Cancer vulnerability in an indigenous Himalayan population in Arunachal Pradesh
Chaitan Kumara, and Moirangthem Momocha Singhb
Department of Management & Humanities, National Institute of Technology, Itanagar, Arunachal Pradesh, India
ahttps://orcid.org/0000-0002-5117-1083
bhttps://orcid.org/0000-0002-2507-698X
Abstract
Cancer incidence and its related mortality has been a public health concern for Arunachal Pradesh in India. However, there is a lack of evidence about the knowledge, attitude and practice (KAP) for cancer risk factors, screening programmes and preventive behaviour – especially among indigenous tribal populations. A cross-sectional survey was conducted using Google Forms from 16 September 2020 to 2 January 2021 among an indigenous population of Arunachal Pradesh. Snowball sampling was used to enrol 565 participants aged ≥18 years (264 were male and 301 were female). Univariate and bivariate analyses were conducted using SPSS version 23 to test the hypothesis of KAP. (There is no difference in the level of knowledge / in the attitude / level of practice among study participants with respect to any independent (socio-demographic and other) factors.) The Papumpare Cancer Registry reported the highest cancer density among women and the second highest among men among all population-based cancer registries in India (Indian Council of Medical Research, Report of National Cancer Registry Programme, Bengaluru, India 2020). Knowledge about the cause of cancer and risk factors was poor among 23% of the respondents. Attitude towards screening was negative among 14.9%. Practice levels to prevent cancer were also low (31%). More than 50% of the cases were treated outside the state and at private hospitals. Knowledge about cancer symptoms and risk factors was limited in the population. There is a need for more effective health promotional services in the state. Mass screening facilities and behavioural change activities are required and could be disseminated through social media platforms. Our analysis of a north-eastern region of India, which has unique geographical and cultural characteristics, informs future policy designs and other related studies for controlling cancer in the area.
Keywords: cancer, knowledge, attitude, practice, prevention, indigenous population
Correspondence to: Chaitan Kumar
Email: chaitandu@gmail.com
Published: 30/05/2022
Received: 05/10/2021
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background
Cancer poses a major public health problem worldwide owing to its high prevalence and incidence along with the associated socio-economic burden. The projected number of patients with cancer in India was 1,392,179 in 2020, with a higher reported incidence among women (712,758) than men (679,421) [1]. The top five common cancer-reported sites are breast, lungs, mouth,
cervix uteri and tongue. As shown in Figure 1, there is marked heterogeneity in the cancer incidence (age-adjusted rate per 100,000 people) among both men and women across different regions within Indian states [1].
The higher incidence of cancer was attributed to higher consumption of tobacco in the North-eastern states, followed by the West and Central regions of India [7]. Among men, the most common cancer sites included lungs, mouth, oesophagus and stomach. Among women, the predominant cancer site was breast, followed by cervix uteri and ovaries [7].
Most of the knowledge, attitude and practice (KAP) studies have been conducted among the general population of India or in different states like Chennai, Kerala, Punjab and Kashmir. These studies documented low levels of knowledge about cancer risk factors, the importance of screening and early detection and protective behaviours [2–4]. An individual’s level of practice of healthy behaviours is even lower than his/her knowledge scores, and there is limited awareness of risk factors among the North-eastern general population [5].
In the extant literature, there is no evidence related to KAP about cancer and its risk factors, screening programmes and protective behaviours among indigenous tribes of Arunachal Pradesh in the North-eastern states of India.
Objectives
a. To assess the knowledge about cancer risk factors and preventive behaviours among an indigenous population.
b. To explore the indigenous population’s awareness of screening methods.
c. To determine the socio-economic impact of cancer on families.
d. To determine the perception of public for stakeholder’s role in the population.
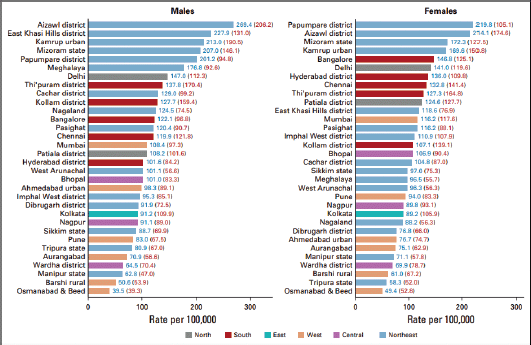
Figure 1. Geographical distribution of cancer rate per 100,000 people in India. Source: Report of National Cancer Registry Programme (ICMR-NCDIR), Bengaluru, India 2020.
Table 1. Composition of a major indigenous population in Arunachal Pradesh.
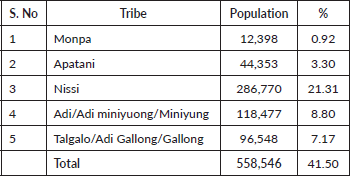
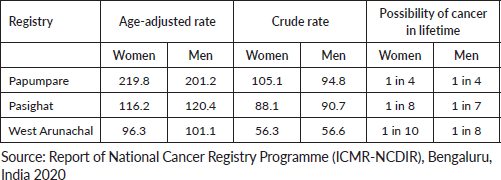
Table 2. Cancer incident rate in various registries.
Methods
This online cross-sectional survey was conducted using Google Forms from 16 September 2020 to 2 January 2021 among an indigenous population of Arunachal Pradesh.
Brief geographical characteristics of the North-eastern states of India and Arunachal Pradesh
Indian has 28 states and 8 union territories. The north-eastern part of India consists of eight states. Most of the population (45,587,982) belong to the hilly and tribal population, per the 2011 Census [6]. Arunachal Pradesh comprises 3% (1,382,611) of the total population of the North-eastern states of India (68.8% tribal population) [6]. The state has a sex ratio that is 938. The literacy rates among women and men are 57.7% and 72%, respectively [6]. The five major tribal communities—Monpa, Apatani, Nissi, Adi, and Galo—constitute 41% (558,546 people) of the population (Table 1).
Cancer epidemiology in Arunachal Pradesh
Cancer registries are maintained for three major geographical sites of Arunachal Pradesh (Table 2): Papumpare (central region), Pasighat (eastern region) and West Arunachal (western region of Arunachal Pradesh). Approximately 3017 cancer cases were reported in Arunachal Pradesh from 2014 to 2016 (51% men and 49% women) [7]. The age-adjusted rate of cancer is highest in Papumapre region, for both men and women [7].
The top four cancer sites among men in West Arunachal Pradesh are stomach, liver, oesophagus and lungs. Among women, stomach, breast, cervix uteri, thyroid and liver are the most prevalent in West Arunachal [7]. In Pasighat, the proportion of stomach cancer (18.1%) was highest among men, followed by lung (7.8%) and liver (5.9%) cancer. In women, the cervix uteri was the leading cancer site (18.5%), followed by breast (16.8%) and stomach (9.6%) cancer [7].
The state has 1 medical college, 6 general hospitals, 15 district hospitals, 51 community healthcare centres, 148 primary healthcare centres, 4 urban primary healthcare centres and 582 sub-healthcare centres [8]. Arunachal Pradesh has developed 136 health and wellness centres, which provide non-communicable disease (NCD) screening facilities along with screening of 3 types of cancers, breast, cervical and oral, for those aged ≥30 years [9]. A tertiary cancer care facility was established under the new medical college; however, a dedicated cancer hospital is absent in the state [9].
Study population and sampling method
Arunachal Pradesh has a population of approximately 1.4 million. Owing to the COVID-19 pandemic and travel restrictions, the survey was conducted online. We used Google Forms via online platforms in urban areas where most people have Internet access. Therefore, we selected districts where the urban population of the indigenous tribes was predominant. Hence, we adopted convenience sampling for selecting the districts.
Furthermore, snowball sampling was used to enrol the participants. We enrolled 565 adults (aged ≥18 years) belonging to a tribal population and residing in urban areas. We requested our relatives and colleagues to forward the link to the questionnaire through email and WhatsApp. Respondents who were aged <18 years, lived outside the state and had not heard about cancer were excluded from the analysis.
We developed and pre-tested the questionnaire by reviewing the existing literature and seeking expert guidance from faculties of the University of Delhi. Validated questions from similar questionnaires on KAP in India were utilised [2–5]. The content and face validity of the tool was established by five subject experts. The tool was pre-tested with 33 participants, and test–retest reliability was established. The overall Cronbach’s alpha value exceeded 0.85, indicating good internal consistency.
Participants were assured of the confidentiality of their personal information. Informed consent was obtained from each participant with a statement that data would be used for academic and research purposes only. Ethical permission was granted by the institute’s research committee before conducting this study. An approval letter from the Directorate of Health Services of Arunachal Pradesh was also sought.
Statistical analysis
The data were cleaned in Excel and exported in the IBM SPSS version 23. The data analysis included univariate, bivariate and multivariable regression modelling. The socio-demographic variables and KAP parameters about cancer risk factors and prevention were analysed and are presented using frequency and percentage.
The variables representing knowledge about symptoms and causes of cancer (multiple response variables), as well as about the ability of vaccines to prevent certain cancers were utilised to generate a variable representing total knowledge score. Each correct response was scored 1 and the response of ‘no knowledge’ was coded 0. The total knowledge score ranged from 0 to 22. A categorical variable representing cancer/NCD patients being at high risk for COVID-19 infection (mutually exclusive choices) was also generated (poor: <33%; moderate: 33–65%; good: ≥66%).
The variables representing attitude included awareness about a screening programme, opinion about self-assessment knowledge in helping early screening of cancer and risk reduction, opinions about telemedicine advice to improve the screening and treatment, and preference of screening for cancer at one’s doorstep to save money. The responses to these were mutually exclusive choices. Each response of ‘yes’ was scored 1, and each response of ‘no’ was scored 0. The total score ranged from 0 to 4. Binary categorical variables representing the attitude (positive: 1 and negative: 0) was also generated.
The variables representing practices included steps taken to reduce the risk of cancer (multiple responses variables), visiting a hospital for a preventive check-up, online searches regarding cancer-related services and information, and participation in a cancer screening programme (mutually exclusive choices). Each correct response as well as response of ‘yes’ was scored 1 and each response of ‘no’ was scored 0. The total score ranged from 0 to 14. A categorical variable representing the three levels of practice (low: <33%; moderate: 33–65%; high: ≥66%) was also generated.
A bivariate analysis was conducted to explore the factors affecting KAP about the prevention of cancer. Chi-square tests were also performed. A binomial regression model was tested for factors that were significantly associated with the nature of attitude about cancer prevention. Similarly, multinomial regression models were tested for factors that were significantly associated with the level of knowledge and practices about cancer prevention. P-values < .05 were deemed significant.
Results
Demographics
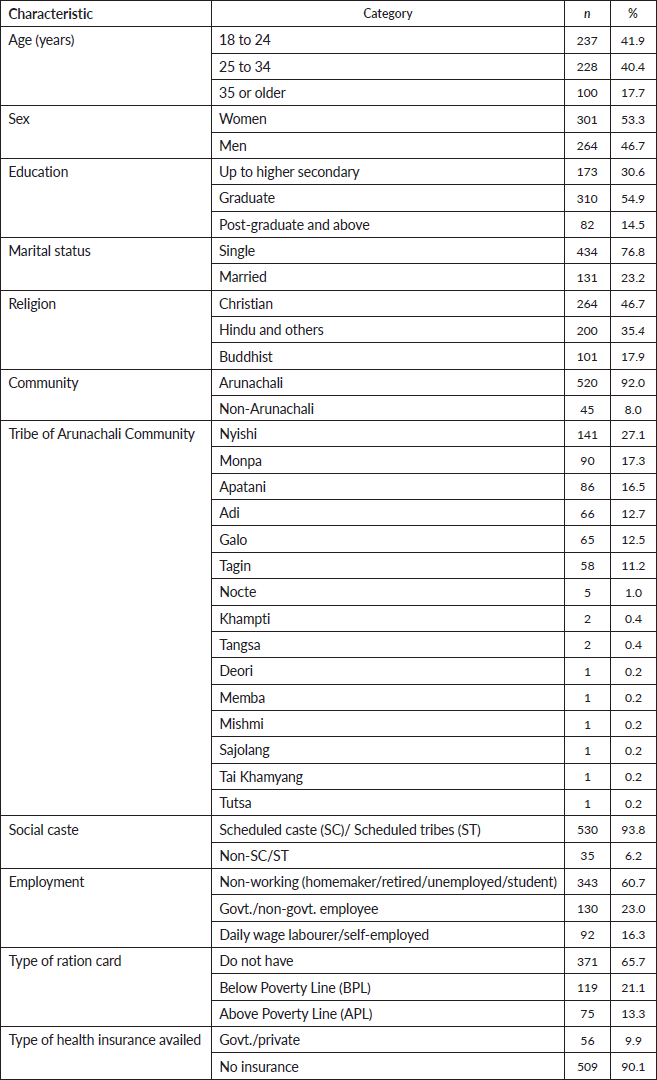
There were 565 participants, aged 18–68 years. The mean age was 27.9 ± 7.8 years. Most of them were aged 18–34 years, women, well-educated, single and unemployed at the time of the survey. The Arunachali community constituted 92% of the study sample (n = 520), and most belonged to the schedule caste and tribe community (n = 530). Most did not own a ration card (for getting subsidised rations) and did not have any kind of health insurance scheme (Table 3).
Table 3. Socio-demographic characteristics of the participants (N = 565).
Knowledge about cancer among participants
Sources of information about cancer
Healthcare workers were the main source of knowledge about cancer for nearly all participants. Other popular options were schools/colleges, social media and print media (Table 4).
Table 4. Knowledge about cancer among the participants (N = 565).
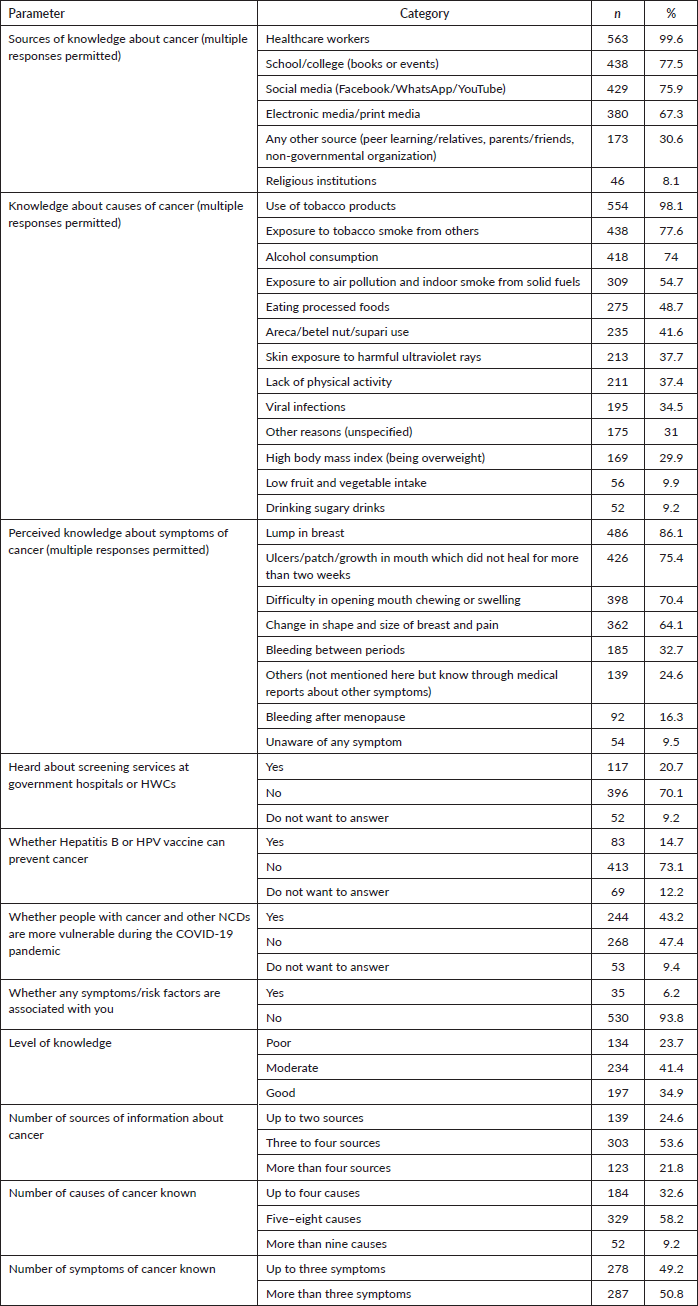
Knowledge about the causes of cancer
Nearly all participants mentioned the use of tobacco products to be the cause of cancer, and three-quarters mentioned second-hand smoke to be one of the causes of cancer. Alcohol consumption was considered to be carcinogenic by 74% of the participants. The other causes of cancer mentioned by participants included exposure to air pollution and indoor smoke from solid fuels, eating processed foods and the use of areca nut/supari or betel. The other causes of cancer mentioned by participants included exposure to harmful ultraviolet rays, lack of physical activity, viral infections, high body mass index and consumption of sugary drinks (Table 4).
Knowledge about the symptoms of cancer
The most perceived cancer symptoms were a lump in the breast, ulcers/patch/growth in mouth that did not heal for more than 2 weeks, difficulty in chewing or swallowing and change in shape or size of breast and pain (Table 4). Furthermore, 70% of the participants had not heard about cancer screening services available at government hospitals or health and wellness centres, and most of them were not aware about the role of vaccines in preventing certain cancers. Two-fifths agreed that the COVID-19 pandemic made patients with cancer or other NCDs more vulnerable.
Approximately half had information on cancer from three to four sources, and more than half were aware of five to eight causes of cancer and more than three symptoms of developing cancer. In sum, the level of knowledge was poor among 23.7% (n = 134), moderate among 41.4% (n = 234) and good among 34.9% (n = 197) of the participants. Table 4 provides the major knowledge sources, the perceived cancer causes and the perceived symptoms of cancer, respectively.
Practices of cancer prevention
Concerning preventive measures taken, tobacco and alcohol use were avoided by most participants. Other common measures included avoiding areca nuts and processed food. Engagement in daily physical activity and maintaining a healthy weight were also common. Nearly 6.6% mentioned that they did not use any preventive measure (Table 5).
Table 5. Practice about cancer prevention among the participants (N = 565).
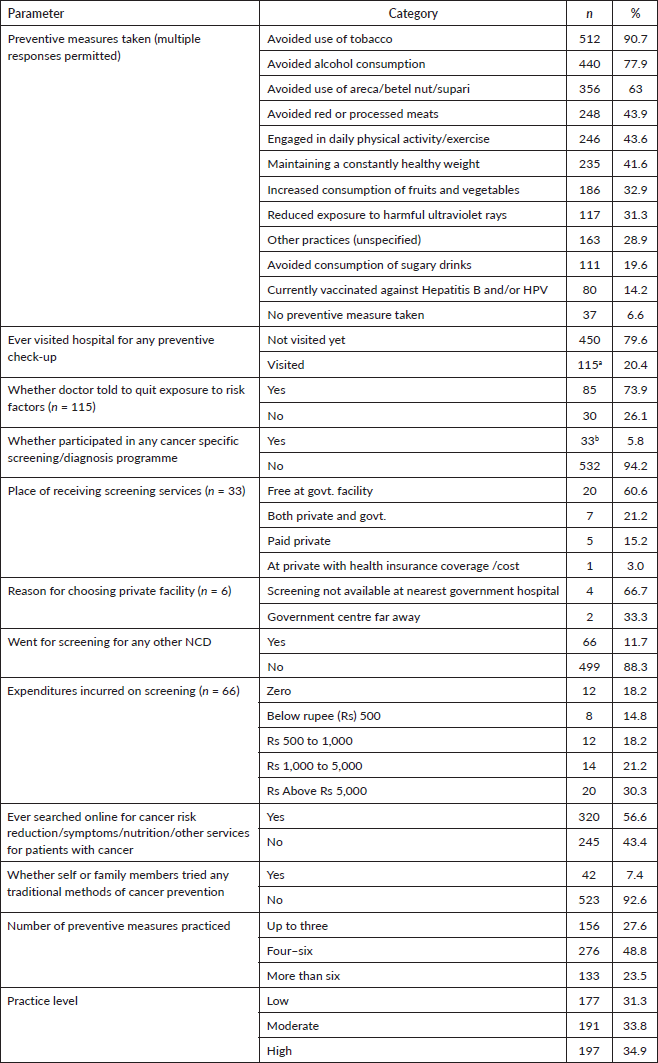
Most had not visited the hospital for a preventive check-up. Of those who went, most were informed by their physicians to avoid exposure to the risk factors.
Only 5.8% had participated in a cancer-specific screening programme. Of these, 60.6% availed the service free from the government facility, whereas 15.2% paid for the service at a private facility. The reasons behind choosing a private facility were unavailability of screening at the nearest government hospital or that it was too far.
Only 11.7% had participated in a screening programme for other NCDs. Of those, 30.3% had paid more than 5,000 rupees (INR). More than half had searched online about cancer risk reduction/symptoms/nutrition/other services.
The assessment of indicators of practice revealed that the distribution of the levels of practice about cancer appropriate behaviour was similar across three categories, including low, medium and high. Majority of the respondents (90.7%) wished to quit tobacco. Figure 2 shows the participants’ responses concerning preventive measures.
Attitude towards cancer prevention
Attitude about getting screened for cancer and other NCDs
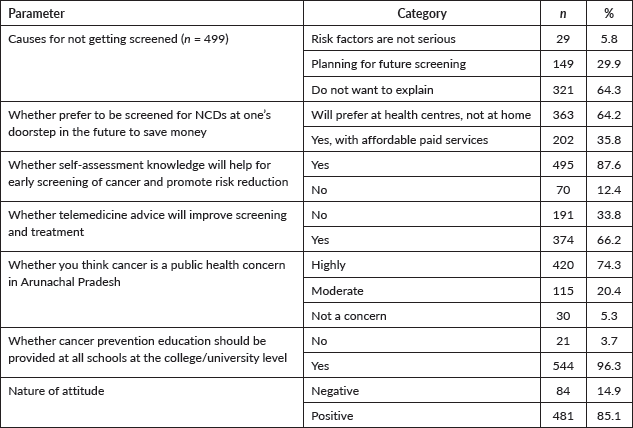
When asked, 5.8% mentioned that the risk factors were not serious, while 29.9% mentioned that they were planning for future screening. Nearly two-thirds were not willing to explain their reason. Most mentioned that they would prefer screening facility at healthcare centres. Most opined that self-assessment knowledge will help in early screening of cancer and promote risk reduction. Most also said that cancer is a high public health concern in Arunachal Pradesh (Table 6).
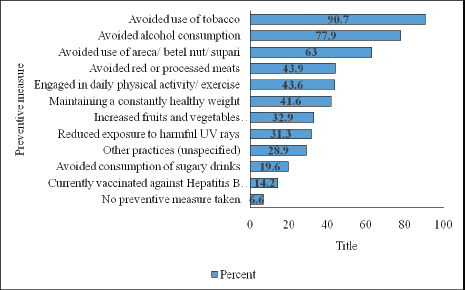
Figure 2. Distribution of preventive measures against cancer taken by participants (multiple responses permitted).
Table 6. Attitude about screening for NCDs among the participants (N = 565).
Family history of cancer and its financial implications
Ninety-seven responded stated that they had some family history of cancer, and the treatment costs are provided in Table 7. Nearly one-third mentioned job loss owing to cancer treatment as a chief financial burden. Some participants had to borrow money or sell property/jewellery to bear the costs (Table 8).
Perceived role of government in controlling cancer and other NCDs
Respondents believe that the government and other stakeholders have crucial roles to play. When asked about their expectation from the government and other stakeholders towards cancer control, three-quarters mentioned that the screening/treatment services in the state must be increased. Two-thirds suggested that more community awareness programmes should be conducted. However, most mentioned that there must be tough bans on the use of tobacco, alcohol and other cancer-causing products. Furthermore, most mentioned the need to involve social enterprises or non-governmental organisations to obtain affordable prices (Figure 3).
Factors affecting KAP
Factors affecting knowledge
In the bivariate analysis, the outcome variables were identified as per the study’s objectives, i.e., KAP about cancer prevention. The factors influencing these outcome variables, also known as independent variables, were tested using chi-square tests as all outcome variables were categorical. Following the bivariate analysis of each outcome variable, the significant associations (p < 0.05) were tested using regression models. Beginning from Tables 9 to 11, each bivariate analysis was conducted using a chi-square test, followed by a regression model (binomial or multinomial). The purpose of regression modelling was to control for confounding factors and thus identify the factors that truly affect the level of knowledge independent of each other. The null hypothesis was as follows: There is no difference in the level of knowledge among participants with respect to any independent (socio-demographic and other) factors.
As shown in Table 9, participants’ age, education, marital status, religion, number of cancer information sources, number of known causes of cancer, number of known causes of symptoms and number of preventive measures taken were significantly associated with the level of knowledge about cancer.
Table 7. Family history of cancer among the participants (N = 565).
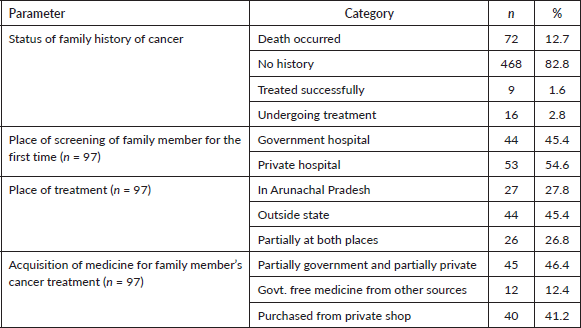
Table 8. Financial implications of cancer treatment (N = 565).
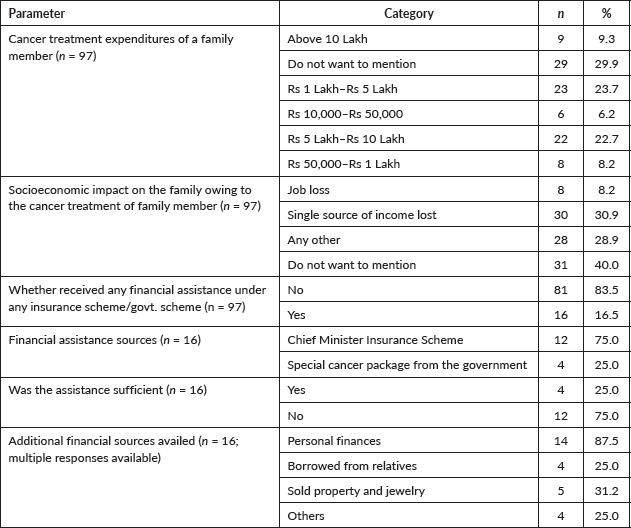
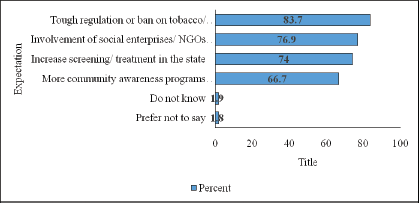
Figure 3. Expectations from the government and other stakeholders towards control of cancer and other NCDs (multiple responses permitted).
Table 9. Factors affecting knowledge about cancer among participants (N = 565).
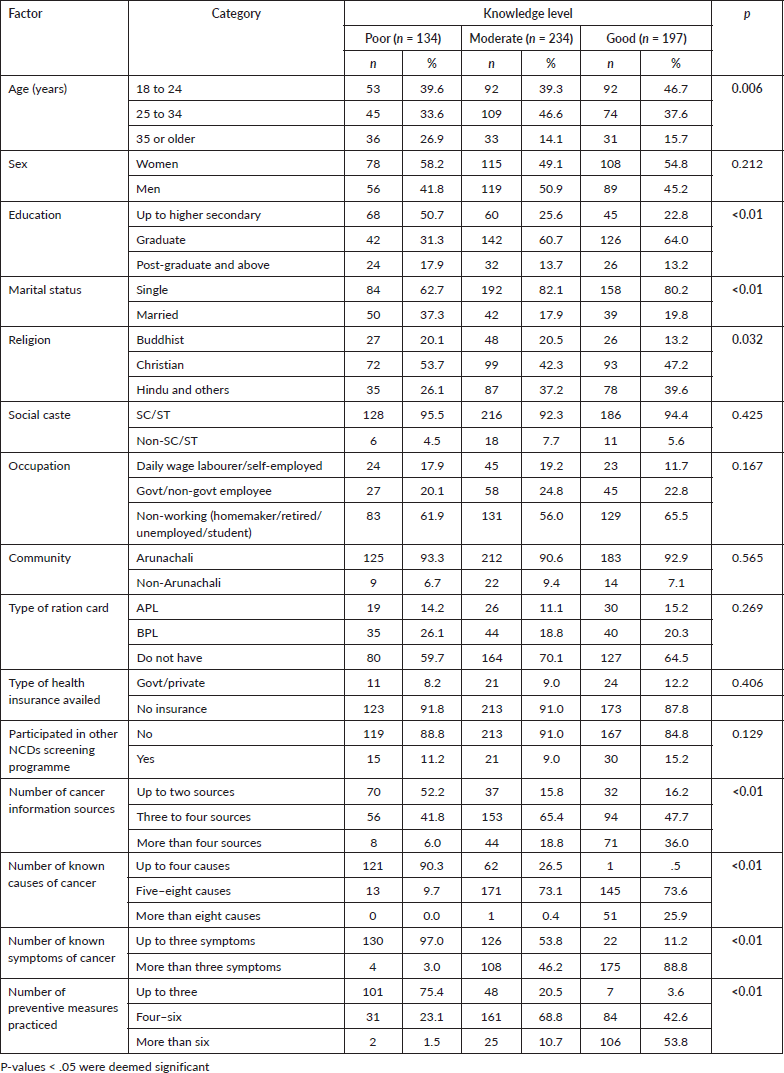
Better knowledge about cancer was more prevalent in younger age groups as compared to their older counterparts. Similarly, the prevalence of a moderate or good level of knowledge was higher among Christians, those who were more educated, and individuals with a moderate knowledge about symptoms, causes or preventive measures as compared to their counterparts.
Factors affecting attitude about cancer
The factors affecting the attitude were tested using chi-square tests of significance, followed by a binomial logistic regression model as the outcome variable on attitude had two categories. The null hypothesis was as follows: There is no difference in the attitude about cancer among participants with respect to any independent (socio-demographic and other) factors.
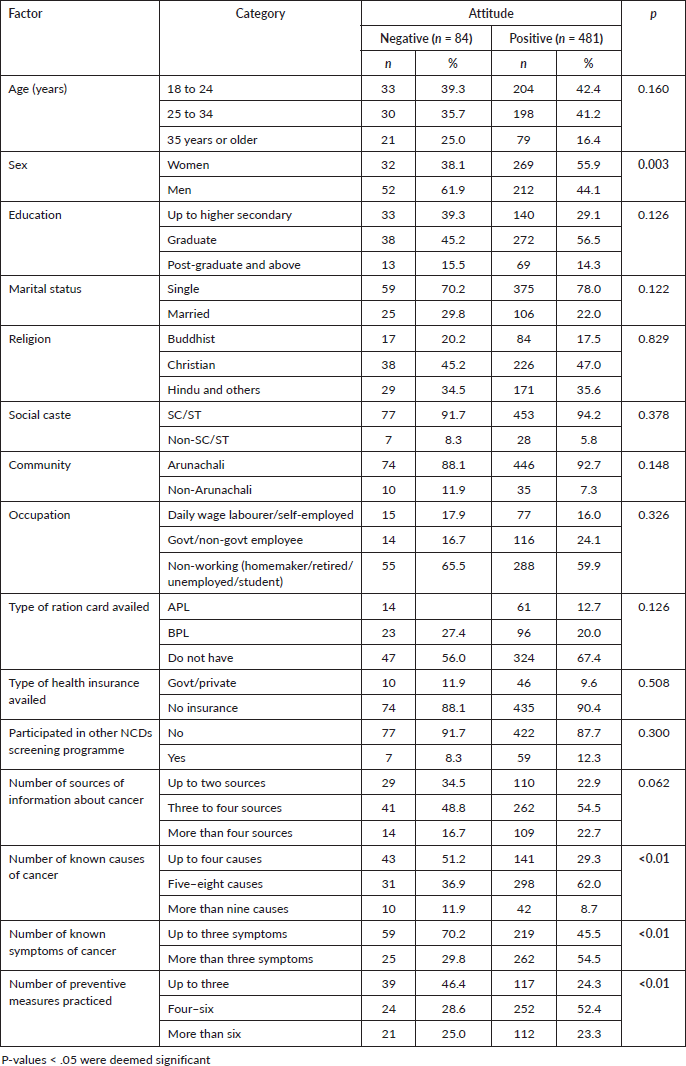
As shown in Table 10, the proportion of negative attitude was higher among men (61.9%) and positive attitude was higher among women (55.9%) (p < 0.05). Furthermore, a higher proportion of individuals with knowledge about fewer (up to 4) causes of cancer held more negative attitudes than did their counterparts. Positive attitude was significantly associated with an increase in the number of known causes of cancer, increase in the number of known symptoms and increase in the number of preventive measures taken by participants.
Table 10. Factors affecting attitude about risk factors of cancer among the participants (N = 565).
Factors affecting practice about cancer prevention
The factors affecting the level of practice were tested using chi-square tests of significance, followed by a multinomial logistic regression model, as the outcome variable on the practice level had more than two categories. The null hypothesis was as follows: There is no difference in the level of practice for cancer prevention among participants with respect to any independent (socio-demographic and other) factors.
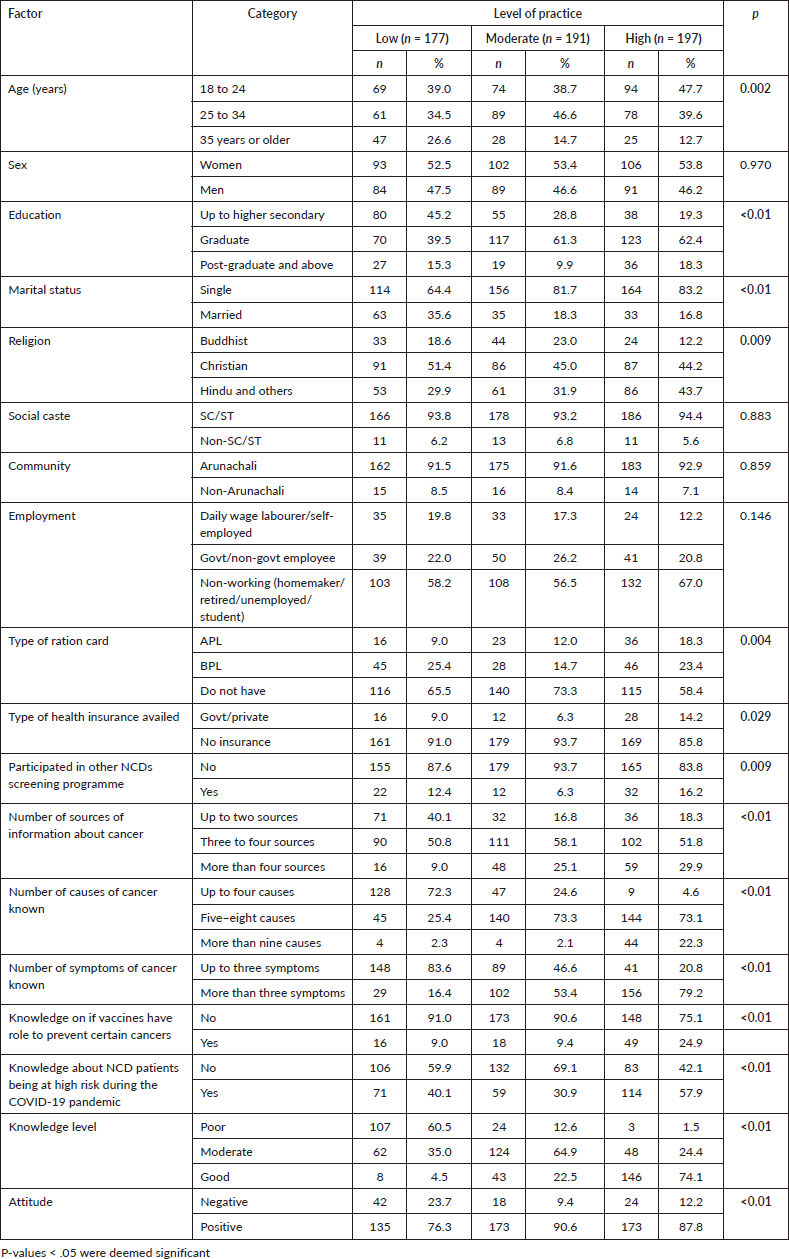
As shown in Table 11, the youngest age group (18–24 years) practiced a high level of cancer prevention, while those aged 25–34 years practiced a moderate level (p < 0.05). Similarly, a low level of practice about cancer prevention was more common among those who were less educated than their counterparts (p < 0.05). Any level of practice of cancer prevention was much higher among those who were single or Christians (p < 0.05). A moderate to high level of practice was found among individuals with no ration card, no insurance scheme, those who obtained information from three to four sources, who knew five to eight causes of cancer, who knew more than three symptoms and who knew the risks associated with NCDs and COVID-19 (p < 0.05). The relationship between the knowledge of symptoms and prevention attitude is shown in Figure 4.
Table 11. Factors affecting practices against risk factors of cancer among the participants (N = 565).
Discussion
Only 35% of the participants had good knowledge, followed by 40% with a moderate level of knowledge, on various aspects of cancer. People knew that tobacco and alcohol consumption were cancer-causing risk factors, which has been reported in the Indian Council of Medical Research (ICMR) reports [7]. Most believed that avoiding alcohol and tobacco can reduce vulnerability. Awareness of common cancer symptoms is limited to all in the community, which is similar to the other states in the North-eastern region in India [5]. One study in Assam found that 92% of the participants enjoyed chewing areca nuts and only 18% tried to quit [10]. However, in our study, approximately 63% of the indigenous population had quit areca nut chewing owing to high levels of awareness in the community.
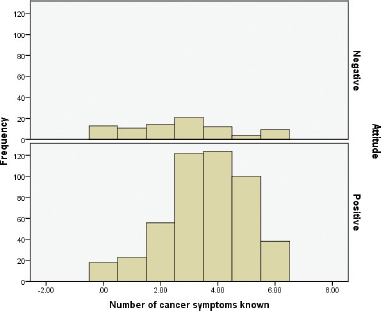
Figure 4. Knowledge about cancer symptoms and attitude towards cancer prevention.
Healthcare workers were the participants’ main source of information. Religious places were rarely noted as generating awareness about cancer. This is an important finding because in India, most people are religious and adhere to the teachings imparted at such places. Thus, to improve awareness and health-promotion activities, religious institutions should disseminate cancer-related information.
Participants’ KAP concerning NCD screening was very low. Most had never heard of the Ayushman Bharat Health and Wellness Centre for NCD screening. Very few had receiving screening. This coincided with prior results which showed that in the North-eastern state of Assam 92.9% of the participants were not aware of screening or had not been screened [11].
This study looked at the available literature on cancer awareness, attitudes and screening practices among the population in the north-eastern part of India. A variety of variables contributed to low cancer screening adherence: a lack of understanding, knowledge and practice; low levels of psychological threat; delayed symptoms and signs in the early stages; stigmatisation linked to cancer; anxieties; expenditures; household duties; and humiliation. In this study, most participants knew that tobacco was associated with a high risk of cancer. In the research carried out in emerging and impoverished states, similar outcomes were found [11]. Nevertheless, these findings contrast with those of the research involving people attending the obstetrics and gynaecology department of a public health facility [4]. Despite adoption of the National Programme for Prevention and Control of Cancer, Diabetes, Cardiovascular Diseases and Stroke in the state, the population has lesser awareness of cancer screening [9]. This could be because primary healthcare clinics have limited facilities for cancer screening.
During our assessment, we found that most participants were aware of the HPV vaccine, but only a handful had taken it. Women, in another study, felt that early screening and HPV vaccination might boost their immune system, even though most women had never been screened.
There was a significant difference in the KAP among participants with respect to various socio-demographic and other factors. Age, education, marital status, religion and number of sources of knowledge were independent predictors of knowledge. Other studies also found that knowledge and practice had significant associations with the level of education and family income [12]. Education, age and per capita income were independent predictors of information, attitudes and practice of cancer screening, which also mirrored prior research globally [13].
To date, no study has explored the KAP of indigenous tribes concerning cancer risk factors, screening behaviours, adoption of healthy lifestyles and availability of various health facilities in Arunachal Pradesh. Our unique findings thus inform policy level decisions to curb cancer in this area.
Limitations and future scope
A key limitation of this study is that respondents completed online questionnaires and were recruited only from urban areas. Future studies should seek different populations to generalise the results.
Conclusion
KAP concerning cancer risk was significantly related to participants’ health- and demographic-related characteristics. The risk factors of cancer in Arunachal Pradesh are high. Public and private providers have a good opportunity to serve the people. Screening and treatment must be improved in the state. Dedicated cancer institutes, diagnosis facilities, sufficient human resources and palliative care centres are required. Improved telemedicine or extending national cancer grid service can be attached with the Tomo Riba Institute of Health And Medical Sciences for better patient services. The state-specific preventive plan should focus on the local ethnic concern of various risk factors like food habits. Knowledge and behavioural change strategies concerning the availability of affordable services should be a public health agenda. Village-wise screening camps could be utilised for mass screening among eligible populations. To overcome the resource constraints, private players or non-profit partners with affordable services should be utilised so patients do not have to migrate to other states for diagnosis and treatment. Knowledge about the relevant government schemes should also be disseminated. Regulations related to tobacco and alcohol need to be tightened. Increasing the number of health workers who work in cancer screening at all hospitals could also further increase detection rates. Self-assessment tools and telemedicine services can play important roles in risk reduction and early detection. Lastly, studies related to the food and culture of Arunachal Pradesh should be carried out to elucidate other factors associated with cancer in the state.
List of abbreviations
APL: Above poverty line; BPL: Below poverty line; Govt.: government; HPV: Human papillomavirus; ICMR: Indian Council of Medical Research; KAP: Knowledge, attitude and practices; NCD: Non-communicable disease; NCDIR: National Centre for Disease Informatics and Research; Rs: Rupee; SC: Scheduled caste; ST: Scheduled tribe
Acknowledgments
The authors would like to thank the Department of Health Family Welfare, community members and health workers for their kind support.
Conflicts of interest
The authors declare that they have no conflicts of interest.
Authors' contributions
The corresponding author was involved in the study’s conception, design, collection and analysis of data and drafting the report. The second author assisted in all stages and made suggestions for technical writing. Both authors approve the submission of this manuscript and are accountable for all aspects of the work.
Funding
This research work was not funded by any organisation.
References
1. National Cancer Registry Programme (ICMR-NCDIR) (2020) (Bengaluru: NCDIR)
2. Aswathy S, Quereshi MA, and Kurian B, et al (2012) Cervical cancer screening: current knowledge & practice among women in a rural population of Kerala, India Indian J Med Res 136 205 PMID: 22960886 PMCID: 3461731
3. Elangovan V, Rajaraman S, and Basumalik B, et al (2017) Awareness and perception about cancer among the public in Chennai, India J Glob Oncol 3 469–479 https://doi.org/10.1200/JGO.2016.006502 PMID: 29094085 PMCID: 5646888
4. Javaeed A, Shoukat S, and Hina S, et al (2019) Knowledge, attitude, and practices related to cervical cancer among adult women in Azad Kashmir: a hospital-based cross-sectional study Cureus 11 e4234 PMID: 31123656 PMCID: 6510573
5. Oswal K, Kanodia R, and Pradhan A, et al (2020) Assessment of knowledge and screening in oral, breast, and cervical cancer in the population of the northeast region of India JCO Glob Oncol 6 601–609 https://doi.org/10.1200/JGO.19.00257 PMID: 32302235 PMCID: 7193798
6. Government of India (2011) Census [https://censusindia.gov.in/2011-common/censusdata2011.html] Date accessed: 01/03/21
7. ICMR-NCDIR (2021) Profile of Cancer and Related Health Indicators in the North East Region of India [https://ncdirindia.org/All_Reports/NorthEast2021/Default.aspx] Date accessed: 02/03/21
8. National Health Profile (2019) [http://www.cbhidghs.nic.in/showfile.php?lid=1147] Date accessed: 05/03/21
9. Ayushman Bharat Health and Wellness Centres in First 18 Months of Implementation April 2018–September 2019 [https://ab-hwc.nhp.gov.in/download/document/340b49eb2c0937e7b79ad8c1d6b975ad.pdf] Date accessed: 10/03/21
10. Kumar A, Oswal K, and Singh R, et al (2021) Assessment of areca nut use, practice and dependency among people in Guwahati, Assam: a cross-sectional study Ecancer 15, 1198 https://doi.org/10.3332/ecancer.2021.1198
11. Pak LM, Purad CC, and Nadipally S, et al (2021) Cancer awareness and stigma in rural Assam India: baseline survey of the Detect Early and Save Her/Him (DESH) Program Ann Surg Oncol 28(12) 7006–7013 https://doi.org/10.1245/s10434-021-10366-7 PMID: 34215953
12. Biswas S, Syiemlieh J, and Nongrum R, et al (2020) Impact of educational level and family income on breast cancer awareness among college-going girls in Shillong (Meghalaya), India Asian Pac J Cancer Prev 21 3639–3646 https://doi.org/10.31557/APJCP.2020.21.12.3639 PMID: 33369463 PMCID: 8046293
13. Singh S, Narayan N, and Sinha R, et al (2018) Awareness about cervical cancer risk factors and symptoms Int J Reprod Contracept Obstet Gynecol 7 4987–4991 https://doi.org/10.18203/2320-1770.ijrcog20184953






