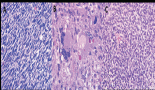
Usual vulvar intraepithelial neoplasia (uVIN) is the most common VIN type, generally related to a human papillomavirus (HPV) infection, predominantly type 16. The incidence of uVIN has been increasing over the last decades, and a bimodal peak is observed at the age of 40–44 and over 55 years.
Almost 40% of patients with uVIN have a past, concomitant or future HPV-associated lesion of the lower genital tract. HPV-related malignancies are associated with a persistent HPV infection. The host immune response is of crucial importance in determining clearance or persistence of both HPV infections and HPV-related VIN. About 60% of the patients present with symptoms. Clinical features of uVIN vary in site, number, size, shape, colour, and thickness of lesions. Multicentric disease is often present.
Most uVIN lesions are positive at immunohistochemistry to p16ink4a and p14arf, but negative to p53.
Irrespective of surgical treatment used, uVIN recurrence rates are high. Positive margins do not predict the development of invasive disease and the need to re-excide the tissue around the scare remains to be demonstrated. Therefore, considering the low progression rate of uVIN and psycosexual sequelae, treatments should be as conservative as possible.
Medical treatments available are mainly based on immunotherapy to induce normalisation of immune cell count in uVIN. None are approved by the food and drug administration (FDA) for the treatment of uVIN. If medical treatment is performed, adequate biopsies are required to reduce the risk of unrecognised invasive disease. Some studies suggest that failure to respond to immunotherapy might be related to a local immunosuppressive microenvironment, but knowledge of the uVIN microenvironment is limited. Moreover, our knowledge of the potential mechanisms involved in the escape of HPV-induced lesions from the immune system has many gaps.
HPV vaccines have been demonstrated to be effective in preventing uVIN, with 94.9% efficacy in the HPV-naive population, while studies on therapeutic vaccines are limited. The low incidence of VIN requires large multicentre studies to determine the best way to manage affected patients and to investigate the immunological characteristics of the ‘vulvar microenviroment’ which leads to the persistence of HPV.