Background: Leptomeningeal metastasis (LMM) from non-small cell lung cancer (NSCLC) is often an underdiagnosed entity, has a dismal prognosis and has very limited data from low- and middle-income countries.
Methods: A single-centre study, which included 1148 adult patients diagnosed as NSCLC, with Eastern Oncology Cooperative Group performance status 0–2, as identified from data of four prospective randomised controlled trials. Two trials included patients who had epidermal growth factor sensitive mutations (CTRI/2015/08/006113 and CTRI/2016/08/007149) and the other two included squamous cell carcinoma (CTRI/2013/02/003422) and adenocarcinoma patients (CTRI/2014/08/00484). The key objectives were to estimate the incidence, risk factors, time to development and outcomes for LMM.
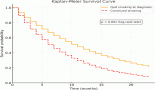
Results: Out of 1148 patients, 36 patients (0.031%; 95%CI: 0.022–0.043) developed leptomeningeal metastasis. In these patients, median time to development of LM was 14.92 months (interquartile range: 7.7–21.84). Among the tested factors, the presence of brain metastasis was the only statistically significant risk factor associated with the development of LMM (p-value = 0.035). The median overall survival (OS) after the development of LM was 61 days (95%CI: 38.95–83.05). The median OS in driver mutated patients was 66 days (95% CI: 14.74–117.26) versus 51 days (95% CI: 14.5–87.5) (p-value = 0.201) in non-driver mutated patients. Only 6 (19.4%) out of 31 epidermal growth factor receptor-mutated patients received osimertinib. Patients treated with osimertinib had a median OS of 245 days (95% CI: 215.48–274.52) versus 52 days (95% CI: 22.62–81.38) for those without (p-value = 0.327).
Conclusion: The incidence of LMM is low in the Indian population. In our study, there was no single factor which impacted survival in patients who developed LMM. This suggests that the overall prognosis is poor in patients with LMM where access to newer therapeutic modalities is limited.