Hypofractionated radiotherapy for localised prostate cancer: the HypoAfrica experience
Azeezat Ajose1, Lensa Seyoum Keno2, Adedayo Joseph1, Solomon Kibudde3, Abba Aji Mallum4, Twalib Ngoma5, Samuel Adeneye1, Awusi Kavuma3, Jumaa Kisukari6, Thokozani Mkhize4, Precious Akowe1, Adewumi Alabi1, Emmanuel Lugina6, Mark Mseti6, Bilinga Tendwa7, Funmilayo Aina-Tolofari1, Ibrahim Elhamamsi1, Stephen Avery8, Katy Graef9, Peter Greer10, Saiful Huq11, Joerg Lehmann10, Heng Li2, Andrej Studen12, William Swanson13, Krishni Wijesooriya14, Luca Incrocci15 and Wil Ngwa2,16
1MedServe-LUTH Cancer Center, Lagos University Teaching Hospital (LUTH), Idi-Araba, Surulere, Lagos 102215, Nigeria
2School of Public Health, Johns Hopkins University, 615 N Wolfe St, Baltimore, MD 21205, USA
3Uganda Cancer Institute, Kampala, Uganda
4University of KwaZulu Natal, Mazisi Kunene Road, Glenwood, Durban 4041, South Africa
5Muhimbili University of Health and Allied Sciences, 9 United Nations Road, Upanga West, Dar es Salaam, Tanzania
6Ocean Road Cancer Institute, Chimara Street, PO Box 65001, Kivukoni, Dar es Salaam, Tanzania
7South Africa Health Product Regulatory Authority, Building A, Loftus Park, 402 Kirkness Street, Arcadia, Pretoria, South Africa
8University of Pennsylvania, 3451 Walnut Street, Philadelphia, PA 19104, USA
9BIO Ventures for Global Health, 2101 Fourth Avenue, Suite 1950, Seattle, WA 98121, USA
10Calvary Mater Newcastle, Edith Street, Waratah, NSW 2298, Australia
11University of Pittsburg Medical Center Hillman Cancer Center, 300 Halket St, Pittsburgh, PA 15213, USA
12University of Ljubljana, Kongresni trg 12, 1000 Ljubljana, Slovenia
13Emory University, 1520 Clifton Rd, Atlanta, GA 30322, USA
14University of Virginia, 1001 Emmet St N, Charlottesville, VA 22903, USA
15Erasmus MC Cancer Institute, Dr. Molewaterplein 40, 3015 GD Rotterdam, The Netherlands
16School of Medicine, Johns Hopkins University, 733 N Broadway, Baltimore, MD 21205, USA
Abstract
Sub-Saharan Africa (SSA) is projected to experience the world’s greatest rise in cancer burden, with prostate cancer incidence and mortality expected to be more than double by 2040. Disparities in disease outcomes are linked to genetic predispositions and limited healthcare resources. Radiotherapy (RT), essential for cancer treatment, remains underutilised in Africa due to infrastructural deficiencies, workforce shortages and limited clinical research. The HypoAfrica consortium was established in 2021 to address these gaps, focusing specifically on hypofractionated radiotherapy (HFRT), a cost-effective treatment modality proven beneficial in European populations but understudied in African populations. This paper presents our experience establishing the HypoAfrica consortium, detailing the challenges encountered, the lessons learned and outlining future directions to improve access to high-quality radiation therapy in SSA. HypoAfrica has confronted substantial challenges, including infrastructural inadequacies, regulatory hurdles, sociocultural barriers, data quality concerns and funding limitations. It implemented strategic solutions such as improved quality assurance (QA) methods, streamlined regulatory engagement, educational outreach, rigorous training programs and innovative financing models. The consortium has significantly enhanced RT capacity and quality across African centers, introducing advanced QA technologies and standardising radiation delivery procedures. These initiatives have fostered professional development and international knowledge exchange through virtual training and global oncology forums. Looking forward, HypoAfrica aims to explore ultra-HFRT to further reduce treatment costs, refine existing HFRT protocols, expand geographically and pursue new collaborations and research avenues, including immunotherapy and implementation science. This work positions HypoAfrica at the forefront of enhancing cancer care accessibility and outcomes across Africa.
Keywords: hypofractionation, radiotherapy, prostate cancer, HypoAfrica
Correspondence to: Katy Graef and Wil Ngwa
Email: kgraef@bvgh.org and wngwa1@jhmi.edu
Published: 30/04/2026
Received: 23/08/2025
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
In 2008, Africa had about 681,000 new cancer cases and 512,000 deaths. By 2030, these are projected to rise to roughly 1.27 million cases and 970,000 deaths due to population growth and aging [1]. Prostate cancer (PCa) is one of the leading causes of cancer morbidity and mortality in men globally [2]. In the GLOBOCAN 2012 reports, PCa incidence and mortality rates in Africa were reported to be 23.2 and 17.0 per 100,000, respectively [3]. Furthermore, PCa is the second most diagnosed and fifth deadliest cancer in men in Sub-Saharan Africa (SSA) [4]. By 2040, incidence and mortality are projected to be more than double, with a 108% increase in incidence and a 112% increase in mortality [4]. Mortality rate in SSA is concerning as it is estimated to be approximately 2.7 times higher than the global average [5]. This disparity is associated with several factors, including genetic and non-genetic factors associated with African ancestry. Individuals of African descent exhibit a higher tumour mutational burden, more genome alterations, increased harmful mutations and specific driver genes such as NCOA2, STK19, DDX11L1, PCAT1 and SETBP1, which significantly increases the risk of presenting with aggressive disease; and the limited availability of healthcare resources such as infrastructure and manpower [5].
Radiation therapy (RT) is an important treatment modality for the cure and palliation of cancer. Most people diagnosed with cancer will require RT at some point in their treatment [6, 7]. In Africa, cancer control is hindered by inadequate access to RT due to limited infrastructure, lack of training programs, skilled workforce shortages and inadequate facilities to meet the increasing need for treatment [6–8]. Similarly, cancer research and care in the Middle East, North Africa and Türkiye region are limited by economic, social and political unrest, with low research output and inadequate cancer registries highlighting the urgent need to strengthen regional capacity [10].
Despite this necessity, there are very few cancer-related trials conducted within Africa and other low- and middle-income regions. Out of 736 documented clinical trials conducted in Africa, only 26 were cancer-related interventional trials, and only six of them were in countries with a predominantly black population [9]. Factors such as cultural considerations, trust issues, concerns about exploiting vulnerable populations and limited human capacity have been suggested as potential contributors to the apparent non-inclusion of African patients in these trials. A recent review revealed that of the total 3,455 global clinical trials for PCa, only 542 were conducted in middle-income countries and none were conducted in low-income countries [11]. Efforts to bridge this research gap in Africa are evident through initiatives like the PCa Transatlantic Consortium (CaPTC), which focuses on understanding the genetic and environmental landscape of PCa in men of African descent [12] and Men of African Descent and Carcinoma of the Prostate [13]. In parallel, the African Consortium for Cancer Clinical Trials (AC3T), which is managed by BIO Ventures for Global Health (BVGH), profiles and promotes the readiness and capabilities of clinical trial sites in Africa with the goal of easing government agencies, academic institutions and industry organisations’ identification and engagement of qualified trial sites. Despite these efforts, clinical trials on RT remain scarce in the region [10, 13].
Hypofractionated radiotherapy (HFRT) improves access by delivering higher radiation doses in fewer sessions, reducing treatment duration. HFRT reduces resource strain for health care systems and improves patient convenience, making it particularly beneficial for regions with limited medical infrastructure [14]. During the COVID-19 pandemic, HFRT was advocated for its potential to improve treatment accessibility, and it has been recommended by the Lancet Oncology Commission to improve radiation treatment access in Africa [14]. However, existing data on HFRT's safety and feasibility are predominantly derived from studies of European descent populations. One example is the conventional or hypofractionated high-dose intensity-modulated radiotherapy for PCa (CHHip) clinical trial. The CHHip Trial was a large, randomised, phase 3 non-inferiority study which enrolled 3,216 men with T1b–T3a disease, who were randomised to one of three regimens: 74 Gy in 37 fractions (conventional, 2 Gy/fraction), 60 Gy in 20 fractions (3 Gy/fraction) or 57 Gy in 19 fractions (3 Gy/fraction), all delivered with intensity-modulated radiotherapy and short-course androgen deprivation therapy. Patient-reported outcomes up to 5 years showed no significant differences in moderate or severe bowel, urinary or sexual symptoms between regimens [15]. Based on these and results from other large-scale randomised trials, moderate hypofractionation is now considered a standard of care for localised PCa [16]. In addition, for low and favourable intermediate-risk PCa, stereotactic body radiotherapy or ultra-hypofractionation, is now accepted as a standard-of-care option, as demonstrated by the PACE-B trial, though longer-term data from broader populations remain desirable [17]. However, evidence supporting the safety and feasibility of HFRT in African populations remains limited. To address this gap, the HypoAfrica consortium was established. This partnership between U.S. and African institutions aims to conduct clinical trials on HFRT for PCa across SSA, focusing on improving treatment efficacy and acceptance in African populations.
HFRT for PCa in Africa (HypoAfrica)
In 2021, BVGH collaborated with the Global Health Catalyst (GHC) and launched the HypoAfrica consortium, which involves several renowned experts from SSA, Europe and the USA. HypoAfrica, inspired by the CHHiP clinical trials findings, was created to conduct a clinical trial aimed at assessing the feasibility and safety of HFRT for localised PCa [15] in SSA.
In the initial stages of the HypoAfrica consortium, the leaders conducted a thorough assessment of radiotherapy centers across Africa that was aimed at evaluating the readiness of these centers for participation in cancer clinical trials. The findings from this comprehensive survey were crucial in shaping the design of the trial and ensuring the ethical approval process was robust, reflecting a commitment to research that is both collaborative and ethically rigorous. The consortium's engagement through regular and ad-hoc meetings at trial sites in Tanzania, Nigeria and South Africa was pivotal in facilitating the exchange of ideas, monitoring the trial's progress and addressing any emergent challenges. This collaborative process is not only focused on evaluating the feasibility of HFRT in SSA but also on identifying and overcoming the obstacles to its wider adoption. By addressing these challenges, HypoAfrica is setting the stage for more expansive clinical trials in the region, aiming to advance the scope of cancer treatment in Africa.
Challenges and recommendations
The team encountered several challenges in implementing HypoAfrica as outlined below:
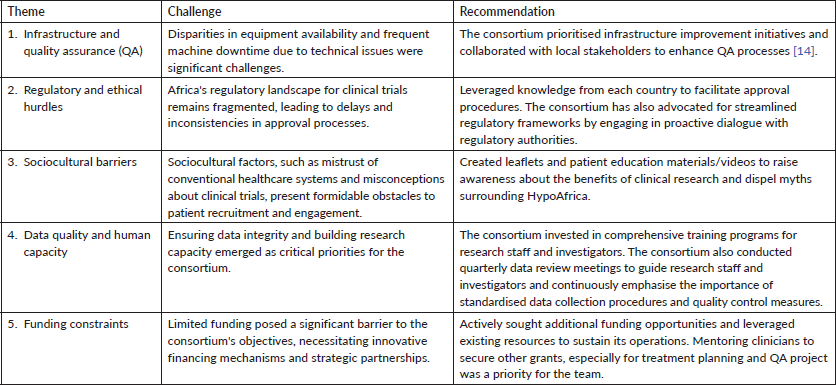
The HypoAfrica consortium's journey offers valuable insights for future RT trials in Africa. Future trials should prioritise localised solutions and engage local stakeholders to address infrastructural, regulatory and sociocultural challenges effectively. In addition, all members of the oncology team, including RT technicians, physicists and oncology nurses, should be included in the research plan to optimise patient outcomes and maximise research impact. Additionally, trials must also embrace principles of diversity, inclusivity and equity, incorporating patient and community perspectives, enhancing access for underserved populations and building local capacity to ensure sustainable improvements in cancer care. Finally, human resource development has been critical to HypoAfrica's success. Future trials should focus on providing continuous support and mentorship to cultivate a skilled workforce capable of conducting high-quality clinical research in African countries. Our consortium leverages local expertise, multidisciplinary collaboration and international partnerships to ensure that the consortium's efforts are not only globally informed but also deeply rooted in local realities, enhancing the relevance and impact.
Impact and future directions
The HypoAfrica consortium has achieved notable progress in advancing RT QA and capacity building throughout the participating sites in Africa. The consortium has improved the precision and efficiency of LINAC QA procedures by introducing innovative QA tools like radiochromic film dosimetry and the Virtual EPID Standard Phantom Audit [18]. For example, at the Ocean Road Cancer Institute, the adoption of radiochromic film dosimetry resulted in significant enhancements in QA uniformity and resource effectiveness, easing staff burdens and ensuring precise radiation dose delivery. Similarly, external audits performed at the NSIA-LUTH Cancer Center have affirmed the quality and reliability of their RT practices [19]. Furthermore, the use of the Klio (Luca Medical Systems), which is an online QA data management tool, has helped promote the uniformity of machine beam outputs across various centers, guaranteeing precise radiation dosage delivery to patients irrespective of their geographic location [20].
Our efforts in education and capacity building, such as weekly virtual meetings utilising web conferencing and specialised training sessions, have provided opportunities for professionals to build capacity in QA protocols and technical competencies. Additionally, the consortium's contributions to publications and presentations at national and international forums, including the GHC Summit, Lancet Oncology Commission on Cancer in SSA launch events in 2022, the American Association of Physicists in Medicine (AAPM) Annual Meeting, American Society for Radiation Oncology Annual Meeting and African Organisation for Research and Training in Cancer Biennial Meeting in 2023, have disseminated valuable insights and best practices, encouraging knowledge sharing and cooperation within the global oncology realm [14, 19–24]. The consortium has successfully attracted funding from the BVGH’s AC3T Study Pool and the AAPM Micro-grant.
In the future, the HypoAfrica project is positioned to pursue transformative avenues to expand its influence and promote cancer care in Africa. We aim to investigate the feasibility of ultra-HFRT to further alleviate the financial burden of treatment for cancer patients in Africa. We also plan to continue to refine HFRT techniques for PCa treatment, integrating cutting-edge technological developments and broadening patient cohorts to amplify treatment results. We will also seek opportunities to extend our scope to additional nations and cultivate partnerships with other research entities. In addition, the HypoAfrica team plans to lead novel initiatives such as the Alliance on Radiotherapy Implementation Science for Equity, which aims to conduct implementation science research on radiation therapy in Africa and research into immunotherapy for cancer patients in Africa.
Conclusion
The HypoAfrica consortium has emerged as a pivotal force in advancing radiotherapy research and capacity building in Africa, marking a significant milestone in the quest to address cancer care disparities on the continent. Through collaborative efforts and strategic initiatives, the consortium has made remarkable progress in enhancing RT QA, fostering knowledge exchange and empowering oncology professionals. Looking ahead, the consortium's blueprint for future trials entails prioritising localised solutions, engaging local stakeholders to address infrastructural, regulatory and sociocultural challenges effectively, and ensuring the inclusion of all members of the oncology team in research plans to optimise patient outcomes.
Conflicts of interest
The author(s) declare that they have no conflicts of interest.
Funding
This study did not receive any external funding.
References
1. Sylla BS and Wild CP (2012) A million Africans a year dying from cancer by 2030: what can cancer research and control offer to the continent? Int J Cancer 130(2) 245–250 https://doi.org/10.1002/ijc.26333
2. Zhang W, Cao G, and Wu F, et al (2023) Global burden of prostate cancer and association with socioeconomic status, 1990-2019: a systematic analysis from the global burden of disease study J Epidemiol Glob Health 13(3) 407–421 https://doi.org/10.1007/s44197-023-00103-6 PMID: 37147513 PMCID: 10469111
3. Adeloye D, David RA, and Aderemi AV, et al (2016) An estimate of the incidence of prostate cancer in Africa: a systematic review and meta-analysis PLoS One 11(4) 153496 https://doi.org/10.1371/journal.pone.0153496
4. Jalloh M, Cassell A, and Niang L, et al (2024) Global viewpoints: updates on prostate cancer in Sub-Saharan Africa BJU Int 133(1) 6–13 https://doi.org/10.1111/bju.16178
5. Jaratlerdsiri W, Jiang J, and Gong T, et al (2022) African-specific molecular taxonomy of prostate cancer Nature 609(7927) 552–559 https://doi.org/10.1038/s41586-022-05154-6 PMID: 36045292 PMCID: 9477733
6. Sarria GR, Torales S, Rossi F, et al (2026) Radiotherapy access in Latin America: socio-economic determinants and equity challenges socio-economic determinants in Latin America for radiotherapy Clin Transl Radiat Oncol 56 101062
7. Mwamba M, Lombe DC, and Msadabwe S, et al (2023) A narrative synthesis of literature on the barriers to timely diagnosis and treatment of cancer in Sub-Saharan Africa Clin Oncol (R Coll Radiol) 35(9) e537–e548 https://doi.org/10.1016/j.clon.2023.05.011 PMID: 37302880
8. Sarria GR, Martinez DA, and Del Castillo R, et al (2022) Radiotherapy and cancer status in Latin America: economic analysis of investment opportunities up to 2030 Lancet Oncol 23(S5) S5 https://doi.org/10.1016/S1470-2045(22)00404-1
9. Ibraheem A, Pillai C, and Okoye I, et al (2021) Cancer clinical trials in Africa-an untapped opportunity: recommendations from AORTIC 2019 Conference Special Interest Group in clinical trials JCO Glob Oncol 7 1358–1363 https://doi.org/10.1200/GO.21.00096 PMID: 34506222 PMCID: 8440011
10. Tolba M, Skelton M, and Abdul Sater Z, et al (2023) Cancer research in vulnerable populations: a call for collaboration and sustainability from MENAT countries JCO Glob Oncol 9 e2300201 https://doi.org/10.1200/GO.23.00201 PMID: 38096463 PMCID: 10730041
11. Halaseh SA, Al-Karadsheh A, Mukherji D, et al (2023) Prostate cancer clinical trials in low- and middle-income countries Ecancermedicalscience 17 1629 https://doi.org/10.3332/ecancer.2023.1629
12. Odedina FT, Ragin C, Martin D, et al (2020) Standardized global behavioral and epidemiological measures for prostate cancer studies in black men Cancer Health Disparities 4
13. Daniel Yilma (2024) Breaking the barriers for conducting clinical trials in Africa: a need for higher commitment and collaborations Ethiop J Health Sci 34(3) 171–172
14. Olatunji E, Swanson W, Patel S, et al (2023) Challenges and opportunities for implementing hypofractionated radiotherapy in Africa: lessons from the HypoAfrica clinical trial Ecancermedicalscience 17 1508 https://doi.org/10.3332/ecancer.2023.1508 PMID: 37113724 PMCID: 10129374
15. Dearnaley D, Syndikus I, and Mossop H, et al (2016) Conventional versus hypofractionated high-dose intensity-modulated radiotherapy for prostate cancer: 5-year outcomes of the randomised, non-inferiority, phase 3 CHHiP trial Lancet Oncol 17(8) 1047–1060 https://doi.org/10.1016/S1470-2045(16)30102-4 PMID: 27339115 PMCID: 4961874
16. Morgan SC, Hoffman K, and Loblaw DA, et al (2018) Hypofractionated radiation therapy for localized prostate cancer: executive summary of an ASTRO, ASCO, and AUA evidence-based guideline Pract Radiat Oncol 8(6) 354–360 https://doi.org/10.1016/j.prro.2018.08.002 PMID: 30322661
17. Brand DH, Tree AC, and Ostler P, et al (2019) Intensity-modulated fractionated radiotherapy versus stereotactic body radiotherapy for prostate cancer (PACE-B): acute toxicity findings from an international, randomised, open-label, phase 3, non-inferiority trial Lancet Oncol 20(11) 1531–1543 https://doi.org/10.1016/S1470-2045(19)30569-8 PMID: 31540791 PMCID: 6838670
18. Zwan BM, Lehmann N, Legge J, et al Remote dosimetric auditing for intensity modulated radiotherapy: a pilot study
19. Kisukari JD LJ, Adeneye SO, Avery SM, et al Commissioning film dosimetry for linac QA in Sub-Saharan Africa - a single institution’s experience
20. SO A. Needs Assessment for Establishing an Imaging and Radiation Oncology Core (IROC) for Africa that Will Support Radiation Oncology and Imaging Clinical Trial Quality Assurance Across the Continent
21. Olatunji EO, Kisukari JD, and Adeneye S, et al (2023) Can advanced radiotherapy clinical trials be conducted in resources limited countries? Int J Radiat Oncol Biol Phys 117(2) e604–e6e5 https://doi.org/10.1016/j.ijrobp.2023.06.1972
22. Olatunji E, Patel S, and Graef K, et al (2023) Utilization of cancer immunotherapy in sub-Saharan Africa Front Oncol 13 1266514 https://doi.org/10.3389/fonc.2023.1266514
23. Mallum A, Barry FA, and Tendwa MB, et al (2024) Cancer research in sub-Saharan Africa: progress in closing the gap Med Res Arch 12(4) https://doi.org/10.18103/mra.v12i4.5080
24. Ajose AO, Graef K, and Mallum AA, et al (2024) Genetic testing in cancer care: an assessment of current practice in Africa J Clin Oncol 42(16_suppl) e13784 https://doi.org/10.1200/JCO.2024.42.16_suppl.e13784
Appendix A : experts involved in the HypoAfrica consortium
Leadership
Prof. Luca Incrocci – Erasmus Medical Center, The Netherlands
Prof. Wil Ngwa – GHC and Johns Hopkins University School of Medicine, USA
Dr. Katy Graef – Bioventures for Global Health
Mentors
Prof. Saiful Huq – University of Pittsburgh, USA
Prof. Heng Li – Harvard Medical School, USA
Prof. Joerg Lehmann – Calvary Mater Newcastle, Australia
Prof. Stephen Avery – University of Pennsylvania, Philadelphia, USA
Africa-based investigators
Prof. Twalib Ngoma – Muhimbili University of Health and Allied Sciences, Tanzania
Dr. Adedayo Joseph – NSIA-LUTH Cancer Center, Lagos University Teaching Hospital, Nigeria
Dr. Abba Mallum – University of KwaZulu-Natal, Durban, South Africa
Dr. Solomon Kibudde – Uganda Cancer Institute, Kampala, Uganda
Team composition
Multidisciplinary team members, including medical physicists, medical dosimetrists, radiation oncologists and data analysts, collaborate to adapt hypofractionated radiotherapy (HFRT) for African clinical settings.
