cancer stigma majorly resulted in negative psychosocial outcomes in patients, there were also instances of posttraumatic growth emanating from the stigma experienced. Literature on cancer-related stigma interventions was scant.
Conclusion: Cancer related stigma remains high in both clinical settings and amongst the general public. There is need for more interventions to combat cancer stigma and its effect in both patient and non-patient population. Anti-cancer public enlightenment campaigns should be sensitively designed to not further fuel stigma against patients with certain types of cancers.
Keywords: cancer, stigma, systematic review
Correspondence to: Elizabeth O Akin-Odanye
Email: toyin_akinodanye@yahoo.co.uk
Published: 25/10/2021
Received: 19/12/2020
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background
Stigma is a discrediting characteristic that reduces a person ‘from a whole and usual person to a tainted, discounted one’ [25]. ‘It is a process whereby the societal reaction to a person or his condition negatively alters the individual's normal identity’ and devalues him in the eyes of others [39, 53]. Health-related stigma refers to stigmatisation of an illness, which can be applied to an
individual or a group of people with the illness, as well as to the illness more generally [61]. Illness stigmatisation is not stable, but is influenced by social attitudes that differ across cultures and change over time [16]. Most of the literature exploring health-related stigma has focused on a small group of illnesses: cancer, disabilities, leprosy, epilepsy, HIV/AIDS, tuberculosis and mental illness [1, 14, 76].
Cancer-related stigma has especially drawn attention to the detrimental burden of social views on the lives of patients [4, 7, 17, 83]. Patients sometimes feel avoided by others once they have received a cancer diagnosis [33] and fear of stigmatisation can be a barrier to disclosure of a cancer diagnosis [70]. Cancer stigma studies and reviews have tended to focus on single cancer types such as lung cancer [9] or specific aspects of cancer patients lives that could be affected by cancer such as work. Few studies have explored cancer stigma across multiple settings although such studies could inform a better understanding of how cancer stigma differ across different populations well as aid in the development of more targeted interventions to combat cancer stigma and its effect on health outcomes.
So far, it is not very clear how stigma is experienced by patients with different types of cancer, how it affects screening and health seeking behaviour and outcomes as well as available interventions to help cancer patients cope with perceived and internalised cancer. Hence, this systematic review was conducted to help inform the current state of stigma, its impact and interventions across multiple cancer types and geographical spread.
Methodology
Protocol: This systematic literature review (SLR) was done using the protocol, search, appraisal, synthesis, analysis and reporting framework [89]. The review scope was defined using the framework of Population, Intervention, Comparison, Outcome and Context (PICOC). The SLR sought to address the following research questions:
1. How is cancer stigma expressed and experienced?
2. How does cancer stigma affect cancer screening and health seeking behaviour?
3. What is the impact of stigma on cancer patients’ psychosocial and health outcomes?
4. How efficacious are available cancer stigma-focused interventions?
Search
The keywords ‘cancer stigma’, ‘cancer stigma interventions’, ‘cancer stigma impact’, ‘cancer stigma effect’, ‘stigma and cancer screening’, ‘Cancer stigma and health seeking behavior’ were used in searching for relevant articles written in English language and restricted to the past 10 years from PubMed, PsycINFO, CINAHL and Google Scholar. The relevant studies were identified based on pre-specified inclusion and exclusion criteria.
Inclusion criteria
Studies with the under listed features will be included in the systematic review
1. Studies describing the experience or expression of cancer stigma in both patient and non-patient population.
2. Studies reporting effect of stigma on cancer screening and health seeking behaviour.
3. Studies reporting impact of cancer stigma on psychosocial, behavioural and treatment outcomes in cancer patients.
4. Studies reporting cancer stigma-focused interventions and their effectiveness.
5. Studies must have been published between 2010 and 2020 and must be written in English.
6. The title of study must include the words ‘cancer’ and ‘stigma’.
Exclusion criteria
Studies with the under listed features will be excluded from the systematic review
1. Studies not reflecting both ‘cancer’ and ‘stigma’.
2. Studies reflecting both ‘cancer’ and ‘stigma’ in their titles but whose contents reveal that were not primarily focused on cancer stigma.
3. Studies reflecting the words ‘cancer’ and ‘stigma’ in their titles that were only focused on validation of instruments used for assessing stigma.
Appraisal
In this phase, all selected papers were screened for relevance based on the objectives set out for this review work. All papers that met the earlier stated inclusion criteria were selected for further content assessments. Papers that were opinion papers without clear methodology and extended abstracts were removed. The flow diagram on Figure 1 shows the screening process for papers selected. Of the 959 peer reviewed studies originally gathered, 54 (5.63%) met the inclusion criteria and were included in this review.
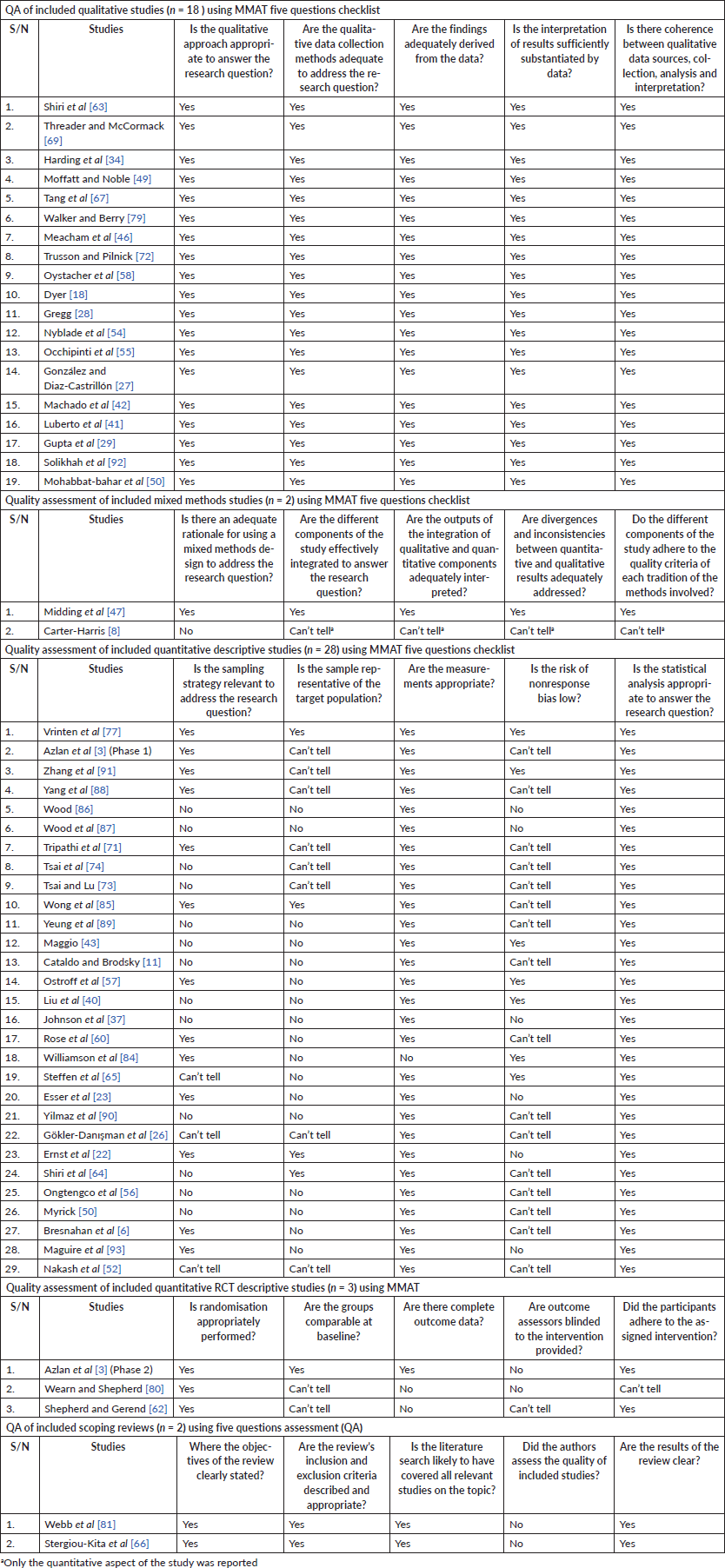
Quality assessment of the selected studies was conducted using the mixed methods appraisal tool (MMAT) version 2018 [36] for all non-systematic review studies. Each scoping literature review in this study was assessed using five quality assessment (QA) questions (see Table 1). All assessment questions were responded to using the options: Yes, Can’t tell or No. Each of the included qualitative study had a ‘Yes’ response to all the assessment questions, indicating they are of high quality. Amongst the quantitative studies, only 1 study had a ‘Yes’ response to all the assessment questions, whilst 16 studies had between three and four ‘Yes’ responses to all the assessment questions. Out of the two mixed methods study, one had all ‘Yes’ responses whilst the other had no ‘Yes’ response because only the quantitative aspect of the study was reported. The scoping reviews had four ‘Yes’ responses each. All studies were included in the review irrespective of adjudged quality (Details in Supplementary Data, Table S1).
Synthesis
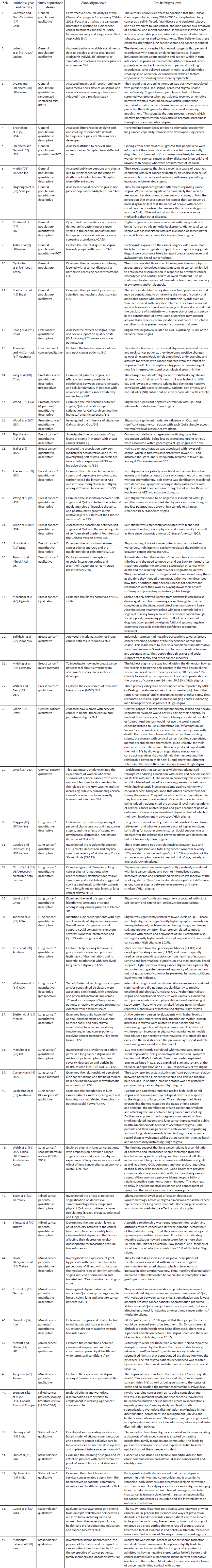
To address the objectives of conducting the SLR, the relevant information from the articles such as names of authors, years of publication, country, study population, method of analysis (quantitative, qualitative, mixed or systematic review), aims, stigma scales and results were extracted into an excel spreadsheet for data processing. The extracted information is presented in Table 2.
Out of the 54 studies reviewed, 19 were conducted in North America (USA – 18 and Mexico – 1), 3 in Africa (South Africa – 1, Uganda – 1 and Senegal – 1), 15 in Asia (India – 4, Taiwan – 1, Israel – 1, Indonesia – 1, Iran – 3, Turkey – 2 and China – 3), 9 in Europe (UK – 6 and Germany – 3), 3 in South America (Chile – 1 and Brazil – 2), 3 in Australia and 2 scoping reviews with multiple countries (see Figure 2). Furthermore, 31 (57.41%) studies used quantitative methods of data analysis, 19 (35.19%) were qualitative, 2 (3.70%) mixed methods studies and 2 (3.70%) scoping reviews (see Figure 3). Lung cancer stigma (LCS) in patients was the focus of 12 of the included studies, 11 of the studies were on stigma in breast cancer patients, 11 on cancer stigma perceptions of the general public, 8 on cancer stigma in a mixed cancer population, 5 on cancer stigma perceptions of stakeholders (cancer patients, families and healthcare providers), stigma in prostate cancer patients was the focus of 3 studies, 2 studies were on cervical cancer stigma whilst 1 each was on oral and head and neck cancer (see Figure 4).
The scales used for assessing stigma in the included studies were Cancer Stigma Scale (CASS) by Marlow and Wardle [45], Social Impact Scale (SIS) by Fife and Wright [24], Body Image After Breast Cancer Questionnaire (BIABCQ) by Baxter et al [5], Self-Stigma Scale-Short Form (SSS) adapted for breast cancer survivors (BCS) by Mak and Cheung [43], Lung Cancer Stigma Scale (LuCaSS) by Maggio [43], the Lung Cancer Stigma Inventory (LCSI) by Hamann et al [31], Cataldo Lung Cancer Stigma Scale (CLCSS) by Cataldo et al [10], six-item stigma scale by Phelan et al [59], Turkish version of the ‘questionnaire for measuring attitudes toward cancer (cancer stigma) – patient version’, by Cho et al [13], discrimination and stigma scale (Adapted from Thornicroft et al [68]), German version of the Social Impact Scale (SIS-D) by Eichhorn et al [20], Cancer Stigma Index (CSI) by Edelen et al [19] and some studies used items adapted from different scales.
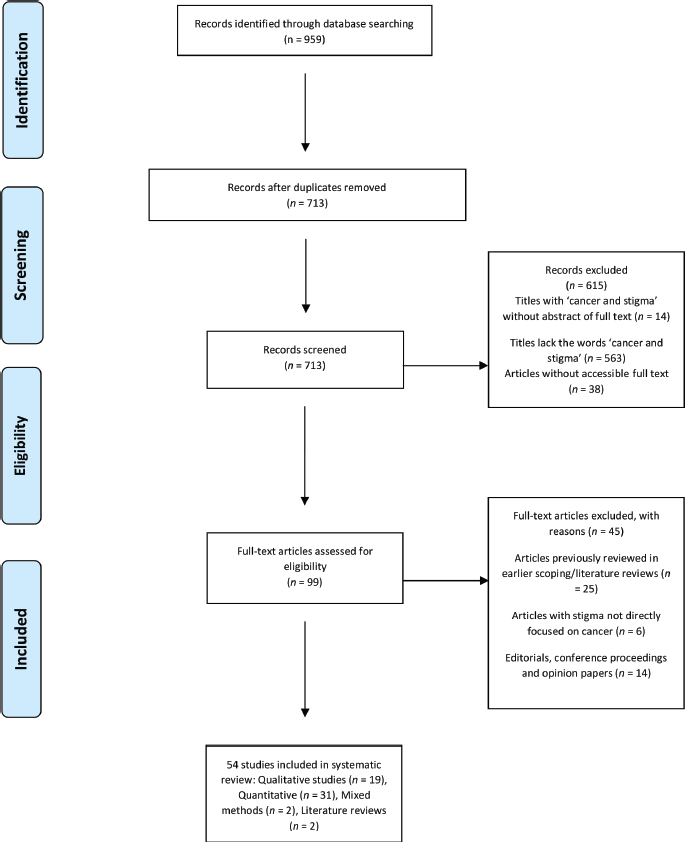
Figure 1. The Preferred Reporting Items for Systematic reviews and Meta-Analyses flowchart of studies included in the review.
Table 1: Scope of SLR using the PICOC framework to the determined objectives.
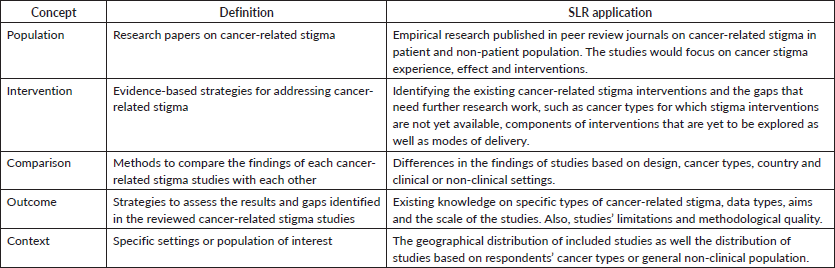
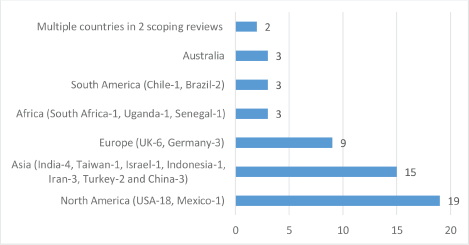
Figure 2.Number of included studies by continent.
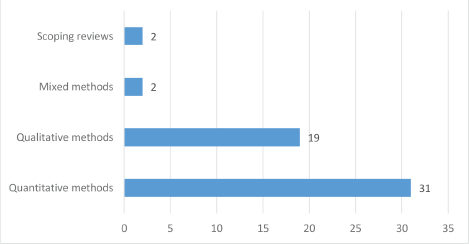
Figure 3. Methods used by included studies.
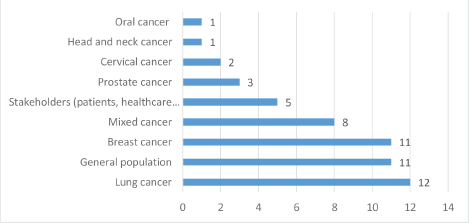
Figure 4. Number of included studies by studied population or cancer types.
Table 2. Characteristics of included studies.
Analysis
Expression and experience of cancer stigma
• Ubiquitous nature of cancer stigma
The prevalence of high cancer stigma in the studies reviewed range from 26.1% amongst a sample of patients with different types of cancer in Iran Shiri et al [64] to 35.5% amongst lung cancer patients in the USA [37]. The included articles showed that the stigma attached to cancer and cancer patients is expressed and experienced from different segments of the society, such as the general public [6, 54, 56, 58, 62, 63, 72], elites [50], media and advertising agencies [18, 27, 55, 80], healthcare providers [28, 34]), policy makers [49] and friends and family members [63, 101].
Cancer stigma and anticipated discrimination often began from being labelled based on physical appearance of perceived signs of cancer [58]. Furthermore, the cost of cancer treatment paired with poor prognosis led to a stigma of draining family resources and being shamed by in-laws for bringing cancer into the family [29, 46]. Stigma induced acts of social and physical isolation include ceasing to invite persons with cancer to social events, physical separation of their personal effects or sleeping quarters, neglect by spouse or family and friends, verbal stigma ranging from gossip to outright abuse were copiously described in some studies [92, 54, 72]. However, narratives of family support also emerged alongside the presence of prevalent and harmful stigma in some studies [29, 46, 54, 92].
• Stigma and type of cancer
Women with breast cancer described the burden of being expected to be positive despite the continued association of cancer with death and how they sometimes had to downplay their private suffering to present a positive front to others [72]. Amongst these women, being less educated and opting for breast conservation surgery [71], being on chemotherapy, having depressive symptoms with high levels of ambivalence over emotional expression and intrusive thoughts [74] were significantly associated with higher self-stigma. Furthermore, there was significant inverse relationship between annual household income [74] and time since diagnosis 100] with self-stigma in patients with breast cancer. Patients with breast and prostate cancers appeared less stigmatised [18, 22, 55, 86, 87]. Respondents in some of the studies opined that the public regards breast cancer as a ‘blameless’ disease [18] that people get ‘pink, warm, and fuzzy’ about [55]. Nevertheless, like with breast cancer patients, time since diagnosis was found to be inversely correlated with prostate cancer patients’ stigma score in a prospective study [88].
The experience of cancer stigma related to shame and blame appeared highest amongst patients with lung and cervical cancers due to their links with smoking [55, 81] and STIs [18, 62], respectively. Studies reported significantly higher levels of stigma in lung cancer patients with younger age, depression, greater social deprivation/constraints, unemployment, higher negative changes following diagnosis, higher cancer stage, perceived blame from others, concealment of cancer diagnosis, lower coping self-efficacy, poor self-esteem and being an ever smoker [93, 40, 43, 57, 81, 84]. However, findings on the relationship between smoking status and level of stigma are inconsistent as some studies did not find significant association between smoking status and lung cancer stigma [8, 40].
Women with cervical cancer, on the other hand, could not risk others finding out they had cancer, for fear of being considered ‘spoiled’ or ‘ruined’ [28] and some felt so ashamed and embarrassed that they tell others they had uterine cancer instead of cervical cancer to avoid being the centre of gossip [18]. A similar experience was shared by men with breast cancer who would rather use the term ‘çhest cancer’ in describing their diagnosis [79].
In patients with mixed cancer types, negative attitudes toward cancer were associated with being older than 60-year-old, possessing higher education, earning low income and feeling socially excluded [90]. Some inconsistencies were, however, found in the association between educational level and stigma in the included studies amongst patients with mixed cancer types [64, 90].
• Impact of stigma on physician–patients–family cancer communications
Stigma associated with communicating a cancer diagnosis is enacted by the clinicians who choose to use euphemisms like ‘inflammation’ or ‘wound’ rather than the word ‘cancer’ [28]. The doctors in conspiracy with family and friends also, often failed to fully disclose to the patient their diagnosis which sometimes resulted in patients’s feeling worried about their condition or becoming so hopeful for a cure that they invest on expensive treatment that further plunge them into debt [92, 34, 54].
• Impact of cancer related stigma on family members of cancer patients
Apart from cancer patients, members of their families and caregivers also experience cancer-related stigma. Caregivers of lung cancer patients, for instance, were found to experience stigma by association as members of the patients support system and reported feeling invisible and unsupported [55]. Also, in Uganda, children of women with cancer of marriageable age risk not getting someone to marry due to the rollover cancer stigma to the children [46].
• Stigma perceived by cancer survivors
Cancer survivors also experienced the structural dimension of stigma in terms of the lack of policies to protect those affected by cancer and the dearth of resources for research, information and support services for patients with some types of cancers [18, 49]. A good number of MBC reported experiencing sexual stigmatisation in the process of accessing cancer care because nothing within the clinical setting points to the possibility of men fitting in, thereby making them feel unwelcomed [48, 79].
• Coping with cancer stigma
Women with breast cancer often cope with public stigma and self‐stigmatisation through social support, prayers, maintaining positive outlook, acceptance of diagnosis and ignoring negative comments [46, 92]. The women with cervical cancer in Recife, Brazil accepted and coped with their lot in life by drawing on stigmatising metaphors to construct narratives that would help them understand the relationship between their new, ill, and, therefore, different selves and the world they have always known [28]. However, most patients and their families in a stakeholders’ study were reported to cope via non-disclosure of cancer and limiting contact with others in other to avoid being an object of sympathy from others and to avoid getting misleading information that may discourage them [50].
• Possible explanations for the experience and expression of cancer stigma
Some authors attempted to make sense of the reasons behind stigma against cancer and those affected by cancer. Amongst the reasons adduced were: blame apportioning, disgust propensity, gender differences, having not experienced cancer or the behaviours that are thought to cause cancer and being a member of an ethnic minority [3, 6, 41, 56, 62, 77]. The role of gender in cancer stigma is not consistent in literature. Whilst women were reported to be more likely than men to express stigmatic behaviours against people with cancer in a study [56], men were more probable culprits in others [62, 77].
Perceived impact of cancer stigma on screening and patients’ health seeking behaviour
The notion of cancer as a terrible disease that is linked with death, dread, doubt, distress, shame and blame [33, 35, 50, 64, 65, 77, 78, 92, 92] lead to disease concealment to avoid being judged, delayed treatment and use of traditional healers rather than biomedical treatment [18, 29, 40, 58, 81, 63].
In the study from Uganda, BCS described breast cancer‐related stigma as a barrier to care even before a diagnosis is made as the stigma could affect their marriage and family [46]. Similarly, in an Indian study, breast and cervical cancer patients stated that cancer stigma was present in their lives and communities, was a feared outcome of a cancer diagnosis and a barrier to cervical screening, early diagnosis and treatment seeking for women even as symptoms worsened [54]. Also in the UK, higher total cancer stigma was significantly associated with less likelihood of screening for cervical, breast and colorectal cancers [77]. In the USA, a statistically significant positive correlation was found between perceived lung cancer stigma and delayed medical help seeking [8]. It thus seems that irrespective of cancer type, across different geographical and cultural divides, cancer stigma presents as a ubiquitous barrier to health seeking behaviour. However, an Australian study reported no significant association between lung cancer stigma and help-seeking behaviours in terms of accessing available hospital services to support their care [60]. Beyond stigma, respondents in a study in India hold the view that the cost of treatment, reliance on alternative medicine, fear of being diagnosed and fatalistic beliefs were the main barriers to health seeking behaviour [29]. However, these reasons, especially fear of being diagnosed and fatalistic beliefs appear to have some indirect link with internalised stigma.
Influence of cancer related stigma on psychosocial, behavioural and health outcomes
The social impact of cancer stigma is strongly enacted in the workplace context affecting cancer survivors’ employability due to high likelihood of hiring discrimination, job loss and limited career advancement [66]. Whilst ability to return to work even if in a limited capacity can help mend the disruption caused by the illness, inability to resume work with the inevitable reliance on others and welfare benefits could confer a stigmatised identity of helplessness in individuals who prior to their diagnosis were conscientious workers and providers for other [49].
Psychologically, a USA based online survey that assessed public perceptions and stigma due to listing cancer as the cause of death in celebrity obituary, found that lung cancer as a cause of death (as compared with liver cancer or death by an undisclosed cause) increased both anxiety and sadness, with anxiety then leading to increased origin-related stigma [51]. The results of this study imply that stigmatization leads to increased symptoms of grief when it is transferred into negative discriminatory behavior, which is also referred to as ‘enacted stigma’. Social stigma attached to cancer, which manifests itself in negative discrimination, may keep patients from disclosing their illness and cause them to ‘suffer in silence’ by isolating them from social interactions and interrupting the resolution of grief. Thus enacted stigma increases the likelihood of negative illness perception which if central to one’s self-definition may result in increased the grief symptomatology. [26]. Furthermore, it was found that within person, fluctuations in stigma were related to social and role functioning in patients with lung cancer, regardless of physical symptoms and were not carried over to the next day [65]. Evidence of positive correlation between stigma and anxiety [11, 88], depression [11, 23, 90, 93], higher self-perceived burden [88], symptom burden [93, 43] and affective interferences [37] were also reported. Body image and social support were found to mediate the relationship between stigma and depression in cancer patients [23, 43].
Studies showed that stigma had negative relationship with QoL and/or some of its subscales in patients with oral cancer, prostate cancer, breast cancer, lung cancer and in a group of patients with different cancer type [22, 37, 52, 84–87, 89, 91]. It also had an inverse relationship with hope and social support [91], posttraumatic growth [85], good healthcare provider communication [81], NK subset of cellular immunity, doctors’ empathy and patients’ self-efficacy [88]. Pain intensity was found to mediate the relationship between stigma and QoL in breast cancer patients [52].
Unexpectedly, some studies reported findings of posttraumatic growth borne out of patients accepting their experience of cancer and the stigma that comes with it [18, 28, 69]. In the USA, one of the positive consequences of cervical cancer-related stigma that some women witnessed and experienced became a powerful catalyst for their involvement in the awareness-raising movement and advocacy to enlighten people about the devastation of cervical cancer and the true prevalence of human papilloma virus (HPV) [18]. The women with cervical cancer in Brazil accepted their lot through reframing and the use of metaphors because for many of them the story of sexual impurity and cervical cancer was not just about stigma and shame but also about the possibility of hope for redemption and a journey back in time to health and sexual purity which their vaginal narrowing and dryness caused by radiation therapy would offer, suggesting that they would not just be healed, but they would become ‘virgins’ again [28]. Also, acceptance triggered an awakening of new life interpretations and psychological growth in head and neck cancer patients in Australia who through their personal experience of stigma were able to acquire previously unfelt empathetic understanding and altruism towards others with cancer [69].
Interventions addressing cancer stigma and their effectiveness
There was a dearth of studies on interventions addressing cancer stigma in the reviewed articles. Only two cancer-related stigma intervention studies were found. The first was an online intervention in the UK conducted to increase cervical cancer screening intention and by extension screening uptake [80]. The authors used public stigma toward people who had not been screened for cervical cancer as a tool to craft emotive narrative within news articles for respondents to read before responding to items on the study instruments. It was found that the emotive narrative within news articles was more effective in enhancing the willingness of women to attend a cervical screening appointment compared to factual information or no information [80]. The authors opined that emotive narratives within news articles can promote screening through increases public stigma.
The other study on cancer-related stigma intervention was located amongst studies reviewed by Webb et al [81]. The authors of the study used telephone acceptance-focused cognitive behavioural intervention to address stigma in people with lung cancer. The pre- and post-test outcome measures were of psychological and cancer-specific distress, depression, health-related stigma and QoL. At post-intervention, significant decrease was reported for psychological and cancer-specific distress, depression and health-related stigma but there was also a decline in QoL [94].
Implications of the present review
Implications for clinicians: The negative impact of cancer stigma on the clinician–patient–family communication reported in this review underscores the need for psychosocial interventions with potential to eliminate barriers to communication and improve patients and clinicians’ communication skills within oncology settings. Furthermore, clinicians ought to recognise that the cancer stigma is a multifaceted phenomenon that varies by type of cancer across factors such as actual or perceived causes, treatments and outcomes as well as the sociocultural environment within which the disease is been experienced. Such realisation would help the attending clinician sensitively tailor consultation to prevent and mitigate both individual and structural level stigma.
Implications for future researchers: There is dearth of interventions for reducing or managing cancer-related stigma both in clinical settings and in the community. Thus, understanding patients and caregiver strategies for coping with cancer stigma as well as what works in preventing or managing it requires further research. It is also noteworthy to observe the paucity of research on social impact of cancer stigma from low and middle income countries especially of Africa where the global cancer burden is huge. This demands the attention of researchers from these regions as well as that of research funding agencies. Further still, more focus could be directed at the stigmatising aspects of cancer and its treatment in future research and in the design of evidence-based psychosocial interventions.
Implications for service development and policy: The findings of the role of the media in innocently promoting stigma against certain cancers as well as the perceived discrimination in the workplace due to cancer diagnosis and structural level stigma in how social and healthcare services are provided have implication for service development and policy. Whilst some countries such as the USA [2] may have legislations to protect cancer patients from work place discrimination, there is need for policy makers in settings where this does not exist to enact policies that further protect the interest of those living with cancer in terms of job hiring, placement and career progression. There is also need for policies to regulate public health communication pro cesses to avert the unintentional labelling and stigmatising of patients [30]. Also, service providers should create destigmatising services (such as support groups and information services) for cancer patients irrespective of gender and cancer types.
Discussion
The experience of cancer stigma was pervasive in most of the studies included in our review. This seemed to agree with the notion of cancer as one of the most stigmatised disease conditions in many societies [19]. The fear of cancer stigma and associated fatalism, shame and anxiety prevent many from engaging in cancer prevention practices, screening and seeking health services [19, 32, 67]. Patients with breast and prostate cancers were less stigmatised compared to those with lung and cervical cancer mainly due to the perception that the latter are self-caused through wrong choices [21, 44] and as such are often blamed for their condition [12].
The use of both adaptive coping strategies such as cognitive reframing, acceptance, religious faith and ignoring negative comments [28, 46, 92] and dysfunctional coping techniques like non-disclosure of diagnosis and avoidance [50] were used by cancer patients to deal with stigma. However, utilising maladaptive coping strategies have been significantly associated with depressive symptoms [59, 95].
Furthermore, cancer stigma negatively impact communication between patients, physician and family members. It also resulted in poorer psychosocial and health outcome for cancer patients as well as work place discrimination, poor QoL, increased depression and anxiety. These findings which were also reported in earlier studies [94, 15, 24, 35] are begging for the development of more evidence-based psychosocial and clinical interventions to reduce stigma. Psychosocial interventions may focus on altering targeted health problems and behaviours using behaviour change interventions and social policies that refute the tendency of perpetrators to stigmatise, and enhance resilience in the stigmatised thereby making them less vulnerable to the negative impact of stigma [35, 82]. Clinical interventions may emphasise the use of biomedical procedures to help reduce the consequences of cancer treatments, thereby reducing stigma associated with certain cancers. For instance, the course of cervical cancer disease and the treatments for it like most gynaecological cancers can compromise fertility and reproductive capacity in affected women further fuelling stigma in this group. However, offering fertility-sparing techniques to young unmarried women with gynaecological cancers may contribute to not only improving the QoL of these women [38, 75] but also to reducing the stigma associated with their diagnosis.
Conclusion
Stigma contributes to the burden of illness for cancer patients and their family members. The findings of this study have provided invaluable direction for developing interventions to tackle cancer stigma in the general populace, amongst clinicians providing care for cancer patients and amongst the cancer patients themselves. The general public need to be better educated about cancer as a non-communicable disease and the place of appropriate screening for early detection to enhance better treatment outcome. Public enlightenment campaigns to promote the adoption of modifiable cancer risk preventive behaviours should be designed to not further escalate cancer stigma. Healthcare providers should be involved in ongoing communication training to enable them act and speak in ways that are destigmatised when relating with those affected by cancer. To prevent or overcome self-stigmatisation, interventions to help cancer patients accept their new identity and improve their body image should be developed [23]. Furthermore, legal instruments as well as administrative and clinical structures should be created to protect the interests of cancer patients in the workplace, at the health facilities where they receive care or at the government or non-governmental agencies where they seek social support for their care.
Strengths and limitations
Our study has some limitations. Firstly, our inclusion criteria that only articles with the terms ‘cancer’ and ‘stigma’ would be reviewed may increase the likelihood of omitting studies without these two key words occurring together in the title but that may have contents that are relevant to cancer stigma. Also, although we endeavoured to include all relevant studies with the words ‘cancer’ and ‘stigma’, there were several studies whose full text contents could not be accessed and we cannot say with certainty that all full text articles available in the public domain were accessed and assessed. However, we did not limit the types of studies reviewed to a specific methodology or a specific population which ensured that a wide variety of studies were reviewed so long as the study was related to cancer stigma.
Funding declaration
This study was funded by the ReTOOL Program (National Cancer Institute/National Institutes of Health R25CA214225).
Conflicts of interest statement
The authors have declared that they have no conflicts of interest.
References
1. Açıkel GY and Pakyüz SÇ (2015) Evaluating the stigma on patients with tuberculosis J Florence Nightingale Nurs 23 136‑145
2. Americans with Disabilities Act, Amendment Acts (2008) ADA Amendments Act of 2008 http://www.eeoc.gov/laws/statutes/adaaa.cfm Date accessed: 30/06/21
3. Azlan HA, Overton PG, and Simpson J, et al (2020) Disgust propensity has a causal link to the stigmatization of people with cancer J Behav Med 43(3) 377–390 https://doi.org/10.1007/s10865-019-00130-4
4. Bamidele OO, McGarvey H, and Lagan BM, et al (2019) Hard to reach, but not out of reach”: Barriers and facilitators to recruiting Black African and Black Caribbean men with prostate cancer and their partners into qualitative research Eur J Cancer Care (Engl) 28 e12977
5. Baxter NN, Goodwin PJ, and McLeod RS, et al (2006) Reliability and validity of the body image after breast cancer questionnaire Breast J 12 221–32 https://doi.org/10.1111/j.1075-122X.2006.00246.x PMID: 16684320
6. Bresnahan MJ, Silk K, and Zhuang, J (2013) You did this to yourself! Stigma and blame in lung cancer J Appl Social Psychol 43 https://doi.org/10.1111/jasp.12030
7. Carter-Harris L and Hall LA (2014) Development of a short version of the Cataldo Lung Cancer Stigma Scale J Psychosoc Oncol 32 665–677 https://doi.org/10.1080/07347332.2014.955238 PMID: 25157591 PMCID: 4224672
8. Carter-Harris, L (2015) Lung cancer stigma as a barrier to medical help-seeking behavior: practice implications J Am Assoc Nurse Pract 27(5) 240–24 https://doi.org/10.1002/2327-6924.12227 PMID: 25736473 PMCID: 4414901
9. Cataldo JK, Jahan TM, and Pongquan VL (2012) Lung cancer stigma, depression, and quality of life among ever and never smokers Eur J Oncol Nurs 16 264‑269 https://doi.org/10.1016/j.ejon.2011.06.008 PMCID: 3360805
10. Cataldo JK, Slaughter R, and Jahan TM, et al (2011) Measuring stigma in people with lung cancer: psychometric testing of the Cataldo Lung Cancer Stigma Scale Oncol Nurs Forum 38 E46–E54 https://doi.org/10.1188/11.ONF.E46-E54 PMCID: 3182474
11. Cataldo JK and Brodsky JL (2013) Lung cancer stigma, anxiety, depression and symptom severity Oncology 85(1) 33–40 https://doi.org/10.1159/000350834 PMID: 23816853
12. Chapple A, Ziebland S, and McPherson A (2004) Stigma, shame, and blame experienced by patients with lung cancer: qualitative study (Electronic version) Br Med J 328 1470 https://doi.org/10.1136/bmj.38111.639734.7C
13. Cho J, Smith K, and Choi EK, et al (2013) Public attitudes toward cancer and cancer patients: a national survey in Korea Psychooncology 22 605‑613 https://doi.org/10.1002/pon.3041
14. Copel L and Al-Mamari K (2015) Stigma in Mental Health: A Concept Analysis College of Nursing, Villanova University, Villanova, PA (Sigma Theta Tau International) pp 1–44
15. Corrigan, P (2004) How stigma interferes with mental health care Am Psychol 59(7) 614–625 https://doi.org/10.1037/0003-066X.59.7.614 PMID: 15491256
16. Crocker J, Major B, and Steele C (1998) Social stigma The Handbook of Social Psychology 4th edn eds DT Gilbert, ST Fiske, and G Lindzey (Boston: McGraw Hill) pp 504–553
17. Dodd RH, Forster AS, and Marlow LAV, et al (2019) Psychosocial impact of human papillomavirus-related head and neck cancer on patients and their partners: a qualitative interview study Eur J Cancer Care (Engl) 28 e12999 https://doi.org/10.1111/ecc.12999
18. Dyer K (2010) 2010 P K New award from cancer to sexually transmitted infection: explorations of social stigma among cervical cancer survivors Hum Organ 69(4) 321–330 https://doi.org/10.17730/humo.69.4.a750670h0784521j
19. Edelen MO, Chandra A, and Stucky B et al (2014) Developing a global cancer stigma index SAGE Open 4(3) 1–9 https://doi.org/10.1177/2158244014547875
20. Eichhorn S, Mehnert A, and Stephan M (2015) German version of the social impact scale (SIS-D)–pilot testing of an instrument for measuring experienced stigmatization in a sample of cancer patients Psychother Psychosom Med Psychol 65(5) 183–190 PMID: 25794353
21. Else-Quest NM and Jackson TL (2014) Cancer stigma The Stigma of Disease and Disability ed P Corrigan (Washington: American Psychological Association) pp 165–182
22. Ernst J, Mehnert A, and Dietz A, et al (2017) Perceived stigmatization and its impact on quality of life - results from a large register-based study including breast, colon, prostate and lung cancer patients BMC Cancer 17(1) https://doi.org/10.1186/s12885-017-3742-2 PMID: 29121876 PMCID: 5680772
23. Esser P, Mehnert A, and Johansen C, et al (2018) Body image mediates the effect of cancer-related stigmatization on depression: a new target for intervention Psychooncology 27(1) 193–198 https://doi.org/10.1002/pon.4494
24. Fife BL and Wright ER (2000) The dimensionality of stigma: a comparison of its impact on the self of persons with HIV/AIDS and cancer J Health Soc Behav 41(1) 50–67 https://doi.org/10.2307/2676360 PMID: 10750322
25. Goffman E (1963) Stigma: Notes on the Management of Spoiled Identity (Englewood Cliffs: Prentice-Hall Inc)
26. Gökler-Danışman I, Yalçınay-Inan M, and Yiğit I (2017) Experience of grief by patients with cancer in relation to perceptions of illness: the mediating roles of identity centrality, stigma-induced discrimination, and hopefulness J Psychosoc Oncol 35(6) 776–796 https://doi.org/10.1080/07347332.2017.1340389
27. González LF, and Diaz-Castrillón F (2019) ‘Until it kills you’: cancer related stigma on the Chilean tobacco packaging warning messages 2014-2016 campaign Int J Health Promot Educ 57(4) 179–190 https://doi.org/10.1080/14635240.2019.1578682
28. Gregg JL (2011) An unanticipated source of hope: stigma and cervical cancer in Brazil Med Anthropol Q 25(1) 70–84 https://doi.org/10.1111/j.1548-1387.2010.01137.x
29. Gupta A, Dhillon PK, and Govil J, et al (2015) Multiple stakeholder perspectives on cancer stigma in North India Asian Pac J Cancer Prev 16(14) 6141–6147 https://doi.org/10.7314/APJCP.2015.16.14.6141 PMID: 26320509 PMCID: 5572627
30. Guttman N and Salmon CT (2004) Guilt, fear, stigma and knowledge gaps: ethical issues in public health communication interventions Bioethics 18 531–552 https://doi.org/10.1111/j.1467-8519.2004.00415.x PMID: 15580723
31. Hamann HA, Shen MJ, and Thomas AJ, et al (2018) Development and preliminary psychometric evaluation of a patient‐reported outcome measure for lung cancer stigma: the Lung Cancer Stigma Inventory (LCSI) Stigma Health 3(3) 195–203 https://doi.org/10.1037/sah0000089 PMID: 30393760 PMCID: 6208151
32. Hall AG, Khoury AJ, and Lopez ED, et al (2008) Breast cancer fatalism: the role of women’s perceptions of the health care system J Health Care Poor Underserved 19 1321–1335 https://doi.org/10.1353/hpu.0.0091 PMID: 19029755
33. Hamilton JB, Moore CE, and Powe BD, et al (2010) Perceptions of support among older African American cancer survivors Oncol Nurs Forum 37 484–493 https://doi.org/10.1188/10.ONF.484-493 PMID: 20591808 PMCID: 2948788
34. Harding R, Nair S, and Ekstrand M (2019) Multilevel model of stigma and barriers to cancer palliative care in India: a qualitative study BMJ Open 9(3) https://doi.org/10.1136/bmjopen-2018-024248
35. Heijnders M and Van Der Meij S (2006) The fight against stigma: an overview of stigma-reduction strategies and interventions Psychol Health Med 11(3) 353–363 https://doi.org/10.1080/13548500600595327 PMID: 17130071
36. Hong QN, Pluye P, and Fàbregues S, et al Mixed Methods Appraisal Tool (MMAT), version 2018 Registration of Copyright (#1148552), Canadian Intellectual Property Office, Industry Canada
37. Johnson LA, Schreler AM, and Swanson, M, et al (2019) Stigma and quality of life in patients with advanced lung cancer Oncol Nurs Forum 46(3) PMID: 31007259
38. Laganà AS, La Rosa VL, and Rapisarda AM, et al (2017) Psychological impact of fertility preservation techniques in women with gynaecological cancer Ecancermedicalscience 8(11) ed62 https://doi.org/10.3332/ecancer.2017.ed62 PMID: 28275393 PMCID: 5336386
39. Lim KS and Tan CT (2014) Epilepsy stigma in Asia: the meaning and impact of stigma Neurol Asia 19 1–10
40. Liu XH, Zhong JD, and Zhang JE et al (2019) Stigma and its correlates in people living with lung cancer: a cross‐sectional study from China Psychooncology 29(2) 287–293 https://doi.org/10.1002/pon.5245 PMID: 31654596
41. Luberto CM, Hyland KA, and Streck, JM, et al (2016) Stigmatic and sympathetic attitudes toward cancer patients who smoke: a qualitative analysis of an online discussion board forum Nicotine Tob Res 18(12) 2194–2201 https://doi.org/10.1093/ntr/ntw166 PMID: 27613953 PMCID: 5103935
42. Machado GD, Biancovilli P, and Jurberg C (2017) Voices about a stigma: cancer in the opinion of three different segments in Brazilian Society J Cancer Educ 32(2) 413–416 https://doi.org/10.1007/s13187-015-0962-5
43. Mak WWS and Cheung RYM (2010) Self-stigma among concealable minorities in Hong Kong: conceptualization and unified measurement Am J Orthopsychiatry 80(2) 267–281 https://doi.org/10.1111/j.1939-0025.2010.01030.x PMID: 20553520
44. Marlow LAV, Waller J and Wardle J (2010) Variation in blame attributions across different cancer types Cancer Epidemiol Biomarkers Prev 19 1799–1805 https://doi.org/10.1158/1055-9965.EPI-09-1298 PMID: 20551306 PMCID: 2901591
45. Marlow LAV and Wardle J (2014) Development of a scale to assess cancer stigma in the non-patient population BMC Cancer 14 285 https://doi.org/10.1186/1471-2407-14-285 PMID: 24758482 PMCID: 4021096
46. Meacham E, Orem J, and Nakigudde G, et al (2016) Exploring stigma as a barrier to cancer service engagement with breast cancer survivors in Kampala, Uganda Psychooncology 25(10) 1206–1211 https://doi.org/10.1002/pon.4215 PMID: 27421234
47. Mengista W, Soromessab T, and Legese G (2020) Method for conducting systematic literature review and meta-analysis for environmental science research MethodsX 7 100777 https://doi.org/10.1016/j.mex.2019.100777
48. Midding E, Halbach SM, and Kowalski C, et al (2018) Men with a “woman’s disease”: stigmatization of male breast cancer patients—a mixed methods analysis Am J Mens Health 12(6) 2194–2207 https://doi.org/10.1177/1557988318799025 PMID: 30222029 PMCID: 6199445
49. Moffatt S and Noble E (2015) Work or welfare after cancer? Explorations of identity and stigma Sociol Health Illn 37(8) 1191–1205 https://doi.org/10.1111/1467-9566.12303 PMID: 26139163
50. Mohabbat-bahar S, Bigdeli I, and Mashhadi A, et al (2017) Investigation of stigma phenomenon in cancer: a grounded theory study Int J Cancer Manag 10(2) e6596
51. Myrick JG (2017) Public perceptions of celebrity cancer deaths: how identification and emotions shape cancer stigma and behavioral intentions Health Commun 32(11) 1385–1395 https://doi.org/10.1080/10410236.2016.1224450
52. Nakash O, Granek L, and Cohen M et al (2019) Association between cancer stigma, pain and quality of life in breast cancer Psychol Community Health 8(1) 275–287 https://doi.org/10.5964/pch.v8i1.310
53. Noroozi M, Noroozi A, and Farhoudian A, et al (2018) Factors associated with HIV testing among people who inject drugs Tehran J Subst Use 23 322–326 https://doi.org/10.1080/14659891.2017.1405093
54. Nyblade L, Stockton M, and Travasso S, et al (2017) A qualitative exploration of cervical and breast cancer stigma in Karnataka, India BMC Womens Health 17(1) https://doi.org/10.1186/s12905-017-0407-x PMID: 28768506 PMCID: 5541646
55. Occhipinti S, Dunn J, and O’Connell DL, et al (2018) Lung cancer stigma across the social network: patient and caregiver perspectives J Thorac Oncol 13(10) 1443–1453 https://doi.org/10.1016/j.jtho.2018.06.015 PMID: 29981928
56. Ongtengco N, Thiam H, and Collins Z, et al (2020) Role of gender in perspectives of discrimination, stigma, and attitudes relative to cervical cancer in rural Sénégal PLoS One 15(4) https://doi.org/10.1371/journal.pone.0232291 PMCID: 7188246
57. Ostroff JS, Riley KE, and Shen MJ et al (2019) Lung cancer stigma and depression: validation of the Lung Cancer Stigma Inventory Psychooncology 28 1011–1017 PMID: 30779396 PMCID: 6506363
58. Oystacher T, Blasco D, and He E, et al (2018) Understanding stigma as a barrier to accessing cancer treatment in South Africa: implications for public health campaigns Pan Afr Med J 29 https://doi.org/10.11604/pamj.2018.29.73.14399 PMID: 29875954 PMCID: 5987085
59. Phelan SM, Griffin JM, and Jackson GL, et al (2013) Stigma, perceived blame, selfblame, and depressive symptoms in men with colorectal cancer Psychooncology 22 65–73 https://doi.org/10.1002/pon.2048
60. Rose S, Boyes A, and Kelly B, et al (2018) Help-seeking behaviour in newly diagnosed lung cancer patients: assessing the role of perceived stigma Psychooncology 27(9) 2141–2147 https://doi.org/10.1002/pon.4779 PMID: 29802652 PMCID: 6175243
61. Scambler G (2009) Health-related stigma Sociol Health Illn 31 441–455 https://doi.org/10.1111/j.1467-9566.2009.01161.x PMID: 19366430
62. Shepherd MA and Gerend MA (2014) The blame game: cervical cancer, knowledge of its link to human papillomavirus and stigma Psychology Health 29(1) 94–109 https://doi.org/10.1080/08870446.2013.834057
63. Shiri FH, Mohtashami J, and Manoochehri H, et al (2018) Explaining the meaning of cancer stigma from the point of view of Iranian stakeholders: a qualitative study Int J Cancer Manage 11(7)
64. Shiri FH, Mohtashami J, and Nasiri M, et al (2018) Stigma and related factors in Iranian people with cancer Asian Pac J Cancer Prev 19 PMCID: 6171385
65. Steffen LE, Vowles KE, and Smith BW et al (2018) Daily diary study of hope, stigma, and functioning in lung cancer patients Health Psychol 37(3) 218–227 https://doi.org/10.1037/hea0000570 PMCID: 5837918
66. Stergiou-Kita M, Qie X, and Yau HK, et al (2017) Stigma and work discrimination among cancer survivors: a scoping review and recommendations Can J Occup Ther 84(3) 178–188 https://doi.org/10.1177/0008417417701229 PMID: 28608726
67. Tang P, Mayer DK, and Chou F, et al (2015) The experience of cancer stigma in Taiwan: a qualitative study of female cancer patients Arch Psych Nurs 30(2) 204–209 https://doi.org/10.1016/j.apnu.2015.08.015
68. Thornicroft G, Brohan E, and Rose D, et al (2009) Global pattern of experienced and anticipated discrimination against people with schizophrenia: a cross-sectional survey Lancet 373(9661) 408–415 https://doi.org/10.1016/S0140-6736(08)61817-6 PMID: 19162314
69. Threader J and Mccormack L (2016) Cancer-related trauma, stigma and growth: the ‘lived’ experience of head and neck cancer Eur J Cancer Care 25(1) 157–169 https://doi.org/10.1111/ecc.12320
70. Tod AM, Craven J, and Allmark P (2008) Diagnostic delay in lung cancer: a qualitative study J Adv Nurs 61 336–343 https://doi.org/10.1111/j.1365-2648.2007.04542.x PMID: 18197868
71. Tripathi L, Datta SS, and Agrawal SK, et al (2017) Stigma perceived by women following surgery for breast cancer Indian J Med Paediatr Oncol 38(2) PMID: 28900322 PMCID: 5582551
72. Trusson D and Pilnick A (2017) Between stigma and pink positivity: women’s perceptions of social interactions during and after breast cancer treatment Sociol Health Illn 39(3) 458–473 https://doi.org/10.1111/1467-9566.12486
73. Tsai W and Lu Q (2019) Ambivalence over emotional expression and intrusive thoughts as moderators of the link between self-stigma and depressive symptoms among Chinese American breast cancer survivors J Behav Med 42(3) 452–460 https://doi.org/10.1007/s10865-018-9996-6 PMCID: 6528814
74. Tsai W, Wu IH, and Lu Q (2019) Acculturation and quality of life among Chinese American breast cancer survivors: the mediating role of self‐stigma, ambivalence over emotion expression, and intrusive thoughts Psychooncology 28 1063–1070 PMID: 30838727 PMCID: 6506386
75. Vitale SG, La Rosa VL, and Rapisarda AM, et al (2018) Fertility preservation in women with gynaecologic cancer: the impact on quality of life and psychological well-being Human Fertil 21(1) 35–38 https://doi.org/10.1080/14647273.2017.1339365
76. Van Brakel WH (2006) Measuring health-related stigma–a literature review Psychol Health Med 11 307–334 https://doi.org/10.1080/13548500600595160 PMID: 17130068
77. Vrinten C, Gallagher A, and Waller J, et al (2019) Cancer stigma and cancer screening attendance: a population based survey in England BMC Cancer 19(1) https://doi.org/10.1186/s12885-019-5787-x PMID: 31185949 PMCID: 6561035
78. Mengist W, Soromessa T, and Legese G (2020) Ecosystem services research in mountainous regions: a systematic literature review on current knowledge and research gaps Sci Total Environ 702 134581 https://doi.org/10.1016/j.scitotenv.2019.134581
79. Walker RK and Berry DL (2019) Men with breast cancer experience stigma in the waiting room Breast J 26(2) 337–338 https://doi.org/10.1111/tbj.13593 PMID: 31538693
80. Wearn A, and Shepherd L (2020) The impact of emotion‐based mass media campaigns on stigma toward cervical screening non participation J Appl Social Psychol 50(5) 289–298 https://doi.org/10.1111/jasp.12659
81. Webb LA, McDonnell KK, and Adams SA, et al (2019) Exploring stigma among lung cancer survivors: a scoping literature review Oncol Nurs Forum 46(4) PMID: 31225843
82. Weiss MG, Ramakrishna J, and Somma D (2006) Health-related stigma: rethinking concepts and interventions Psychol Health Med 11(3) 277–287 https://doi.org/10.1080/13548500600595053 PMID: 17130065
83. Weiss J, Yang H, and Weiss S, et al (2017) Stigma, self-blame, and satisfaction with care among patients with lung cancer J Psychosoc Oncol 35 166–179 https://doi.org/10.1080/07347332.2016.1228095
84. Williamson TJ, Choi AK, and Kim JC, et al (2018) A longitudinal investigation of internalized stigma, constrained disclosure, and quality of life across 12 weeks in lung cancer patients on active oncologic treatment J Thorac Oncol 13(9) 1284–1293 https://doi.org/10.1016/j.jtho.2018.06.018 PMID: 29981926 PMCID: 6291203
85. Wong CC, Pan-Weisz BM, and Pan-Weisz TM, et al (2019) Self-stigma predicts lower quality of life in Chinese American breast cancer survivors: exploring the mediating role of intrusive thoughts and posttraumatic growth Qual Life Res 28(10) 2753–2760 https://doi.org/10.1007/s11136-019-02213-w PMID: 31123880
86. Wood A (2015) The Influence of Stigma on Quality of Life and Relationship Satisfaction for Prostate Cancer Survivors and Their Partners Electronic Theses and Dissertations, 1195 (University of Central Florida) https://stars.library.ucf.edu/etd/1195
87. Wood AW, Barden S, and Terk M, et al (2017) The influence of stigma on the quality of life for prostate cancer survivors J Psychosoc Oncol 35(4) 451–467 https://doi.org/10.1080/07347332.2017.1307896 PMID: 28318410
88. Yang N, Xiao H, and Wang W, et al (2018) Effects of doctors’ empathy abilities on the cellular immunity of patients with advanced prostate cancer treated by orchiectomy: the mediating role of patients’ stigma, self-efficacy, and anxiety Patient Prefer Adher 12 1305–1314 https://doi.org/10.2147/PPA.S166460
89. Yeung NC, Lu Q, and Mak WW (2019) Self-perceived burden mediates the relationship between self-stigma and quality of life among Chinese American breast cancer survivors Support Care Cancer 27(9) 3337–3345 https://doi.org/10.1007/s00520-018-4630-2 PMID: 30617433
90. Yilmaz M, Dissiz G, and Usluoğlu A, et al (2020) Cancer-related stigma and depression in cancer patients in a middle-income country Asia Pac J Oncol Nurs 7(1) 95 https://doi.org/10.4103/apjon.apjon_45_19
91. Zhang Y, Cui C, and Wang Y, et al (2020) Effects of stigma, hope and social support on quality of life among Chinese patients diagnosed with oral cancer: a cross-sectional study Health Qual Life Outcomes https://doi.org/10.1186/s12955-020-01353-9
92. Solikhah S, Matahari R, and Utami FP, et al (2020) Breast cancer stigma among Indonesian women: a case study of breast cancer patients BMC Women’s Health 20 116 https://doi.org/10.1186/s12905-020-000983-x
93. Maguire R, Lewis L, and Kotronoulas G, et al (2019) Lung cancer stigma: a concept with consequences for patients Cancer Rep (Hoboken) 2019 2(5) e1201 https://doi.org/10.1002/cnr2.1201. Epub 2019 Jun 24 PMID: 32721137 PMCID: 7941499
94. Chambers SK, Morris BA, and Clutton S, et al (2015) Psychological wellness and health-related stigma: a pilot study of an acceptance-focused cognitive behavioural intervention for people with lung cancer Eur J Cancer Care 24 60–70 https://doi.org/10.1111/ecc.12221
95. Bennett KK, Compas BE, and Beckjord E, et al (2005) Self-blame and distress among women with newly diagnosed breast cancer J Behav Med 28 313–323
Supplementary Data
Table S1. Methodological QA of all included studies.