A nationwide pilot study on breast cancer screening in Peru
Jhajaira M Araujo1,2, Andrea C Gómez1, Winston Zingg-De Jongh3, Jhon Ausejo4, Iván Córdova4, Luis J Schwarz4, Denisse Bretel5, Williams Fajardo6, Luis G Saravia-Huarca7, Joshuan Barboza-Meca8, Zaida Morante1, Juan R Guillén9, Henry Gómez5, Nadezhda K Cárdenas4, Lady Hernández4, Walter Melo4, Cynthia Villarreal-Garza10, Christian Caglevic11, Carolina Palacio12, Héctor García13, Gerson Mejía14, Claudio Flores1, Carlos Vallejos1 and Joseph A Pinto1,4
1Centro de Investigación Básica y Traslacional, AUNA-Ideas, Guardia Civil 571, San Borja, Lima 16036, Peru
2Escuela Profesional de Medicina Humana, Universidad Privada San Juan Bautista, Chorrillos, Lima 15067, Peru
3Department of Molecular and Cellular Medicine, Texas A&M University, TX 77843, E.E.U.U., USA
4Escuela Profesional de Medicina Humana-Filial Ica, Universidad Privada San Juan Bautista, Ica 11004, Peru
5Grupo de Estudios Clínicos Oncológicos Peruano (GECOPERU), Santiago de Surco, Lima 15038, Peru
6Servicio de Medicina Interna, Hospital Nacional Dos de Mayo, Lima 15003, Peru
7Servicio de Medicina Interna, Hospital Regional de Ica, Ica 107, Peru
8Universidad Norbert Wiener, Lima 15046, Peru
9Hospital Félix Torrealva Gutiérrez- ESSALUD, Ica 11001, Peru
10Centro de Cáncer de Mama, Hospital Zambrano Hellion, Tecnológico de Monterrey, 66278 San Pedro Garza García, Monterrey, México
11Cancer Research Department, Fundacion Arturo Lopez Perez, Santiago de Chile 7500921, Chile
12Departamento de Oncología Clínica, Instituto de Cancerología Las Américas - AUNA, Medellín 050022, Colombia
13Facultad de Medicina, Universidad de Antioquia, Medellín 050010, Colombia
14Departamento de Oncología Médica, Hospital Clínico VIEDMA, Cochabamba 0304, Bolivia
Abstract
Introduction: A high prevalence of advanced breast cancer (BC) is a common scenario in Latin America. In Peru, the frequency of BC at Stages III/IV is ≈50% despite implementation of a programme for breast cancer screening (BCS) along the country. We carried out a study to assess the feasibility and develop an instrument to evaluate the knowledge, barriers and perception about BCS in a nationwide pilot study in Peru among candidates for BCS.
Methods: We conducted a systematic review of 2,558 reports indexed in PubMed, Scopus, Web of Science, Medline-Ovid and EMBASE, regarding to our study theme. In total, 111 were selected and a 51-items survey was developed (eight items about sociodemographic characteristics). Patients were recruited in public hospitals or private clinics, in rural and urban areas of nine departments of Peru.
Results: We surveyed 488 women from: Lima (150), Cajamarca (93), Ica (59), Arequipa (56), Loreto (48), Ancash (38), Junín (15), Puerto Maldonado (15) and Huancavelica (14); 27.9% of them were from rural areas. The mean of age was 53.3 years (standard deviation ± 9.1). Regarding education level, 29.8% had primary, 33.2% secondary and 37.0% higher education. In total, 28.7% of women did not know the term ‘mammogram’ and 47.1% reported never receiving a BCS (36.9% from urban and 73.5% from rural population). In women that underwent BCS, only 67% knew it is for healthy women. In total, 54.1% of patients had low levels of knowledge about risk factors for BC (i.e. 87.5% of women respond that injuries in the breast produce cancer). Cultural, economic and geographic barriers were significantly associated with having a mammogram where 56.9% of participants considered a cost ≤ 7 USD as appropriate. Mammogram was perceived as too painful for 54.9% of women. In addition, women with a self-perception of low-risk for BC and a fatalistic perception of cancer were less likely to have a BCS.
Conclusion: We found that it is feasible to conduct a large-scale study in Peru. The results of this pilot study highlight an urgent need of extensive education and awareness about BCS in Peru.
Keywords: breast cancer, health knowledge, attitudes, practice, breast neoplasms/diagnosis, breast neoplasms/prevention & control
Correspondence to: Joseph A Pinto
Email: joseph.pinto@auna-ideas.org
Published: 09/01/2023
Received: 22/08/2022
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Cancer is generally thought to be a predominant disease in developed nations. However, for breast cancer (BC), 50% of cases and 58% of deaths occur in developing nations [1]. Although the incidence is evenly split between developed and developing nations, the latter experience a much greater mortality rate. Some of the causes for the discrepancy in the mortality rate are lack of early detection, inadequate diagnosis and sub-par treatment facilities [2].
In 2013, according to the American Cancer Society, 21.77% of BC diagnosis found the cancer in situ. A remarkably high number, highlighting the advance screening process and public awareness in the United States. As for the diagnosis of invasive cases, the Surveillance, Epidemiology and End Results Programme reported that from 2013 to 2017, 64.71% of cases were of localised BC, 27.52% of cases were of regional cancer, 5.7% were distant cases and 2.07% of unstaged diagnosis. This data demonstrates a high amount of early diagnosis per incidence rate in the United States, aiding the low mortality rate present in the country [3].
Latin America presents a more severe situation. According to Global Cancer Observatory (GLOBOCAN) 2020, the mortality-per-incidence (MPI) ratio for BC in Peru, Chile and Ecuador’s is 0.27, 0.31 and 0.30, respectively. Although the other countries in Latin America present improved ratios, none are close to United States’ MPI (0.18) [4].
Peru has a high prevalence of advanced BC, approximately 50% of cases are at stage III/IV [1]. The primary factors associated to late diagnosis are lack of awareness, misconceptions about BC causes and treatment outcomes, social status and educational level [5, 6]. Besides, the guidelines should take into consideration the public knowledge, and social and cultural barriers in order to implement better strategies that motivate women to undergo screening [7, 8]. Detecting BC cases in early stages has demonstrated to be detrimental for a low MPI. Countries such as Sweden, Norway, the United States and the UK present high percentiles regarding the early detection of BC and consequently, low mortality per case [9, 10]. Improvements on early detection for BC would improve Peru’s MPI since patients could receive timely treatment and improve their prognostic.
In order to further understand methods to improve Peru’s BC MPI, a study was conducted to evaluate women’s knowledge, attitude and barriers regarding BC and breast cancer screenings (BCS).
Methods
Study design
We conducted an observational, descriptive, transversal and nationwide pilot study to evaluate the level of knowledge, barriers and attitudes of Peruvian women regarding BCS.
Study population and sample size
The study population included Peruvian women from 40 to 70 years old. The sample size of a minimum of 385 women was calculated with an expected proportion at 50% (worst-case scenario), 95% confidence and 5% margin of error using the Epidat 3.1 program. The sample was stratified to represent the access to the different types of insurance, Integral Health Insurance (SIS) 60%, Social Health Insurance (ESSALUD) 30% and private clinics 10%; as well as the distribution of the population in the evaluated departments.
In total, 488 participants were surveyed in nine departments that represent the north, middle and south of the country as well as the coastal, Andean and Amazonian regions, in national and private institutions. The departments were Lima, Cajamarca, Ica, Arequipa, Loreto, Ancash, Huancavelica, Junín and Madre Dios. The survey was conducted during September and October 2019.
Selection criteria
We included women from 40 to 70 years old at the moment we applied the survey and, women with no current or past diagnosis of BC. On the contrary, we excluded women who go to a hospital with a BC patient, women with a condition that prevents them from reading the informed consent and, women who underwent unilateral or bilateral mastectomy for any reason.
Survey design
We use the Rayyan QCRI platform (https://rayyan.qcri.org/welcome) to conduct a systematic review on PubMed, Scopus, Web of Science, Medline-Ovid and EMBASE; our strategy of search is on Supplementary Table 1.
We found 2,558 reports that assess the level of knowledge, barriers, attitudes or other aspects of BCS. We excluded case reports, editorials, narrative reviews and meta-analysis. Finally, 111 studies were selected.
We evaluated each of the selected studies and made a list of questions. Duplicate questions were removed and the remaining were sorted into categories: knowledge about BC, knowledge about BCS, barriers and attitudes. The list was evaluated by experts on the field and they decided which question was included or excluded. The final version of the survey was validated through Expert Judgement (two oncologists and a primary health care physician) and included 43 questions. Some questions were culturally adapted to be easily understood in Peru as for example, in the question about the suggested cost of the mammogram, the possible answers were in soles (Peruvian currency) instead of dollar.
In addition, we collected information about sociodemographic variables such as age, city of residence, residence at an urban or rural area, marital status (single, married/live-in partner and divorced/separated/widow), children (yes or no), level of education (primary or less, secondary and higher), employment status (unemployed, employed and retired) and type of insurance (SIS, ESSALUD or Armed forces, and private).
Statistical analysis
Measures of central tendency and measures of dispersion were evaluated for quantitative data while frequencies and percentages were estimated for categorical data. The internal consistency of the questionnaire was evaluated according to the nature of each question; for questions about barriers and attitudes, the Cronbach’s alpha was used. Statistical analyses were performed using Statistical Package for the Social Sciences (SPSS®) software ver. 24.0 (IBM®, Armonk, NY, USA).
Results
General characteristics
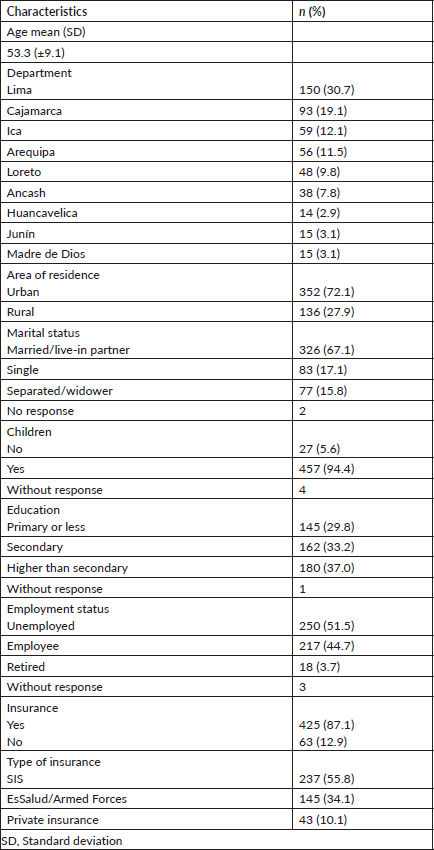
In total, 488 women accepted to participate in the study; 30.7% were from Lima and 72.1% lived in an urban area. The mean of age was 53.3 (standard deviation: ± 9.1). Most of them were married or had a live-in partner (67.1%), and had children (93.6%). Regarding educational level, 37.0% had higher education. About half of participants were unemployed (51.2%) and 12.9% did not have any insurance (Table 1).
The internal consistency of the barriers and attitudes sections was good (Cronbach’s alpha: 0.793 and 0.779, respectively).
Table 1. Demographic characteristics of surveyed women (n = 488).
Knowledge about BC and BCS
Most of the participants incorrectly believed that a breast injury can cause cancer (86.5%), and that start of menstruation before 12 years old was not a risk factor for BC (67.7%). In contrast, 84.4% were aware that having family history of BC increased their risk (Figure 1).
In total, 28.7% of women were unfamiliar with the term ‘mammogram’ and 47.1% never had a BCS (36.9% from urban and 73.5% from rural population). In women that underwent BCS, 67% knew it is for healthy women.
Barriers
The most frequent reason to avoid mammogram was fear of the results (58.2% strongly agreed). For 39.6%, cost was an impediment to underwent screening and 44.5% reported that they never remember to make an appointment.
About half of patients (51.0%) preferred that a woman performed the exam and believed that mammogram was painful (48.8%). In addition, 37.5% considered that they had more important problems than getting a mammogram; 32.6%, that the staff are not very sensitive; 29.3%, that mammogram exposes them to unnecessary radiation; 20.3%, that they were too old to need examination and 17.5% that mammogram requires too much time.
Also, 30.2% of participants did not know what to do to get a mammogram, 29.7% were afraid because they did not know what to expect during the exam and 24.9% said that the felt ashamed of having a mammogram.
In total, 17% of women reported that their spouses did not like that a physician checked their breast.
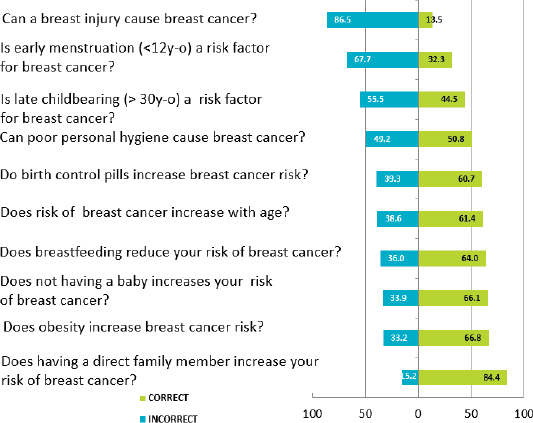
Figure 1. Knowledge about BC.
Attitudes
Regarding attitudes towards BCS (Figure 3), most of the participants strongly disagreed with the questions. However, 35.9% said that they preferred a breast ultrasound instead of mammogram, 35.3% think that there is no cure for cancer, 27.1% prefer not to know if they had BC and 20.1% believe that mammogram can cause cancer.
Remarkably, some women think that screening is not necessary since they do not have pain (25.7%), believe that they are at low risk (25.4%) and do not have any changes in their breasts (22.6%).
Discussion
In this study, we explore the knowledge, barriers and attitudes of Peruvian women towards BCS. Although several efforts to enhance early detection of this neoplasm have been conducted, it is necessary to characterise our population in order to establish better strategies.
Our study revealed some misconceptions about risk factors for BC. Surprisingly, 86.5% of participants believed that a breast injury and poor hygiene (49.2%) can lead to BC. Also, 67.7% and 55.5% of women did not know that early menarche (before 12 years old) and bearing a first child after 30 years of age, respectively, increase the risk of BC. Educational campaigns are critical to educate our population and promote awareness of BC risk factors. Similar results were found in studies that included Hispanic and Jordanian women (Figure 2) [11, 12].
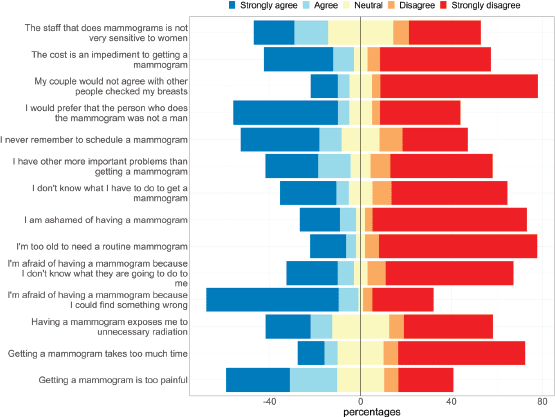
Figure 2. Barriers towards BCS.
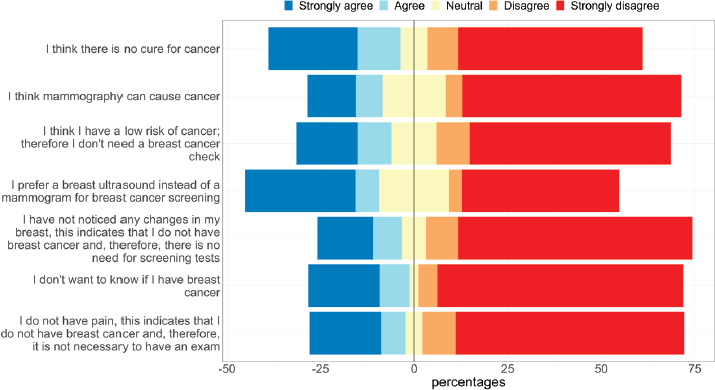
Figure 3. Perceptions towards BCS.
Regarding reasons why women prefer not to undergo BC screening, most of them were related to lack of knowledge about mammogram; such as considering that mammogram was painful or that it exposes them to excessive radiation. Misinformation about cancer screening and fear are critical factors that affect a considerable percentage of the target population. Therefore, it is crucial to improve patient education and clinicians and healthcare workers may play an important role in this movement [13].
An initiative similar to the Yo me cuido® Program could be carried out in Peru. This programme was initiated by the Moffitt Cancer Center to educate the Hispanic population living in the USA. The follow-up for mammography screenings showed that 52% of women had a screening mammogram within their first year after participating in the programme [14].
Another important factor to consider is the socioeconomic status; for 39.6%, cost was an impediment to undergo screening and, although it was not a question in the survey, participants living in the provinces manifest that the hospitals did not have the equipment and they were obligated to travel to other cities or visit private clinics if they wanted to have access to BCS. A study showed that Peruvian women with a higher level of education, higher wealth quintile and those from the capital city underwent screening mammogram in higher proportions; also, in a multivariate analysis, the highest wealth index quintile (prevalence ratio: 5.75; 95% confidence interval: 2.97–11.15) compared to the lowest quintile, was significantly associated with having a mammogram [15].
Unfortunately, Peruvian women still consider that if they do not have pain (25.7%) or any changes in their breast (22.6%), then they do not need to undergo screening, and 20.1% believe that a mammogram can cause cancer. Also 35.9% believed that there is no cure for cancer and 27.1% prefer not to know if they had cancer. This seems to be a frequent scenario in low-middle income countries. In Western Kenya, most of the interviewed women considered breast cancer a fatal disease and declared that they were afraid of having a mammogram because of a positive result [8]. In Ghana, the mean length of delay to attend diagnosis since presentations of sign or symptoms was 1.2 years, with a range of 2 weeks to 4 years. The main reasons were fear of mastectomy due to stigma, religion, myths and misconceptions about BC, no association between a painless breast lump with BC and financial reasons [16]. In Pakistan, 26% of the evaluated women reported that the reasons for delay in presentation were anxiety, fear and misconceptions about BC diagnosis and treatment and other social factors such as socioeconomic status and a negative impact on their relationship with their husband [17].
Altogether, these aspects may be the explanation as to why in Peru, most women are diagnosed when they manifest symptoms (93%) and only 6% by mammogram screening and 1% during screening clinical breast examination [18]. According to the Demographic and Family Health Survey (ENDES, in Spanish) 2017, only 17.1% of women between 40 and 59 years had a mammogram in the year prior to the survey; figures considerably lower compared to other countries where 50%–80% of the target population had had a mammogram [19–21].
Despite efforts from the Ministry of Health, a great proportion of cases are diagnosed in advanced stages. An analysis of patients diagnosed and treated at the Instituto Nacional de Enfermedades Neoplasicas (INEN) has shown that 35.9% of BC patients were stages III or IV at diagnosis in 2000–2002; that figure did not significantly change in the 2010–2012 period, where 36.7% were diagnosed with advanced BC [22, 23]. However, a recent study, conducted during the COVID-19 pandemic, has shown that 55.4% of cancer patients diagnosed and treated during 2019–2020 had an advanced stage [24]. In addition to the negative impact of COVID-19, the Peruvian healthcare system’s inequities have worsened BC early detection. Many women had to postpone their visit to oncological centres since they could not travel to the big cities where the facilities are located, or could not access telemedicine since they did not have Internet connection; therefore, diagnosis was postponed and mortality rates have increased [25, 26].
This study has some limitations. Because of its descriptive design, we cannot determine factors associated with the evaluated aspects in the study. However, our results are critical for a better design of strategies to encourage women to undergo BCS, especially considering that the COVID-19 pandemic has had a negative impact on cancer diagnosis.
Conclusion
We found that it is feasible to conduct a large-scale study in Peru. The participants had misconceptions about BC and BCS. The results of this pilot study highlight an urgent need for extensive education and awareness about BCS in Peru.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Funding statement
The study was funded by Oncosalud-AUNA.
Author contributions
JMA: Methodology, formal analysis, investigation, data curation, writing – original draft, writing – review & editing, visualisation, project administration; ACG: Investigation, data curation, writing – original draft; WZDJ: Investigation, data curation, writing – original draft; JA: Investigation; IC: Investigation; LJS: Data curation; DB: Data curation; WF: Investigation; LGSH: Investigation; JBM: Methodology; ZM: Investigation; JRG: Investigation; HG: Conceptualisation; NKC: Investigation; LH: Investigation; WM: Investigation; CVG: Writing – review & editing; CC: Writing – review & editing; CP: Writing – review & editing; HG: Writing – review & editing; GM: Writing – review & editing; CF: Methodology; CV: Conceptualisation; JAP: Conceptualisation, methodology, formal analysis, supervision, funding acquisition.
References
1. Cazap E (2018) Breast cancer in latin America: a map of the disease in the region Am Soc Clin Oncol Educ B 38(38) 451–456 https://doi.org/10.1200/EDBK_201315
2. Igene H (2008) Global health inequalities and breast cancer: an impending public health problem for developing countries Breast J 14(5) 428–434 https://doi.org/10.1111/j.1524-4741.2008.00618.x PMID: 18821930
3. National Cancer Institute SEER*Explorer Application [Internet] [https://seer.cancer.gov/explorer/application.html?site=55&data_type=1&graph_type=10&compareBy=stage&chk_stage_104=104&chk_stage_105=105&chk_stage_106=106&chk_stage_107=107&series=9&sex=3&race=1&age_range=1&advopt_precision=4&advopt_show_ci=on&advopt_display=2] Date accessed 05/07/21
4. Sung H, Ferlay J, and Siegel RL, et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries CA Cancer J Clin 71(3) 209–249 https://doi.org/10.3322/caac.21660 PMID: 33538338
5. Gulzar F, Akhtar MS, and Sadiq R, et al (2019) Identifying the reasons for delayed presentation of Pakistani breast cancer patients at a tertiary care hospital Cancer Manag Res 11 1087–1096 https://doi.org/10.2147/CMAR.S180388 PMID: 30774437 PMCID: 6357878
6. Madkhali NA, Santin O, and Noble H, et al (2019) Breast health awareness in an Arabic culture: a qualitative exploration J Adv Nurs 75(8) 1713–1722 PMID: 30895639
7. Ogunkorode A, Holtslander L, and Anonson J, et al (2017) Promoting early detection of breast cancer and care strategies for Nigeria Afr J Reprod Health 21(2) 18–25 https://doi.org/10.29063/ajrh2017/v21i2.3
8. Kisiangani J, Baliddawa J, and Marinda P, et al (2018) Determinants of breast cancer early detection for cues to expanded control and care: the lived experiences among women from Western Kenya BMC Womens Health 18(1) 81 https://doi.org/10.1186/s12905-018-0571-7 PMID: 29859095 PMCID: 5984781
9. Williams J, Garvican L, and Tosteson ANA, et al (2015) Breast cancer screening in England and the United States – a comparison of provision and utilisation Int J Public Health 60(8) 881 https://doi.org/10.1007/s00038-015-0740-5 PMID: 26446081 PMCID: 6525304
10. Walters S, Maringe C, and Butler J, et al (2013) Breast cancer survival and stage at diagnosis in Australia, Canada, Denmark, Norway, Sweden and the UK, 2000-2007: a population-based study Br J Cancer 108(5) 1195–1208 https://doi.org/10.1038/bjc.2013.6 PMID: 23449362 PMCID: 3619080
11. Kratzke C, Amatya A, and Vilchis H (2015) Breast cancer prevention knowledge, beliefs, and information sources between non-Hispanic and Hispanic college women for risk reduction focus J Community Health [Internet] 40(1) 124–130 [https://pubmed.ncbi.nlm.nih.gov/24989348/] Date accessed 20/09/21 https://doi.org/10.1007/s10900-014-9908-9
12. Al-Mousa D, Alakhras M, and Hossain S, et al (2020) Knowledge, attitude and practice around breast cancer and mammography screening among Jordanian women Breast Cancer [Internet] 12 231–242 Date accessed 20/09/21 PMID: 33204150 PMCID: 7666976
13. Peek ME, Sayad JV, and Markwardt R (2008) Fear, fatalism and breast cancer screening in low-income African-American women: the role of clinicians and the health care system J Gen Intern Med [Internet] 23(11) 1847–1853 [https://link.springer.com/article/10.1007/s11606-008-0756-0] Date accessed 20/09/21 https://doi.org/10.1007/s11606-008-0756-0 PMID: 18751758 PMCID: 2585682
14. Davis J, Ramos R, and Rivera-Colón V, et al (2015) The Yo me cuido® program: addressing breast cancer screening and prevention among Hispanic women J Cancer Educ 30(3) 439–446 https://doi.org/10.1007/s13187-014-0710-2
15. Hernández-Vásquez A and Chacón-Torrico H (2019) Use of mammography in Peruvian women: an analysis of the 2018 demographic and health survey Medwave [Internet] 19(09) e7701 [/link.cgi/English/Original/Research/7702.act] Date accessed 20/09/21 https://doi.org/10.5867/medwave.2019.09.7701 PMID: 31665129
16. Martei YM, Vanderpuye V, and Jones BA (2018) Fear of mastectomy associated with delayed breast cancer presentation among Ghanaian women Oncologist 23(12) 1446–152 https://doi.org/10.1634/theoncologist.2017-0409 PMID: 29959283 PMCID: 6292549
17. Shamsi U, Khan S, and Azam I, et al (2020) Patient delay in breast cancer diagnosis in two hospitals in Karachi, Pakistan: preventive and life-saving measures needed JCO Glob Oncol [Internet] 6(6) 873–883 Date accessed 12/05/22 https://doi.org/10.1200/GO.20.00034 PMID: 32579484 PMCID: 7328101
18. Unger-Saldaña K, Cedano Guadiamos M, and Burga Vega AM, et al (2020) Delays to diagnosis and barriers to care for breast cancer in Mexico and Peru: a cross sectional study Lancet Glob Heal 8 S16 https://doi.org/10.1016/S2214-109X(20)30157-1
19. Instituto Nacional de Estadística e Informática (2017) Perú Enfermedades No Transmisibles y Transmisibles, 2017 [Internet] (Instituto Nacional de Estadística e Informática) [https://www.inei.gob.pe/media/MenuRecursivo/publicaciones_digitales/Est/Lib1526/index.html]
20. Theme Filha M, Leal M, and Oliveira E, et al (2016) Regional and social inequalities in the performance of Pap test and screening mammography and their correlation with lifestyle: Brazilian national health survey, 2013 Int J Equity Health [Internet] 15(1) Date accessed 20/09/21 https://doi.org/10.1186/s12939-016-0430-9 PMID: 27852313 PMCID: 5112710
21. Chkotua S and Peleteiro B (2017) Mammography use in portugal: national health survey 2014 Prev Chronic Dis [Internet] 14 E100 Date accessed 20/09/21 https://doi.org/10.5888/pcd14.170054 PMID: 29049019 PMCID: 5652236
22. Gomez H, Vigil C, and Moscol A, et al (2014) Descripción y evaluación del cáncer de mama en el Instituto Nacional de Enfermedades Neoplásicas 1st edn, (Lima: INEN)
23. Gomez H and Cotrina JM (2022) Descripción y evolución del cáncer de mama en el Instituto Nacional de Enfermedades Neoplásicas 1st edn, (Lima)
24. Valdiviezo N, Alcarraz C, and Castro D, et al (2022) Oncological care during first Peruvian national emergency COVID-19 pandemic: a multicentric descriptive study Cancer Manag Res 14 1075 https://doi.org/10.2147/CMAR.S350038 PMID: 35300062 PMCID: 8922040
25. Sessa C, Cortes J, and Conte P, et al (2022) The impact of COVID-19 on cancer care and oncology clinical research: an experts’ perspective ESMO Open 7(1) 100339 https://doi.org/10.1016/j.esmoop.2021.100339
26. Malagón T, Yong JHE, and Tope P, et al (2022) Predicted long-term impact of COVID-19 pandemic-related care delays on cancer mortality in Canada Int J Cancer 150(8) 1244 https://doi.org/10.1002/ijc.33884
Supplementary Material
Supplementary Table 1. Search strategies in PubMed, Scopus and Web of Science (WOS).







