The current status of geriatric oncology in India
Vanita Noronha1, Abhijith Rajaram Rao2, Anant Ramaswamy1, Anita Kumar1, Anupa Pillai1, Ratan Dhekale1, Jyoti Krishnamurthy1, Akhil Kapoor3, Shreya Gattani1, Arshiya Sehgal4, Sharath Kumar4, Renita Castelino4, Sarika Mahajan5, Anuradha Daptardar5, Lekhika Sonkusare6, Jayita Deodhar6, Nabila Ansari7, Manjusha Vagal7, Purabi Mahajan8, Shivshankar Timmanpyati8, Manjunath Nookala4, Ankita Chitre9, Prem Naganath Narasimhan10, Joyita Banerjee11, Vikram Gota4, Shripad Banavali1, Rajendra A Badwe12 and Kumar Prabhash1
1Department of Medical Oncology, Tata Memorial Centre, Homi Bhabha National Institute, Mumbai 400012, India
2Department of Geriatric Medicine, All India Institute of Medical Science, New Delhi 110023, India
3Department of Medical Oncology, Mahamana Pandit Madan Mohan Malviya Cancer Center & Homi Bhabha Cancer Hospital, Varanasi 221005, India
4Department of Clinical Pharmacology, Advanced Centre for Treatment Research and Education in Cancer, Navi Mumbai 410210, India
5Department of Physiotherapy, Tata Memorial Centre, Homi Bhabha National Institute, Mumbai 400012, India
6Department of Psycho-oncology, Tata Memorial Centre, Homi Bhabha National Institute, Mumbai 400012, India
7Department of Occupational Therapy, Tata Memorial Centre, Homi Bhabha National Institute, Mumbai 400012, India
8Department of Digestive Diseases and Clinical Nutrition, Tata Memorial Centre, Homi Bhabha National Institute, Mumbai 400012, India
9Department of Physiotherapy, Mahamana Pandit Madan Mohan Malviya Cancer Center & Homi Bhabha Cancer Hospital, Varanasi 400012, India
10Consultant Geriatrician, Jaslok Hospital and Research Center, Mumbai 400026, India
11Venu Geriatric Care Centre, Venu Charitable Society, New Delhi 110017, India
12Department of Surgical Oncology, Tata Memorial Centre, Homi Bhabha National Institute, Mumbai 400012, India
Abstract
Geriatric oncology in India is relatively new. The number of older persons with cancer is increasing exponentially; at our institution, 34% of patients registered are 60 years and over. Apart from the Tata Memorial Hospital in Mumbai, there are currently no other Indian centers that have a dedicated geriatric oncology unit. Geriatric assessments (GAs) are done sporadically, and older patients with cancer are usually assessed and treated based on clinical judgement. Challenges to increasing the uptake of GA include a lack of training/time/interest or knowledge of the importance of the GA. Other challenges include a lack of trained personnel with expertise in geriatric oncology, and a paucity of research studies that seek to advance the outcomes in older Indian patients with cancer. We anticipate that over the next 10 years, along with the inevitable increase in the number of older persons with cancer in India, there will be a commensurate increase in the number of skilled personnel to care for them. Key goals for the future include increased research output, increased number of dedicated geriatric oncology units across the country, India-specific geriatric oncology guidelines, geriatric oncology training programs, and a focus on collaborative work across India and with global partners. In this narrative review, we provide a broad overview of the status of geriatric oncology in India, along with a description of the work done at our center. We hope to spark interest and provide inspiration to readers to consider developing geriatric oncology services in other settings.
Keywords: India, LMIC, collaboration, research, education, training, older, elderly
Correspondence to: Kumar Prabhash
Email: kumarprabhashtmh@gmail.com
Published: 31/08/2023
Received: 06/03/2023
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Geriatric oncology in India is in its infancy. The majority of older Indian patients with cancer are not evaluated systematically with a validated geriatric assessment (GA), but rather are assessed using clinical judgement. Due to a severe shortage of persons skilled in geriatric oncology, and the lack of dedicated geriatric oncology units both in major academic centers as well as in corporate hospitals and private practices in India, the care provided to older Indian patients with cancer is likely to be sub-optimal [1]. Besides, several GA tools and scales that were developed in the West are not suitable for some older Indian patients, due to differences in cultural experiences, illiteracy, and varying life expectancies [2].
The functional status is a measure of the ability of an individual to perform tasks that maintain independence [3]. This functional status declines progressively with age, making older individuals vulnerable to stressors and rendering some incapable of living independently, functionally and socially [4]. There is heterogeneity in the ageing process, which further contributes to the complexity of treatment decisions. These factors result in age-related variations in treatment patterns and outcomes, potentially culminating in under- or overtreatment, which can influence both the risks of treatment toxicity, and survival [5]. Though the Eastern Cooperative Oncology Group (ECOG) performance status (PS), which is the traditional method used by oncologists to evaluate functional status globally, has been found to correlate moderately well with vulnerabilities in various geriatric domains, it cannot replace a formal GA [6]. Despite the broad scope of geriatric oncology, only a few Indian centers offer a formal geriatric oncology service, or the ability to provide specialised care to an older person with cancer.
There are myriad other issues plaguing geriatric oncology in India, including a lack of teaching programs, almost no research studies that either include older persons with cancer or focus on issues important to older patients with cancer, and a lack of an inter-institutional and pan-India collaborative effort to advance the care of older Indian patients with cancer. Many of these issues are not unique to India, but are global phenomena. We explore the current status of geriatric oncology in India, the challenges, strengths and opportunities and suggest the key focus areas over the course of the next decade. Through this review article, we hope to inspire at least some readers to build up geriatric oncology services at their clinics, and establish centers of excellence in geriatric oncology at various institutions across India.
Epidemiology of older adults in India
In 2010, 524 million individuals globally were aged 65 years or older. By the year 2050, the World Health Organisation has predicted that 1.5 billion people will be 65 years or older [7]. Nearly 80% of these older individuals will be living in low-and middle-income countries [8]. This will have a tremendous impact on the global cancer burden. India is also witnessing a demographic transition. In 2011, older persons constituted 8.6% of India’s total population, equalling 103 million [9]. This proportion is expected to increase exponentially and is projected to reach 19.5% in 2050, equalling 319 million people. The proportion of the oldest-old, i.e., those aged 75 years and over, is projected to rise by 340% [10, 11].
Advancing age is a risk factor for the development of malignancy, with persons over 65 years accounting for 60% of newly diagnosed malignancies and 70% of cancer deaths. These mainly include cancers of the breast, lung, prostate, cervix, esophagus and ovary [12]. Globally, there are geographic and economic factors that affect the number of older people living with and surviving cancer, but data show a common trend that a large proportion of people with cancer are older [13, 14]. The Indian Council of Medical Research National Cancer Registry Program estimates that the number of cancer diagnoses will increase from 1.39 million in 2020 to 1.57 million by 2050 [15]. Thus, the number of older persons with cancer is expected to rise exponentially in India over the next few years. Data from our hospital-based registry at the Tata Memorial Hospital in Mumbai revealed that between January 2019 and December 2021, there were 29,768 patients with cancer registered who were over 60 years old among the total pool of 87,101 newly registered patients, i.e., 34.2% of the total number of patients with cancer registered at our institute were 60 years or older [unpublished data].
Uptake of the GA in India
We conducted a survey among 100 physicians to assess the situation at the ground level regarding the extent of knowledge and practice of GA in India [16]. Although 99% of respondents cared for older patients with cancer, with 87% caring for 10 or more per week, 51% did not routinely perform a GA. Almost 70% of the survey participants relied on ‘intuition’ to formulate the management plan; less than 10% used validated tools. Additionally, 44% were unaware of the American Society of Clinical Oncology (ASCO) geriatric oncology guidelines. Barriers to performing the GA routinely included lack of time, staff, awareness, resources and space, and an uncertainty regarding which GA tools to use. The results of our survey underlined the need to devise a tailored GA tool in India for screening, evaluation, and management in limited resource settings [16].
Oncologists’ perceptions of the need for assessing individual domains in the GA and worthwhile outcomes
We conducted a follow-up survey among 234 healthcare professionals (71% medical oncologists, 11.7% radiation oncologists, and 10.7% surgical oncologists) to understand the perceived relative importance of assessing various GA domains [17]. Over 99% participants thought that it was important to assess comorbidities, polypharmacy, medications, drug interactions and social support. Over 98% thought it important to assess function, falls, and quality of life (QoL). Approximately 97% thought that assessment of nutrition and cognition was important, while 93.6% thought that psychological evaluation was important. Regarding the goals of performing a GA, 90% hoped that it would lead to an improvement in QoL, 65.6% desired a decrease in toxicity, and 42.9% wished for survival prolongation. Regarding the relative importance of a decrease in treatment toxicity or improvement in QoL versus survival prolongation in older patients with cancer, 62.6% found toxicity + QoL more important, 36.9% found them as important and only 0.5% respondents felt that decreasing toxicity and improving QoL were less important than prolonging survival [17].
Defining the age-cutoff for ‘old’
The answer to the question, ‘How old is old?’ varies based on multiple factors. For an individual, the factors are myriad; however, at the population level, the answer is straightforward and based on life expectancy and retirement age [18]. The International Society of Geriatric Oncology (SIOG) defines this age as 70 years, while the ASCO recommendations are for persons aged 65 years and older. When we started the geriatric oncology clinic at the Tata Memorial Hospital (TMH), in Mumbai, India, we evaluated patients aged >65 years based on the ASCO guidelines [19]. We later realised that the age cut-off to define ‘old age’ varies across cultures, and that using the age cutoff established by an American organisation was not appropriate for Indian patients. The average life expectancy in India is 70.4 years overall; 71.8 years for women, and 69.2 years for men [20], which is much lower than that of people living in Japan (85 years) or the United States (79 years). In Japan, the age cut-off for the geriatric population is considered to be 75 years, while in India, according to the National Program for Health Care of the Elderly (NPHCE) [21] established by the Government of India, an older person is defined as anyone who is 60 years or older. Hence the age cut-off in our geriatric oncology clinic was changed to 60 years [22]. This age cut-off is followed by other Indian clinicians as well [23, 24].
Geriatric oncology service at the Tata Memorial Hospital
TMH has a well-established geriatric oncology multidisciplinary service for patients aged 60 years and above with cancer. Starting on June 15, 2018, as a 1-day-a-week outpatient clinic, the service now functions daily, both for outpatients and inpatient consultations. Our goal is to perform detailed GAs and provide multidisciplinary, patient-specific care plans (Figure 1). In addition, we also run an academic teaching program and are attempting to bridge the research gap. The clinic is run by two medical oncologists; other members include a geriatric oncology fellow (trainee), senior residents, and patient coordinators. This multidisciplinary clinic also comprises clinical pharmacologists, geriatricians, onco-psychologists, physiotherapists, occupational therapists, dieticians, and social workers. Although initial referrals to our clinic were sparse, these have increased exponentially over time (except for the brief period when we closed the clinic from Apr to Jun 2020 during the peak of the COVID-19 pandemic), and currently, we assess approximately 20–30 patients a week. Between Jun 15, 2018, and May 12, 2023, we have assessed 2,322 patients (Figure 2).
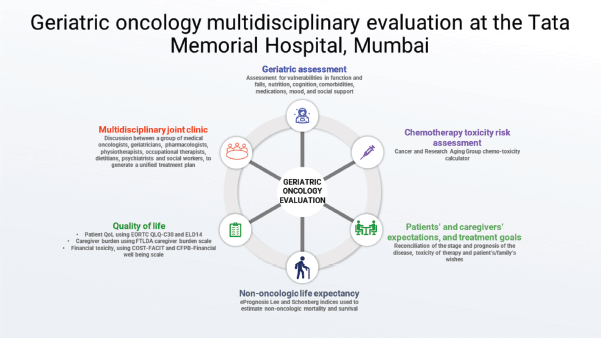
Figure 1. The process of evaluation and assessment in the geriatric oncology at the Tata Memorial Hospital in Mumbai, India.
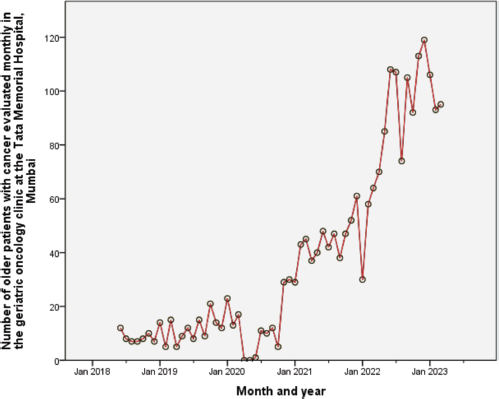
Figure 2. The progressive increase in the number of older patients with cancer evaluated monthly in the geriatric oncology clinic at the Tata Memorial Hospital (Mumbai, India) since inception on June 15, 2018.
GA done at the Tata Memorial Hospital and details of the tools used
Overall assessment
All patients referred to our geriatric oncology clinic undergo a detailed evaluation for the presence of vulnerabilities in various geriatric non-oncologic domains and caregiver burden. Patients are evaluated for geriatric syndromes (constipation, insomnia, lower urinary tract symptoms, urinary incontinence, osteoporosis, pressure sores), visual and hearing impairment, voice, and oral health. We assess chemotherapy toxicity risk using the Cancer and Aging Research Group (CARG) tool and estimate the non-oncologic life expectancy using ePrognosis. We also evaluate financial toxicity, and overall QoL (Table 1).
Non-oncologic domains
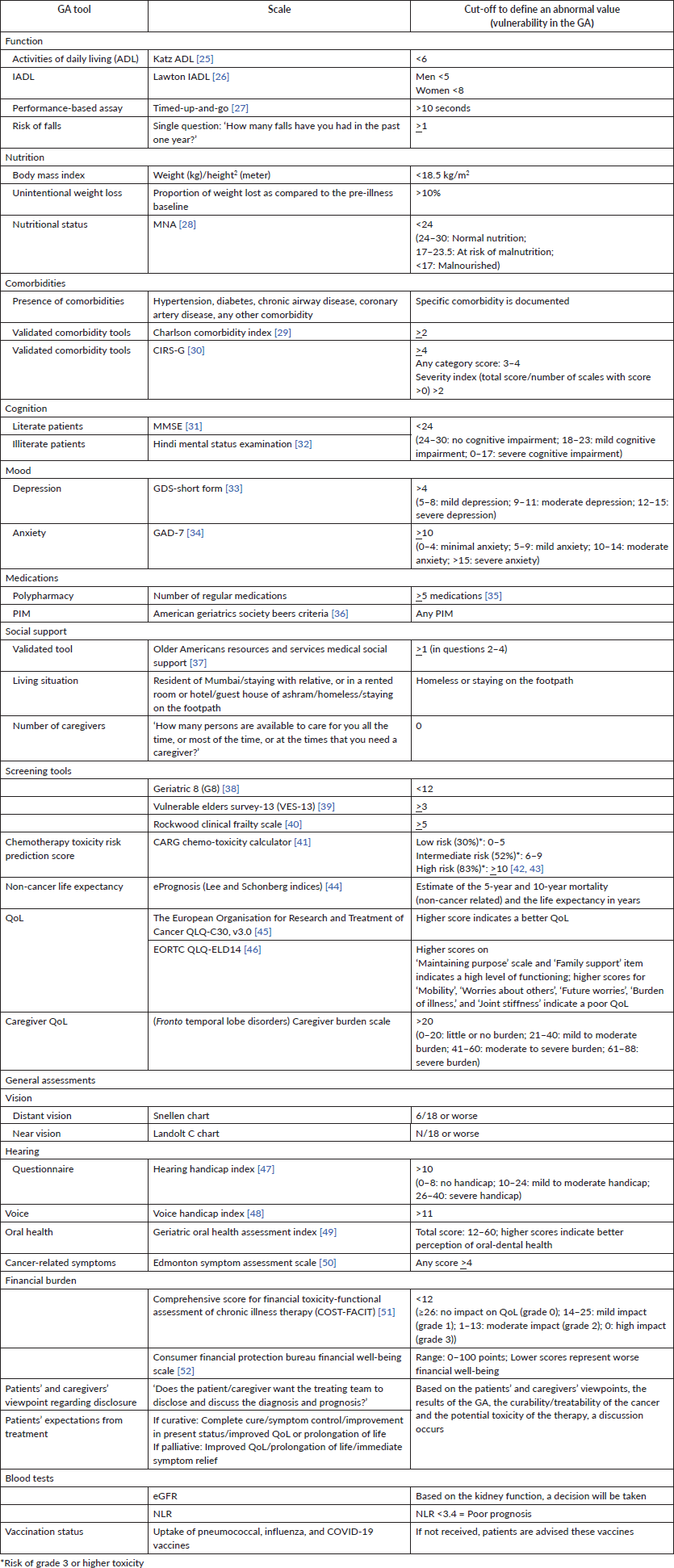
The various GA tools used at our clinic, along with the cut-offs have been provided in Table 1.
Table 1. Details of the tools used, assessments performed and questionnaires administered as a part of the GA at the Tata Memorial Hospital (Mumbai, India).
Blood tests
The patient's baseline haemoglobin, creatinine, albumin and sodium are noted, and the estimated glomerular filtration rate (eGFR) is calculated for all patients. Additionally, we determine the patient's neutrophil-lymphocyte ratio (NLR) considering it a prognostic inflammatory marker in older patients with cancer.
Patients’ and caregivers’ goals of therapy
The patient's perspective regarding the intent of therapy (curative/palliative) and the patient's expectations from treatment and the patients’/primary caregivers' wishes regarding disclosure about the diagnosis/prognosis are discussed, and integrated into the care plan.
Appropriateness of GA tools for older Indian adults
The GA has been developed in a predominantly western urban cohort of patients, and multiple aspects are culturally inappropriate for our Indian patients [2]. The problems with individual assessment using tools, such as instrumental activities of daily living (IADL) (roles and responsibilities within family vary diversely), mini-mental status examination (MMSE) (literacy, relocation to Mumbai for treatment, unawareness of dates according to the Gregorian calendar), mini-nutritional assessment (MNA) (lack of access to a weighing scale, thin body habitus), a cumulative illness rating scale for geriatrics (CIRS-G) (lack of strong primary healthcare systems, so no robust diagnosis and therapy of comorbidities), geriatric depression scale (GDS) and generalised anxiety disorder assessment-7 (GAD7) (culturally inappropriate questions) are prevalent. We have found that multiple portions of the GA are culturally inappropriate and could not be analysed or led to unreliable results [2]. The first step in tackling this issue was taken by Banerjee et al [54], who developed a short-35-item screening tool that would be appropriate for Indian patients. Further, they also identified suitable cut-off scores that correlated with survival, which could help streamline care in a resource-limited setting [55]. By reconciling the cultural differences and establishing a GA directed at Indian patients with cancer, we hope to be able to provide better service to our patients.
In addition to socio-cultural differences, phenotypic diversity cannot be ignored. The normal range of the body mass index (BMI) for the Asian population is lower as compared to that in western countries [56]. We identified that the cut-off TUG score of 12 seconds [19] was not as sensitive, and a lower cut-off score of 10 seconds was more appropriate for older Indian patients with cancer [57].
Prevalence of non-oncologic vulnerabilities in older persons with cancer in India
In our geriatric oncology clinic at TMH, the median time to perform a GA is 50 minutes (IQR, 40–61) [58]. Despite the time-consuming process, we found that the GA was very valuable in detecting geriatric vulnerabilities. About 98% of our patients had vulnerabilities in at least one geriatric domain. The abnormalities noted were in the domains of comorbidities (79%), fatigue (77%), nutrition (65%), function and falls (52%), mood (32%), and cognition (18%) [58]. We also observed that 55% of the patients had polypharmacy, 80% were on potentially inappropriate medications (PIM), and nearly 23% were taking alternative medications (ayurvedic/naturopathic/homeopathic) [59]. Almost 60% needed referrals to a physiotherapist and occupational therapist, 69% required dietary intervention and 29% required evaluation and management by a psychologist/counsellor.
Impact of the GA on the systemic therapy plan
Globally, it is well recognised that systematic evaluation of older patients with cancer with a GA is valuable and leads to better treatment choices, lowers toxicity and improves communication. However, conducting the GA is time-and labor-intensive, and resources are limited at most centers in India. At our institution, the GA led to a change in cancer-directed systemic therapy plan in 38.7% of cases, with the commonest change being treatment de-intensification in 32.1% of patients [60]. Thus, a significant proportion of our older patients with cancer are over-treated in cases where a GA is not performed.
Geriatric oncology education programs
The Department of Medical Oncology at the Tata Memorial Hospital runs a 1-year geriatric oncology fellowship training program [61]. The program admits doctors trained in Internal Medicine, Geriatric Medicine, and Medical Oncology. The fellow undergoes rigorous training in patient assessment, care-plan development, academic learning, and research protocol development and implementation. The department also conducts Geriatric Oncology workshops at least twice a year to train oncologists and primary care physicians. The goal of such continuous medical education includes spreading awareness of geriatric oncology, imparting education regarding the principles of geriatric oncology, and training for performing GAs for older patients with cancer. The Tata Memorial Center has also partnered with SIOG to conduct an annual advanced course in geriatric oncology [62].
Status of research in geriatric oncology in India
Due to the heterogeneous population and lack of data from older Indian patients with cancer, we generally need to extrapolate the results from studies done in other populations [63]. Broadly, we envision that the most impactful geriatric oncology research in India would include epidemiologic research to understand the demographic profile and various other epidemiologic parameters; tool validation research to test the appropriateness of assessment tools; implementation research to discover and test methods to increase the uptake/streamline or improve the efficiency of the GA; observational studies to understand the various aspects of geriatric oncology; therapeutic research aimed either at testing, cancer-directed therapy or treatment-related toxicities; and patient-centric research to understand and improve the experiences/perspectives/challenges faced by patients/caregivers (Table 2). A major challenge to conducting geriatric oncology research in India is the lack of collaboration. A limiting factor is the lack of centers that have geriatric oncology units and clinicians who have expertise in geriatric oncology. We have attempted to address this issue by forming a group of like-minded clinicians from various centers across India who have an interest in geriatric oncology. Several initiatives have been taken in this group to bridge the knowledge and research gap in geriatric oncology in India, some of which have been described in Table 2.
Patient and caregiver support groups
Addressing the supportive care needs of an increasing number of older patients with cancer and their caregivers requires innovative strategies and delivery methods. Support groups bring together people who are going through or have gone through similar experiences. Online support groups are social spaces where people with shared interests can gain and share information and support. Spurred on by the COVID-19 pandemic and the increasing need for additional counselling/support/advice by patients and caregivers, in May 2022 we started an online support group for patients and caregivers of older patients with cancer. This is conducted with the help of a non-governmental organisation, and has been held on a virtual platform successfully every month. Along with patients and caregivers sharing their views and experiences, they are also educated regarding the importance of maintaining the patients' functionality, nutrition, cognitive capacity and mood.
Action points for the next decade
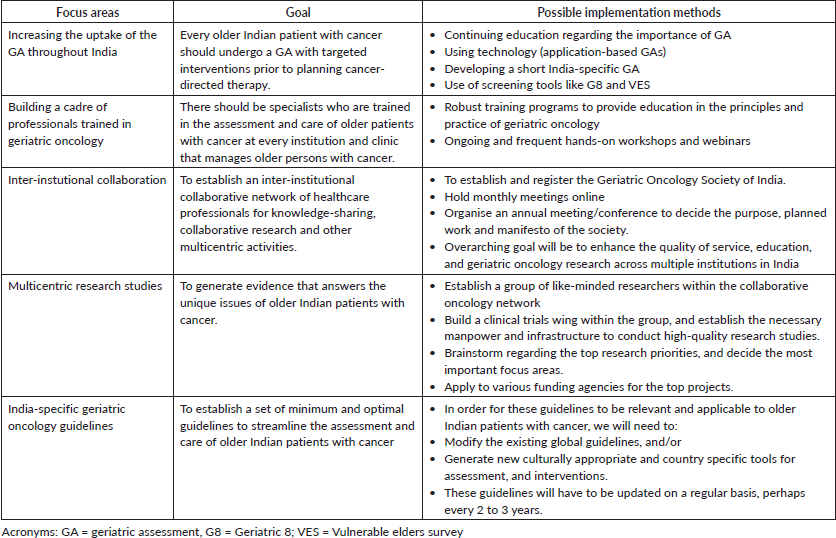
In the coming decade, there will be an exponential increase in the number of older persons with cancer. In order to provide optimal support for these older and often frail patients, our focus will be on five high-impact areas, outlined in Table 3.
Conclusion
There is a need for awareness of geriatric oncology among practicing physicians who care for older patients with cancer. Only a few institutes in India provide specialised geriatric oncology services. Recognising the importance and implementing such a service to optimally manage this vulnerable population is an urgent necessity. At the Tata Memorial Hospital in Mumbai, we have established a comprehensive multidisciplinary geriatric oncology service and are attempting to fill the gap in terms of providing specialised care to older patients with cancer, designing and implementing research studies that focus on this cohort of patients, and disseminating high-quality education to students and colleagues. Since the clinic was established in June 2018, we have accomplished a lot in terms of clinical service, education and research; however, much more needs to be done. More physicians, oncologists, geriatricians, and nursing staff need to be trained to perform GAs, interpret the results, and prepare tailored care plans. There is a need to develop and validate suitable and culturally appropriate tools to assess older Indian patients with cancer.
Conflicts of interest
None.
Funding
None.
Table 2. Some of the research studies (completed, ongoing and planned) to bridge the knowledge gap of geriatric oncology in India.
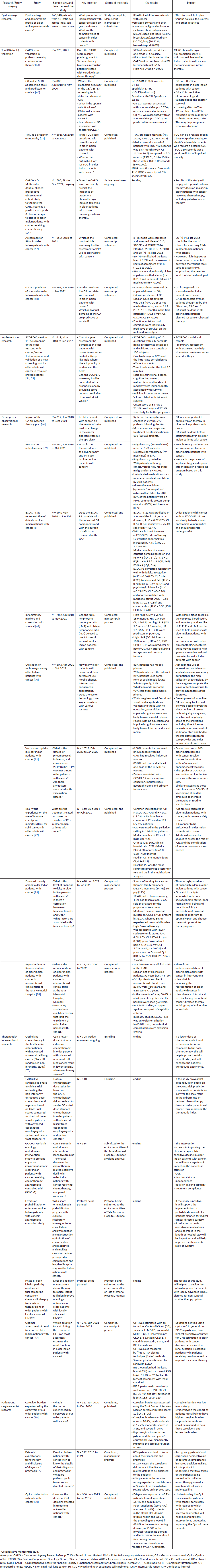
Table 3. Action points and implementation strategies to take geriatric oncology in India forward in the next decade.
References
1. Parikh PM, Chaitanya K, and Boppana M, et al (2020) Geriatric oncology landscape in India – current scenario and future projections Cancer Res Stat Treat 3 296–969 https://doi.org/10.4103/CRST.CRST_150_20
2. Noronha V, Ramaswamy A, and Banavali S, et al (2020) Ethnocultural inequity in the geriatric assessment Cancer Res Stat Treat 3 808–813 https://doi.org/10.4103/crst.crst_353_20
3. Molenaar EA, Barten JA, and te Velde S, et al (2020) Functional independence in the community dwelling older people: a scoping review J Popul Ageing 16 243–262 https://doi.org/10.1007/s12062-020-09315-1
4. Overcash J (2015) Assessing the functional status of older cancer patients in an ambulatory care visit Healthcare 3(3) 846–859 https://doi.org/10.3390/healthcare3030846 PMID: 27417801 PMCID: 4939579
5. Bouchardy C, Rapiti E, and Fioretta G, et al (2003) Undertreatment strongly decreases prognosis of breast cancer in elderly women J Clin Oncol 21(19) 3580–3587 https://doi.org/10.1200/JCO.2003.02.046 PMID: 12913099
6. Gattani S, Ramaswamy A, and Noronha V, et al (2022) ECOG performance status as a representative of deficits in older Indian patients with cancer: a cross-sectional analysis from a large cohort study Cancer Res Stat Treat 5(2) 256 https://doi.org/10.4103/crst.crst_127_22
7. Ageing and health [Internet] [https://www.who.int/news-room/fact-sheets/detail/ageing-and-health] Date accessed: 07/11/22
8. Officer A, Schneiders ML, and Wu D, et al (2016) Valuing older people: time for a global campaign to combat ageism Bull World Health Organ 94(10) 710A–710A https://doi.org/10.2471/BLT.16.184960
9. [https://www.who.int/india/health-topics/ageing] Date accessed: 05/03/23
10. Elderly in India 2021 (2021) [Internet] [https://ruralindiaonline.org/en/library/resource/elderly-in-india-2021/] Date accessed: 07/11/22
11. United Nations Population Division and Department of Economic and Social Affairs (2019) World Population Prospects 2019: Data Booklet (ST/ESA/SER.A/424) (New York: United Nations)
12. American Cancer Society Cancer facts & figures 2022 [Internet] [
13. Bray F, Ferlay J, and Laversanne M, et al (2015) Cancer incidence in five continents: inclusion criteria, highlights from volume X and the global status of cancer registration Int J Cancer 137(9) 2060–2071 https://doi.org/10.1002/ijc.29670 PMID: 26135522
14. IARC (2014) Cancer Incidence in Five Continents Volume X [Internet] [https://publications.iarc.fr/Book-And-Report-Series/Iarc-Scientific-Publications/Cancer-Incidence-In-Five-Continents-Volume-X-2014] Date accessed: 07/11/22
15. Report of National Cancer Registry Programme 2020 [Internet] [
16. Noronha V, Talreja V, and Joshi A, et al (2019) Survey for geriatric assessment in practicing oncologists in India Cancer Res Stat Treat 2(2) 232 https://doi.org/10.4103/CRST.CRST_99_19
17. Noronha V, Kalra D, and Ramaswamy A, et al (2021) Oncologists’ perceptions of the need for assessing individual domains in the geriatric assessment and worthwhile outcomes in treating older patients with cancer: a questionnaire-based survey Cancer Res Stat Treat 4(3) 492–498
18. Sahoo TP (2021) Can patients aged 60 years and over be called elderly? Cancer Res Stat Treat 4 582–583
19. Mohile SG, Dale W, and Somerfield MR, et al (2018) Practical assessment and management of vulnerabilities in older patients receiving chemotherapy: ASCO guideline for geriatric oncology J Clin Oncol 36(22) 2326–2347 https://doi.org/10.1200/JCO.2018.78.8687 PMID: 29782209 PMCID: 6063790
20. Worldometer (2023) Life expectancy by country and in the world [Internet] [https://www.worldometers.info/demographics/life-expectancy/] Date accessed: 21/01/23
21. Ministry of Health and Family Welfare | GOI (2023) National programme for health care of the elderly(NPHCE) [Internet] [https://main.mohfw.gov.in/major-programmes/Non-Communicable-Diseases/Non-Communicable-Diseases-1] Date accessed: 21/01/23
22. Dhanawat A, Noronha V, and Ramaswamy A, et al (2022) The prevalence of cognitive impairment in older Indian persons with cancer and brain metastases Ecancermedicalscience 16 1372 https://doi.org/10.3332/ecancer.2022.1372 PMID: 35702404 PMCID: 9117002
23. Nethan S, Cherian M, and Brain E, et al (2022) Cancer in the older Indian population: understanding the current context in an emerging economy J Geriatr Oncol 13(3) 273–281 https://doi.org/10.1016/j.jgo.2021.10.013
24. Mishra S, Radhakrishnan V, and Ganesan P, et al (2017) Predictors of chemotherapy related toxicities in elderly lymphoma patients: experience from a tertiary cancer centre Indian J Hematol Blood Transfus 33(4) 470–476 https://doi.org/10.1007/s12288-017-0794-z PMID: 29075056 PMCID: 5640546
25. Katz S, Ford AB, and Moskowitz RW, et al (1963) Studies of illness in the aged. The index of adl: a standardized measure of biological and psychosocial function JAMA 185 914–919 https://doi.org/10.1001/jama.1963.03060120024016 PMID: 14044222
26. Graf C (2008) The Lawton instrumental activities of daily living scale Am J Nurs 108(4) 52–62 quiz 62–63 https://doi.org/10.1097/01.NAJ.0000314810.46029.74 PMID: 18367931
27. Podsiadlo D and Richardson S (1991) The timed “Up & Go”: a test of basic functional mobility for frail elderly persons J Am Geriatr Soc 39(2) 142–148 https://doi.org/10.1111/j.1532-5415.1991.tb01616.x PMID: 1991946
28. Vellas B, Guigoz Y, and Garry PJ, et al (1999) The mini nutritional assessment (MNA) and its use in grading the nutritional state of elderly patients Nutrition 15(2) 116–122 https://doi.org/10.1016/S0899-9007(98)00171-3 PMID: 9990575
29. Charlson ME, Pompei P, and Ales KL, et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation J Chronic Dis 40(5) 373–383 https://doi.org/10.1016/0021-9681(87)90171-8 PMID: 3558716
30. Miller MD, Paradis CF, and Houck PR, et al (1992) Rating chronic medical illness burden in geropsychiatric practice and research: application of the cumulative illness rating scale Psychiatry Res 41(3) 237–248 https://doi.org/10.1016/0165-1781(92)90005-N PMID: 1594710
31. Folstein MF, Folstein SE, and McHugh PR, et al (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician J Psychiatr Res 12(3) 189–198 https://doi.org/10.1016/0022-3956(75)90026-6 PMID: 1202204
32. Ganguli M, Ratcliff G, and Chandra V, et al (1995) A Hindi version of the MMSE: the development of a cognitive screening instrument for a largely illiterate rural elderly population in India Int J Geriatr Psychiatry 10(5) 367–377 https://doi.org/10.1002/gps.930100505
33. Burke WJ, Roccaforte WH, and Wengel SP, et al (1991) The short form of the Geriatric Depression Scale: a comparison with the 30-item form J Geriatr Psychiatry Neurol 4(3) 173–178 https://doi.org/10.1177/089198879100400310 PMID: 1953971
34. Spitzer RL, Kroenke K, and Williams JBW, et al (2006) A brief measure for assessing generalized anxiety disorder: the GAD-7 Arch Intern Med 166(10) 1092–1097 https://doi.org/10.1001/archinte.166.10.1092 PMID: 16717171
35. Masnoon N, Shakib S, and Kalisch-Ellett L, et al (2017) What is polypharmacy? A systematic review of definitions BMC Geriatr 17 230 https://doi.org/10.1186/s12877-017-0621-2 PMID: 29017448 PMCID: 5635569
36. By the 2019 American Geriatrics Society Beers Criteria® Update Expert Panel (2019) American geriatrics society 2019 updated AGS beers criteria® for potentially inappropriate medication use in older adults J Am Geriatr Soc 67(4) 674–694 https://doi.org/10.1111/jgs.15767
37. Burholt V, Windle G, and Ferring D, et al (2007) Reliability and validity of the older americans resources and services (oars) social resources scale in six European countries J Gerontol Ser B 62(6) S371–S379 https://doi.org/10.1093/geronb/62.6.S371
38. Bellera CA, Rainfray M, and Mathoulin-Pélissier S, et al (2012) Screening older cancer patients: first evaluation of the G-8 geriatric screening tool Ann Oncol 23(8) 2166–2172 https://doi.org/10.1093/annonc/mdr587 PMID: 22250183
39. Saliba D, Elliott M, and Rubenstein LZ, et al (2001) The vulnerable elders survey: a tool for identifying vulnerable older people in the community J Am Geriatr Soc 49(12) 1691–1699 https://doi.org/10.1046/j.1532-5415.2001.49281.x
40. Rockwood K, Song X, and MacKnight C, et al (2005) A global clinical measure of fitness and frailty in elderly people CMAJ Can Med Assoc J 173(5) 489–495 https://doi.org/10.1503/cmaj.050051
41. Cancer and Aging Research Group Chemo-toxicity calculator [Internet] [https://www.mycarg.org/?page_id=2405] Date accessed: 08/11/22
42. Hurria A, Togawa K, and Mohile SG, et al (2011) Predicting chemotherapy toxicity in older adults with cancer: a prospective multicenter study J Clin Oncol 29(25) 3457–3465 https://doi.org/10.1200/JCO.2011.34.7625 PMID: 21810685 PMCID: 3624700
43. Hurria A, Mohile S, and Gajra A, et al (2016) Validation of a prediction tool for chemotherapy toxicity in older adults with cancer J Clin Oncol 34(20) 2366–2371 https://doi.org/10.1200/JCO.2015.65.4327 PMID: 27185838 PMCID: 5321104
44. ePrognosis Lee Schonberg Index [Internet] [https://eprognosis.ucsf.edu/leeschonberg.php] Date accessed: 08/11/22
45. Aaronson NK, Ahmedzai S, and Bergman B, et al (1993) The European organization for research and treatment of cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology J Natl Cancer Inst 85(5) 365–376 https://doi.org/10.1093/jnci/85.5.365 PMID: 8433390
46. [https://qol.eortc.org/questionnaire/qlq-eld14/] Date accessed: 05/03/23
47. Ventry IM and Weinstein BE (1982) The hearing handicap inventory for the elderly: a new tool Ear Hear 3(3) 128–134 https://doi.org/10.1097/00003446-198205000-00006 PMID: 7095321
48. Jacobson BH, Johnson A, and Grywalski C, et al (1997) The Voice Handicap Index (VHI) Am J Speech Lang Pathol 6(3) 66–70 https://doi.org/10.1044/1058-0360.0603.66
49. Dable RA, Nazirkar GS, and Singh SB, et al (2013) Assessment of oral health related quality of life among completely edentulous patients in western India by using GOHAI J Clin Diagn Res JCDR 7(9) 2063–2067 PMID: 24179944 PMCID: 3809683
50. Bruera E, Kuehn N, and Miller MJ, et al (1991) The edmonton symptom assessment system (ESAS): a simple method for the assessment of palliative care patients J Palliat Care 7(2) 6–9 https://doi.org/10.1177/082585979100700202 PMID: 1714502
51. [
52. Consumer Financial Protection Bureau Measure and score financial well-being [Internet] [https://www.consumerfinance.gov/consumer-tools/educator-tools/financial-well-being-resources/measure-and-score/] Date accessed: 06/03/23
53. [
54. Banerjee J, Satapathy S, and Upadhyay AD, et al (2019) A short geriatric assessment tool for the older person with cancer in India – development and psychometric validation J Geriatr Oncol 10(2) 222–228 https://doi.org/10.1016/j.jgo.2018.09.001
55. Banerjee J, Behal P, and Satapathy S, et al (2021) Implementing and validating a care protocol for older adults with cancer in resource limited settings with a newly developed screening tool J Geriatr Oncol 12(1) 139–145 https://doi.org/10.1016/j.jgo.2020.04.013
56. Verma M, Rajput M, and Kishore K, et al (2019) Asian BMI criteria are better than WHO criteria in predicting hypertension: a cross-sectional study from rural India J Fam Med Prim Care 8(6) 2095–2100 https://doi.org/10.4103/jfmpc.jfmpc_257_19
57. Rao AR, Kumar S, and Dhekale R, et al (2022) Timed up and go as a predictor of mortality in older Indian patients with cancer: an observational study Cancer Res Stat Treat 5(1) 75–82 https://doi.org/10.4103/crst.crst_79_22
58. Noronha V, Ramaswamy A, and Dhekle R, et al (2020) Initial experience of a geriatric oncology clinic in a tertiary cancer center in India Cancer Res Stat Treat 3(2) 208 https://doi.org/10.4103/CRST.CRST_119_20
59. Noronha V, Ramaswamy A, and Gattani SC, et al (2021) Polypharmacy and potentially inappropriate medication use in older Indian patients with cancer: a prospective observational study Cancer Res Stat Treat 4(1) 67 https://doi.org/10.4103/crst.crst_50_21
60. Noronha V, Rao A, and Gattani S, et al (2022) Impact of the geriatric assessment on cancer-directed systemic therapy in older Indian persons with cancer: an observational study Cancer Res Stat Treat 5 673–680 https://doi.org/10.4103/crst.crst_298_22
61. [https://tmc.gov.in/m_events/events/EventDetail?id=8730&type=2&pg_tp=intr] Date accessed: 06/03/23
62. [
63. Noronha V (2018) Making a case for cancer research in India Cancer Res Stat Treat 1 71–74
64. Ostwal V, Ramaswamy A, and Bhargava P, et al (2021) Cancer aging research group (CARG) score in older adults undergoing curative intent chemotherapy: a prospective cohort study BMJ Open 11 e047376 https://doi.org/10.1136/bmjopen-2020-047376 PMID: 34187825 PMCID: 8245449
65. Shah M, Noronha V, and Ramaswamy A, et al (2022) G8 and VES-13 as screening tools for geriatric assessment and predictors of survival in older Indian patients with cancer J Geriatr Oncol 13(5) 720–730 https://doi.org/10.1016/j.jgo.2022.02.013 PMID: 35283049
66. [https://ctri.nic.in/Clinicaltrials/pmaindet2.php?trialid=75907&EncHid=&userName=CTRI/2022/10/046865] Date accessed: 06/03/23
67. Castelino R, Noronha V, and Ramaswamy A, et al (2018) Comparison of validated screening tools for the assessment of potentially inappropriate medications in older Indian patients with cancer J Clin Oncol 39(15_suppl)
68. Rao AR, Ramaswamy A, and Kumar S, et al (2012) Geriatric assessment as a predictor of survival among older Indian patients with cancer J Clin Oncol 40(16_suppl) e24012 https://doi.org/10.1200/JCO.2022.40.16_suppl.e24012
69. Noronha V, Rao AR, and Ramaswamy A, et al (2022) SIOG2022-0090* – inflammatory markers and overall survival in India older adults with cancer J Geriatr Oncol 13(8) Suppl 1 S2 https://doi.org/10.1016/S1879-4068(22)00248-X
70. Rao AR, Gattani S, and Castelino R, et al (2021) Utilization of technology among older Indian patients with cancer: a cross-sectional study Cancer Res Stat Treat 4 656–662 https://doi.org/10.4103/crst.crst_290_21
71. Sabu TM, Noronha V, and Rao AR, et al (2023) Uptake of vaccination in older Indian patients with cancer: a cross-sectional observational study Cancer Res Stat Treat 6 52–61 https://doi.org/10.4103/crst.crst_29_23
72. Abraham G, Jobanputra KN, and Noronha V, et al (2021) Immune checkpoint inhibitors in older patients with solid tumors: real-world experience from India Cancer Res Stat Treat 4 270–276 https://doi.org/10.4103/crst.crst_86_21
73. Ramaswamy A, Rao AR, and Noronha V, et al (2023) An evaluation of the financial toxicity amongst older patients with cancer in India J Clin Oncol [ABSTRACT #415036] 41 12048 https://doi.org/10.1200/JCO.2023.41.16_suppl.12048
74. Noronha V, Prabhash K, and Ramaswamy A, et al (2023) Representation of older Indian pts with cancer in interventional clinical trials at Tata Memorial [SIOG 2023 abstract]
75. [https://ctri.nic.in/Clinicaltrials/pmaindet2.php?trialid=75907&EncHid=&userName=CTRI/2022/07/044193] Date accessed: 06/03/23
76. [https://ctri.nic.in/Clinicaltrials/pmaindet2.php?trialid=66186&EncHid=&userName=CTRI/2022/03/040884] Date accessed: 06/03/23
77. Gota V, Gandhi KA, and Castelino R, et al (2023) Comparison of glomerular filtration rate estimating equations in Indian geriatric patients with cancer [SIOG 2023 abstract] J Clin Oncol 41 e24025 https://doi.org/10.1200/JCO.2023.41.16_suppl.e24025
78. Menon N, Patil VM, and Ramaswamy A, et al (2022) Caregiver burden in older Indian patients with cancer – experience from a tertiary care center J Geriatr Oncol 13(7) 970–977 https://doi.org/10.1016/j.jgo.2022.05.008 PMID: 35750629
79. Noronha V, Gattani S, and Ramaswamy A, et al (2021) SIOG2021-0128* – patients’ expectations from therapy and disclosure of diagnosis/ prognosis in older adults with cancer: a retrospective cohort study J Geriatr Oncol 12(Supplement 1) S22 https://doi.org/10.1016/S1879-4068(21)00369-6
80. Soni N, Banerjee J, and Saravanan M, et al (2022) Health-related quality of life in treatment-naive, older patients with cancer from India: a prospective observational study Cancer Res Stat Treat 5 474–481






