Strengthening capacity for cancer research in conflict settings: key informant insights from the Middle East
Zahi Abdul-Sater1, Marilyne Menassa1, Nassim El Achi1, Rima A. Abdul-Khalek1, Ghassan Abu-Sittah1 and Deborah Mukherji2
1Global Health Institute, American University of Beirut, Beirut, Lebanon
2Naef K Basile Cancer Institute, Faculty of Medicine, American University of Beirut, Beirut, Lebanon
Abstract
Background: Management of cancer in the Middle East and North Africa (MENA) region is accompanied by multiple challenges including heterogeneous access to early detection and treatment options and limited implementation of national cancer control plans. Furthermore, protracted armed conflicts across the region have had dramatic effects, including disruption of healthcare systems and the migration of healthcare professionals. Strengthening capacity for cancer research has been identified as a key intervention to correct data poverty, inform policy, manage limited resources and improve health outcomes.
Objective: The main objective of this study is to gain insights into the landscape, barriers and enablers of cancer training, research and care in the MENA region.
Method: We utilised purposive sampling to interview 16 key informants from a diverse academic, medical and research background originating from countries affected by conflicts, such as Lebanon, and from active conflict zones including Iraq and Syria.
Results: The themes that emerged from the interviews focused on the barriers to cancer care, barriers to cancer research and training, strengths and importance of cancer research and training recommendations. The detrimental effect of conflict on cancer provision and research was a cross-cutting sub-theme disrupting cancer care provision and research due to unsafe environments, fragmented facilities, absence of drugs and migration of personnel. When asked about perceived optimal training format for cancer research, most informants recommended a post-graduate, face-to-face training focusing on cancer research methods and concepts.
Conclusion: This study offers a unique insight into the barriers affecting cancer research and capacity-strengthening priorities from oncologists and researchers working in conflict-affected areas of the MENA region. These data will form the base for future capacity-strengthening initiatives addressing specific regional challenges.
Keywords: cancer research, capacity strengthening, MENA region
Correspondence to: Deborah Mukherji
Email: dm25@aub.edu.lb
Published: 10/12/2020
Received: 31/08/2020
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background
The global cancer burden continues to rise in low- and middle-income countries (LMIC) (Table 1). By 2035, it is estimated that two-thirds of cancer cases will occur in developing countries, including countries in the Middle East and North Africa (MENA) region [1]. Multiple acute and chronic conflicts have affected the provision of cancer care services to populations in the MENA region and exacerbated existing challenges, including lack of universal health coverage, absent cancer control plans, inadequate human resource capacity and limited access to early detection and treatment options [2–7]. Furthermore, protracted armed conflicts across the region have directly led to mass migration and dismantlement of healthcare systems resulting in relative data poverty (Table 1) [13, 14].
Key mitigation strategies include multi-level interventions across the cancer care continuum, improving local health systems capacity, enhancing cancer registration and, importantly, generating contextually relevant data through research [15, 4]. Research plays an essential role in understanding disease burden, detecting geographical cancer patterns, assessing the success of interventions, addressing cancer health disparities and producing evidence-based health policies [16–18]. The relatively low regional research output in volume and quality has recently been highlighted [13]. Thus, it is imperative to mobilise individual, institutional, national and international efforts to strengthen cancer research capacity in conflict-affected MENA countries (Table 1). Against this backdrop, and to explore the factors affecting cancer research activity, we conducted key informant interviews (KIIs) aiming to understand the contextual landscape, barriers and enablers of cancer training, research and care. This work is part of the needs assessment phase of the Research for Health in Conflict in the Middle East and North Africa (R4HC-MENA) project efforts for capacity strengthening of cancer research in conflict settings within the MENA region [19].
Methods
Sampling and tools for data collection
A purposive sampling approach was used to identify key informants. We also employed a snowball sampling technique to help increase the number of respondents and used a semi-structured questionnaire to conduct face-to-face interviews with key informants. To establish a more holistic understanding of the impediments to cancer research, we interviewed key informants from various academic and clinical backgrounds, including oncology surgery, as well as individuals from non-governmental organizations (NGOs). Respondents originated from conflict-affected countries, including Lebanon, a refugee-host country, in addition to Syria and Iraq, both of which harbour active conflicts [20]. Participants were identified by the research team’s knowledge of cancer leaders in the three countries and the snowballing sampling method employed. At the end of the interviews, we asked the KIs to suggest key informant(s), who in their opinion could add valuable insights in line with the aims of the study. Interviews were done until data saturation was reached. Seventy-five informants were identified and sent invitations for interviews by e-mail, in English and Arabic, including a brief explanation of the rationale and aims of the study. Two reminder e-mails were sent to non-responders within two weeks of the first e-mail. Informants provided their consent through a form that was attached to the sent e-mail. Sixteen KIs responded to the email and were subsequently interviewed. The rest of the identified KIs did not respond to the emails we sent. At the start of each interview, verbal consent using the consent form for participating and recording the interview was obtained. Only one participant did not consent to recording the interview. On average, recorded interviews lasted 20 minutes.
After obtaining ethical approval from the American University of Beirut’s Institutional Review Board (IRB, Approval number: SBS-2018-0492) to conduct the interviews, a semi-structured guide was developed to gather contextual information on the clinical landscape, barriers and enablers of cancer training, research and patient care. Three researchers, ZAS, NEA and RAK, were involved in the interviewing process. ZAS and RAK developed the interview guide (supplemental document 1). The guide included six main questions that focused on (a) KIs’ perception of the individual and institutional barriers and enablers of cancer research and training and (b) the nature of training attended, given or recommended by the informants. The interview guide was developed in English and translated to Arabic by a certified translator and was piloted with 2 KIs and then revised. The interviews were conducted in English or Arabic, depending on the informant’s preference.
Table 1. Key definitions included in the manuscript text.

Data analysis
Interviews were transcribed verbatim and then read several times by the researchers for familiarity with the collected data and for establishing a general thematic tone. Two researchers (ZAS and NEA) independently coded two interviews and described the coding book accordingly. All discrepancies in the coding were discussed between them, and the codebook was revised as needed. After agreeing on the coding structure, the rest of the interviews were coded by ZAS. The interview data were managed using the NVivo 12 software (QSR International), and thematic analysis was performed, as previously described [21]. Upon coding the transcripts segments into inclusive themes, we developed more specific secondary and tertiary sub-themes. The thematic analysis was then revised and finalised by ZAS and NEA. Direct quotations from the key informants are presented in italics to support and highlight key themes and findings.
Results
A total of 16 key informant interviews were conducted either in person (14 interviews), by telephone (1 interview) or using Skype (1 interview) between February and July 2019. Thematic analysis of the interviews yielded a rich description of the three major themes. First, key informants provided a detailed description of contextual barriers and challenges of cancer training, research and patient care. Interviewees also discussed the strengths and importance of cancer research. Finally, they gave recommendations regarding capacity strengthening activities, including cancer research training (Figure 1).
Key informants demographics and training profile
The KIs interviewed had extensive research portfolios in cancer prevention, clinical research, cancer education and basic cancer biology (Figure 2). The interviews also provided information about the capacity strengthening activities that were attended by the key informants. Five KIs mentioned that they attended the training including workshops or courses on topics like research ethics during their PhD, medical training or post-medical training. Twelve KIs delivered capacity strengthening activities touching on research methods, cancer control, capacity strengthening, advocacy, radiation oncology, clinical trials research ethics, clinical practise management and surgery. The nature of the delivered activities varied among KIs but included seminars, courses, workshops, face-to-face training and programs. Two KIs mentioned that offering capacity strengthening activities free of charge, describing their importance and stressing the need for such activities motivated people to attend. The breadth of the research and training profiles of KIs ensures the relevance and value of their perceptions and recommendations to the current study.
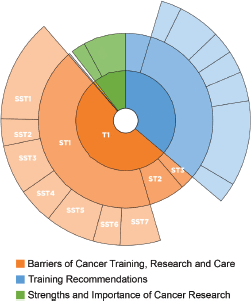
Figure 1. Hierarchical distribution of thematic analysis of Key Informant Interviews. Each colour represents a theme, which is dissected into sub-themes (ST) and sub-sub-themes (SST).
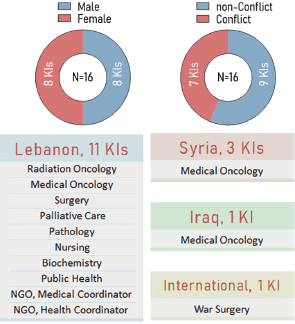
Figure 2. Key Informants’ profile, including gender, conflict status, country, and specialty distribution.
Barriers to cancer care in the MENA (Theme 1)
Analysis of interviews revealed cultural, logistical and financial barriers to optimal cancer care in the MENA.
Cultural barriers
Few key informants focused on patients’ perception of cancer as a cultural barrier to cancer care and hence research, including paternalistic approach when disclosing cancer diagnosis and lack of understanding of the value of multi-disciplinary, informed cancer care.
RID2: ‘Paternalistic approach’ whereby ‘the family or the head of the family must know before the patient’.’
RID4: ‘That people don’t understand the value of what we do even’ when it comes to palliative care’.
RID5: ‘Problems in the stigma, in understanding cancer in the population’.’
Logistical barriers
In Syria and Iraq, cancer care barriers were heavily influenced by the active conflict plaguing both countries. This included the absence of equipment and medications, travel difficulties and security issues.
RID11: ‘We used to have only one running machine, till the time of 2014 when ISIS invaded the city. Now, after liberation, that only machine is not working too’ and ‘many of the patients from….are either travelling to…or even to abroad to get treatment’.’
RID14: ‘Absence of ports…central lines…pumps’ due to economic sanctions and patients travelling ‘400-500 Km’ to get to a cancer care centre.
RID16: ‘Lack of drug. So, we give a patient a drug then we face a shortage of this drug. So, we would have to stop it,’ and ‘in Syria, we rely on auto-transportation. Sometimes the road is dangerous, and there could be kidnapping, you know... Our centre was in a hot spot... So, the patient can pass away because of a bullet you know or rocket’.’
Financial barriers
Few KIs detailed that financial difficulties prevent patients from accessing cancer treatment.
RID3: ‘Most people either cannot afford the hospitalization or cannot afford the treatment, and that includes both Lebanese and non-Lebanese.’
RID6: ‘The clinical challenges are mainly related to two issues. One is the economy of the country and the amount or the number of patients who do not afford clinically’.’
RID7: ‘The main barriers to delivering cancer care are financial, and patients access to treatments…mainly the challenges patients mainly who don’t have any sort of financial coverage and have only coverage from the Ministry of Health because cancer treatments are so expensive’.’
Interestingly, one KI mentioned that international NGOs operating in Lebanon, which provide limited support for cancer patients, face fundraising difficulties when it comes to cancer care since ‘support for cancer patients might not be sustainable’, given the high treatment cost and poor prognosis of some patients with cancer (RID12) [22, 3, 4].
Barriers of cancer research and training
Seven thematic barriers to cancer research were identified (Table 2). (1) Funding and support, which included a lack of financial resources and institutional support, were the most highly mentioned by interviewees. This was followed by (2) human resource capacity, which mainly focused on the lack of qualified personnel and insufficient research training. Importantly, KIs discussed the fragmentation of (3) facilities in Iraq and the lack of equipment and reagents in Syria. Furthermore, the (4) lack of research culture, including deprioritising cancer prevention, on the level of researchers, institutions and governments in countries of the MENA constituted the research culture barrier discussed by the KIs. Several key informants also reported difficulties in fostering (5) collaboration among institutions, organizations and countries. In addition to lack of collaboration, KIs highlighted multiple impediments that are related to (6) conflict, which included high patient drop-out rate due to the absence of drugs and personnel fleeing or affected directly by conflict-related violence. Lastly, international NGOs working for the benefit of the organization rather than the country was one of the (7) political economy barriers discussed. Example quotes of the aforementioned barriers are listed.
Barriers for conducting research training were similar to the research barriers and included insufficient time to conduct capacity strengthening activities, lack of funding and qualified personnel, and travel and safety issues due to conflict. Example quotes from two informants are found below.
RID4: ‘Time is the biggest one and probably cost, but time is a big barrier, especially people in practice have limited time’. ‘We have challenges in the prevention in Lebanon because the government prefers to pay money for drugs and treating people and not putting his money in prevention’.
RID9: ‘Let’s say Gaza today, students, who say I have a scholarship waiting for me in Europe or the United States. I don’t have a visa…I can’t get out of Gaza and then get back in. Yemen, if you are in Aden, you could get out, where the coalition, the Saudi coalition. But if you are in Sanaa, how…do you get out. It is not obvious, and once you are out, how do you get back in’.
Table 2. Thematic barriers of cancer research.
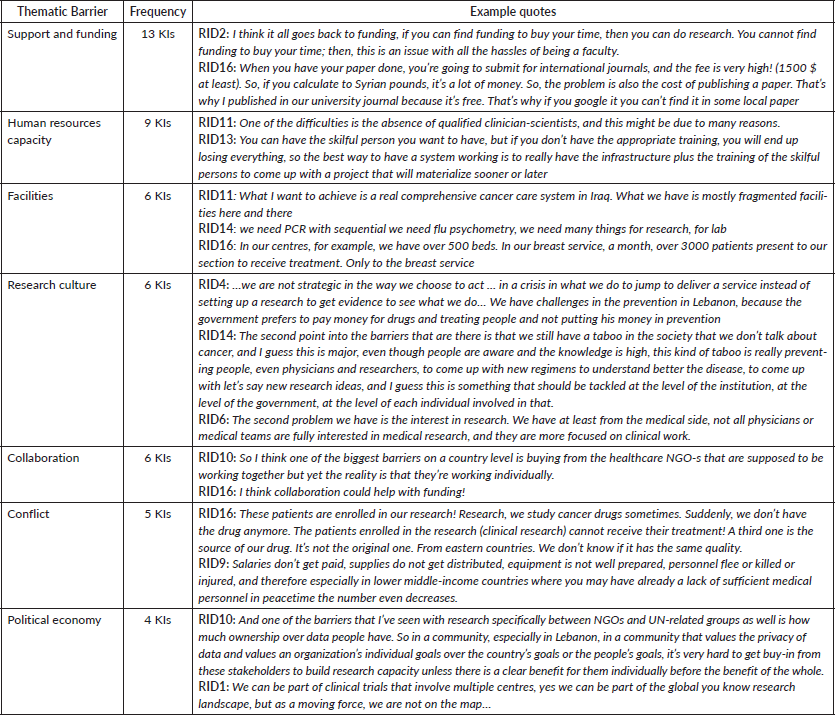
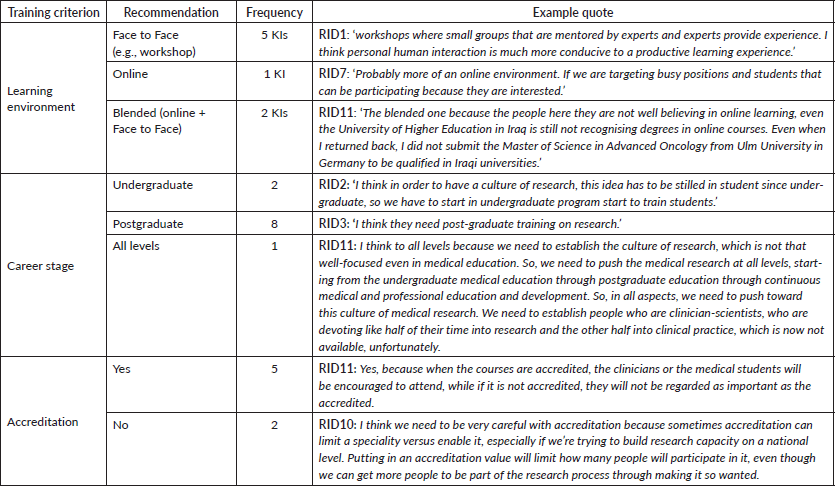
Table 3. Training recommendations by informants.
Strengths and importance of cancer research (Theme 2)
We extracted the perceptions of the strengths and importance of cancer research from the KIIs. Generally, KIs focused on the importance of research advancement in terms of incorporating research in the medical curricula, institutional support, availability of equipment and research capacity. Strikingly, all six informants who discussed research strengths were from well-known academic institutions in Lebanon. Examples highlighting the strengths of cancer research in the MENA include: ‘At the institution, I think we deliver decent level and decent amount because we have the quantity and quality of research’ (RID5) and ‘so I think Lebanon sort of does punch about its weight in terms of medical research in general and there is a lot of cancer research here’ (RID 7). The importance of cancer research in improving clinical practice, lowering treatment costs, shaping policy and disseminating knowledge was highlighted by five informants. For example, KIs mentioned that producing data is important to ‘get institutional support’ (RID4), provides ‘better understanding of our population may be of use of our population’ (RID4), ‘you prevent a disease it’s better than treating it. It’s less expensive, better outcome and better results’ (RID5); developing research stratified guidelines can help patients ‘to benefit from whatever they can get access to in the best cost-efficient way’ (RID7); not publishing research is like ‘training for the marathon and not crossing the finish line’ (RID1).
Training Recommendations (Theme 3)
Informants were then asked to provide recommendations about the structure and nature of research training that would be ideal to develop, given the strengths and challenges prevalent in conflict settings. The results are summarised in Table 3. Briefly, most KIs found that an accredited face-to-face training on the postgraduate level on a variety of research topics is the optimal combination for research training. The online learning environment was not recommended by informants because of lack of internet access or lack of recognition of online courses in their country. KIs also preferred to give these training on the postgraduate level, specifically during the medical residency training. The topics that were recommended by informants included having workshops and sessions discussing qualitative and quantitative research methods, statistical analysis and conceptualising research projects. Selected quotes from informants discussing their topics preference are listed below.
RID13: ‘I think a workshop that will tell these people how to start a good research project that will have an impact on the patient, it should be given, and that would entail a brief description of the importance of getting the appropriate clinical measures, the repository of biospecimen, the repository of diagnostic results including CTs and MRIs, and trying to do to force collaboration between people who are knowledgeable in all these’.
RID17: ‘Epidemiology, data collection, ethical issues…it’s very lacking in lots of places. Some basic statistical analysis, critical literature, forming guidelines’.
RID9: ‘The epidemiological is quantitative, but the functioning of a system for taking care of cancer patients is qualitative research, so you’re not involved in statistics and statistical analysis. You are involved in something else. You are involved in interviews and so forth and gathering other information. So, the epidemiological part is quantitative, but the system functioning is qualitative, and yes, people are given the basics’.
Informants also provided valuable insight into how to motivate KIs to attend research training. They detailed that accrediting the training, providing practical training instead of didactic presentations and providing opportunities for networking, publishing, joining research projects, receiving mentorship and funding would be useful ways to motivate KIs to attend such training. Relevant quotes from informants are listed below.
RID10: ‘You need to see the value of wise research importance. And I think one way that research is important to any healthcare professional is the fact that every guideline we have has come from some sort of research. So, making the courses appealing in terms of ‘understand your guidelines through research’ or ‘building upon the day to day work again tying it back to the research process’.’
RID17: ‘Probably, there had to be people interested, students, medical students, junior doctors have big motivation to publish and get involved in such projects. So, if you meet people by linking their mentors and projects, they can get involved’.
RID13: ‘Ask them to come up with their own questions so that they can discuss them in group and to see how we can implement these ideas in actual settings where you know we have the limited resources that you have and the limited budget that you have’.
Lastly, informants were asked about ways of sustaining recommended research training. Eight KIs gave answers that focused on making such training an institutional priority, fostering collaborations among professionals, incentivising researchers, providing support from the government, securing funding and ensuring satisfactory outcomes. An example quote is listed below.
RID2: ‘I think by creating collaboration among professionals, you would be able to sustain it. So, by having this link among different faculties from different universities would help to sustain this program of research, we can have a focus on oncology, and then we can have different sub-groups, and each group will be working on a topic, and then from there, you would generate more and more publications’.
Other forms of research capacity strengthening activities were also recommended by many KIs. The informants argued that capacity strengthening should extend beyond training or courses into strengthening capacity for systems in place. For example, one informant discussed strengthening capacity for cancer centres on how to create a fully functioning system for cancer care, starting with receiving patients. Furthermore, strengthening capacity for cancer registration through completing the records and unifying data entry was mentioned by two KIs from Syria. Lastly, one KI highlighted that training should not only be limited to medical doctors but should also extend to strengthening capacity for nurses and paramedics in cancer and cancer research in conflict settings. Example quotes are listed below.
RID10: ‘But, we really need to work on a research community in making the research more practical and more accessible. And that happens from an early design process of why are we even asking these questions, and why are we creating a document about research capacity, how is this really going to translate into something that’s going to better the community’s lives and better the individuals’ lives’.
RID13: ‘So, I understand when you are in the conflicting zone, you need to adapt to the environment, and one important thing is that you need to let alone all the major things that we can worry about and foster collaboration, so the first step is that we need to foster collaborations with existing institutions around the region so again we talk about Iraq and Syria, Lebanon will be a place, Jordan will be a place where they can help with, and the starting point you know is to train personnel using the system built-in these institutions in Jordan and Lebanon and try to align with their goals and standards so that at least you start building a system that will work there’.
Discussion
The underlying contextual landscape and barriers to health research in general, let alone cancer research, training and clinical care in conflict-affected MENA countries are not well understood [23, 24]. To this end, we sought to explore these barriers by conducting interviews with key informants working in conflict-affected environments in the region. The themes emerged from these interviews are in accordance with those listed in the conceptual framework designed by colleagues at R4HC-MENA for the capacity strengthening of health research in conflict-affected MENA countries (Table 2, [23]). However, even within these themes, there are specificities of cancer research, training and clinical care in such settings which are not captured in the framework and thus need to be highlighted.
For instance, KIs from Iraq and Syria examined the detrimental impact of conflict on the delivery of cancer care. This included inaccessibility of cancer care facilities due to blocked and unsafe roads, equipment and drug shortages due to economic sanctions and scarcity of cancer care centres. The impact of conflict on the provision of healthcare in Iraq is not new. The Iraqi health system was considered the best in the Middle East before 1980, but recurrent conflicts and economic sanctions, starting with the war against Iran to the civil war in 2014, have dismantled the health sector, including cancer care infrastructure and human capacity [25, 26]. In Syria, the recent civil war has caused a progressive increase in poverty and a decrease in healthcare provision, including cancer care. For example, essential cancer diagnostic and therapeutic tools like tomography scanners and radiation therapy only exist in Damascus and Latakia, which restricts access to millions of people under siege or in remote areas. When accessible, some services require out-of-pocket payment, which may be inaccessible to many given the loss of wealth endured by the Syrian population. These barriers result in a delay in early detection, diagnosis and treatment. Indeed, many reports document that most cancers emanating from many MENA countries are diagnosed at later stages and affect a younger population when compared to the world average [8–12]. This highlights the importance of contextualised strengthening of the capacity for cancer prevention in the MENA. Next, informants highlighted impediments for cancer research and training, which ranged from inadequate support and funding to weak human resource capacity, fragmented facilities, absence of research culture and weak collaborative efforts. Importantly, conflict-related barriers were also explored by KIs, and they included the sudden absence of drugs during research, lack of quality control over drugs and fleeing of personnel. These interviews highlight the unique nature of barriers experienced by oncologists and researchers in conflict settings to conduct research, attend training and deliver cancer care.
Strengthening capacity for cancer research through training workshops or courses should account for these contextual challenges. To this end, we asked informants to recommend the nature of capacity strengthening activities given the context of conflict. They recommended that an accredited face-to-face training on the postgraduate level on topics, including research methods, conceptualising research projects and statistical analysis, is the optimal combination for research training. Lastly, such activities should take into consideration existing capacity, which was also mentioned by informants from Lebanon, where research capacity is strong [13]. Previous studies aimed at understanding the need for courses to enhance research skills have been conducted in conflict-affected settings. Specifically, researchers at Birzeit University in Palestine have established the need for a capacity building course focused on mental and psychosocial health research [27]. Our study and the study by Birzeit University are an integral part of the contextualization of the assessment, success and sustainability of capacity strengthening in such settings. Indeed, setting research agendas in LMICs by international funders hinders capacity strengthening and promotes research that aligns with funders’ agenda rather than countries’ capacity needs [28–31]. This was also highlighted as a political economy barrier for cancer research by one of the key informants (Table 2).
It is crucial to consider the limitations of the study conducted. First, the results are limited to the key informants who agreed to be a part of the study and the sample may not be representative of all viewpoints. Many insights regarding the barriers and recommendations for cancer care and research might have been missed as a result. For example, it would have been important to interview employees in the public sector, especially at the Ministry of Public Health to highlight the barriers from the perspective of the health system as well. Second, KIs came from different academic and clinical backgrounds, and while this provides a more inclusive understanding of the aims of the study, it might weaken the study findings since their perception of the needs might be different and potentially conflicting.
Conclusions
Many studies aimed at understanding the needs for cancer care and research have been conducted within the MENA context and beyond [32, 18]. However, to our knowledge, this is the first study to explore, in depth, the needs and recommendations of oncologists and cancer researchers in conflict-affected settings. The study is a part of the need assessment phase of the cancer workstream within the R4HC-MENA project that aims to strengthen research capacity in conflict-affected areas. Importantly, this work is driven by countries within the conflict-affected MENA region, which is essential for ensuring the success of the capacity strengthening phase. It was found that barriers for cancer training, care provision and research in conflict-affected MENA countries are multi-faceted. Institutional, national and international efforts are sorely needed to alleviate the challenges facing cancer research and training in conflict settings in the MENA region. This work will serve as a primer for future R4HC project needs assessment initiatives focusing on identifying the training needs for cancer research in conflict-affected MENA countries. Upon finalising the needs assessment phase, we aim to launch evidence-based capacity strengthening activities for cancer research in the MENA region.
Author contributions
Substantial contributions to the conception or design of the work and/or the acquisition, analysis or interpretation of data for this work were done by ZAS and DM. Drafting the work or revising it critically for important intellectual content was done by all authors. Final approval of the version to be published was provided by all authors.
Acknowledgments
Dr Gladys Honein-AbouHaidar is acknowledged for her contribution to the methodology.
Conflicts of interest
The authors have no conflicts of interest to declare.
Ethics and consent
Ethical approval was obtained from the Institutional Review Board at the American University of Beirut (IRB approval number: SBS-2018-0492). All participants consented for being interviewed. Participants who were recorded gave their consent to being recorded.
Funding information
This publication is funded through the UK Research and Innovation GCRF Research for Health in Conflict in the Middle East and North Africa (R4HC-MENA) Project, developing capability, partnerships and research in the Middle and North Africa ES/P010962/1.
References
1. Cancer, International Agency for Research on. 2012 GLOBOCAN 2012: estimated cancer incidence, mortality and prevalence worldwide in 2012
2. Mateen FJ, Carone M, and Al-Saedy H, et al (2012) Cancer diagnoses in Iraqi refugees Acta Oncol 51(7) 950–951 https://doi.org/10.3109/0284186X.2012.667148 PMID: 22404173
3. El Saghir NS, de Celis ESP, and Fares JE, et al (2018) Cancer care for refugees and displaced populations: middle East conflicts and global natural disasters. Am Soc Clin Oncol Educ Book 38 433–440 https://doi.org/10.1200/EDBK_201365 PMID: 30231320
4. Spiegel P, Khalifa A, and Mateen FJ (2014) Cancer in refugees in Jordan and Syria between 2009 and 2012: challenges and the way forward in humanitarian emergencies Lancet Oncol 15(7) e290–e297 https://doi.org/10.1016/S1470-2045(14)70067-1 PMID: 24872112
5. Lyons G, Sankaranarayanan R, and Millar AB, et al (2018) Scaling up cancer care in the WHO Eastern Mediterranean Region East Mediterr Health J 24(1) 104–110 https://doi.org/10.26719/2018.24.1.104 PMID: 29658627
6. Bray F (2014) Transitions in human development and the global cancer burden World Cancer Rep 54–68.
7. Bray F and Møller B (2006) Predicting the future burden of cancer Nat Rev Cancer 6(1) 63 https://doi.org/10.1038/nrc1781
8. Arafa MA, Rabah DM, and Farhat KH (2020) Rising cancer rates in the Arab World: now is the time for action East Mediterr Health J 26(6) 638–640 https://doi.org/10.26719/emhj.20.073 PMID: 32621496
9. Jazieh AR, Algwaiz G, and Alshehri SM, et al (2019) Lung Cancer in Saudi Arabia J Thorac Oncol 14(6) 957–962 https://doi.org/10.1016/j.jtho.2019.01.023 PMID: 31122559
10. Salim EI, Moore MA, and Al-Lawati JA, et al (2009) Cancer epidemiology and control in the arab world-past, present and future Asian Pac J Cancer Prev 10(1) 3–16 PMID: 19469617
11. Elobaid Y, Aw T-C, and Lim JNW, et al (2016) Breast cancer presentation delays among Arab and national women in the UAE: a qualitative study SSM-Population Health 2 155–163 https://doi.org/10.1016/j.ssmph.2016.02.007 PMID: 29349136 PMCID: 5757829
12. Al-Jaber A, Al-Nasser L, and El-Metwally A (2016) Epidemiology of oral cancer in Arab countries Saudi Med J 37 (3) 249 https://doi.org/10.15537/smj.2016.3.11388 PMID: 26905345 PMCID: 4800887
13. Hamadeh RR, Borgan SM, and Sibai AM (2017) Cancer Research in the Arab World: a review of publications from seven countries between 2000-2013. Sultan Qaboos Univ Med J 17(2) e147–e154 https://doi.org/10.18295/squmj.2016.17.02.003 PMID: 28690885 PMCID: 5488814
14. Arnold LD, Barnoya J, and Gharzouzi EN, et al (2014) A training programme to build cancer research capacity in low- and middle-income countries: findings from Guatemala Bull World Health Organ 92(4) 297–302 https://doi.org/10.2471/BLT.13.126516 PMID: 24700998 PMCID: 3967575
15. Spiegel, Paul B, and Checchi F, et al (2010) Health-care needs of people affected by conflict: future trends and changing frameworks Lancet 375(9711) 341–345 https://doi.org/10.1016/S0140-6736(09)61873-0 PMID: 20109961
16. Syrimi E, Lewison G, and Sullivan R, et al (2020) Analysis of global pediatric cancer research and publications JCO Glob Oncol 6 9–18 https://doi.org/10.1200/JGO.19.00227 PMID: 32031437 PMCID: 7000229
17. Abudu RM, Cira MK, and Pyle DHM, et al (2019) Landscape of global oncology research and training at national cancer institute–designated cancer centers: results of the 2018 to 2019 global oncology survey J Glob Oncol 5 1–8 PMID: 31756139 PMCID: 6882505
18. Kilic B, Phillimore P, and Islek D, et al (2014) Research capacity and training needs for non-communicable diseases in the public health arena in Turkey BMC Health Serv Res 14(1) 373 https://doi.org/10.1186/1472-6963-14-373 PMID: 25193671 PMCID: 4165910
19. R4HC-MENA [https://r4hc-mena.org/]
20. Malmvig H and Dreyer J (2020) Immanent Conflict Without Immanent War: Local Actors and Foreign Powers are Scrabbling for Influence in Iraq and Syria (København: Danish Institute for International Studies)
21. Braun V and Clarke V (2006) Using thematic analysis in psychology Qual Res Psychol 3(2) 77–101 https://doi.org/10.1191/1478088706qp063oa
22. UNHCR (2015) UNHCR Global Trends Forced Displacement in 2014 (Geneva, Switzerland: UNHCR)
23. El Achi N, Papamichail A, and Rizk A, et al (2019) A conceptual framework for capacity strengthening of health research in conflict: the case of the Middle East and North Africa region Global Health 15(1) 1–15 https://doi.org/10.1186/s12992-019-0525-3
24. Bowsher G, Papamichail A, and El Achi N, et al (2019) A narrative review of health research capacity strengthening in low and middle-income countries: lessons for conflict-affected areas Global Health 15(1) 23 https://doi.org/10.1186/s12992-019-0465-y PMID: 30914049 PMCID: 6434620
25. Mula-Hussain L (2015) Cancer in a war-torn Arab community-Iraq: description of its trends [A review] 7th International Conference on Health Issues in Arab Communities ACCESS Health Journal
26. Mula-Hussain L (2019) War and Its consequences for cancer trends and services in Iraq War and Health: The Medical Consequences of the Wars in Iraq and Afghanistan vol 4 p 172 https://doi.org/10.18574/nyu/9781479875962.003.0009
27. Rita G, Hammoudeh W, and Kienzler H, et al (2018). Training Needs Assessment for Mental Health Research in War and Conflict
28. Costello A and Zumla A (2000) Moving to research partnerships in developing countries BMJ 321(7264) 827–829 https://doi.org/10.1136/bmj.321.7264.827 PMID: 11009530 PMCID: 1118627
29. Kok MO, Rodrigues A, and Silva AP, et al (2012) The emergence and current performance of a health research system: lessons from Guinea Bissau Health Res Policy Syst 10(1) 5 https://doi.org/10.1186/1478-4505-10-5 PMID: 22321566 PMCID: 3295730
30. Sitthi-amorn C, Reeder JC, and Simon J, et al (2000) Strengthening health research capacity in developing countries: a critical element for achieving health equityCommentary: health research and human development in Papua New GuineaCommentary: does strengthening research capacity improve health equity? BMJ 321(7264) 813 https://doi.org/10.1136/bmj.321.7264.813 PMID: 11009525 PMCID: 1118622
31. Franzen SRP, Chandler C, and Lang T (2017) Health research capacity development in low and middle income countries: reality or rhetoric? A systematic meta-narrative review of the qualitative literature BMJ Open 7(1) e012332 https://doi.org/10.1136/bmjopen-2016-012332 PMID: 28131997 PMCID: 5278257
32. Barratt H and Fulop NJ (2016) Building capacity to use and undertake research in health organisations: a survey of training needs and priorities among staff BMJ Open 6(12) e012557 https://doi.org/10.1136/bmjopen-2016-012557 PMID: 27927657 PMCID: 5168601
33. World Bank (2017) World Bank Country and Lending Groups (Washington (DC): World Bank Data Help Desk)
34. Bates I, Akoto AYO, and Ansong D, et al (2006) Evaluating health research capacity building: an evidence-based tool PLoS Med 3(8) https://doi.org/10.1371/journal.pmed.0030299 PMID: 16942394 PMCID: 1502158
35. Pettersson T and Wallensteen P (2015) Armed conflicts, 1946–2014 J Peace Res 52(4) 536–550 https://doi.org/10.1177/0022343315595927
36. World Bank (2020) Classification of Fragile and Conflict-Affected Situations. 2020 The World Bank [https://www.worldbank.org/en/topic/fragilityconflictviolence/brief/harmonized-list-of-fragile-situations] Date accessed: 20/04/20
37. Azar EE, Jureidini P, and McLaurin R (1978) Protracted social conflict; theory and practice in the Middle East J Palestine Stud 8(1) 41–60 https://doi.org/10.2307/2536101
38. El-Erian MA and Fischer S (2000) Is MENA a region? The scope for regional integration Economic and Political Impediments to Middle East Peace (Berlin: Springer) pp 70–86 https://doi.org/10.1057/9780333994269_5






