Assessment of barriers to optimal cancer control in adult cancer treatment centres in Cameroon
Berthe Sabine Esson Mapoko1, Andreas Frambo2, Yauba Saidu2,3, Esther Dina Bell Mbassi4, Etienne Atenguena1, Kareen Azemafac1, Emily Kobayashi2, Lionel Tabola1, Glenda Nkeng1, Anne Sango5, Anne Marthe Maison4, Sidonie Ananga Noa4, Ambroise Ntama4, Ruth Rosine Meka’h Mapenya1, Rachel Tayou6, Francine Kouya7, Glenn Mbah7,8, Pelagie Douanla1, Celestin Fonkwa9, Martin Essomba Biwole4, Zacharie Sando1, Albert Mouelle Sone4 and Paul Ndom1
1Faculty of Medicine and Biomedical Sciences, University of Yaoundé I, Yaoundé 99322, Cameroon
2Clinton Health Access Initiative, Yaoundé 99322, Cameroon
3Institute for Global Health, University of Siena, Siena 53100, Italy
4Faculty of Medicine and Pharmaceutical Sciences, University of Douala, Douala 99322, Cameroon
5Faculty of Health Sciences, University of Buea, Buea 99322, Cameroon
6Faculty of Health Sciences, University of Dschang, Dschang 99322, Cameroon
7Mbingo Baptist Hospital, Bamenda 99322, Cameroon
8Faculty of Health Sciences, University of Bamenda, Bamenda 99322, Cameroon
9Laquintinie Hospital oF Douala, Douala 99322, Cameroon
Abstract
Approximately 20,745 new cases of cancer were registered annually with 13,199 (64%) deaths in 2020 in Cameroon. Despite the increasing cancer burden, there is a paucity of reliable data that can enhance decision-making for cancer control in Cameroon. This assessment was, therefore, designed to generate data that may enable stakeholders, policymakers and funders to make data-driven decisions on cancer control. We conducted a cross-sectional survey in July 2020, which enabled us to collect data on key cancer variables from six adult cancer treatment centres in Cameroon. The key components of the assessment included case detection, service availability, human resource capacity, cost of chemotherapy and radiotherapy, the safety of chemotherapy sessions, data systems, patient education, palliative care, funding for chemotherapy and chemotherapy stock. Data were compiled and analysed using Microsoft Excel 2016. Data from four of the 6 sites show that 1,636 new cases were recorded representing an annual case detection rate of 11.8%. All the six assessed facilities offered chemotherapy services, 5/6 (83.3%) offered surgery for cancers, while just 1 (16.7%) offered radiotherapy services. In addition, none offered nuclear medicine services for cancer care and treatment. Similarly, none of the facilities had the WHO-recommended number of human resources for optimal cancer care. Overall, there were only 6 medical oncologists, 2 surgical oncologists, 3 radiation oncologists and 14 oncology nurses providing services across the 6 cancer treatment centres. Treatment services are expensive for an average national, with a complete course of chemotherapy followed by radiotherapy costing ~XAF 1,240,000 (~$2,480). None of the survey facilities had a recommended safe biosafety cabinet and clean room for the preparation of chemotherapies, rendering the preparation of chemotherapies suboptimal and hazardous. Data collection tools were manual, relatively available and very different across all the surveyed sites and the interval for data collection and transmission was collectively undefined. Optimal cancer care in adult cancer treatment centres is limited by several health systems and socio-economic factors. The identification of these barriers has enabled the formulation of action-oriented interventions, leveraging on the recently adopted national strategy for the prevention and control of cancers in the country.
Keywords: assessment, barriers, cancer control, Cameroon
Correspondence to: Berthe Sabine Esson Mapoko
Email: mapokob@yahoo.fr
Published: 21/09/2023
Received: 26/11/2022
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Cameroon, like most resource-challenged countries, is experiencing a significant increase in cancer-related morbidity and mortality. According to estimates from the World Health Organisation, International Agency on Research in Cancer, over 20,745 new cases of cancer and approximately 13,199 (67.95%) cancer-related deaths occurred in 2020 [1]. The burden appears to be particularly high in women. For instance, in 2020, nearly 60% of 20,745 new cases were recorded in women [1]. In both sexes, the top five cancers are breast, cervix uteri, prostate, non-Hodgkin lymphoma and Kaposi sarcoma [1].
In response to this cancer situation, the Government of the Republic of Cameroon, through its Ministry of Public Health, was created in 1990 and later re-organised in 2002, a National Committee for the Fight Against Cancer (NACFAC) [2]. In 2019, NACFAC developed a 5-year national strategic plan to reduce cancer-related morbidity and mortality by 2024, by 10%, and attenuating its socio-economic impact on the development of the country. Progress towards attaining this goal has been slow, because of several factors including limited access to affordable cancer medication, scarcity of cancer specialists, dilapidated infrastructure, outdated platforms, high treatment discontinuation rates and underfunding of interventions amongst others [2]. To date, limited efforts have been invested to explore the barriers to holistic and optimal cancer care in the country. This study was, therefore, designed to investigate the key obstacles to accessing optimal cancer care in the functional oncology services in Cameroon. Specifically, we sort to describe cancer care and treatment capacity across six approved treatment sites; evaluate human resource capacity involved in the management of cancers; identify potential factors affecting access to cancer care and treatment with a focus on chemotherapy, radiotherapy and surgery; evaluate existing patient follow-up systems, including patient education and palliative care; describe existing cancer data collection and reporting systems and to understand the funding landscape for chemotherapy.
Methods
We conducted a cross-sectional study in July 2020 in the six adult cancer treatment centres of Cameroon. These were Yaoundé General Hospital (YGH), Yaoundé Central Hospital (YCH), Douala General Hospital (DGH), Douala Laquintinie Hospital (DLH), Bonassama District Hospital (BDH) in Douala and Mbingo Baptist Hospital (MBH) in Bamenda.
In collaboration with key stakeholders, we designed, pre-tested and validated a structured questionnaire (see Supplementary Data) that captured data on various aspects of cancer treatment in the study sites. The questionnaire had seven sections. The first section captured health facility information, including the address, the type of facility, the category of the facility and the bed capacity amongst others. The second section captured information on the number of health staff available as well as the proportion of staff that have been capacitated on oncology. The third and fourth sections covered information relating to accessing cancer care and treatment with a focus on chemotherapy, surgery, radiotherapy and nuclear medicine. The fifth section essentially focused on the follow-up of cancer patients including preparation and administration of chemotherapy sessions, patient education, tracking patients on chemotherapy and palliative care amongst others. The sixth section captured information on data systems for cancers and finally, the seventh section focused on stock management for chemotherapy.
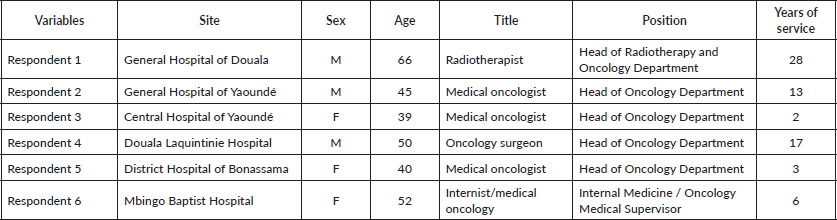
The tool was reviewed and approved during a joint meeting, which brought together various stakeholders, including the United Nations International Children's Emergency Fund, the International Atomic Energy Agency (IAEA), the NACFAC and the Clinton Health Access Initiative (CHAI). Following this approval, the study team under the leadership of the cancer programme, proceeded to collect data from six adult cancer treatment centres in Cameroon. The data were collected by visiting the sites, interviewing a focal point of the staff and consulting registers. We then entered the collected data into a pre-established database and subsequently analysed it using Microsoft Excel. Table 1 presents the characteristics of the responders in the different centres.
Table 1. Characteristics of the respondents.
Results
Overall, we surveyed one private faith-based hospital and five state-owned hospitals. In these centres, we sought to assess the availability and provision of various cancer care and treatment services, including chemotherapy, radiotherapy, nuclear medicine, surgery and palliative care.
Cancer service availability
Table 1 shows the cancer care services that were provided at the study sites during the time of the study. As can be seen, all six surveyed facilities offered adult chemotherapy services and palliative care. Surgery was offered by five of the six hospitals, while radiotherapy was offered by just one hospital. No nuclear medicine service is available (Table 2).
In adults, 1,636 new cases were diagnosed annually across four treatment sites, representing about 11.8% (1,636/13,830) of adult cancer case detection.
Human resource capacity
Six medical oncologists, 2 surgical oncologists, 3 radiation oncologists and 14 oncology nurses were the trained human resource providing services across the 6 cancer treatment centres (Table 2). About 85% (143/168) of staff working in cancer treatment centres have not received prior training in cancer care (Table 3).
Table 2. Cancer service availability.
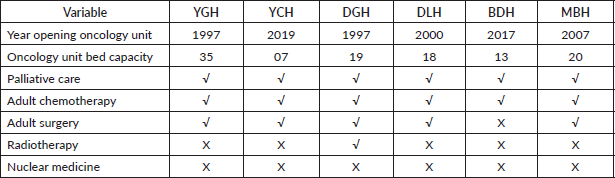
Table 3. Distribution of human resources for cancer care and treatment.
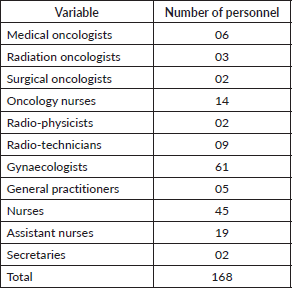
Table 4. Average cost of complete curative cancer treatment.
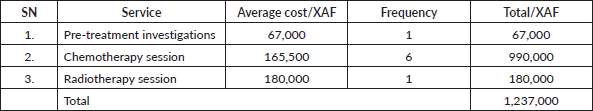
Access to cancer treatment
Chemotherapy services require about XAF 67,000 (~$134) for pre-treatment investigations prior to starting chemotherapy. The average cost of one cycle of chemotherapy is XAF 165,500 (~$331) and six cycles of chemotherapy is averagely required for a complete curative cancer treatment. A full course of radiotherapy costs XAF 180,000 (~$316). This figure reduces when treatment is palliative. Complete chemotherapy followed by radiotherapy will cost ~XAF 1,240,000 (~$2,480) as illustrated in Table 4. In addition to this cost, which is paid out of pocket, patients will also cover transport, accommodation and meals amongst others.
Safety of chemotherapy sessions
Chemotherapy sessions are essentially prepared by nurses, and pharmacy technicians when available. These staff have received on-the-job training for chemotherapy preparation and administration and they basically work on average 2–5 days per week and then change shifts. Personal protective equipment (PPE) for chemotherapy sessions seems to be lacking as only three hospitals (43%) had all the essential PPEs in use. The spaces allocated for the preparation of chemotherapy sessions are inadequate.
Chemotherapy stock
All the six surveyed hospitals had a pharmacy where they could stock anticancer medicines. However, only four of the six surveyed sites had dedicated personnel who oversee chemotherapy stock. Overall, the sources of chemotherapy stock were pharmaceutical companies (43%), the National Drug Procurement Agency (CENAME) (29%) and private pharmacies (14%). The MBH procures through the CBCHS Central Pharmacy from abroad and other local private wholesalers. Only three of the six surveyed hospitals provided information on the current chemotherapy stock. Amongst them, two were entirely stocked out. Only two of the assessed hospitals had visibility on the quantity of procured versus used stock for 2019. Overall, the quantities procured were lesser than the quantities used. With stockouts in these hospitals, patients procure from private pharmacies where prices are significantly higher.
Patient education
Disclosure of cancer status to patients is essentially done by the already overburdened oncologists and a few other medical specialists for adults. Flyers, posters and health talks are the main education and sensitisation materials. Patient follow-up is mainly with hospital registers and sometimes patient records.
Palliative care
Palliative care services are available. Morphine (rarely available), dexamethasone, metoclopramide and diazepam are the main palliative medicines given to patients.
Data systems
Data collection tools were manual, relatively available, and very different across all the surveyed sites. The interval for data collection was collectively undefined. Data reporting was infrequent as three sites (50%, (3/6)) reported data only when necessary.
Funding for chemotherapy
Funding for chemotherapy procurement was provided by the state (22%), hospital-generated funds (33%) and non-governmental organisation like Max Foundation, Bayonne Hospital and Chemotherapy Solidarity (44%). None of the surveyed hospitals provided verifiable data on the amount spent on chemotherapy procurement. In one hospital, an anecdotal estimate of XAF 4,900,000 (~USD 8,604) was used to purchase anticancer medicines for a year. In the other hospitals, the data were either non-existent or unknown.
Discussion
The purpose of this study was to provide a detailed outline of the status quo of cancer care and treatment in the six approved adult cancer care and treatment centres in Cameroon. The goal was to provide stakeholders, policymakers and funders with information that can enable them to understand the main factors affecting access to cancer care and treatment as this may galvanise the design and implementation of evidence-based interventions. Overall, we found that optimal cancer care and treatment in Cameroon is marred with several limitations, including inadequate adult chemotherapy, radiation therapy and nuclear medicine services. These findings are in line with those reported by Vanderpuye et al [3] and Stefan [4], who observed that resources allocated to cancer care and treatment services are inadequate, a challenge that will only continue to increase premature deaths from cancers [5]. Our findings suggest that urgent actions are needed to improve access to cancer care and treatment services in Cameroon. In the short to medium term, this need should focus on redressing access challenges to chemotherapy and radiotherapy in the six hospitals while in the long term, focus should be directed towards expanding chemotherapy and radiotherapy services to other regions of the country.
We also found that cancer care and treatment centres lacked the necessary human resource capacity for optimal cancer treatment and survival. For instance, only 6 medical oncologists, 3 radiation oncologists, 2 surgical oncologists and 14 oncology nurses were available across all 6 treatment centres in the country. The IAEA recommends training radiation/clinical oncologists who can prescribe both radiation and chemotherapy for common solid cancers and that the number of specialists needed should be based on the number of cancer patients [6]. The agency also recommends that to ensure proper coverage, each treatment centre should have at least two surgical oncologists, two radiation/clinical oncologists, two haematologist oncologists, etc. [6]. This was not the case in all the surveyed hospitals. Worst still, nearly 85% of staff working in the surveyed cancer treatment centres have not received prior training on cancer care. These limitations highlight the need for strengthening health resource capacity for cancer control through targeted interventions to immediately strengthen the skills of the existing health resource workforce in the short to medium term. Setting up a mechanism to increase the existing pool of oncologists (doctors and nurses) will be needed to curb the human resource challenges in the long run. As a result, deliberate investment by governments would be critical to ensure the availability of a trained and competent workforce to redress premature deaths resulting from cancer [5].
We also found that the cost of chemotherapy is largely beyond the financial capacity of the majority of the population, including 37.5% of the ones who are already living below the poverty threshold of XAF 931 (~$1.8) per day [7]. Indeed, our data show that a patient will have to spend an average of XAF 67,000 (~$134) for pre-treatment investigations, XAF 990,000 ($1980) for six-cycle chemotherapy course. In addition, where indicated, a patient will need to spend XAF 180,000 (~$316) for a complete radiotherapy session. Indeed, nationals that are living below the poverty line will need to save all on their monthly income of approximately XAF 28,309 (~$49) for over six months to be able to raise the amount needed for radiotherapy alone [7]. Given this financial challenge, the majority of people suffering from cancer requiring a curative chemotherapy followed by radiotherapy are likely to abandon treatment due to cost [8]. As such, rendering chemotherapy (pre-treatment investigations, hospital stay and medicines) and radiotherapy affordable may significantly improve access, thereby impacting survival rates after cancer treatment [9]. This may go a long way to prevent patients from abandoning treatment [5] or driving their families into dire poverty [10, 11]. Indeed, cost is one of the major reasons why many patients abandon their treatments in Africa as patients frequently must pay out of pocket to access care, incurring expenses that can be financially high [3, 5, 10, 11].
Patient education remains one of the critical components for achieving better survival rates with cancer treatment [12]. There is absolute need for building the capacity of healthcare workers, community workers and most importantly, the caregivers, on key elements for improving survival including disclosure of cancer status [13, 14]. Furthermore, conducting awareness and sensitisation interventions will indirectly improve patient education and facilitate adherence to cancer treatment [15].
Palliative care services are available for cancer and other diseases. However, very few drugs are being used for this purpose and these aren’t readily available. A substantial number of cancer patients are in need of palliative care seeing the late stage at which most cancers are being diagnosed in Cameroon. Studies have shown that over 80% of people in urgent need of palliative care live in low- and middle-income countries where basic health care is less well developed [16]. Palliative care service is generally not limited to what we found in this study such as the administration of palliative drugs. Hence, there are proposals on increasing the palliative health care package in the country [17–20].
Data systems for capturing and reporting information relating to cancer care and treatment are unstructured and embryonic. Indeed, there is a need for an overhaul of the existing data-capturing system to embrace harmonised and user-friendly tools including basic registers and monthly reporting forms for the short and medium term. Setting up a cancer registry at regional levels will facilitate the availability and synthesis of key indicators to enable decision-making in the long term [21]. The International Agency for Research on Cancer insisted on the fact that the unique value of cancer registry data is manifested in its contribution to decision-making in cancer control [22]. However, few countries in Africa have adequate cancer registries in place [22]. It was therefore recommended that funding new cancer registries and improving the quality of existing ones should be considered a high priority on the agenda of African health policy-makers, Cameroon inclusive [23]. Patient tracking mechanisms were weak suggesting the need to institute robust patient tracking mechanisms to monitor treatment progress and measure dropout rates [15].
Access to adequate financial resources appears to be the major barrier to the implementation of optimal cancer control interventions. Indeed, most surveyed facilities lack ready funds to secure resources for basic cancer services including chemotherapy. Consequently, it is not uncommon for these facilities to entirely rely on stakeholders to support the availability of chemotherapy medicines [24].
Conclusion
The findings of the survey have enabled the identification of gaps in cancer control. The above findings suggest that to sustainably improve access to cancer care and treatment, a wide range of interventions targeting the major arms of cancer care and treatment will be required. The Government of Cameroon has demonstrated good political will in this line and has translated the recommendations into actionable interventions for implementation. This report complements the 5-year national strategic plan for prevention and cancer response and enhances the endeavour of the Ministry of Health.
Conflicts of interest
AF, YS and EK work at CHAI which funds the current study. EDBM works at Laboratoire ROCHE as part of its ACCESS CANCER programme in Cameroon. However, Laboratoire ROCHE is neither closely nor remotely involved in the conception, writing or financing of this research work. The other authors do not have any conflicts of interest.
Funding
This study was financed by the UBS Foundation through the CHAI.
Author contributions
Conception and design: YS, AF, EK, BSEM, and NP.
Data collect: BSEM.
Data analysis and interpretation: AF, BSEM, and KA.
Manuscript writing: BSEM, AF, KA, TL, and GN.
Manuscript revision: BSEM, AF, YS, EK, EDBM, KA, TL, EA, AJFS, AMMM, SAN, RT, RRMM, AN, PD, FK, GM, CF, MEB, AMS, ZS, and PN.
All the authors approved the final version of the manuscript.
References
1. Sung H, Ferlay J, and Siegel RL, et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries CA Cancer J Clin 71(3) 209–249 https://doi.org/10.3322/caac.21660 PMID: 33538338
2. National Strategic Plan for Prevention and Cancer Control [Internet] [https://www.iccp-portal.org/system/files/plans/FINAL%20COPY%20OF%20PSNPLCa%20ENGLISH.pdf] Date accessed: 23/09/22
3. Vanderpuye V, Hammad N, and Martei Y, et al (2019) Cancer care workforce in Africa: perspectives from a global survey Infect Agents Cancer 14(1) 11 https://doi.org/10.1186/s13027-019-0227-8
4. Stefan DC (2015) Cancer care in Africa: an overview of resources JGO 1(1) 30–36 https://doi.org/10.1200/JGO.2015.000406
5. WHO | Regional Office for Africa (2022) Where does cancer care stand in Africa today? [Internet] [https://www.afro.who.int/news/where-does-cancer-care-stand-africa-today] Date accessed: 27/08/22
6. Human Resources for Treating New Cancer Cases in Cameroon [Internet] [https://rrp.cancer.gov/programsResources/lowIncome/cameroon.pdf] Date accessed: 22/09/22
7. CAMEROUN – Quatrième Enquête Camerounaise Auprès des Ménages (2014) [Internet] [http://slmp-550-104.slc.westdc.net/~stat54/nada/index.php/catalog/114] Date accessed: 23/09/22
8. Kingham TP, Alatise OI, and Vanderpuye V, et al (2013) Treatment of cancer in sub-Saharan Africa Lancet Oncol 14(4) e158–e167 https://doi.org/10.1016/S1470-2045(12)70472-2 PMID: 23561747
9. Gorey KM, Luginaah IN, and Bartfay E, et al (2011) Effects of socioeconomic status on colon cancer treatment accessibility and survival in Toronto, Ontario, and San Francisco, California, 1996–2006 Am J Public Health 101 112–119 [Internet] Date accessed: 06/10/22 https://doi.org/10.2105/AJPH.2009.173112
10. Iragorri N, de Oliveira C, and Fitzgerald N, et al (2021) The out-of-pocket cost burden of cancer care – a systematic literature review Curr Oncol 28(2) 1216–1248 https://doi.org/10.3390/curroncol28020117 PMID: 33804288 PMCID: 8025828
11. Ogunbiyi JO, Stefan DC, and Rebbeck TR (2016) African Organization for Research and Training in cancer: position and vision for cancer research on the African continent Infect Agent Cancer 11(1) 63 https://doi.org/10.1186/s13027-016-0110-9 PMID: 27980610 PMCID: 5139075
12. Niksic M, Rachet B, and Duffy SW, et al (2016) Is cancer survival associated with cancer symptom awareness and barriers to seeking medical help in England? An ecological study Br J Cancer 115(7) 876–886 https://doi.org/10.1038/bjc.2016.246 PMID: 27537388 PMCID: 5046204
13. Thomas TH, Campbell GB, and Lee YJ, et al (2021) Priorities to improve cancer caregiving: report of a caregiver stakeholder workshop [Internet] Support Care Cancer 29(5) 2423–2434 Date accessed: 06/10/22 https://doi.org/10.1007/s00520-020-05760-y PMCID: 7952464
14. MacRae MC, Fazal O, and O’Donovan J (2020) Community health workers in palliative care provision in low-income and middle-income countries: a systematic scoping review of the literature BMJ Global Health 5(5) e002368 https://doi.org/10.1136/bmjgh-2020-002368 PMID: 32457030 PMCID: 7252978
15. Holden CE, Wheelwright S, and Harle A, et al (2021) The role of health literacy in cancer care: a mixed studies systematic review PLoS One 16(11) e0259815 https://doi.org/10.1371/journal.pone.0259815 PMID: 34767562 PMCID: 8589210
16. van der Plas WY, Benjamens S, and Kruijff S (2020) The increased need for palliative cancer care in Sub-Saharan Africa Eur J Surg Oncol 46(7) 1373–1376 https://doi.org/10.1016/j.ejso.2020.03.212 PMID: 32265092
17. Parkin DM, Sitas F, and Chirenje M, et al (2008) Part I: cancer in indigenous Africans – burden, distribution, and trends Lancet Oncol 9(7) 683–692 https://doi.org/10.1016/S1470-2045(08)70175-X PMID: 18598933
18. Kanavos P (2006) The rising burden of cancer in the developing world Ann Oncol 17 viii15–viii23 https://doi.org/10.1093/annonc/mdl983 PMID: 16801335
19. Knaul FM, Bhadelia A, and Rodriguez NM, et al (2018) The Lancet Commission on Palliative Care and Pain Relief—findings, recommendations, and future directions Lancet Glob Health 6 S5–S6 https://doi.org/10.1016/S2214-109X(18)30082-2
20. Boyle P, Ngoma T, and Sullivan R, et al (2019) Cancer in Africa: the way forward Ecancermedicalscience [Internet] 13 953 Date accessed: 28/09/22 PMID: 31552126 PMCID: 6722114
21. Okobia MN (2003) Cancer care in sub-Saharan Africa – urgent need for population-based cancer registries Ethiop J Health Dev 17(2) 89–98
22. IAEA (2016) Cancer Registries for Africa: Regional Workshop in Brazzaville Highlights Need for Action [Internet] [https://www.iaea.org/newscenter/news/cancer-registries-for-africa-regional-workshop-in-brazzaville-highlights-need-for-action] Date accessed: 27/08/22
23. Omonisi AE, Liu B, and Parkin DM (2020) Population-based cancer registration in Sub-Saharan Africa: its role in research and cancer control JCO Glob Oncol 6 1721–1728 https://doi.org/10.1200/GO.20.00294 PMID: 33180635 PMCID: 7713579
24. Ocran Mattila P, Ahmad R, and Hasan SS, et al (2021) Availability, affordability, access, and pricing of anti-cancer medicines in low- and middle-income countries: a systematic review of literature Front Public Health [Internet] 9 628744 Date accessed: 06/10/22 https://doi.org/10.3389/fpubh.2021.628744 PMID: 33996712 PMCID: 8120029
Supplementary data
Assessment of the barriers to optimal cancer care and treatment in Cameroon
Questionnaire Date July 2020
Section 1: Health facility information

Section 2: Human resource
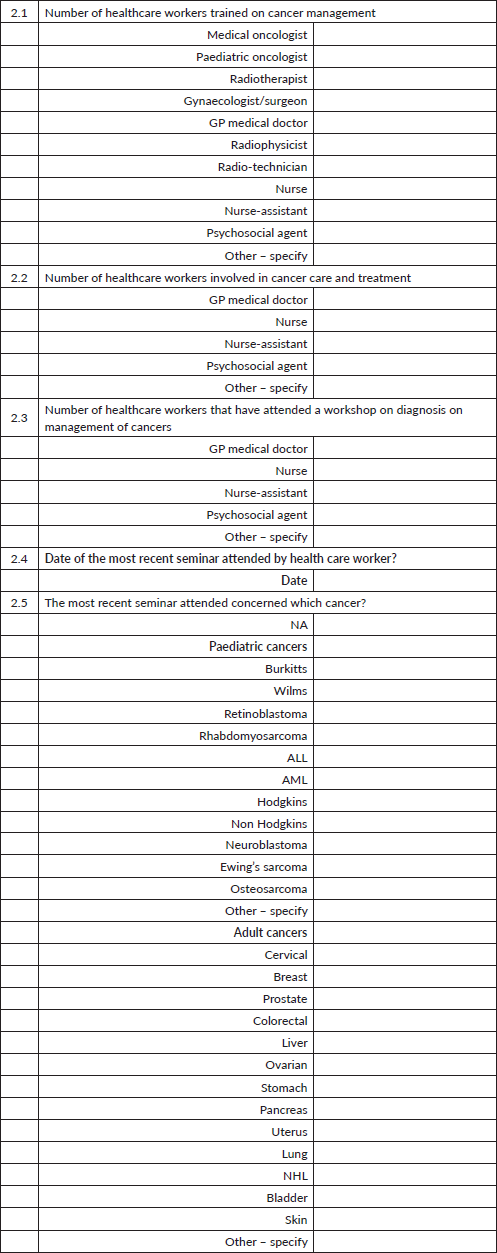
Section 3: Chemotherapy

Section 4: Radiotherapy and nuclear medicine
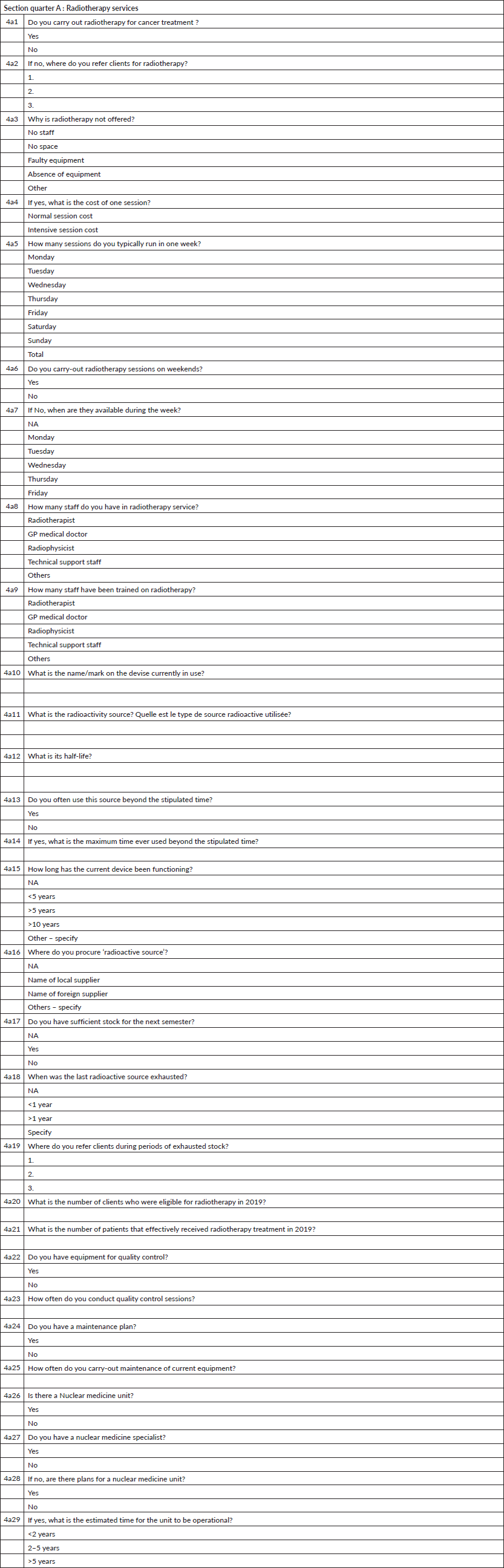
Section 4B: Surgery for cancers
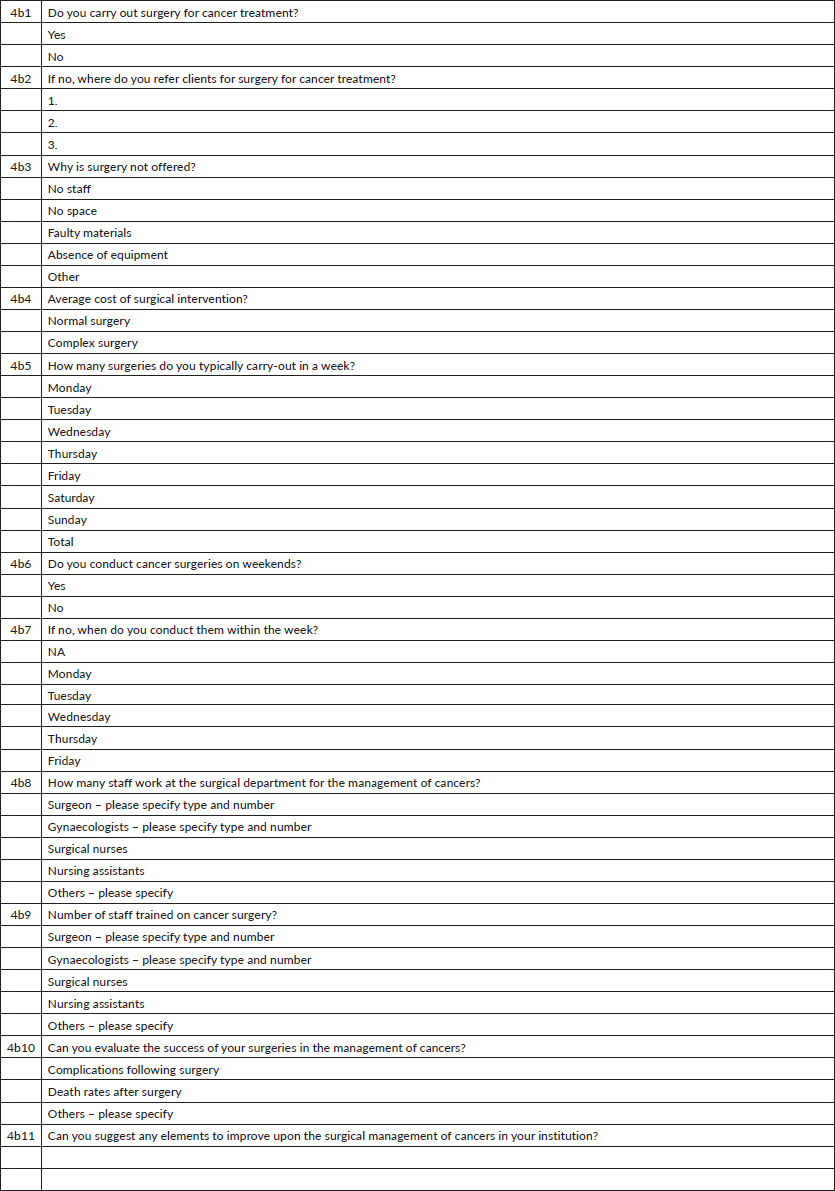
Section 5: Patient follow-up and palliative care
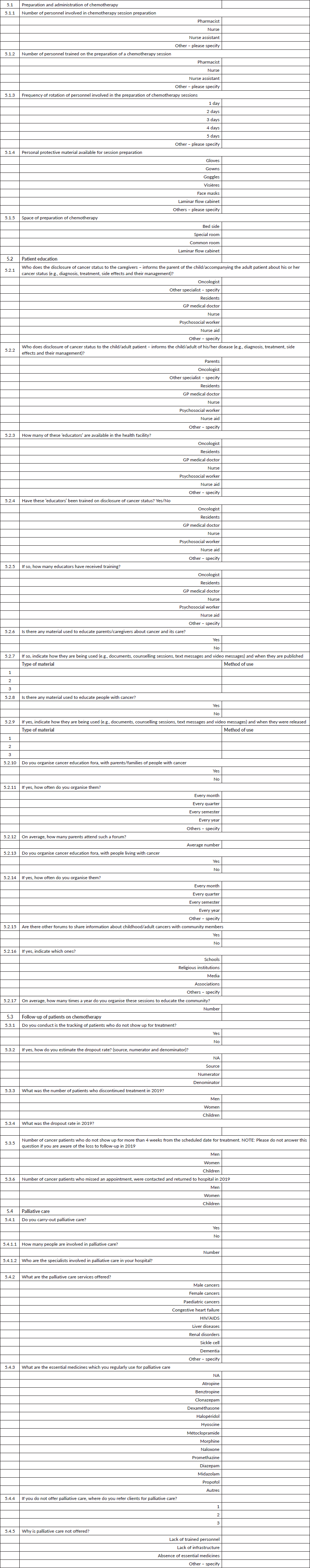
Section 6: Data systems

Section 7: Chemotherapy stock management

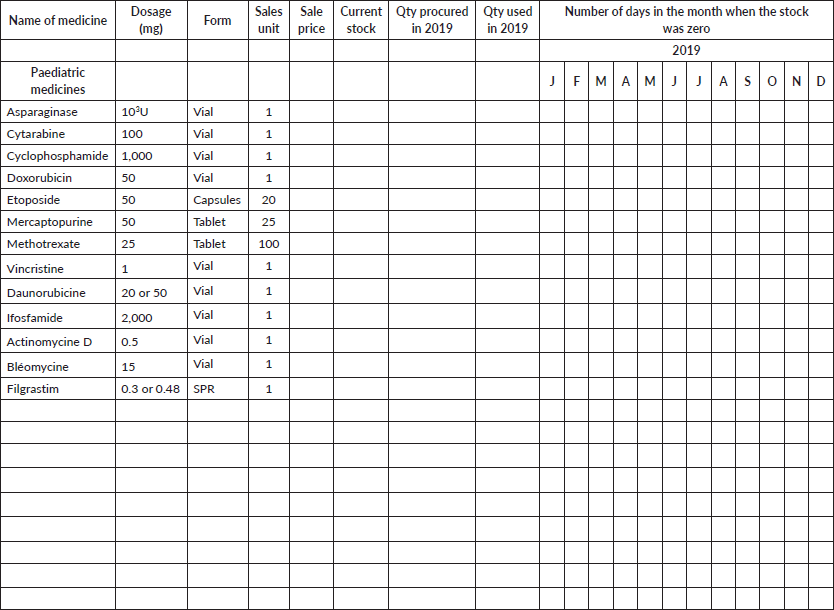
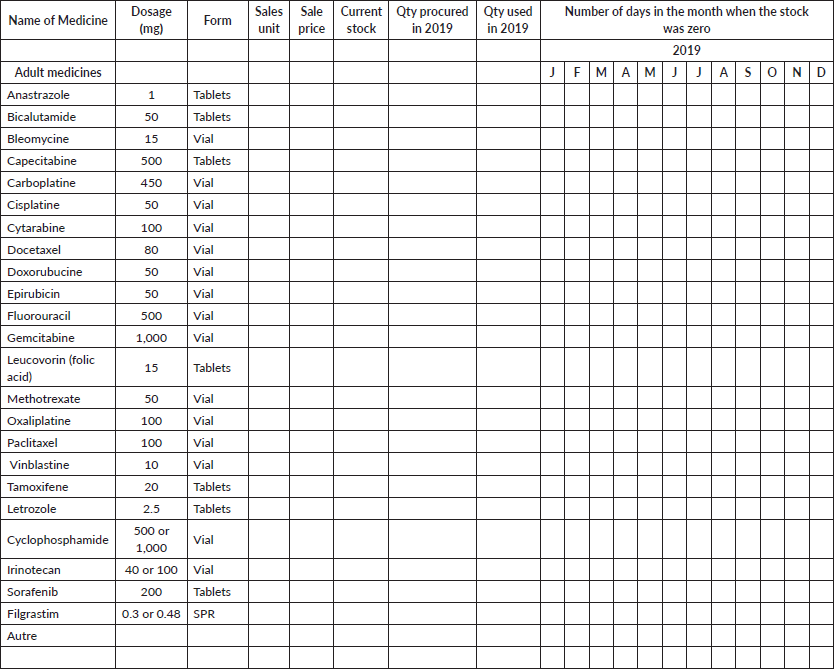
Contacts