Genetic polymorphisms related to the vitamin D pathway in patients with cirrhosis with or without hepatocellular carcinoma (HCC)
Beatriz de Jesus Brait1, Simone Perpétua da Silva Lima1, Franciana Luísa Aguiar1, Rafael Fernandes-Ferreira2,3, Camila Ive Ferreira Oliveira-Brancati1, Joyce Aparecida Martins Lopes Ferraz1, Graciele Domitila Tenani1, Marcela Augusta de Souza Pinhel1, Leticia Carolina Paraboli Assoni1, Augusto Haniu Nakahara1, Natalia dos Santos Jábali1, Octavio Pennella Fenelon Costa1, Maria Eduarda Lopes Baitello1, Sidney Pinheiro Júnior1, Renato Ferreira Silva1, Rita de Cássia Martins Alves Silva1 and Doroteia Rossi da Silva Souza1
1São José do Rio Preto Medical School (FAMERP), São José do Rio Preto, SP, 15090-000, Brazil
2Campinas State University (UNICAMP), Campinas, SP, 13083-970, Brazil
3Paulista University (UNIP) São Paulo, SP, 01311-000, Brazil
ahttps://orcid.org/0000-0002-8901-3996
Abstract
Objective: To evaluate the association of genetic polymorphisms of vitamin D transporter protein (DBPrs4588 and DBP-rs7041) and cytochrome P450-24A1 (CYP24A1-rs6013897) in patients with cirrhosis with or without hepatocellular carcinoma (HCC), including demographic/clinical/biochemical profiles.
Methods: A total of 383 individuals were studied, considering the total group (TotalG) of patients with cirrhosis (TotalG: N = 158) with or without HCC, distributed into Group 1 (G1): cirrhosis and HCC; Group 2 (G2): isolated cirrhosis; and 225 individuals without hepatopathies (G3). Polymorphisms were analysed by real-time polymerase chain reaction. An alpha error of 5% was admitted.
Results: CYP24A1-rs6013897 predominated the genotype with at least one polymorphic allele (_/T) in G1 (98.3%) versus G2 (88.8%; p = 0.0309). There was a moderate positive correlation between vitamin D and parathyroid hormone in patients (TotalG: R2 = 0.3273). Smoking, alcoholism and diabetes mellitus (DM) stood out as independent factors for cirrhosis, as well as for cirrhosis with HCC, except for smoking, adding, in this case, advanced age, male gender, polymorphic allele of CYP24A1-rs6013897, viral hepatitis and high levels of serum gamma-glutamyl transferase (GGT), alpha-fetoprotein (AFP) and creatinine. An increase in survival was observed in the presence of the polymorphic allele of DBP-rs7041 (p = 0.0282).
Conclusion: CYP24A1-rs6013897 is associated with cirrhosis and HCC as a predictor, while DBP-rs4588 is associated with reduced vitamin D, and DBP-rs7041 provides increased survival, suggesting a protective characteristic. Advanced age, alcoholism, DM, viral hepatitis and high levels of GGT, AFP and creatinine are also confirmed as predictors of HCC and cirrhosis, while smoking, alcoholism and DM for isolated cirrhosis only.
Keywords: liver, single nucleotide polymorphism, neoplasia, vitamin D
Correspondence to: Beatriz de Jesus Brait
Email: beatrizjbrait@gmail.com
Published: 04/05/2022
Received: 26/07/2021
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Cirrhosis, the tenth leading cause of death in the world [1], is an irreversible chronic liver disease characterised by fibrosis, several structural liver lesions [2] and the formation of regenerative nodules [3], whose prevalence is underestimated in asymptomatic patients [4].Cirrhosis is directly associated with the development of hepatocellular carcinoma (HCC) [2], present in 90% of the cases of this tumour type [5]. HCC represents the main primary liver neoplasia [6], being the second most common cause of cancer-related deaths [6] in the world, with 905,677 cases per year [7].
Admittedly, biomolecular events that trigger hepatic carcinogenesis may result from alterations that interfere with the synthesis of deoxyribonucleic acid (DNA) [8]. In addition, the role of vitamin D stands out, being recognised for maintaining calcium homeostasis, immunomodulation, participation as a modulator of cell proliferation and for its inhibitory power in cancer [9].
The vitamin D transporter protein gene (DBP) participates and functions in metabolic and biological pathways, such as the regulation of bone development, including actin capture and modulation of immune responses [10]. In this case, the genetic variants DBP-rs4588 and DBP-rs7041 are associated with reduced serum levels of 25-hydroxy-vitamin D [25(OH)D] [11], which may have clinical consequences [11], which need clarification for cirrhosis and HCC.
The gene of the cytochrome P450 from the family 24, subfamily A, member 1 (CYP24A1) encodes 25-hydroxyvitamin D3-24-hydroxylase. This enzyme catalyses the conversion of 25(OH)D3 and 1.25(OH)2D3 into hydroxylated products, which constitute the degradation of the vitamin D [12] molecule. Additionally, the increased expression of CYP24A1, a regulator of vitamin D, and the activity of the respective 24-hydroxylase enzyme are associated with the degradation of 25(OH)D3 into 24.25(OH)2D3 [13]. CYP24A1 induces low serum levels of 25(OH)D3, which has been shown with liver disease severity in studies with non-alcoholic fatty liver disease (NAFLD) [14] and patients with hepatitis C (HCV) [15]. Furthermore, some studies suggest that CYP24A1 single nucleotide polymorphisms (SNPs) contributes to a chronic HCV infection, progressing to more defined conditions [16], such as the risk for liver cancer [17].
It is noteworthy that vitamin D, in its active form 1.25(OH)2D, regulates several genes, including the key effector of its catabolism, the CYP24A1 [18] related to prostate cancer [19], whose expression is increased in patients with advanced stage disease [20]. Furthermore, the genetic variants of CYP24A1 (rs6013897) are associated with inflammatory reactions [21], which should be clarified in liver diseases.
Thus, this study aimed at evaluating the association of genetic polymorphisms of DBP (rs4588 and rs7041) and CYP24A1 (rs6013897) in cirrhosis with or without HCC, considering demographic–clinical–biochemical profile, as well as lifestyle and survival habits.
Methods
A total of 383 individuals were studied and distributed into groups. The total group (TotalG), consisting of 158 patients, was subdivided into Group 1 (G1) = 60 (46–81 years), with a diagnosis of cirrhosis with HCC; and Group 2 (G2) = 98 (16–71 years), with isolated cirrhosis, both monitored at the Liver Transplant Service and Cancer Institute, Base Hospital/São José do Rio Preto Medical School-HB/FAMERP. A group of 225 individuals without clinical and laboratory evidence (serum levels of aspartate aminotransferase (AST), alanine aminotransferase (ALT) and gamma-glutamyl transferase (GGT)) of liver diseases – control group – (G3), aged 20–84 years, was selected at the Blood Centre – HB/FAMERP, in addition to the volunteers. This study was approved by the Research Ethics Committee of São José do Rio Preto Medical School (CEP/FAMERP; Process number 435/2011 and 6910/2011).
Exclusion criteria included diseases correlating with reduced serum levels of vitamin D, such as type 1 diabetes, Crohn’s disease, tuberculosis, Hansen’s disease, multiple sclerosis, autoimmune hepatitis, psoriasis, Graves’ disease, and the use of vitamin supplements with vitamin D.
The diagnosis of cirrhosis was made by the combination of clinical criteria present in the disease (reduced liver volume, irregular surface and increased consistency, splenomegaly and peripheral signs of chronic liver disease and portal hypertension), laboratory tests (plateletopenia, hypoalbuminemia and coagulation disorders) and imaging (reduced liver volume, irregular surface and signs of portal hypertension), and by biopsy, when necessary.
The diagnosis of HCC was carried out according to the practice guidelines of the American Association for the Study of Liver Disease [22]. The degree of staging for cirrhosis and HCC was classified using the Child-Pugh and model for end-stage liver disease methods, and both were used to classify the severity of liver disease [23].
Data on comorbidities (systemic arterial hypertension (SAH) and diabetes mellitus (DM)), lifestyle (smoking and alcohol consumption), demographic profile (gender and age) and biochemical profile (AST, ALT, GGT, alpha-fetoprotein (AFP), bilirubin and albumin) were obtained through a questionnaire, electronic or physical medical records and pre-established protocols for routine follow-up of patients in those services.
Serum dosages of vitamin D and parathyroid hormone (PTH) were measured in the subgroups: TGd = 30 patients from the TotalG, 4 with cirrhosis and HCC (G1d) and 26 with isolated cirrhosis (G2d); and G3d = 20 individuals in the control group without hepatopathies. Altered values for vitamin D, serum levels <30 ng/mL [24] and for PTH <15 and >65 pg/mL [25] were considered.
After genomic DNA extraction from the peripheral blood [26], SNPs of the DBP-rs4588 (C___8278879_10), DBP-rs7041 (C___3133594_30) and CYP24A1-rs6013897 (C__29958084_10) genes were genotyped by TaqMan® (Thermo Fisher) by polymerase chain reaction (PCR), according to the manufacturer’s manual. The reactions for the amplification of the polymorphic segments were carried out in the following thermocycles: 95°C for 10 minutes, followed by 47 cycles at 92°C for 15 seconds each and 60°C for 1 minute, in the StepOnePlus Real-Time PCR System (Applied Biosystems). Allele discrimination was conducted using the StepOne software v2.3 (Applied Biosystems) programme.
Fisher’s exact test or chi-square test was applied to analyse qualitative variables, including genotypic and allelic frequencies, sex, distribution of altered values for biochemical profile, comorbidities and lifestyle habits. T-test or Mann–Whitney test was used to analyse quantitative variables (age and biochemical profile) in the GraphPad Prism programme (version 5.0). Actuarial survival curve (Kaplan–Meier) was analysed considering at least one polymorphic allele, as well as logistic regression analysis (StatsDirect Statistical Analysis). For SNPs, the Hardy–Weinberg equilibrium (HWE) and linkage disequilibrium (LD) were analysed. In this case, the Arlequin v.3.11 and GraphPad Prism (version 5.0) programmes were used, respectively. A significance level was assumed for a value of p < 0.05.
Results
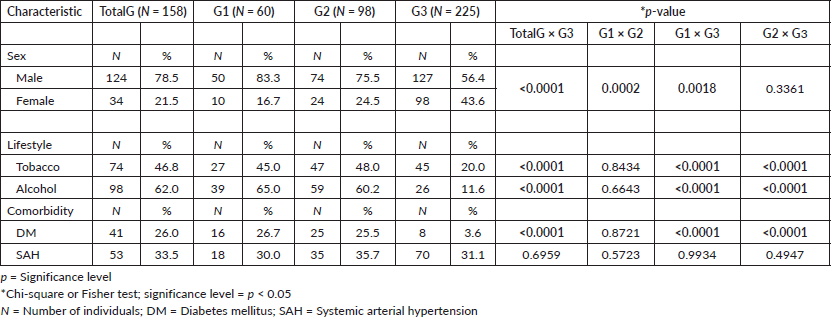
There was a prevalence of males in all groups, especially in patients with cirrhosis and HCC (G1) compared to the group with cirrhosis (G2; p = 0.0002) and G3 (p = 0.0018). Smoking, alcohol consumption and DM prevailed in patients compared to the controls (p < 0.0001; Table 1). Regarding the genetic profile, for DBP-rs4588 and DBP-rs7041, there was a similarity between groups in all comparisons for genotypic and allelic distribution (p > 0.05). For CYP24A1-rs6013897, the genotype with at least one polymorphic allele (_/T) predominated in G1 (98.3%) versus G2 (88.8%; p = 0.0309) (Table 2). HWE was observed for all SNPs, in patients and controls (p > 0.05). The LD analysis showed significance for the rs4588-rs7041 association in patients and controls (p = 0.0001, for both). The haplotypes were reconstructed for the set of DBP SNPs (rs4588 and rs7041) and compared between TotalG and G3, with no significant difference between groups (p > 0.05).
Regarding vitamin D, 30% (TGd) of the patients had altered values (<30 ng/mL), and the same was observed in 35% of the individuals without liver disease (G3d); for PTH, altered values (<15 or >65 ng/mL) corresponded to 16.7% and 15%, respectively, with a similarity between groups (p > 0.05), for both analyses. Patients with cirrhosis with or without HCC showed a moderate positive correlation (R2 = 0.3273) between serum vitamin D and PTH values, but this was not observed in the controls (R2 = 0.0106). Reduced levels of vitamin D in TotalG showed association with genotypes with at least one mutant allele (_/A) for DBP-rs4588 (77.8%) compared to G3 (14.3%; p = 0.0406).
Smoking, alcohol consumption and DM stood out as independent factors for isolated cirrhosis; while for cirrhosis with HCC alcoholism, DM, age, male gender, presence of polymorphic allele of CYP24A1-rs6013897 (_/T), viral hepatitis and altered serum levels of GGT, AFP and creatinine were the factors (Table 3).
There was a higher frequency of survival in patients with at least one polymorphic allele of DBP-rs7041 (_/G = 66.5% ± 6.0%), in 11 years of follow-up, compared to wild homozygote (T/T = 50.3% ± 8.7%; p = 0.0282; Figure 1a). However, there was a similarity between the subgroups of patients without transplantation (Figure 1b) and with transplantation (Figure 1c; p > 0.05). The same occurred for the polymorphisms DBP-rs4588 (Figure 2a–c) and CYP24A1-rs6013897 (Figure 3a–c) (p > 0.05).
Table 1. Demographic profile, lifestyle and comorbidities in the TotalG of patients, patients with cirrhosis and HCC (G1), with isolated cirrhosis (G2) and individuals without the disease (G3).
Discussion
Among patients with or without HCC, smoking [27], alcoholism and DM [28] stood out, with a predominance of males [29]. Logistic regression analysis showed these factors as independent risk factors for cirrhosis with or without HCC [30], alcoholism and DM for both, and smoking, particularly in cirrhosis. In addition to cirrhosis with HCC, advanced age and male gender corroborated Mak et al’s [29] study. Viral hepatitis [31] and elevated serum creatinine [32] in patients with HCC were also observed in this study.
Admittedly, excessive alcohol intake increases inflammation and oxidative stress [31], causing liver tissue damage with the development of fibrosis, cirrhosis and HCC [33]. Studies show that alcoholism is associated with tobacco addiction, frequent in patients with both cirrhosis and HCC, acting together for the development of the disease, being a potential risk factor for causing DNA damage and thus responsible for hepatocarcinogenesis [31].
In this study, DM also stood out in patients. This metabolic disorder, which is a global public health problem, confers a risk for the development of NAFLD, cirrhosis and HCC [31]. In addition, type 2 DM implies insulin resistance and hyperinsulinemia, causing inflammation, cell proliferation, inhibition of apoptosis and mutation of tumour suppressor genes, which are also responsible for the development of cancer [34].
HWE was confirmed for all SNPs, corroborating the literature [35]. It was also found that LD for DBP-rs4588-DBP-rs7041, indicating non-random association or co-segregation of these SNPs, was also observed in a series with chronic hepatitis [36], as well as in Brazilian women with polycystic ovary syndrome [37]. The reconstruction of haplotypes for DBP showed a similarity between patients and controls, indicating no relationship with risk or protection for the disease, in agreement with a study conducted by Azevedo et al [38] in casuistry with chronic hepatitis C.
In this study, patients and controls showed similarity in the genotypic and allelic distribution of DBP-rs4588 and DBP-rs7041, as well as in other series [38]. On the other hand, there is a reference to the association of the mutant allele of DBP-rs7041 (G) with HCC [39] which, however, in this study provided increased survival in patients, with or without transplantation (general group), compared to those with wild genotype (T/T) in 11 years of follow-up, which did not occur when stratified into transplanted and non-transplanted ones. Yet, this polymorphism was associated with decreased survival in patients with lung cancer or kidney disease [40]. In this context, the various factors involved in the pathophysiology must also be considered, as well as the profile of the casuistry.
Table 2. Allelic and genotypic frequencies for the DBP (rs4588 and rs7041) and CYP24A1 (rs6013897) polymorphisms in the TotalG of patients, patients with cirrhosis and HCC (G1), patients with isolated cirrhosis (G2) and individuals without the disease (G3).
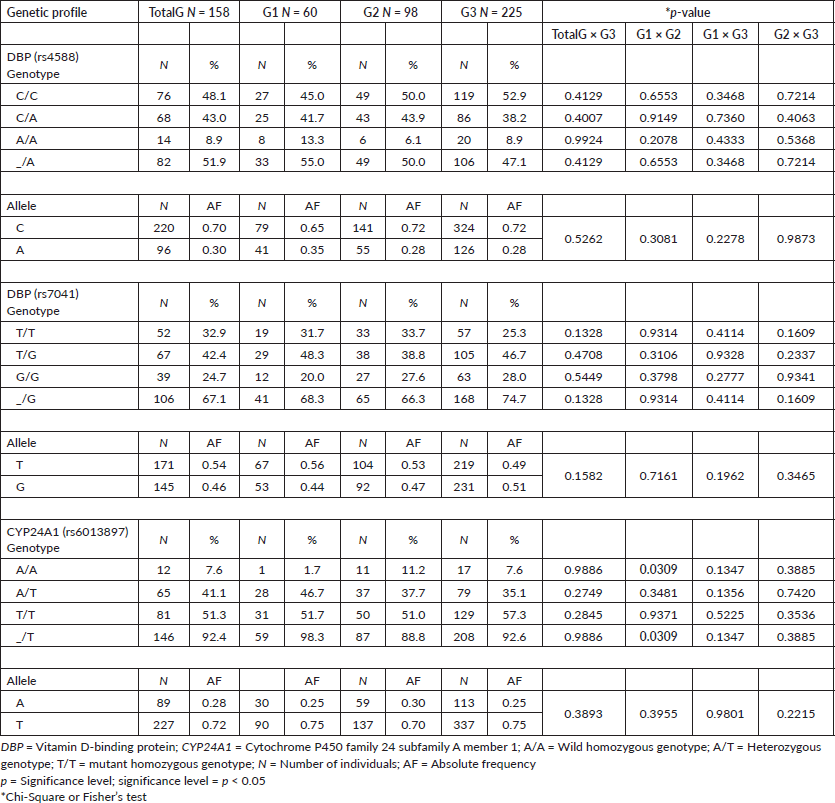
Table 3. Risk profile by logistic regression analysis in a TotalG of patients (TotalG = cirrhosis with or without HCC), with cirrhosis and HCC (G1), with isolated cirrhosis (G2) and subgroups with vitamin dosage D (TGd, G1d and G2d), compared to individuals without liver disease.
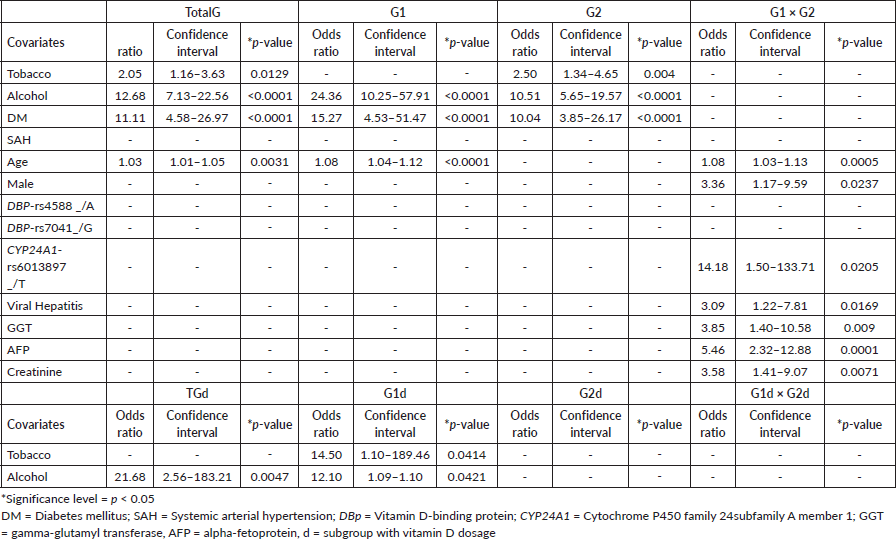
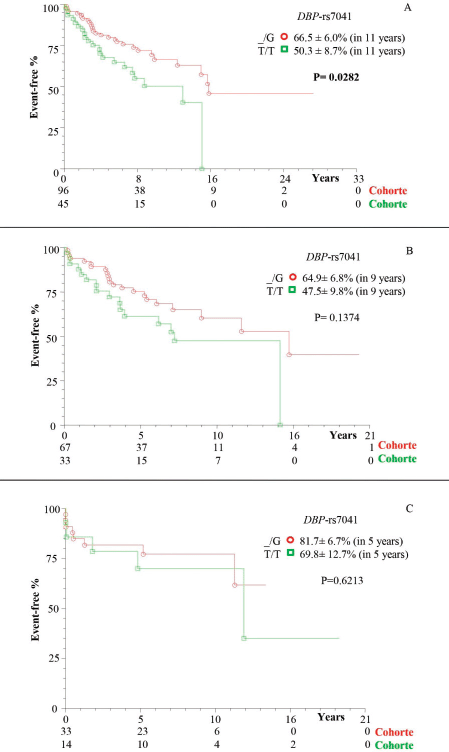
Figure 1. Kaplan–Meier actuarial curve for patients with cirrhosis with or without death event-free HCC, considering the DBP-rs7041 polymorphism. (a) TotalG of patients (with and without transplant); (b) patients without transplantation; and (c) transplant patients; carriers of genotypes with at least one polymorphic allele (_/G) compared to the wild homozygous genotype (T/T). DBP = Vitamin D-binding protein.
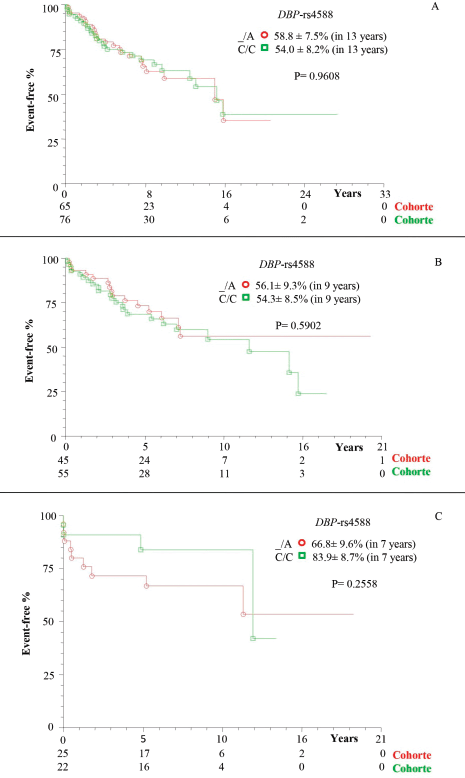
Figure 2. Kaplan–Meier actuarial curve for patients with cirrhosis with or without death event-free HCC, considering the DBP-rs4588 polymorphism. (a) TotalG of patients (with and without transplant); (b) patients without transplantation; and (c) transplant patients; carriers of genotypes with at least one polymorphic allele (_/A) compared to wild homozygous genotype (C/C). DBP = Vitamin D-binding protein.
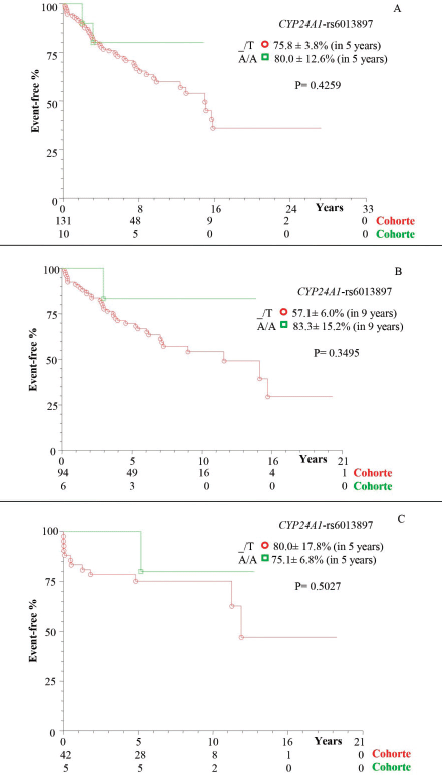
Figure 3. Kaplan–Meier actuarial curve for patients with cirrhosis with or without death event-free HCC, considering the CYP24A1-rs6013897 polymorphism. (a) TotalG of patients (with and without transplant); (b) patients without transplantation; and (c) transplant patients; carriers of genotypes with at least one polymorphic allele (_/T) compared to the wild homozygous genotype (A/A). CYP24A1= Cytochrome P450 family 24 subfamily A member.
The effect of genetic variants on the structure and activity of DBP stands out, influencing its affinity to vitamin D, as well as the concentration of 25(OH)D, as reported for the DBP polymorphisms rs7041 and rs458836. Incidentally, this study showed a higher frequency of reduced vitamin D levels in patients with cirrhosis with or without HCC carrying at least one mutant allele (_/A) for DBP-rs4588, compared to the control group, in agreement with Santos et al [37]. There is also a reference to the influence of the polymorphisms of DBP-rs7041 and DBP-rs4588 affecting the binding affinity of DBP with vitamin D, which could consequently influence its anti-tumorigenesis activity [41]. However, haplotype variations in different ethnicities may contribute to divergences between studies [39, 42].
In this study, CYP24A1-rs6013897 (_/T) polymorphism was also associated with cirrhosis and HCC, as an independent factor for the disease, while the wild homozygous genotype (A/A) prevailed in controls. There is reference to the association of the CYP24A1-rs6013897 polymorphism with colorectal cancer [43], in addition to inflammatory reactions, however, there are few studies on cirrhosis with or without HCC [21], thus highlighting the contribution of the present study.
In the logistic regression analysis, GGT was identified as an independent factor in the worsening of HCC. The GGT enzyme is a serum marker found in hepatic and biliary cells. Elevated serum levels are associated with an increased risk of developing liver, metabolic, cardiovascular and diabetes diseases [44]. Additionally, increased AFP values prevailed in patients with cirrhosis and HCC, compared to the group with cirrhosis, corroborating the literature [45], also presenting itself as an independent factor for the disease. Widely used in the diagnosis of liver cancer, AFP is considered an important serological marker. However, it is advisable to use this marker only as a preventive and non-diagnostic method for HCC [46], considering that high levels of AFP can also be found in chronic liver disease [45].
Regarding vitamin D, there was similarity between the groups; however, another casuistry showed an association of reduced levels of vitamin D with various types of cancer [47]. Furthermore, a cohort study showed vitamin D deficiency associated with advanced stages of the disease and mortality [48]. In the present study, approximately 30% of the patients and controls showed serum vitamin D levels <30 ng/mL. Nevertheless, it is reported that about two-thirds of patients with HCC present vitamin D deficiency, showing that serum levels are inversely correlated with the progression of liver diseases [49].
A Brazilian epidemiological study showed reduced levels of vitamin D in the southeast region of the country [50]. However, the Brazilian population of mixed ethnicity and the fluctuation of 25(OH)D3 levels during the seasons of the year must be considered [51]. In addition to that, the restricted number of patients for vitamin D analysis, although it did not prevent the statistical analysis of the data, was a limiting factor in this study.
The correlation analysis between vitamin D and PTH levels was also carried out, considering that even in situations of vitamin D deficiency, the active form [1,25(OH)2D] can present satisfactory levels under the mediation of PTH [52]. In this process, PTH acts on the bone to increase the influx of calcium and phosphate, with the purpose of increasing the synthesis of vitamin D, which, in turn, suppresses the production and secretion of PTH, ending the negative feedback cycle [53].
In this study, patients and controls showed similarity in PTH levels, corroborating a study in breast cancer [54]. On the other hand, vitamin D and PTH showed a moderate positive correlation only in patients, while in another casuistry [55], a negative correlation was observed, suggesting high PTH values in vitamin D deficiency and vice versa. In this context, it is noteworthy that genetic alterations in DBP, which actively participate in the vitamin D metabolic pathway, could influence its serum level, with compensatory PTH secretion in case of vitamin D deficiency [52], which may have occurred in the presence of DBP-rs4588 which in this series was associated with reduced levels of vitamin D.
Conclusion
In conclusion, the CYP24A1-rs6013897 polymorphism is associated with cirrhosis and HCC, standing out as a predictor of the disease, while the DBP-rs4588 polymorphism can influence in the reduction of vitamin D level in patients and, on the other hand, the variant DBP-rs7041 confers increased survival, suggesting a protective character. Age, alcoholism, DM, viral hepatitis and high levels of GGT, AFP and creatinine are also confirmed as predictors of both diseases, while smoking, alcoholism and DM are predictors of isolated cirrhosis.
Conflicts of interest
There are no conflicts of interest to declare.
Acknowledgments and funding
The authors thank all the collaborators of the Research Centre in Biochemistry and Molecular Biology-NPBIM; Prof Dr Moacir Fernandes de Godoy for his statistical assistance; the Post-Graduate Programme in Health Sciences of the Medical School of São José do Rio Preto-FAMERP for their technical and scientific support; and the Foundation for Research Support of the State of São Paulo (FAPESP) for their financial support in the execution of this research (Process: 2015/04338-1).
References
1. Institute for Health Metrics and Evaluation (IHME) (2018) GBD compare data visualization [http://vizhub.healthdata.org/gbd-compare] Date accessed: 14/2/19
2. Li J, Wang Y, and Ma M, et al (2019) Autocrine CTHRC1 activates hepatic stellate cells and promotes liver fibrosis by activating TGF-β signaling EBioMedicine 40 43–55 https://doi.org/10.1016/j.ebiom.2019.01.009 PMID: 30639416 PMCID: 6412555
3. Mihai F, Trifan A, and Stanciu C, et al (2020) Liver remodeling on CT examination in patients with HCV compensated cirrhosis who achieved sustained virological response after direct-acting antivirals treatment Medicina (Kaunas) 56 171 https://doi.org/10.3390/medicina56040171
4. Marcellin P and Kutala BK (2018) Liver diseases: a major, neglected global public health problem requiring urgent actions and large-scale screening Liver Int Suppl 1 2–6 https://doi.org/10.1111/liv.13682
5. Baitello MEL, Tenani GD, and Ferreira RF, et al (2016) VEGF polymorphisms related to higher serum levels of protein identify patients with hepatocellular carcinoma Can J Gastroenterol Hepatol 2016 1–9 https://doi.org/10.1155/2016/9607054
6. Fu Y, Liu S, and Zeng S, et al (2019) From bench to bed: the tumor immune microenvironment and current immunotherapeutic strategies for hepatocellular carcinoma J Exp Clin Cancer Res 38 396 https://doi.org/10.1186/s13046-019-1396-4 PMID: 31500650 PMCID: 6734524
7. Sung H, Ferlay J, and Siegel RL, et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries CA Cancer J Clin 71 209–249 https://doi.org/10.3322/caac.21660 PMID: 33538338
8. Yvamoto EY, Ferreira RF, and Nogueira V, et al (2015) Influence of vascular endothelial growth factor and alpha-fetoprotein on hepatocellular carcinoma Genet Mol Res 14 17453–17462 https://doi.org/10.4238/2015.December.21.16
9. Molin A, Baudoin R, and Kaufmann M, et al (2015) CYP24A1 mutations in a cohort of hypercalcemic patients: evidence for a recessive trait J Clin Endocrinol Metab 100 E1343–E1352 https://doi.org/10.1210/jc.2014-4387 PMID: 26214117
10. Allegra S, Cusato J, and De Francia S, et al (2018) Role of CYP24A1, VDR and GC gene polymorphisms on deferasirox pharmacokinetics and clinical outcomes Pharmacogenomics J 18 506–515 https://doi.org/10.1038/tpj.2017.43
11. Newton DA, Baatz JE, and Kindy MS, et al (2019) Vitamin D binding protein polymorphisms significantly impact vitamin D status in children Pediatr Res 86 662–669 https://doi.org/10.1038/s41390-019-0322-y PMID: 30712059 PMCID: 6677641
12. Cappellani D, Brancatella A, and Kaufmann M, et al (2019) Hereditary hypercalcemia caused by a homozygous pathogenic variant in the CYP24A1 gene: a case report and review of the literature Case Rep Endocrinol 2019 4982621 PMCID: 6476011
13. Jorde R (2019) The role of vitamin D binding protein, total and free 25-hydroxyvitamin D in diabetes Front Endocrinol (Lausanne) 10 79 https://doi.org/10.3389/fendo.2019.00079
14. Wang M, Zhang R, and Wang M, et al (2021) Genetic polymorphism of vitamin D family genes CYP2R1, CYP24A1, and CYP27B1 are associated with a high risk of non-alcoholic fatty liver disease: a case-control study Front Genet 12 717533 https://doi.org/10.3389/fgene.2021.717533 PMCID: 8415785
15. Petta S, Cammà C, and Scazzone C, et al (2010) Low vitamin D serum level is related to severe fibrosis and low responsiveness to interferon-based therapy in genotype 1 chronic hepatitis C Hepatology 51 1158–1167 https://doi.org/10.1002/hep.23489 PMID: 20162613
16. Fan HZ, Zhang R, and Tian T, et al (2019) CYP24A1 genetic variants in the vitamin D metabolic pathway are involved in the outcomes of hepatitis C virus infection among high-risk Chinese population Int J Infect Dis 84 80–88 https://doi.org/10.1016/j.ijid.2019.04.032 PMID: 31075507
17. Xiong Q, Jiao Y, and Yang P, et al (2020) The association study between CYP24A1 gene polymorphisms and risk of liver, lung and gastric cancer in a Chinese population Pathol Res Pract 216 153237 https://doi.org/10.1016/j.prp.2020.153237 PMID: 33065483
18. Meyer MB and Pike JW (2020) Mechanistic homeostasis of vitamin D metabolism in the kidney through reciprocal modulation of CYP27B1 and CYP24A1 expression J Steroid Biochem Mol Biol 196 105500 https://doi.org/10.1016/j.jsbmb.2019.105500 PMCID: 6954286
19. Negri M, Gentile A, and de Angelis C, et al (2020) Vitamin D-induced molecular mechanisms to potentiate cancer therapy and to reverse drug-resistance in cancer cells Nutrients 12 1798 https://doi.org/10.3390/nu12061798 PMCID: 7353389
20. Han J, Tang Y, and Zhong M, et al (2019) Antitumor effects and mechanisms of 1,25(OH)2D3 in the Pfeiffer diffuse large B lymphoma cell line Mol Med Rep 20 5064–5074 PMID: 31638226 PMCID: 6854594
21. Wang Y, Wang O, and Li W, et al (2015) Variants in vitamin D binding protein gene are associated with gestational diabetes mellitus Medicine (Baltimore) 94 e1693 https://doi.org/10.1097/MD.0000000000001693 PMCID: 4616752
22. Bruix J, Sherman M, and American Association for the Study of Liver Diseases (2011) Management of hepatocellular carcinoma: an update Hepatology 53 1020–1022 https://doi.org/10.1002/hep.24199 PMID: 21374666 PMCID: 3084991
23. Peng Y, Qi X, and Guo X (2016) Child-Pugh versus MELD score for the assessment of prognosis in liver cirrhosis: a systematic review and meta-analysis of observational studies Medicine (Baltimore) 95 e2877 https://doi.org/10.1097/MD.0000000000002877
24. Holick MF (2018) The death D-fying vitamin Mayo Clin Proc 93 679–681 https://doi.org/10.1016/j.mayocp.2018.04.014 PMID: 29866279
25. Rivelli GG, Lima ML, and Mazzali M (2020) Therapy for persistent hypercalcemic hyperparathyroidism post-renal transplant: cinacalcet versus parathyroidectomy Braz J Nephrol 42 315–322 https://doi.org/10.1590/2175-8239-jbn-2019-0207
26. Salazar LA, Hirata MH, and Cavali SA, et al (1998) Optimized procedure for DNA isolation from fresh and cryopreserved clotted human blood useful in clinical molecular testing Clin Chem 44 1748–1750 https://doi.org/10.1093/clinchem/44.8.1748 PMID: 9702967
27. Bajaj JS, Garcia-Tsao G, and Biggins SW, et al (2021) Comparison of mortality risk in patients with cirrhosis and COVID-19 compared with patients with cirrhosis alone and COVID-19 alone: multicentre matched cohort Gut 70 531–536 https://doi.org/10.1136/gutjnl-2020-322118
28. Vaz J, Eriksson B, and Strömberg U, et al (2020) Incidence, aetiology and related comorbidities of cirrhosis: a Swedish population-based cohort study BMC Gastroenterol 20 84 https://doi.org/10.1186/s12876-020-01239-6 PMID: 32245414 PMCID: 7118963
29. Mak LY, Cruz-Ramon V, and Chinchilla-Lopez P, et al (2018) Global epidemiology, prevention, and management of hepatocellular carcinoma Am Soc Clin Oncol Educ Book 38 262–279 https://doi.org/10.1200/EDBK_200939 PMID: 30231359
30. Sánchez-Jimenez BA, Brizuela-Alcantara D, and Ramos-Ostos MH, et al (2018) Both alcoholic and non-alcoholic steatohepatitis association with cardiovascular risk and liver fibrosis Alcohol 69 63–67 https://doi.org/10.1016/j.alcohol.2017.11.004 PMID: 29660603
31. Tunissiolli NM, Castanhole-Nunes MMU, and Biselli-Chicote PM, et al (2017) Hepatocellular carcinoma: a comprehensive review of biomarkers, clinical aspects, and therapy Asian Pac J Cancer Prev 18 863–872 PMID: 28545181 PMCID: 5494234
32. ElGhandour AM, Bayoumy EM, and Ibrahim WA, et al (2021) Vascular endothelial growth factor in relation to the development of hepatocellular carcinoma in hepatitis C virus patients treated by direct-acting antivirals Egypt Liver J 11 5 https://doi.org/10.1186/s43066-020-00073-5
33. Nguyen-Khac E, Thiele M, and Voican C, et al (2018) Non-invasive diagnosis of liver fibrosis in patients with alcohol-related liver disease by transient elastography: an individual patient data meta-analysis Lancet Gastroenterol Hepatol 3 614–625 https://doi.org/10.1016/S2468-1253(18)30124-9 PMID: 29983372
34. Hassan K, Bhalla V, and Ezz El, et al (2015) Nonalcoholic fatty liver disease: a comprehensive review of a growing epidemic WJG 20 12082–12101 https://doi.org/10.3748/wjg.v20.i34.12082
35. Trummer O, Schweighofer N, and Haudum CW, et al (2020) Genetic components of 25-hydroxyvitamin D increase in three randomized controlled trials J Clin Med 9 570 https://doi.org/10.3390/jcm9020570 PMCID: 7074051
36. Mateos-Muños B, Garcia-Martín E, and Torrejón MJ, et al (2016) GC gene polymorphism and unbound serum retinol-binding protein 4 are related to the risk of insulin resistance in patients with chronic hepatitis C: a prospective cross-sectional study Medicine (Baltimore) 95 e3019 https://doi.org/10.1097/MD.0000000000003019
37. Santos BR, Lecke SB, and Spritzer PM (2017) Genetic variant in vitamin D-binding protein is associated with metabolic syndrome and lower 25-hydroxyvitamin D levels in polycystic ovary syndrome: a cross-sectional study PLoS One 12 e0173695 https://doi.org/10.1371/journal.pone.0173695 PMID: 28278285 PMCID: 5344505
38. Azevedo LA, Matte U, and Silveira TR, et al (2017) Effect of vitamin D serum levels and GC gene polymorphisms in liver fibrosis due to chronic hepatitis C Ann Hepatol 16 742–748 https://doi.org/10.5604/01.3001.0010.2748 PMID: 28809744
39. Peng Q, Yang S, and Lao X, et al (2014) Association of single nucleotide polymorphisms in VDR and DBP genes with HBV-related hepatocellular carcinoma risk in a Chinese population PLoS One 9 e116026 https://doi.org/10.1371/journal.pone.0116026 PMID: 25541958 PMCID: 4277456
40. Grzegorzewska AE, Świderska MK, and Mostowska A, et al (2016) Polymorphisms of vitamin D signaling pathway genes and calcium-sensing receptor gene in respect to survival of hemodialysis patients: a prospective observational study Int J Endocrinol 2016 2383216 https://doi.org/10.1155/2016/2383216 PMID: 27642296 PMCID: 5011523
41. Niforou A, Konstantinidou V, and Naska A (2020) Genetic variants shaping inter-individual differences in response to dietary intakes – a narrative review of the case of vitamins Front Nutr 7 558598 https://doi.org/10.3389/fnut.2020.558598
42. Ying HQ, Sun HL, and He BS, et al (2015) Circulating vitamin D binding protein, total, free and bioavailable 25-hydroxyvitamin D and risk of colorectal cancer Sci Rep 5 7956 https://doi.org/10.1038/srep07956 PMID: 25609140 PMCID: 4302314
43. Vidigal VM, Silva TD, and de Oliveira J, et al (2017) Genetic polymorphisms of vitamin D receptor (VDR), CYP27B1 and CYP24A1 genes and the risk of colorectal cancer Int J Biol Markers 32 e224–e230 https://doi.org/10.5301/jbm.5000248
44. Praetorius Bjork M and Johansson B (2018) Gamma-glutamyltransferase (GGT) as a biomarker of cognitive decline at the end of life: contrasting age and time to death trajectories Int Psychogeriatr 30 981–990 https://doi.org/10.1017/S1041610217002393
45. Yang JG, He XF, and Huang B, et al (2018) Rule of changes in serum GGT levels and GGT/ALT and AST/ALT ratios in primary hepatic carcinoma patients with different AFP levels Cancer Biomark 21 743–746 https://doi.org/10.3233/CBM-170088
46. Piñero F, Dirchwolf M, and Pessôa MG (2020) Biomarkers in hepatocellular carcinoma: diagnosis, prognosis and treatment response assessment Cells 9 1370 https://doi.org/10.3390/cells9061370 PMCID: 7349517
47. Calmarza P, Sanz Paris A, and Prieto Lopez C, et al (2018) Vitamin D levels in patients with recent cancer diagnosis Nutr Hosp 35 903–908 PMID: 30070880
48. Finkelmeier F, Kronenberger B, and Koberle V, et al (2014) Severe 25-hydroxyvitamin D deficiency identifies a poor prognosis in patients with hepatocellular carcinoma – a prospective cohort study Aliment Pharmacol Ther 39 1204–1212 https://doi.org/10.1111/apt.12731 PMID: 24684435
49. Zhao XY, Li J, and Wang JH, et al (2016) Vitamin D serum level is associated with Child-Pugh score and metabolic enzyme imbalances, but not viral load in chronic hepatitis B patients Medicine (Baltimore) 95 e3926 https://doi.org/10.1097/MD.0000000000003926
50. Pereira-Santos M, Santos J, and Carvalho GQ, et al (2019) Epidemiology of vitamin D insufficiency and deficiency in a population in a sunny country: geospatial meta-analysis in Brazil Crit Rev Food Sci Nutr 59 2102–2109 https://doi.org/10.1080/10408398.2018.1437711
51. Pena SDJ (2005) Dossiê raça, genética, identidades e saúde: Razões para banir o conceito de raça da medicina brasileira Hist Ciênc Saúde Manguinhos 12 321–346 https://doi.org/10.1590/S0104-59702005000200006
52. Castro LC (2011) The vitamin D endocrine system Arq Bras Endocrinol Metabol 55 566–575 https://doi.org/10.1590/S0004-27302011000800010
53. John GB, Cheng CY, and Kuro-o M (2011) Role of Klotho in aging, phosphate metabolism, and CKD Am J Kidney Dis 58 127–134 https://doi.org/10.1053/j.ajkd.2010.12.027 PMID: 21496980 PMCID: 3191324
54. Almquist M, Bondeson AG, and Bondeson L, et al (2010) Serum levels of vitamin D, PTH and calcium and breast cancer risk-a prospective nested case-control study Int J Cancer 127 2159–2168 https://doi.org/10.1002/ijc.25215 PMID: 20112341
55. Martins JS, Palhares MO, and Teixeira COM, et al (2017) Vitamin D status and its association with parathyroid hormone concentration in Brazilians J Nutr Metabol 28 1–5 https://doi.org/10.1155/2017/9056470






