Predictors of Pap smear testing uptake among women in Lagos, Nigeria
Kehinde S Okunade1,2, Sarah John-Olabode3, Adebola A Adejimi4, Yusuf A Oshodi5,6, Benedetto Osunwusi2, Aloy O Ugwu2, Ayodeji Adefemi6 and Rose I Anorlu1,2
1Department of Obstetrics & Gynaecology, College of Medicine, University of Lagos, Surulere, Lagos, Nigeria
2Department of Obstetrics & Gynaecology, Lagos University Teaching Hospital, Surulere, Lagos, Nigeria
3Department of Haematology and Blood Transfusion, College of Medicine, University of Lagos, Surulere, Lagos, Nigeria
4Department of Community Health and Primary Care, College of Medicine, University of Lagos, Surulere, Lagos, Nigeria
5Department of Obstetrics & Gynaecology, Lagos State University College of Medicine, Ikeja, Lagos, Nigeria
6Department of Obstetrics & Gynaecology, Lagos State University Teaching Hospital, Ikeja, Lagos, Nigeria
Abstract
We assessed the predictors of Pap smear testing uptake within 6 months after cervical cancer prevention education among women in Lagos, Nigeria. This was a prospective follow-up study conducted as part of the ‘mHealth-Cervix trial’ in the two teaching hospitals in Lagos, Nigeria, between August 2020 and April 2021. Participants were followed up for 6 months after pre-enrolment cervical cancer prevention education. The potential socio-demographic and clinical predictors of Pap smear testing uptake during the 6-month follow-up were tested using the predictive model in a binary logistic regression analysis. Statistical significance was reported as p < 0.05. The rate of Pap smear testing uptake during the 6-month follow-up was 35.7%. Following the adjustments in the final multivariate analysis, participants’ previous awareness of Pap smearing (RR = 6.92, 95% CI: 8.37–56.68, p = 0.001) and attendance at the general outpatient clinic during the period of follow-up (RR = 11.22, 95% CI: 1.54–81.51, p = 0.017) independently predict Pap smear testing uptake. We will, therefore, explore the impact of continuous provision of health promotion on cervical cancer prevention and its effect in the context of routine clinical care in our next implementation research agenda. We recommend, in the meantime, that regular health education of women on cervical cancer prevention by healthcare providers should be further reinforced as an integral part of health promotion in clinics to reduce the burden of cervical cancer in most low- and middle-income settings.
Keywords: cervical cancer, health promotion, mHealth-Cervix, Nigeria, Pap smear uptake
Correspondence to: Kehinde Sharafadeen Okunade
Email: sokunade@unilag.edu.ng
Published: 31/03/2022
Received: 18/01/2022
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Cervical cancer is the most common cancer of the reproductive tract and a leading cause of cancer deaths among women in sub-Saharan African countries, including Nigeria [1]. An estimated 570,000 new cases of cervical cancer and over 300,000 related deaths were reported in 2018, with 70% of these deaths occurring in developing countries [2].
The incidence of the disease and its associated mortality have remained high in many resource-limited settings, due to the lack of organised regular screening programmes to detect and treat cervical precursor lesions [3].
Screening with Papanicolaou (Pap) smear has remained an effective public health intervention for reduction of the incidence and mortality of cervical cancer disease [4,5]. However, this is largely applied through opportunistic screening in most developing countries, including Nigeria, as payment for testing is usually done out of pocket [6–8]. This method is less effective as it targets only women who come in contact with healthcare providers for other reasons in the healthcare facility [6,9]. Furthermore, in areas with limited access to screening tests, various studies have also reported very low levels of Pap smear [5,8,10,11]. Approximately 50%–90% of the women who developed cervical cancer or died as a result of the disease have never been screened [6], and even more worrisome is that a large proportion of these women were never aware of cervical cancer or its available prevention strategies [5,12,13].
Several factors are reported to influence the uptake of Pap smear testing and these include a high level of education, reduced perception of risk of developing cervical cancer, lack of knowledge about the benefits of Pap smear and lack of familiarity with screening locations [7,14–16]. The healthcare providers also play a significant role in improving the knowledge of cervical cancer prevention and uptake of any of its screening methods [17]. This is because the previous lack of awareness due to the non-recommendation of Pap smear testing by healthcare practitioners is a major reason why women are unable to take up screening [17]. Therefore, this study will seek to improve cervical cancer screening awareness by providing pre-enrolment cervical cancer prevention education that highlights the benefits of Pap test screening in women. These women were followed up individually for 6 months to assess their willingness to return for Pap smear testing. The outcome of this study could be used to suggest effective strategies to improve the uptake of cervical cancer screenings aong women in Lagos, Nigeria.
Materials and methods
Study design and settings
This was a prospective follow-up study conducted as part of the ‘mHealth-Cervix trial’ [16]. The study involved women who attended the general outpatient (GOP) clinics of Lagos University Teaching Hospital and Lagos State University Teaching Hospital, Nigeria, between August 2020 and April 2021. These are the two foremost healthcare institutions in Lagos that serve as referral centres for other government-owned and private hospitals in Lagos and its neighbouring states. The hospitals provide a variety of care including integrated gynaecologic oncology prevention services such as Pap smearing, human papillomavirus testing and colposcopy services, including biopsy and histology. The GOP clinics in the participating hospitals are opened each day of the week and attendees are mainly the National Health Insurance Scheme enrollees who have routine Pap smear screening as part of their standard health insurance coverage [18].
Study population and eligibility criteria
The study participants were women in the control arm of the ‘mHealth-Cervix trial’ [16]. They were women aged 25–65 years without prior history of cervical premalignant or malignant lesions; those who have not had a Pap smear in the past 3 years; and those with sufficient physical and mental capacities to understand the purpose of the study. Women who were considering a change of residential relocation at any time in the following 6 months and those who failed to give consent at enrolment or withdrew their consent at follow-up were excluded from the study.
Study procedures and data collection
Initial health education on cervical cancer and its prevention was given to all women attending the GOP clinics as part of the usual health promotion programme. Eligible women from the clinics were subsequently identified and invited to enrol in the ‘mHealth-Cervix trial’ [16]. After obtaining their baseline socio-demographic and clinical information, the women were then followed up for 6 months as indicated in the control arm of the trial [16]. The women’s monthly income and educational status were used as independent determinants of their socio-economic status according to the classification by Yoon et al [19]. Participants’ tracking was via phone calls and/or review of medical records in the 6 months follow-up period. The study endpoints were the predictive effects of socio-demographic and clinical factors on Pap smear screening uptake during 6 months of follow-up.
Statistical methods
The sample size for the mHealth-Cervix trial [16] was calculated using G*Power for Windows version 3.1.9.2 (Kiel University, Germany). We extracted the data of the 100 women in the control arm of the trial to assess the influence of various socio-demographic and clinical factors on Pap smear testing uptake. Statistical analyses were carried out using SPSS version 27.0 for Windows (Armonk, NY: IBM Corp.). Descriptive statistics were presented as frequency (and percentage) and mean (± standard deviation) and the associations between categorical variables were tested using Pearson’s Chi-square (X2) test. Using the predictive model in a binary logistic regression analysis, we assessed the influence of various socio-demographic and clinical factors as predictors of Pap smear screening uptake. Statistical significance was reported as p-value < 0.05.
Ethical considerations
The Health Research Ethics Committee of the College of Medicine, University of Lagos, approved the mHealth-Cervix trial with approval number: CMUL/HREC/12/19/704. We applied the ethical principles of Helsinki during the study. Following counselling, participants read and signed an informed consent form before their enrolment in the study. Strict confidentiality of participants’ information was ensured during and after the completion of the study.
Results
Out of 100 women enrolled into the control arm of the mHealth-Cervix trial, 2 were lost to follow-up. As shown in Table 1, the mean age of the participants enrolled in the study was 38.0 ± 10.3 years and the mean residential location from the clinic was 15.1 ± 8.5 km. The participants were predominantly multiparous (n = 76, 77.6%), premenopausal (n = 77, 78.6%), married (n = 71, 72.4%), had at least secondary school education (n = 69, 70.4%) and of middle to upper income level (n = 59, 60.2%). A small proportion of the study participants were previously aware of Pap testing (n = 38, 38.8%), while an even smaller proportion had previously had Pap smear done (n = 27, 27.6%).
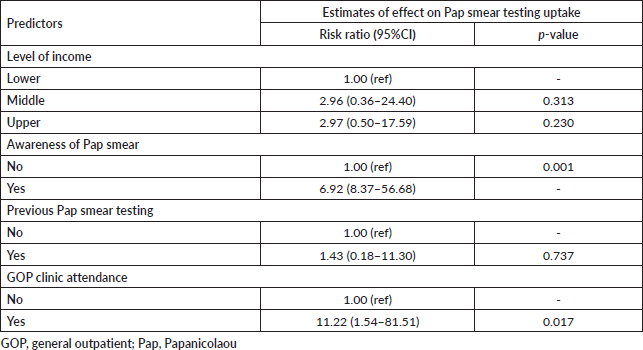
The Pap test uptake rate during the 6-month follow-up was 35.7% (n = 63) (Table 2). In the univariate binary logistic regression analysis, participants with middle- (p = 0.004) and upper-income (p = 0.003) levels, previous knowledge of Pap smear (p = 0.001), who had Pap smear testing in the past (p = 0.001) and those who attended the GOP clinics during the follow-up period for other various reasons (p = 0.001) were significantly more likely to have Pap smear testing. While keeping other covariates constant in the final multivariate model, participants’ previous awareness of Pap smearing (RR = 6.92, 95%CI: 8.37–56.68, p = 0.001) and GOP clinic attendance during their follow-up period (RR = 11.22, 95%CI: 1.54–81.51, p = 0.017) were the only independent predictors of Pap smear testing uptake in the study (Table 3).
Discussion
The Pap test uptake rate recorded in this prospective follow-up study was 35.7%, and we found that participants’ prior knowledge of Pap smear as a means of cervical cancer screening and their GOP clinic attendance during the period of follow-up were significant independent predictors of Pap smear screening uptake.
The mean age of the participants in the study (38.0 ± 10.3 years) was only slightly higher than the mean ages of 35.7 ± 9.74 years [20] and 35.9 ± 9.5 [14] recorded in our previous studies that assessed the knowledge of cervical cancer prevention among women in Lagos. These findings suggest that clinic attendees who willingly participate in such clinical research in our settings are of a relatively younger age group.
We recorded a Pap smear uptake rate of 35.7% in this study and this is much higher than the previous testing rate of 22.9% reported in a similar clinic setting in Lagos [14] and much higher than the 3.2% rate recorded by Ajenifuja et al [12] in Ile-Ife. The higher screening uptake in this study overemphasised the importance of cervical cancer prevention education, an integral component of complementary health promotion, provided to potential participants at enrolment in clinics on the overall improvement in the women’s health-seeking behaviour.
Table 1. Baseline characteristics of participants at enrolment (n = 98).a
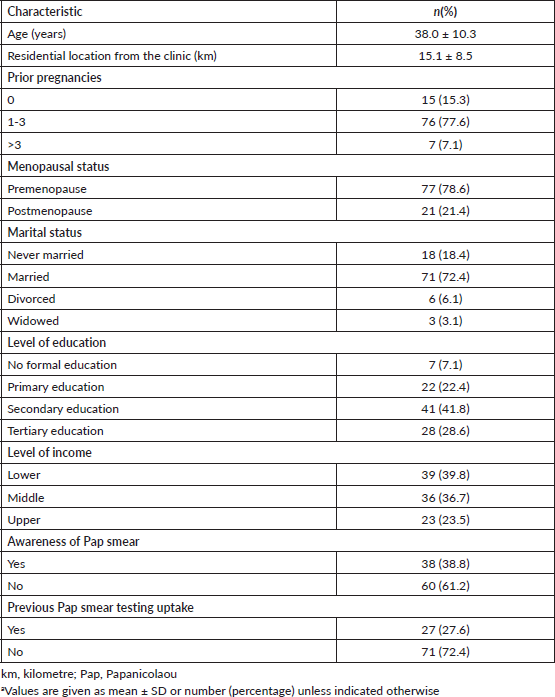
Table 2. Univariate analyses of socio-demographic and clinical predictors of Pap smear testing uptake after 6 months of follow-up (n = 98)
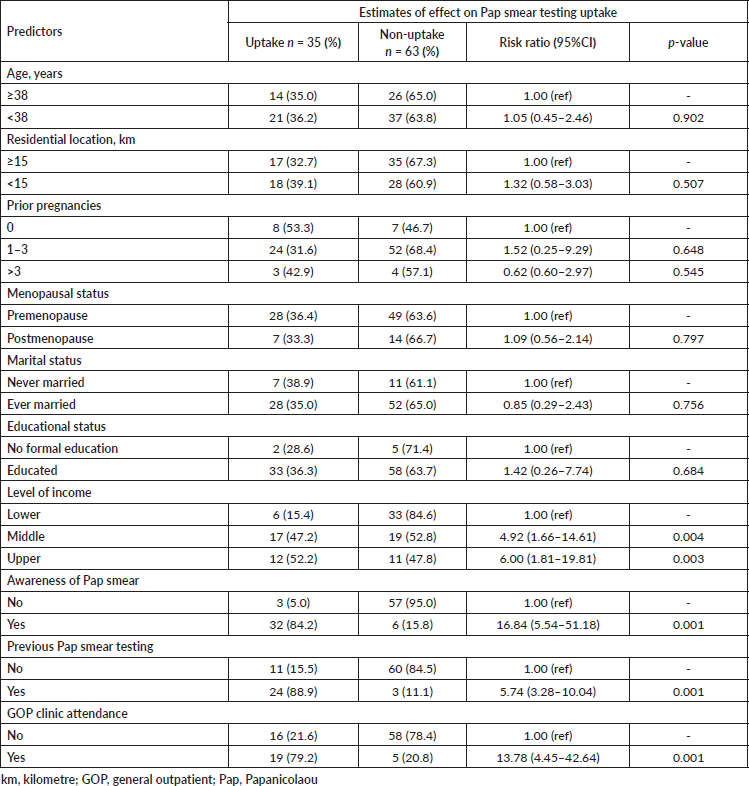
Table 3. Multivariate analyses of predictors of Pap test uptake after 6 months of follow-up (n = 98)
Our study revealed no impact of the distance of the women’s homes to the participating health facilities and their uptake of Pap smear testing, and this corroborated the findings of several other studies that found no relationship between distance to nearest facility and healthcare utilisation [21]. This showed that in most contexts, other barriers to access, such as an individual’s perception of the disease, social support, time availability and health decision autonomy, may even be more important factors that affect health-seeking behaviour [22]. Similar to other previous studies conducted in Africa [14,16,23], the attainment of any form of Western education did not positively influence the uptake of Pap smear testing in this study. However, another Nigerian study by Wright et al [13] reported that having a formal education is a significant predictor of uptake of cervical cancer screening. These contrasting findings suggest that education, despite being a vital tool in healthcare promotion, may not necessarily be the sole determinant of an individual’s health-seeking behaviour. Surprisingly, in the current study, participants’ income status has no association with Pap test uptake and this is in contrast to the findings reported from the total participants’ data in the mHealth-Cervix trial that reported that women in the middle- and upper-income statuses are significantly more likely to have Pap smear testing done [16]. This is because women of higher income levels are more financially empowered to access healthcare information and take healthcare decisions, leading to healthcare service uptake independent of any other factors.
Women with previous awareness of Pap testing showed an increased Pap smear uptake in the current study and this corroborated the findings from our previous study [16], which thus suggests that the provision of health education on cervical cancer prevention by healthcare professionals at any time in the regular clinics will reinforce previous knowledge of Pap smear screening which will further increase the likelihood of uptake of Pap testing among women. As GOP clinic attendance for various other reasons during the period of follow-up significantly influenced the Pap smear screening uptake among women in the study, it further suggests that the constraint for time usually pushes many individuals to use the opportunity of visiting the healthcare facilities during infirmities to seek other necessary and accessible healthcare prevention services [16].
The study is mainly limited in terms of generalisation as it was conducted within the hospital settings. In addition, the 6-month period adopted for follow-up in the study may be too short to assess the impact of long-term behavioural changes following the pre-enrolment health education on the real-world uptake of cervical cancer screening. Nevertheless, the data provide useful data on the potential factors that may predict women’s uptake of Pap smear screening after a routine and targeted cancer prevention education by healthcare providers in healthcare facilities in low- and middle-income settings.
Conclusion
In the cohort of participants from this current study, we reported that a woman’s prior knowledge of Pap smear testing and her attendance at the GOP clinic for other healthcare consultations had a positive influence on her Pap smear screening uptake. We will, therefore, aim to further explore the long-term impact of continuous health education and promotion on cervical cancer prevention and its effect in the context of routine clinical care. This will be introduced alongside methods to increase the flow of information and value of content for women in the real world and hospital settings. In the meantime, we recommend that regular health education on cervical cancer prevention be further reinforced as an integral part of complementary health promotion by healthcare providers in the clinics to reduce the overall high burden of cervical cancer incidence and deaths in most low- and middle-income settings.
Conflicts of interest
The authors have no conflicts of interest.
Acknowledgments
The authors appreciate all the women who voluntarily participated in this study. The authors are equally grateful to the clinical staff in the GOP clinics of all the participating hospitals for their invaluable roles in the enrolment process.
Funding declaration
This work was partly supported by the Fogarty International Centre of National Institutes of Health (Award Numbers D43TW010934, D43TW010134 and D43TW010543) and the Conquer Cancer International Innovation Grant (Project ID 16576). The views expressed by the authors are theirs alone and do not reflect the official views of the National Institutes of Health and the American Society of Clinical Oncology® or Conquer Cancer®.
Reference
1. Thomas J, Ojemakinde O, and Izebraye I (2002) Current concepts in cervical carcinogenesis and new perspectives in prevention Arch Ibadan Med 3(1) 36–39
2. Bray F, Ferlay J, and Soerjomataram I, et al (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries CA Cancer J Clin 68(6) 394–424 https://doi.org/10.3322/caac.21492 PMID: 30207593
3. Walboomers JM, Jacobs MV, and Manos MM, et al (1999) Human papillomavirus is a necessary cause of invasive cervical cancer worldwide J Pathol 189 12–19 https://doi.org/10.1002/(SICI)1096-9896(199909)189:1<12::AID-PATH431>3.0.CO;2-F PMID: 10451482
4. Peirson L, Fitzpatrick-Lewis D, and Ciliska D, et al (2013) Screening for cervical cancer: a systematic review and meta-analysis Syst Rev 2 35 https://doi.org/10.1186/2046-4053-2-35 PMID: 23706117 PMCID: 3681632
5. Bakari M, Takai IU, and Bukar M (2015) Awareness and utilization of Papanicolaou smear among health care workers in Maiduguri, Nigeria Niger J Basic Clin Sci 12 34–38 https://doi.org/10.4103/0331-8540.156682
6. Owoeye IOG and Ibrahim IA (2013) Knowledge and attitude towards cervical cancer screening among female students and staff in a tertiary institution in the Niger Delta Int J Med Biomed Res 2(1) 48–56 https://doi.org/10.14194/ijmbr.219
7. Toye MA, Okunade KS, and Roberts AA, et al (2017) Knowledge, perceptions and practice of cervical cancer prevention among female public secondary school teachers in Mushin local government area of Lagos State, Nigeria Pan Afr Med J 28 221 https://doi.org/10.11604/pamj.2017.28.221.13980
8. Udigwe GO (2006) Knowledge, attitude and practice of cervical cancer screening (Pap smear) among female Nurses in Nnewi, south-eastern Nigeria Niger J Clin Pract 9(1) 40–43 PMID: 16986288
9. Anorlu RI, Rabiu KA, and Abudu OO, et al (2007) Cervical cancer screening practices among general practitioners in Lagos Nigeria J Obstet Gynaecol 27(2) 181–184 https://doi.org/10.1080/01443610601124398 PMID: 17454471
10. Bukar M, Takai IU, and Audu BM (2012) Determinants of utilization of Papanicolaou’s smear among outpatient clinic attendees in Northeastern Nigeria Afr J Med Med Sci 41 183–189 PMID: 23185917
11. Oyebode TA, Sagay SA, and Ekwempu CC, et al (2006) The possible role of the gynaecologist in the poor awareness and non-utilization of the pap smear among female health workers Trop J Obstet Gynaecol 23 (Suppl 1) S20
12. Ajenifuja KO and Adepiti CA (2008) Knowledge of cervical cancer and utilization of Pap smear among patients in a tertiary centre in southwest Nigeria Ibom Med J 3(2) 56–60
13. Wright KO, Faseru B, and Kuyinu YA, et al (2011) Awareness and uptake of the Pap smear among market women in Lagos, Nigeria J Publ Health Afr 2 e14 https://doi.org/10.4081/jphia.2011.e14
14. Okunowo AA, Daramola ES, and Soibi-Harry AP, et al (2018) Women’s knowledge of cervical cancer and uptake of Pap smear testing and the factors influencing it in a Nigerian tertiary hospital J Cancer Res Pract 5(3) 105–111 https://doi.org/10.1016/j.jcrpr.2018.02.001
15. Leung SSK and Leung I (2010) Cervical cancer screening: knowledge, health perception and attendance rate among Hong Kong Chinese women Int J Womens Health 2 221–228 https://doi.org/10.2147/IJWH.S10724 PMID: 21072314 PMCID: 2971734
16. Okunade KS, Soibi-Harry A, and John-Olabode S, et al (2021) Impact of mobile technologies on cervical cancer screening practices in Lagos, Nigeria (mHealth-Cervix): a randomized controlled trial JCO Glob Oncol 7 1418–1425 https://doi.org/10.1200/GO.21.00258 PMID: 34554814 PMCID: 8478387
17. Al Sairafi M and Mohamed FA (2009) Knowledge, attitudes, and practice related to cervical cancer screening among Kuwaiti women Med Princ Pract 18 35–42 https://doi.org/10.1159/000163044
18. Okunade KS, Salako O, and Adejimi AA, et al (2020) Impact of mobile technologies on cervical cancer screening practices in Lagos, Nigeria (mHealth-Cervix): protocol for a randomised controlled trial F1000Res 9 322 https://doi.org/10.12688/f1000research.22991.1 PMID: 32528665 PMCID: 7265590
19. Yoon YS, Oh SW, and Park HS (2006) Socioeconomic status in relation to obesity and abdominal obesity in Korean adults: a focus on sex differences Obesity (Silver Spring) 14(5) 909–919 https://doi.org/10.1038/oby.2006.105
20. Okunade KS, Sunmonu O, and Osanyin GE, et al (2017) Knowledge and acceptability of human papillomavirus vaccination among women attending the gynaecological outpatient clinics of a University Teaching Hospital in Lagos, Nigeria J Trop Med 2017 8586459 https://doi.org/10.1155/2017/8586459
21. Kim ET, Singh K, and Speizer IS, et al (2019) Availability of health facilities and utilization of maternal and newborn postnatal care in rural Malawi BMC Pregnancy Childbirth 19 503 https://doi.org/10.1186/s12884-019-2534-x PMID: 31847872 PMCID: 6918704
22. Rutherford ME, Mulholland K, and Hill PC (2010) How access to health care relates to under-five mortality in sub-Saharan Africa: systematic review Trop Med Int Health 15 508–519 https://doi.org/10.1111/j.1365-3156.2010.02497.x PMID: 20345556
23. Ebu NI, Mupepi SC, and Siakwa MP, et al (2015) Knowledge, practice, and barriers toward cervical cancer screening in Elmina, Southern Ghana Int J Womens Health 7 31–39 PMID: 25565902 PMCID: 4284003






