Objectives: Cancer is frequently complicated by thromboembolic events (TEs). We aimed to determine the incidence of TEs in lung cancer patients treated with platinum-based chemotherapy and study patients’ baseline and treatment attributes correlating with its onset.
Materials and methods: Advanced lung cancer patients started on platinum-based chemotherapy were evaluated at baseline and during routine visits for the development of TEs. The duration of follow-up was 4 weeks from the last chemotherapy. A TE occurring between the first dose of chemotherapy and 4 weeks after the last dose was considered to be chemotherapy associated.
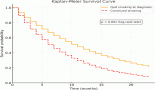
Results: Of the 165 patients on platinum chemotherapy who completed follow-up, TEs occurred in 4.8% (8 out of 165) patients. Among these, three patients had developed venous pulmonary thromboembolism and five patients had developed cerebral infarction, out of which four had arterial cerebral infarction and one patient had a superior sagittal sinus thrombosis. The majority of events (7 out of 8) occurred within 100 days of starting platinum chemotherapy. Overall, the median time until occurrence of TE was 48 days (range, 10–130 days). None of the presumed risk factors were found be associated with the occurrence of TEs on univariate analysis.
Conclusions: Advanced lung cancer patients on platinum chemotherapy are predisposed to thromboembolism due to many factors. Despite its lower incidence in our study, exclusion of patients with prior thrombosis suggests the incidence of de novo thrombosis, and hence raises a valid question of the need of thromboprophylaxis in a selected group of patients.