Radiotherapy waiting time in Northern Nigeria: experience from a resource-limited setting
Nuhu Tumba1, Sunday Adeyemi Adewuyi2, Kelechi Eguzo3, Adeniyi Adenipekun4 and Rasaaq Oyesegun5
1Department of Radiology, Division of Radiation/Clinical Oncology Bingham University Teaching Hospital, Jos 930214, Nigeria
2Department of Radiotherapy & Oncology Ahmadu Bello University Teaching Hospital, Zaria 810105, Nigeria
3Department of Obstetrics & Gynaecology, University of Saskatchewan, S4N 2B7, Canada
4Department of Radiation Oncology, University College Hospital, Ibadan 200284, Nigeria
5Department of Radiotherapy & Oncology, National Hospital Abuja 900211, Nigeria
Abstract
Background: Access and availability of radiotherapy treatment is limited in most low- and middle-income countries, which leads to long waiting times and poor clinical outcomes. The aim of our study is to determine the magnitude of waiting times for radiotherapy in a resource-limited setting.
Methods: This is a retrospective cohort study of patients with the five most commonly treated cancers managed with radiotherapy between 2010 and 2014. Data includes diagnosis, patients’ demographics and treatment provided. The waiting time was categorised into intervals (1) between diagnosis and first radiation consultation (2) First consultation to radiotherapy treatment (3) Decision-to-treat to treatment and (4) Diagnosis to treatment.
Results: A total of 258 cases were involved, including cervical (50%; 129/258), breast (27.5%; 71/258), nasopharynx (12.8%; 33/258), colorectal (5%; 13/258) and prostate cancers (4.7%; 12/258). Mean age was 48 (±12.9) years. Treatment with radical intent comprised 67% (178/258) of cases, while 33% (80/258) had palliative treatment. The median time from diagnosis to first radiation consultation was 40 (IQR 17–157.75) days for all the patients, with prostate cancer having the longest time – 305 days (IQR 41–393.8). The median time between the first radiation oncology consultations and first radiotherapy treatment was 130.5 (IQR 14–211.5) days; cervical cancer patients waited a median of 139 (IQR 13–195.5) days. The median time between diagnosis and first radiotherapy for breast cancer patients was 329 (IQR 207–464) days, compared to 213 (IQR 101.5–353.5) days for all the patients.
Conclusion: The study shows that waiting time for radiotherapy in Nigeria was generally longer than what is recommended internationally. This reflects the need to improve access to radiotherapy in order to improve cancer treatment outcomes in resource-limited settings.
Keywords: waiting time, radiotherapy, resource-limited-setting
Correspondence to: Nuhu Tumba
Email: nuhu.tumba@binghamuni.edu.ng
Published: 04/09/2020
Received: 17/03/2020
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Background
Radiotherapy is an important component of modern cancer treatment, with an estimated 50%–60% of all cancer cases receiving it during the course of their treatment. Yet access to this vital modality of cancer treatment is limited or even absent in most low- and middle-income countries (LMICs), especially in sub-Saharan Africa. It is estimated that 80% of the world’s cancer burden is in LMICs, but only 5% of the world’s radiotherapy resources are in LMICs. Therefore, about 90% cancer patients who need radiotherapy have no access to it and those who do have access have to wait a long time to receive treatment [1–6].
The fundamental reason for long waiting times for radiotherapy is the increasing demand for radiotherapy due to raising cancer incidence in LMICs as shown by epidemiological studies and the recent GLOBACAN 2018 reports published by the International Agency for Research on Cancer. This rising incidence has not been matched with a proportional expansion in radiotherapy infrastructure and the current capacity does not match the existing needs and unless this is addressed urgently, the situation will even be more critical in the next decade. Other factors include insufficient radiotherapy professionals (radiation oncologist, medical physics, therapy radiographers and mould room technicians), increasing complexity in the treatment process, poor maintenance which increases machine downtime and frequent strike action by health care professionals to demand for better working conditions and remuneration [7, 8].
Several clinical studies have shown the adverse effects of delay in initiation of radiotherapy treatment. Long waiting time or delayed radiotherapy have been shown to increase the risk of local recurrence and decrease in overall survival in certain clinical settings [9–14]. Jansen et al [15] have estimated a decreased local control rate of 8% per month of delay in a study of head and neck cancers. Apart from these obvious poor clinical outcomes, delayed radiotherapy exacerbates the anxiety that arises from a cancer diagnosis in patients and their caregivers. Losses of productivity and income as well as increased medical expenditure are often overlooked consequences of long waiting times [16, 17].
Many studies have examined the problems of waiting, especially in high-income countries, but few studies have examined radiotherapy waiting time in resource-limited settings.
The aim of our study is to determine the magnitude and the variation of waiting time across different categories of cancer patients.
Materials and methods
Study setting
The Ahmadu Bello University Teaching Hospital is situated in Zaria, Kaduna state with an estimated population of 8,252,366. However, we receive patients from all over Nigeria, usually when there is breakdown of machines in the other centres and from the neighbouring countries of Chad, Cameroun and Niger.
The Radiotherapy & Oncology Department, Ahmadu Bello University Teaching Hospital is the first radiotherapy facility in northern Nigeria. It was established in 1995 and has a low dose rate brachytherapy machine which mainly treats cervical cancers. The cobalt-60 tele therapy machine was commissioned in April 2000, and it is currently one of two megavoltage machines in the northwestern region (the other centre being at the Usman Dan Fodio University Teaching Hospital, in Sokoto State) comprising seven states with an estimated combined population as of 2016 of 48,942,347 [18, 19].
The department is also one of the four institutions for residency training programme in radiation and clinical oncology in the country. The others are Lagos University Teaching Hospital, University College Hospital Ibadan and National Hospital, Abuja.
Typically, new and stable patients present through the new patient clinics on Mondays or Thursdays during which they are seen and given laboratory investigations and imaging studies to do. They are subsequently reviewed by the consultant-in-charge who takes the decision for treatment. Emergencies are seen every day either from the wards or through the accident and emergency unit of the hospital.
Table 1. Current staff strength and distribution in the Radiotherapy & Oncology Department, Ahmadu Bello University Teaching Hospital, Zaria.
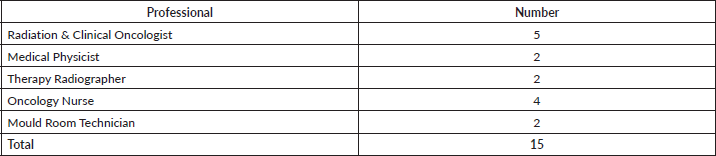
Radiotherapy treatments are done every weekday, Monday to Friday between 8:00 am and 4:00 pm local time. No treatments are carried out in out-of-work-hours, weekends and public holidays. This is essentially due to a lack of adequate staff. Table 1 shows the current staff distribution [20, 21].
Study population
A total of 2.902 patients were referred to the department during the period under review (January 2010–December 2015) with an annual average of 580 patients. We included patients with histologically confirmed cancer, complete medical and treatment records treated with at least one fraction of radiotherapy between 2010 and 2014.
A total of 342 met our inclusion criteria; however, we included only tumour sites with frequency of more than ten (which represent the commonly treated tumour sites in the department) for analysis leading to a total of 258 cases. This is to enable reasonable comparison between tumour sites.
This study did not include patients treated with brachytherapy because it is only offered to patients with cervical cancer.
Emergency treatment is given to any patient presenting with an oncological emergency, defined as any acute, potentially life-threatening event, either directly or indirectly related to a patient’s cancer or its treatment. Examples includes tumour haemorrhage, severe tumour pain and bone metastasis with imminent cord compression.
Design and data collection
This is a retrospective cross-sectional study design. Data on sociodemographic variables and waiting time were collected using a pre-tested structured data collection form. We defined four dates as follows:
1. Date of diagnosis defined as date the pathology report was signed by the pathologist
2. Date of first consultation defined as the date patient was first seen at the radiation oncology clinic. This is when patients are seen and given imaging and laboratory test to do.
3. Date of review/decision-to-treat. This is when patients are reviewed with imaging and laboratory reports and the decision to treat is made during this visit
4. Date of first radiotherapy treatment. This is the date of first treatment.
Four time intervals were considered as shown in Figure 1 (Patients Care Pathway). The time was measured in weeks.
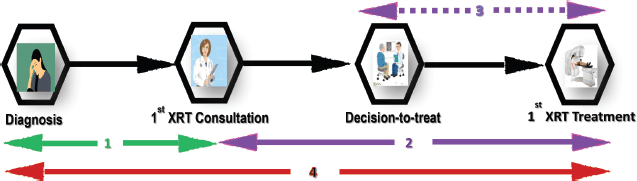
Figure 1. Patient pathway from diagnosis to treatment in the radiotherapy waiting time study 2010–2014.
1. Interval between date of diagnosis to 1st consultation (WT1)
2. Interval between 1st consultation and 1st radiotherapy treatment (WT2)
3. Internal from decision-to-treat to 1st radiotherapy treatment (WT3)
4. Interval from diagnosis to radiotherapy treatment (WT4)
(XRT = Radiotherapy)
Statistical analysis
Data were analysed using SPSS version 25. Descriptive statistics was computed for all the variables. Waiting time was measured as median, interquartile range and the 90th percentile. Because it is a continuous but skewed distribution, we used the Kruskal–Wallis test to compare median waiting time between groups. Alpha value of p ≤ 0.05 is taken as significant.
Ethical consideration
The study was approved by the Ahmadu Bello University Teaching Hospital ethical review committee.
Results
A total of 258 cases were reviewed, mean age was 48 (±12.9) years, males account for 37 (14.3%) while females account for 221 (85.7%). Cervical cancer accounts for 50% of cases followed by breast cancer (27.5%). Other patients’ characteristics are shown in Table 2.
Tables 3 and 4 show a summary of the waiting time measures, including the median, interquartile range based on cancer type, treatment intent, waiting list and stage of disease.
The median time from diagnosis to radiation oncology consultation (WT1) is 6 (IQR 2–30] weeks with 90% of cases being seen within 43 weeks (≈10 months) after diagnosis. There is significant variation in the median time to radiation oncology consultation across cancer sites (p value = 0.000) with cervical cancer being delayed the least with a median time of 4 (IQR 2–8) weeks while prostate cancer was delayed for 44 (IQR 6–56) weeks.
The median time from radiation oncology consultation to radiotherapy (WT2) is 19 (IQR 2–22) weeks which varies significantly across the cancer sites/diagnosis (p value = 0.000). prostate being the least with a median of 1 (IQR 0-8] weeks while nasopharynx was 28 (IQR 15–37) weeks. 90% of cases waited for 91weeks.
Table 2. Characteristics of cases in the radiotherapy waiting time study, Zaria 2010–2014.
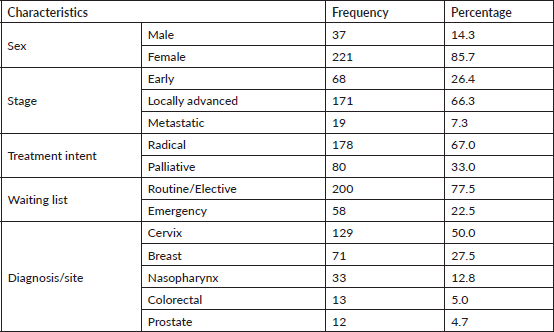
Table 3. Median and interquartile range in weeks in the radiotherapy waiting time study, Zaria.
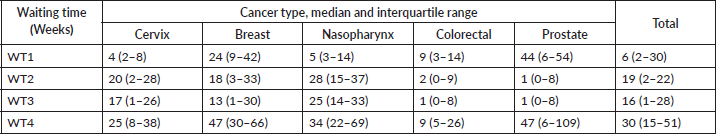
The decision-to-treat to 1st radiotherapy (WT3) is the interval from when patients imaging and laboratory reports are reviewed by the physician-in-charge and the decision for treatment is taken. The median time for all cases is 16 weeks (IQR 1–28). The longest duration is seen in nasopharyngeal carcinomas 25 weeks (IQR 14–33), while prostate cancer has a median time of 1week (IQR 0–7). The variation across the cancer site is statistically significant (p value = 0.000).
The overall time from diagnosis to 1st radiotherapy treatment shows the total time spent waiting for radiotherapy treatment. Median time is 30 weeks (IQR 15–51) – those with breast cancer waited the longest with a median time of 47 weeks (IQR 30–66) and colorectal cancer patients waited the least with a median time of 9 weeks (IQR 5–26).
Table 5 shows the proportions of cases meeting the best-practice-target as recommended in the literature for radical and palliative treatments.
Table 6 shows proportions of delay beyond 3, 6 and 12 months, respectively. Only 27.5% and 43% of cases were treated within the recommended 30 days and 10 days for radical and palliative radiotherapy, respectively.
Table 4. The median and interquartile range in weeks of radiotherapy waiting time across treatment intent, waiting list and stage, Zaria 2010–2014.
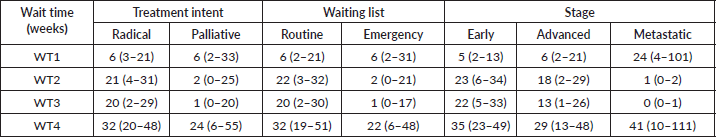
Table 5. Proportion of cases meeting best-practice-target in the radiotherapy waiting time study, Zaria 2010–2014.
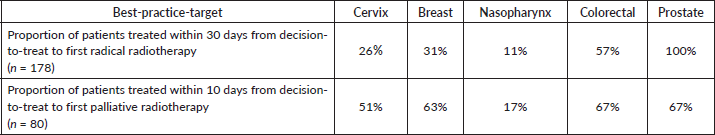
Table 6. Delay in days and proportion (%) of patients seen within 3 months and delay of >3, 6 and 12 months for all cancer diagnoses/site in the radiotherapy waiting time study, Zaria 2010–2014.
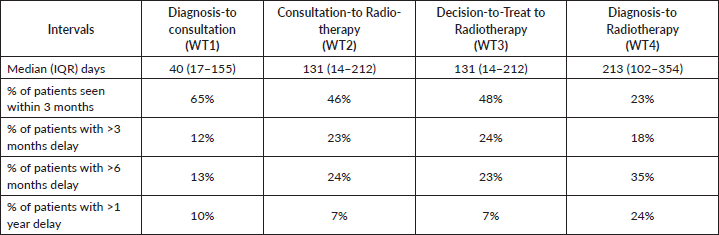
Table 7. Comparisons across the different categories of cases in the radiotherapy waiting time study, Zaria 2010–2014.
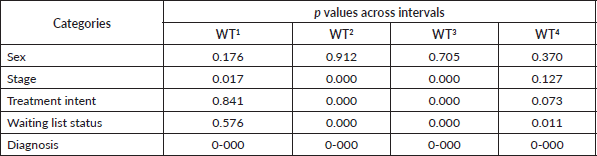
Table 7 shows a comparison of the various waiting time intervals between the different categories of patients. There is no significant difference between males and females across all the different time intervals. However, there are some variations by diagnosis/site, stage, treatment intent and waiting list status
Discussion
The timeliness of cancer treatment is of essence and affects its outcomes as shown by several clinical and experimental studies. This is particularly important in LMICs where access and availability are limited, with 70%–80% of patients presenting with advanced disease and up to 70% require radiotherapy [1, 6, 22, 23].
Our study describes cardinal points of interest in the radiotherapy treatment process; diagnosis, consultation and decision-to-treat and treatment. It also represents different sets of patients, provider and systemic factors that influence delay at each point
In our study, the median interval between diagnosis to first radiation oncology consultation is about 6 weeks. This represents the delay in referral by the clinician who made the diagnosis and is influenced by his/her experience, knowledge of the benefits, indications and sequence of radiotherapy relative to other treatment modalities. The delay in presentation to the radiotherapy by the patient even after diagnosis could be influenced by the factors, such as ignorance, lack of finance and use of complementary and alternative medicines. Furthermore, systemic factors such as lack of clearly defined referral protocols, clinical pathways and non adherence to clinical guidelines which leads to poor care coordination and unnecessary delays. Our findings are similar to a study by Lohlun et al [9] in South African patients with cervical cancer where patients delayed for about 5 weeks from referral to radiation oncology consultation. But it is more than The European Board and College of Obstetrics and Gynaecology recommendation of 2 weeks from referral of suspected or proven gynaecological cancer to consultation [24].
This component of delay has been significantly reduced in other health systems by setting benchmarks and a target time within which referral to a specialist is done. Accelerated and dedicated pathways for referrals are also established to reduce unnecessary delays [25–28].
Although this component of the delay is beyond the control of the radiotherapy facility or the radiation oncologist, it contributes to the overall waiting time and adds to the cumulative negative effect on treatment outcome.
There is also some difference between the different tumour sites with prostate cancer delaying more than cervical cancer. These variations may be due to biological and clinical features of these tumours and the referring clinician’s disposition to it. Cervical cancer causes bleeding with associated foul vaginal discharge. The fear and anxiety associated with blood and the shame and embarrassment of an offensive vaginal discharge not only puts pressure on the clinician to refer quickly, it is also a concern for the patient to present early. Prostate cancer is generally insidious in the onset of symptoms and patients usually commence their treatment with the urologist. They are referred only when there are indications for radiotherapy and this is when disease is castrate-resistant and or metastatic.
The time from first radiation oncology consultation to first radiotherapy treatment (WT2) includes the time spent undergoing these laboratory investigations after initial consultation and decision-to-treat and treatment interval (WT3) which is a subset of the interval between consultation and treatment (WT2) as shown in Figure 1. The interval shows the real waiting time for radiotherapy because it starts when the patients have been fully evaluated and the decision to treat is made and excludes the time spent during evaluation. Although it can be argued that the primary standard of care for cancers like cervix and nasopharyngeal is radiotherapy, especially when diagnosed at an advanced stage and therefore waiting time starts at diagnosis. Both intervals reflect availability of diagnostic and radiotherapy treatment infrastructure and manpower. The current status of radiotherapy facilities in Nigeria is largely due to lack of planning and steady investment, and partly due to huge initial capital investment required for equipment, infrastructure and training. Although Nigeria is the most populous country in Africa, it has only 0.05 megavoltage machines per million people as opposed to 4 per million people as recommended by the IAEA. This is far below Egypt and South Africa where 60% of Africa’s radiotherapy resources are [3, 5, 6, 20, 22, 29–32].
The IAEA recommends 1 radiation oncologist per 250–300 patients. Nigeria has currently less than 100 radiation oncologists and an estimated 100,000 new cases of cancer every year and still has a great deficit of megavoltage machines and radiation oncologists. This will require sustained and incremental investment over the next decade [3, 5, 21, 30–36].
The total median waiting time from diagnosis to treatment (WT4) is significantly long (about 8 months). This period is long enough to cause tumour stage migration (i.e. progression from a lower stage to more advanced stage) which may change the treatment intent from curative to palliation and the waiting list status from routine/elective to emergency. This explains why treatment outcomes in LMICs are poor and made even worse with more than 70% of patients already presenting with locally advanced or metastatic disease.
Our result is lower than 12.2 months reported from University College Hospital in Ibadan Nigeria. This may be due to the small sample size of the study. It is unacceptably long when compared with similar studies in High Income Countries (UK and Nova Scotia in Canada)[25, 30].
Such prolonged waiting times will also cause significant anxiety for both patients and their care givers, loss of productivity and additional health expenses.
Taking a cut-off point of ≥ 3 months as delay from diagnosis to treatment (WT4), our study shows that 77% (Table 6) of our patients experienced delays in receiving radiotherapy and more than half (59%) were delayed for more than 6 months. This is more than 50.4% of patients reported from Botswana with a median time from diagnosis to treatment of approximately 3 months 91 (63–238) days. However, this study included all treatment modalities and the Botswana government covers all or subsidizes some of the costs of cancer treatment which may be responsible for the shorter delay. Delay may be pronounced in countries like Malawi where radiotherapy facilities are not available and patients have to travel abroad for treatment [37–39].
There is no significant difference between males and females across all the different time intervals., (WT1, WT2, WT3 and WT4). However, the interval WT2 and WT3 vary significantly across all cancer sites by stage, treatment intent or by the waiting list status. Advanced and metastatic diseases are less likely to delay because they are likely to be treated with palliative intent or as emergencies. These factors reflect the clinical decision-making process in the choice of treatment in oncology in general but particularly in radiotherapy. Palliative and emergency treatment planning are easier, faster, and given with hypo fractionation while curative/radical treatments require meticulous planning and takes time. This is illustrated by the fact that only about a quarter of radical treatments were done within 30 days and about half of palliative treatments were done within the 10 days as recommended in the literature. The proportion of palliative cases treated is more than radical treatments.
Our study has established that although patients may delay presenting for radiotherapy for reasons such as fear, travel distance and socio-economic factors, greater delay is experienced by those who made it to the radiotherapy facility due to inadequacy of equipment and manpower. It is, therefore, safe to propose that the triad of late stage-at-diagnosis, delay in seeing a specialist after a cancer diagnosis and the delay in starting treatment are the main reasons why the outcomes such as survival are abysmally low in most resource limited settings.
The results of our study have several implications for current and future planning, expansion and investment in radiotherapy services at local and national levels in Nigeria and other LMICs in Africa and beyond.
First: at the local level, delay in receiving radiotherapy is unlikely to improve without expansion and upgrade of the current equipment and increase in number and training of current radiotherapy professionals. This is necessary given the fact that the current equipment is about 20 years since its commissioning in April 2000 and it is time to change it. The staff presently cannot run more than a shift due to inadequacy especially the therapy radiographers and medical physics. Of the five radiation oncologists, three are in the professorial cadre with additional academic and administrative responsibilities. There is a need to increase this number for adequate service delivery. At the national level, there is a need for long-term planning and investment, improvement in procurement processes to include training and maintenance contracts and equitable geographical spread across the country. There is also a need for improved working conditions, remuneration and other incentives for healthcare workers particularly radiotherapy professionals to avoid the brain-drain phenomenon that is rampant across the country and the continent at large.
Secondly: systemic factors such as poor or absence of radiotherapy referral protocols, appropriate use of clinical guidelines and pathways should be integrated into the national cancer control policy to reduce delay in referrals among cancer care service providers. The introduction of functional multi-disciplinary teams into our practice will reduce poor coordination and reduce delays significantly, this has been shown to reduce delay by up to 50% in Botswana [3, 6, 8, 20, 40].
Lastly: radiotherapy is the most cost effective and needed modality of treatment in our current setting where an estimated 70% of all cancer patients will require it as part of their treatment. However, it is expensive for individual patients and their families because of out-of-pocket payments. At present, the national health insurance scheme coverage is less than 5% of the population and does not cover radiotherapy treatments. Including it will reduce financial burden and delays due to lack of finance for those covered by the scheme. For the majority not covered by the scheme, a kind of government subsidy or government bearing the cost of radiotherapy as is practiced in Botswana may be an appropriate strategy [30, 37, 39].
Limitations
This is a retrospective audit of patients records and the quality of data in such a study design is associated with missing and incomplete information. However, we deliberately chose dates and intervals that are routinely documented.
Conclusion
This study shows that radiotherapy waiting time in LMICs like Nigeria is causing a lot of delay in receiving radiotherapy and is longer than international best-practice targets. Urgent steps need to be taken to address the problems of infrastructure, insufficient radiotherapy professionals, poor care coordination and out-of-pocket payments to minimise the delays so that they are as short as reasonably achievable.
Conflicts of interest
All authors declared that they have no conflicts of interest.
Funding
There was no funding support for this study.
References
1. Abdel-Wahab M, Bourque J-M, and Pynda Y, et al (2013) Status of radiotherapy resources in Africa: an International Atomic Energy Agency analysis Lancet Oncol 14(4) e168–e175 https://doi.org/10.1016/S1470-2045(12)70532-6 PMID: 23561748
2. Zubizarreta EH, Fidarova E, and Healy B, et al (2015) Need for radiotherapy in low and middle income countries—the silence crisis continues Clin Oncol (R Coll Radiol) 27(2) 107–114 https://doi.org/10.1016/j.clon.2014.10.006 PMID:25455407
3. Nwankwo KC, Dawotola DA, and Sharma V (2013) Radiotherapy in Nigeria : current status and future challenges West Afr J Radiol 20(2) 84–8 https://doi.org/10.4103/1115-1474.121099
4. Yap ML, Zubizarreta E, and Bray F, et al (2016) Global access to radiotherapy services: have we made progress during the past decade? J Glob Oncol 2(4) 207–215 https://doi.org/10.1200/JGO.2015.001545 PMID: 28717703 PMCID: 5497622
5. International Atomic Energy Agency (2011) Planning National Radiotherapy Services: A Practical Tool Human Health Series No. 14 (Vienna: IAEA) pp 54–67 [Internet] [http://www.iaea.org/Publications/index.html] Date accessed: 1/07/20
6. Ndlovu Ntokozo (2019) Radiotherapy treatment in cancer control and its important role in Africa ecancer 13 942 https://doi.org/10.3332/ecancer.2019.942
7. Bray F, Ferlay J, and Soerjomataram I, et al (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries CA Cancer J Clin 68(6) 394–424 https://doi.org/10.3322/caac.21492 PMID: 30207593
8. Reichenvater H and Matias LDS (2016) Is Africa a “Graveyard” for linear accelerators? Clin Oncol R Coll Radiol G B 28(12) e179–e183 https://doi.org/10.1016/j.clon.2016.08.010
9. Lohlun KN, Kotzen JA, Lakier R (2015) A prospective study on the impact of waiting times for radiotherapy for cervical cancer at Charlotte Maxeke Johannesburg Academic Hospital S Afr J Obstet Gynaecol 21(1) 6–9 https://doi.org/10.7196/sajog.985
10. Shurell E, Olcese C, and Patil S, et al (2018) Delay in radiotherapy is associated with an increased risk of disease recurrence in women with ductal carcinoma in situ Cancer 124(1) 46–54 https://doi.org/10.1002/cncr.30972 PMID: 28960259 PMCID: PMC5734990
11. Wang Y, Wang G, and Wei LH, et al (2011) Neoadjuvant chemotherapy for locally advanced cervical cancer reduces surgical risks and lymph-vascular space involvement Chin J Cancer 30(9) 645–654 https://doi.org/10.5732/cjc.011.10050 PMID: 21880186 PMCID: 4013327
12. Huang J, Barbera L, and Brouwers M, et al (2003) Does delay in starting treatment affect the outcomes of radiotherapy? A systematic review J Clin Oncol 21(3) 555–563 https://doi.org/10.1200/JCO.2003.04.171 PMID: 12560449
13. Mackillop WJ, Bates JH, and O’sullivan B, et al (1996) He effect of delay in treatment on local control by radiotherapy W Int J Radiat Oncol Biol Phys 34(1) 243–250 https://doi.org/10.1016/0360-3016(95)02049-7 PMID: 12118558
14. Mackillop WJ (2007) Killing time: the consequences of delays in radiotherapy Radiother Oncol 84(1) 1–4 https://doi.org/10.1016/j.radonc.2007.05.006 PMID: 17574695
15. Jensen AR, Nellemann HM, and Overgaard J (2007) Tumor progression in waiting time for radiotherapy in head and neck cancer Radiother Oncol 84(1) 5–10 https://doi.org/10.1016/j.radonc.2007.04.001 PMID: 17493700
16. Bultz BD and Carlson LE (2005) Emotional distress: the sixth vital sign in cancer care J Clin Oncol 23(26) 6440–6441 https://doi.org/10.1200/JCO.2005.02.3259 PMID: 16155033
17. Van den Berg B, Gafni A, and Portrait F (2007) Attributing a monetary value to patients’ time: a contingent valuation approach Soc Sci Med 179 182–190 https://doi.org/10.1016/j.socscimed.2017.02.025 PMID: 28288314
18. Dawotola DA and Olasinde TA (2004) Radiotherapy in Cancer Management at Ahmadu Bello University Teaching Hospital (ABUTH), Zaria, Nigeria. Assessment of clinical impact the new radiotherapy facilities Niger Med Pract 45(3) 45–48 https://doi.org/10.4314/nmp.v45i3.28701
19. National Bureau of Statistics National population estimates 2006–2016 [Internet] https://nigerianstat.gov.ng/elibrary Date accessed: 1/07/20
20. Irabor OC, Nwankwo KC, and Adewuyi SA (2016) The stagnation and decay of radiation oncology resources: lessons from Nigeria Int J Radiat Oncol Biol Phys 95(5) 1327–1333 https://doi.org/10.1016/j.ijrobp.2016.04.026 PMID: 27479720
21. Adewuyi S, Ajekigbe A, and Campbell O, et al (2012) Pattern of oncological emergencies seen in adult cancer patients attending the Radiotherapy & Oncology Centre, Ahmadu Bello University Teaching Hospital, Zaria-Nigeria Niger Postgrad Med J 19(4) 208–214 PMID: 23385675
22. Zubizarreta E, Van Dyk J, and Lievens Y (2017) Analysis of global radiotherapy needs and costs by geographic region and income level Clin Oncol 29(2) 84–92 https://doi.org/10.1016/j.clon.2016.11.011 PMID: 27939337
23. Balogun O, Rodin D, and Ngwa W, et al (2017) Challenges and prospects for providing radiation oncology services in Africa Semin Radiat Oncol 27(2) 184–188 https://doi.org/10.1016/j.semradonc.2016.11.011 PMID: 28325246 PMCID: 5653208
24. Bambury I, Fletcher C, and Rattray C, et al (2016) An audit of wait times for service offered by the gynaecology oncology unit at the university hospital in jamaica: are we meeting the standards? J Glob Oncol 2(3) 74s–74s
25. Johnston GM, MacGarvie VL, and Elliott D, et al (2004) Radiotherapy wait times for patients with a diagnosis of invasive cancer, 1992–2000 Clin Investig Med 27(3) 142–156 PMID: 15305806
26. Benk V, Ho V, and Fortin PR, et al (1998) Predictors of delay in starting radiation treatment for patients with early stage breast cancer Int J Radiat Oncol Biol Phys 41(1) 109–115 https://doi.org/10.1016/S0360-3016(98)00046-7 PMID: 9588924
27. Dixon P, Mackillop J, and Henry F, et al (1994) Waiting for radiotherapy in Ontario Int J Radiat Oncol Biol Phys 30(1) 221–228 https://doi.org/10.1016/0360-3016(94)90538-x PMID: 8083117
28. Ash D, Barrett A, and Hinks A, et al (2004) Re-audit of radiotherapy waiting times 2003 Clin Oncol 16(6) 387–394 https://doi.org/10.1016/j.clon.2004.06.006 PMID: 15487130
29. Abdel-Wahab M, Zubizarreta E, and Polo A, et al (2017) Improving quality and access to radiation therapy—an IAEA perspective Semin Radiat Oncol 27(2) 109–117 https://doi.org/10.1016/j.semradonc.2016.11.001 PMID: 28325236
30. Anakwenze CP, Ntekim A, and Trock B, et al (2017) Barriers to radiotherapy access at the University College Hospital in Ibadan, Nigeria Clin Transl Radiat Oncol 5 1–5 https://doi.org/10.1016/j.ctro.2017.05.003 PMID: 29594210 PMCID: PMC5833915
31. Datta NR, Samiei M, and Bodis S (2014) radiation therapy infrastructure and human resources in low- and middle-income countries: present status and projections for 2020 Int J Radiat Oncol 89(3) 448–457 https://doi.org/10.1016/j.ijrobp.2014.03.002 PMID: 24751411
32. Adewuyi SA, Campbell OB, and Ketiku KK, et al (2013) Current status of radiation oncology facilities in Nigeria West Afr J Radiol 20(1) 30–36 https://doi.org/10.4103/1115-1474.117909
33. Rosenblatt E, Barton M, and Mackillop W, et al (2015) Optimal radiotherapy utilisation rate in developing countries: an IAEA study Radiother Oncol 116(1) 35–37 https://doi.org/10.1016/j.radonc.2015.06.012 PMID: 26164776
34. Abdel-Wahab M, Fidarova E, and Polo A (2017) Global access to radiotherapy in low- and middle-income countries Clin Oncol 29(2) 99–104 https://doi.org/10.1016/j.clon.2016.12.004 PMID: 28040092
35. International Atomic Energy Agency (2017) Radiotherapy in Cancer Care: Facing the Global Challenge (Vienna: International Atomic Energy Agency)
36. Manpower and Standards of Care in Radiation Oncology Committee (2000) Definition of RT Waiting Canadian Association of Radiation O oncologist [http://caro-acro.ca/wp-content/uploads/2016/10/Manpower-and-Standards-of-Care-in-Radiation-Oncology-Committee-Definition-of-RT-Waiting-September-2000.pdf Date accessed: 1/07/20
37. Bhatia R, Rayne S, and Rate W, et al (2018) Factors associated with delays in obtaining cancer care in Botswana J Glob Oncol 4 1–13 https://doi.org/10.1200/jgo.18.00088 PMID: 30199305 PMCID: PMC6223504
38. Chadza E, Chirwa E, and Maluwa A, et al (2012) Factors that contribute to delay in seeking cervical cancer diagnosis and treatment among women in Malawi Health (Irvine Calif) 04(11) 1015–1022 http://dx.doi.org/10.4236/health.2012.411155
39. Brown CA, Kohler RE, and John O, et al (2018) Multilevel factors affecting time to cancer diagnosis and care quality in Botswana Oncologist 23(12) 1453–1460 https://doi.org/10.1634/theoncologist.2017-0643 PMID: 30082488 PMCID: 6292540
40. Grover S, Chiyapo SP, and Puri P, et al (2017) Multidisciplinary gynecologic oncology clinic in Botswana: a model for multidisciplinary oncology care in low- and middle-income settings J Glob Oncol 3(5) 666–670 https://doi.org/10.1200/JGO.2016.006353 PMID: 29094103 PMCID: 5646885






