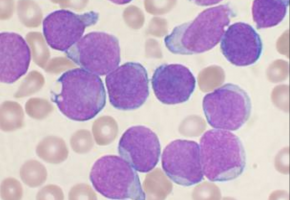
Scientists identify two signalling proteins in cancer cells that make them resistant to chemotherapy, and show that blocking the proteins along with chemotherapy eliminate human leukaemia in mouse models.
Reporting results March 20 in Nature Medicine, researchers at Cincinnati Children's Hospital Medical Center suggest that blocking the signalling proteins c-Fos and Dusp1 as part of combination therapy might cure several types of kinase-driven, treatment-resistant leukaemia and solid tumour cancers.
These include acute myeloid leukaemia (AML) fuelled by the gene FLT3, lung cancers fuelled by genes EGFR and PDGFR, HER2-driven breast cancers, and BCR-ABL-fuelled chronic myeloid leukaemia (CML), according to Mohammad Azam, PhD, lead investigator and a member of the Division of Experimental Haematology and Cancer Biology.
"We think that within the next five years our data will change the way people think about cancer development and targeted therapy," Azam says. "This study identifies a potential Achilles heel of kinase-driven cancers and what we propose is intended to be curative, not just treatment."
The weak spot is a common point of passage in cells (a signalling node) that appears to be required to generate cancer cells in both leukaemia and solid tumours.
The node is formed by the signalling proteins c-Fos and Dusp1, according to study authors.
The researchers identified c-Fos and Dusp1 by conducting global gene expression analysis of mouse leukaemia cells and human chronic myeloid leukaemia (CML) cells donated by patients.
CML is a blood cancer driven by an enzyme called tyrosine kinase, which is formed by the fusion gene BCR-ABL.
This fusion gene is the product of translocated chromosomes involving genes BCR (chromosome 22) and ABL (chromosome 9).
Analysis of human CML cells revealed extremely high levels of c-FOS and DUSP1 in BCR-ABL-positive chemotherapy resistant cells.
Cancer cells often become addicted to the mutated gene that causes them, such as BCR-ABL in kinase-driven chronic myeloid leukaemia.
Most chemotherapies work by blocking molecular pathways affected by the gene to shut down the disease process.
In the case of CML, a chemotherapy called imatinib is used to block tyrosine kinase, which initially stops the disease.
Unfortunately the therapeutic benefit is temporary and the leukaemia comes back.
Azam and colleagues show in their CML models that signalling from tyrosine kinase - and growth factor proteins that support cell expansion (like interleukins IL3, IL6, etc.) - converge to dramatically elevate c-Fos and Dusp1 levels in the cancer cells.
Working together these molecules maintain the survival of cancer stem cells and minimal residual disease.
The dormant cells wait around under the radar screen to rekindle the disease by acquiring additional genetic mutations after initially effective chemotherapy.
Azam says Dusp1 and c-Fos support the survival of cancer stem cells by increasing the toxic threshold needed to kill them.
This means conventional imatinib chemotherapy will not eliminate the residual disease stem cells.
Doctors can't just increase the dose of chemotherapy because it doesn't target the Dusp1 and c-Fos proteins that regulate toxic threshold.
After identifying c-Fos and Dusp1, the authors tested different treatment combinations on mouse models of CML, human CML cells, and mice transplanted with human leukaemia cells.
They also tested treatments on B-cell acute lymphoblastic leukaemia (B-ALL).
The treatment combinations included: 1) solo therapy with just the tyrosine kinase inhibitor, imatinib; 2) solo treatment with just inhibitors of c-Fos and Dusp1; 3) treatment with all three combined - imatinib along with molecular inhibitors of c-Fos and Dusp1.
As suspected, treatment with imatinib alone initially stopped CML progression but the leukaemia relapsed with the continued presence of residual disease cells. Treatment with c-Fos and Dusp1 inhibitors alone significantly slowed CML progression and prolonged survival in a majority of mice but wasn't curative. Treatment for one month with
Treatment for one month with c-Fos/Dusp1 inhibitors and imatinib cured 90 percent of mice with CML, with no signs of residual disease cells.
Azam and his colleagues also point to an interesting finding involving solo treatment with just the deletion of c-Fos and Dusp1. This eliminated expression of the signalling proteins and was sufficient to block B-ALL development, eradicating the disease in mouse models.
The authors stress that because the study was conducted in laboratory mouse models, additional research is needed before the therapeutic strategy can be tested in clinical trials.
They are following up the current study by testing c-Fos and Dusp1as treatment targets for different kinase-fueled cancers, including certain types of lung cancer, breast cancers and acute forms of leukaemia.
We are an independent charity and are not backed by a large company or society. We raise every penny ourselves to improve the standards of cancer care through education. You can help us continue our work to address inequalities in cancer care by making a donation.
Any donation, however small, contributes directly towards the costs of creating and sharing free oncology education.
Together we can get better outcomes for patients by tackling global inequalities in access to the results of cancer research.
Thank you for your support.