Retrospective analysis: checkpoint inhibitor accessibility for thoracic and head and neck cancers and factors influencing it in a tertiary centre in India
Vijay Patil†, George Abraham†, Madala Ravikrishna, Atanu Bhattacharjee, Vanita Noronha, Deevyashali Parekh, Nandini Menon, Jyoti Bajpai and Kumar Prabhash
Department of Medical Oncology, Tata Memorial Center and HBNI, Parel, Mumbai 400012, India
†These authors contributed equally
Abstract
Background: Access to cancer care is an issue in low and low middle-income countries. The problem is worse with respect to access to new therapies like checkpoint inhibitors. Hence, we decided to audit our practice in the head and neck and thoracic medical oncology unit from 2015 to 2019 to study the accessibility of checkpoint inhibitors and factors influencing it.
Methods: All patients who were registered in the head and neck and thoracic medical oncology unit between 2015 and 2019 were included in the study. Patients who received immunotherapy were identified from the prospective database of immunotherapy maintained by the department. We made a list of patients who were eligible for immunotherapy per year and identified how many of them received recommended immunotherapy. The indication for eligibility of immunotherapy was based on published pivotal data and it was applicable from the date of publication of the study online. Descriptive statistics were performed. For nominal and ordinal variable percentage with 95% confidence intervals (95% CI) was provided. Factors impacting the accessibility of immunotherapy were identified.
Findings: A total of 15,674 patients were identified who required immunotherapy; out of them only 444 (2.83%, 95% CI: 2.58–3.1) received it. Among head and neck cancer patients, 4.5% (156 out of 3,435) received immunotherapy versus 2.35% (288 out of 12,239) among thoracic cancer patients (p < 0.001). Among the general category (low socioeconomic), 0.29% (28 out of 9,405 ) versus 6.6% (416 out of 6,269) among the private category (high socioeconomic) received immunotherapy (p < 0.001). While 3.7% (361 out of 9,737) among males versus 1.39% (83 out of 5,937) females received immunotherapy (p < 0.001). There was also a temporal trend seen in the accessibility of immunotherapy (p < 0.001).
Conclusion: The accessibility of immunotherapy is below 3% in India. Patients with head and neck cancers, those registered as private category and male patients had higher access to this therapy. There was also a temporal trend observed suggesting increased accessibility over the years.
Keywords: accessibility, immunotherapy, checkpoint inhibitors, low & middle-income countries
Correspondence to: Kumar Prabhash
Email: kumarprabhashtmh@gmail.com
Published: 03/11/2022
Received: 12/09/2022
Publication costs for this article were supported by ecancer (UK Charity number 1176307).
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Checkpoint inhibitors have revolutionised the treatment of cancer. These drugs have improved life span and quality of life and on most occasions when used alone have had a lower rate of grade 3 or higher adverse events [1–10]. As a result in multiple situations, these have received approvals for use from regulatory authorities across the globe. Like with any new therapy, patients in high-income countries have more access to immunotherapy, whereas in low or low-middle-income countries (LMICs) access is limited to a small minority of patients.
Access to cancer care is an issue in low-income countries and LMICs [11]. This disparity in cancer care is further highlighted when we look at the access to new therapies in LMICs. Multiple new advances were seen in oncology in the last 2 to 3 decades such as robotic surgery, proton therapy and checkpoint inhibitor therapy. Among these checkpoint inhibitors are probably the only ones that have shown an overall survival benefit in multiple settings in randomised clinical trials [12–14]. Hence, having access to these life-saving medications is important. We work at a premier academic tertiary care centre in Mumbai in India. Our centre sees more than 35,000 new cancer patients per year which represents a significant cancer burden of the country. We decided to audit our data from 2015 to 2019 to study the access to checkpoint inhibitors in our setting and the factors that influence it.
Methods
Data collection
Patients receiving immunotherapy were identified from two databases: the immunotherapy database and the pharmacy database. The immunotherapy database is a prospective database of all patients receiving immunotherapy maintained by a subunit under ‘solid tumor’ in the Department of Medical Oncology at the Tata Memorial Center. The pharmacy maintains the pharmacy database at our centre and we identified all patients who had taken checkpoint inhibitors from this database. The data from these two databases were reconciled and from this reconciled database we extracted data of the patients who met the criteria below:
1. Adults aged > or = 18 years
2. Cancer site (one of the below)
a. Head and neck
b. Thorax
3. The time period between January 2015 and December 2019
4. Receiving Nivolumab, Pembrolizumab, Atezolizumab, Durvalumab, Avelumab or Ipilimumab.
Patients who had performance status 3 or greater and those that were unwilling for further treatment were excluded.
This data of immunotherapy recipients were collected as a part of a retrospective analysis approved by the Institutional Ethics Committee. Data regarding gender and patient category were extracted from these patients. Categories were defined as general or private. General and private categories in the institute are chosen by the patient. Patients who are willing to pay for their treatment, have personal insurance or have state-central government employee insurance fall in the private category. The rest were classified as a general category.
Patients eligible for immunotherapy – These patients were identified from individual outpatient department databases where available and from annual reports.
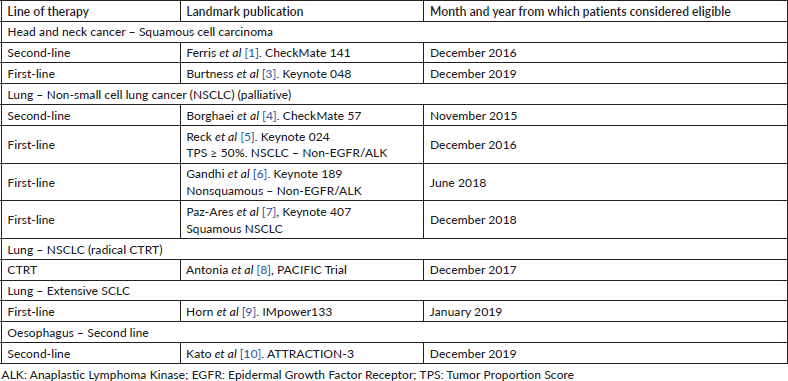
Medical Oncology maintains a meticulous annual report which categorises patients in detail as per the treatment received and by its indication. Thus, for each year, there was detailed data stratifying patients by the line of treatment received, best supportive care, Programmed cell death ligand (PDL) assumption, etc. We used the usage indication for each checkpoint inhibitor as per the respective landmark study (Table 1) and thus patients from our annual review database who met the usage criteria for these checkpoint inhibitors were included as ‘eligible’. These were patients who were offered systemic therapy. These were identified and subjected to the below-mentioned criteria listed.
1. Adult patients ( age > or = 18 years)
2. Cancer disease site (one of the below)
a. Head and neck
b. Thorax
3. The time period between January 2015 and December 2019
4. Patients for particular indications were considered eligible for immunotherapy from 1 month after the first publication of any positive checkpoint inhibitor data in abstract presentations or peer-reviewed journals. The table used for the identification of the patient pool is shown in Table 1.
In addition, the data for gender and category distribution were extracted from the hospital’s annual report.
Statistical analysis
Descriptive statistics were performed. Percentage with its 95% confidence intervals (CI) is provided. Factors impacting access to immunotherapy were sought using the proportion test. A p-value of 0.05 was considered significant.
Results
Accessibility
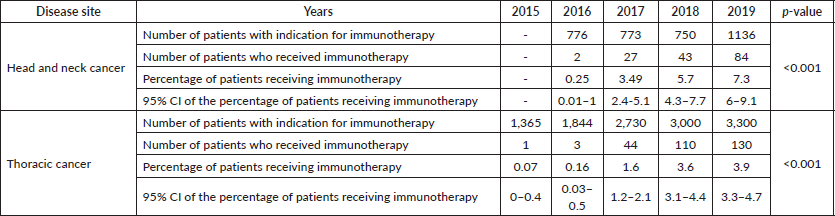
A total of 15,674 patients were identified who required immunotherapy; of which only 444 (2.83%, 95% CI: 2.58–3.10) received it. The distribution of patients eligible as per cancer disease management group and time period is shown in Table 2. A temporal trend was seen suggesting an increase in the accessibility of immunotherapy over the years (p < 0.001, Table 2).
Table 1. Table depicting indication of checkpoint inhibitor applicable during the study period of January 2015 to December 2019.
Factors impacting accessibility
Factors affecting accessibility were the site of the disease, gender and socio-economic status of the patient. The percentage of patients who received immunotherapy was higher in head and neck cancers compared to thoracic cancer patients (4.5% (156 out of 3,435) versus 2.35% (288 out of 12,239) (p < 0.001)). More male patients received immunotherapy as compared to female patients (3.7% (361 out of 9,737) versus 1.39% (83 out of 5,937) (p < 0.001) (Table 3). Among the general category (low socioeconomic), 0.29% (28 out of 9,405) of patients received immunotherapy as compared to 6.6%(416 out of 6,269) of the private category (relatively high socioeconomic) patients (p < 0.001).
Discussion
To the best of the authors’ knowledge, this is the first study evaluating the accessibility of checkpoint inhibitors from LMICs. The study shows a real-life picture of the access to these molecules in a LMIC. Less than 3% of patients at our centre can access checkpoint inhibitors. Hence, there is an urgent need to address the issue of accessibility. This accessibility is variable across broad disease management groups with the maximum still not crossing 5% and this was statistically significant. There was a significant difference in accessibility by gender and category of patient. As explained in the Methods section, private category patients have either higher socio-economic status or have access to insurance. Hence, the accessibility in this cohort was higher. However, in spite of accessibility being higher, it was below 10%. This suggests that even in affording patients or those with insurance, these drugs are largely inaccessible.
All our patients were from outside of clinical trials. We had a few clinical trials on checkpoint inhibitors ongoing at our centre however since the indications were not yet Food and Drug Administration (FDA) approved, the patients under those trials have not been included in this study. We do not have detailed demographic information for patients included in this specific study; however, we have the demographic details of patients that visit our centre for treatment. 50% of patients are from the state of Maharashtra while 50% are from states outside of Maharashtra. 20% of patients are from the city of Mumbai.
The cost of new medications, especially life-saving drugs, is a complex issue. The cost of these drugs is enormous [15–17] and unfortunately, there is a lack of guidelines suggesting fair pricing. The costs are kept similar across the globe and there is limited support for patients from LMICs. These costs which might be affordable for high-income countries are not necessarily affordable by LMIC. Hence, we are of the opinion that having differential pricing across the globe might help in improving accessibility. The presence of patient assistance programmes can further add to this context. The non-availability of these drugs is another issue influencing accessibility. The late introduction of drugs in LMICs is not uncommon. Drugs are either not introduced or introduced late in multiple low-income countries thus impacting their use. For example, Ipilimumab was launched in India after 2019 [18], while the seminal publication of this drug came in 2010 in melanoma [19].
Table 2. Table depicting accessibility of checkpoint inhibitors from 2015 to 2019.
Nivolumab received approval for lung cancer in India in June 2016 and for head and neck cancers in October 2017. Ipilimumab, as mentioned, only began being sold for use in October 2020. Pembrolizumab received approval for lung cancer in July 2018 and for head and neck cancers in September 2021.
In India, multiple government schemes support treatment [20]. Similarly, multiple non-governmental organisations or trusts also support patients’ needs. However, these schemes commonly do not support treatment that comes under the title of ‘palliative’ therapy irrespective of its benefit. For example, surgical treatments like Whipple’s surgery (for pancreatic cancer) [21] or pneumonectomy (locally advanced lung cancer) [22] where most of the patients fail within 1 year are supported as these treatments are labelled as ‘curative’. But, on the contrary, treatments like checkpoint inhibitors or even drugs like osimertinib in Epidermal Growth Factor Receptor (EGFR) mutated lung cancer [23] are not commonly supported. Even though the benefit of these drugs is much beyond the benefit of the above-mentioned procedures. Obviously, the high cost of these drugs prohibits government schemes and makes it challenging. Further, most government schemes are not flexible for the accommodation of patient assistance programmes. A combination of the decrease in drug cost, use of patient assistance programmes in government schemes and distribution of government resources on 2–5 year survival benchmarks might help in improving accessibility to these drugs. Other issues include drugs/pharmaceutical companies reaching LMICs relatively later as well as accessibility challenges with these drugs being available at pharmacies only in tier 1 cities in India, for example, and not in other cities.
Multiple insurances available in India do not support palliative treatment or treatment with targeted or immunotherapy [24] thus limiting the usefulness of such insurances in treating cancer patients. Additionally, this might further limit their accessibility [25]. There is an urgent need for national and international bodies to have a guideline on what treatments need to be reimbursed by insurance.
Table 3. Table depicting factors impacting the accessibility of checkpoint inhibitors.
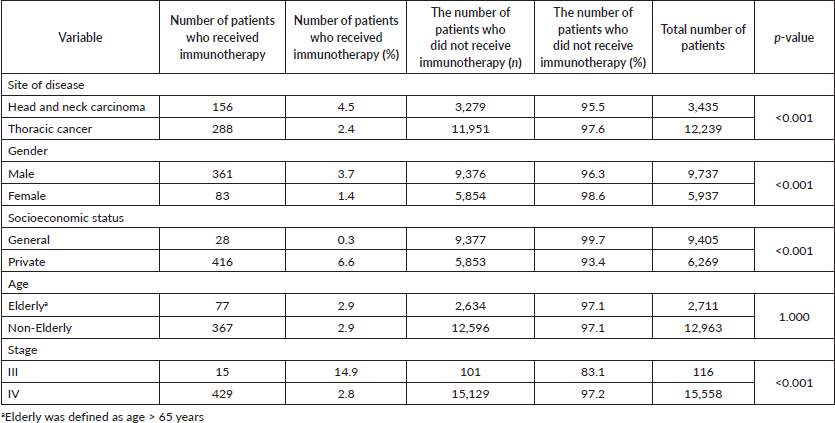
Table 4. Table depicting the site, intent, lines of treatment and drugs used.

aElderly was defined as age > 65 years 
There is a need for positive steps from LMICs for addressing this disparity in the accessibility of high-cost anti-cancer drugs. The development of generic or bio-similar molecules and innovative studies on low-dose regimens or longer duration treatment schedules would help bring down the cost of treatment and improve accessibility in these regions. There are multiple retrospective analyses that suggest that such schedules might be helpful [26–28]. However, there is need for performing dose response, minimum effective dose finding studies and these need to be backed up by phase 2 and phase 3 randomised studies. Our team has completed one such randomised phase 3 study evaluating 20 mg Nivolumab in head and neck squamous cell carcinoma which suggested use of low-dose nivolumab in comparison with chemotherapy does improve outcomes. Our team is running another randomised study (CTRI/2020/02/023441) evaluating the role of altered schedules. If these studies meet their endpoints, then such schedules would help in improving accessibility. These and similar innovative strategies need to be undertaken in LMICs to combat this issue.
The study is not without its limitations. This was a single centre study and the data collection was retrospective. However, our centre is a premier centre in the country and nearly 50% of our patients are from regions outside where the centre is located. The data were limited to head and neck and thoracic malignancies as the investigator team largely works in this domain. Thus, our results on checkpoint inhibitor accessibility are limited to thoracic and head and neck cancers. A large multicentric international study might be able to cover a greater range of sites. Our study also wasn’t designed to evaluate if cost discrimination in different countries could potentially be a solution for low access.
The criteria used for immunotherapy were evolving over the course of the study period. As updates on indications of immunotherapy across lines of treatment came in over the study period, we updated the eligibility of patients for immunotherapy accordingly. The drugs used by site, intent and line of treatment are depicted in Table 4.
Conclusion
The accessibility of immunotherapy is below 3% in India. Patients with head and neck cancers, those registered as private category and male patients had higher access to this therapy. There was also a temporal trend observed suggesting increased accessibility over the years.
Funding
None.
Conflicts of interest
The authors certify that they have no affiliations with or involvement in any organisation or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership or other equity
NSCLC, Non-small cell lung cancer; SCLC, Small cell lung cancer interest; and expert testimony or patent-licensing arrangements) or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Author contribution
Concept: All authors
Design: Dr Kumar Prabhash, Dr Vijay M. Patil
Literature search: All authors
Data acquisition: All authors
Data analysis: Dr Kumar Prabhash, Dr Vijay M. Patil
Statistical analysis: Dr Kumar Prabhash, Dr Vijay M. Patil
Manuscript preparation: All authors
Manuscript editing: All authors
Manuscript review: All authors
Data sharing statement:
Data would be shared post-publication for a period of 5 years for scientific purposes on request, as per the rules and regulations of the Government of India. Data would be available on contacting Dr Kumar Prabhash at kumarprabhashtmh@gmail.com.
Declaration of interest:
Vijay Maruti Patil
Research funding – AstraZeneca (Inst); Eisai Germany (Inst); Intas (Inst); Johnson & Johnson/Janssen (Inst); NATCO Pharma (Inst); Novartis (Inst).
George Abraham
No relationships to disclose.
Madala Ravikrishna
No relationships to disclose.
Atanu Bhattacharjee
No relationships to disclose.
Vanita Noronha
Research funding – Amgen (Inst); AstraZeneca (Inst); Dr. Reddy’s Laboratories (Inst); Intas (Inst); Sanofi/Aventis (Inst).
Travel, accommodations, expenses – American Society of Clinical Oncology.
Deevyashali Parekh
No relationships to disclose.
Nandini Sharrel Menon
No relationships to disclose.
Jyoti Bajpai
No relationships to disclose.
Kumar Prabhash
Research funding – Alkem Laboratories (Inst); BDR Pharmaceutics (Inst); Biocon (Inst); Dr Reddy’s Laboratories (Inst); Fresenius Kabi (Inst); NATCO Pharma (Inst); Roche (Inst).
References
1. Ferris RL, Blumenschein G Jr, and Fayette J, et al (2016) Nivolumab for recurrent squamous-cell carcinoma of the head and neck N Engl J Med 375(19) 1856–1867 https://doi.org/10.1056/NEJMoa1602252 PMID: 27718784 PMCID: 5564292
2. Cohen EE, Harrington KJ, and Le Tourneau C, et al (2017) Pembrolizumab (pembro) vs standard of care (SOC) for recurrent or metastatic head and neck squamous cell carcinoma (R/M HNSCC): phase 3 KEYNOTE-040 trial Ann Oncol 28 v628 https://doi.org/10.1093/annonc/mdx440.040
3. Burtness B, Harrington KJ, and Greil R, et al (2019) Pembrolizumab alone or with chemotherapy versus cetuximab with chemotherapy for recurrent or metastatic squamous cell carcinoma of the head and neck (KEYNOTE-048): a randomised, open-label, phase 3 study Lancet 394(10212) 1915–1928 https://doi.org/10.1016/S0140-6736(19)32591-7 PMID: 31679945
4. Borghaei H, Paz-Ares L, and Horn L, et al (2015) Nivolumab versus docetaxel in advanced nonsquamous non-small-cell lung cancer N Engl J Med 373(17) 1627–1639 https://doi.org/10.1056/NEJMoa1507643 PMID: 26412456 PMCID: 5705936
5. Reck M, Rodríguez-Abreu D, and Robinson AG, et al (2016) Pembrolizumab versus chemotherapy for PD-L1-positive non-small-cell lung cancer N Engl J Med 375(19) 1823–1833 https://doi.org/10.1056/NEJMoa1606774 PMID: 27718847
6. Gandhi L, Rodríguez-Abreu D, and Gadgeel S, et al (2018) Pembrolizumab plus chemotherapy in metastatic non-small-cell lung cancer N Engl J Med 378(22) 2078–2092 https://doi.org/10.1056/NEJMoa1801005 PMID: 29658856
7. Paz-Ares L, Luft A, and Vicente D, et al (2018) Pembrolizumab plus chemotherapy for squamous non-small-cell lung cancer N Engl J Med 379(21) 2040–2051 https://doi.org/10.1056/NEJMoa1810865 PMID: 30280635
8. Antonia SJ, Villegas A, and Daniel D, et al (2018) Overall survival with durvalumab after chemoradiotherapy in stage III NSCLC N Engl J Med 379(24) 2342–2350 https://doi.org/10.1056/NEJMoa1809697 PMID: 30280658
9. Horn L, Mansfield AS, and Szczęsna A, et al (2018) First-line atezolizumab plus chemotherapy in extensive-stage small-cell lung cancer N Engl J Med 379(23) 2220–2229 https://doi.org/10.1056/NEJMoa1809064 PMID: 30280641
10. Kato K, Cho BC, and Takahashi M, et al (2019) Nivolumab versus chemotherapy in patients with advanced oesophageal squamous cell carcinoma refractory or intolerant to previous chemotherapy (ATTRACTION-3): a multicentre, randomised, open-label, phase 3 trial Lancet Oncol 20(11) 1506–1517 https://doi.org/10.1016/S1470-2045(19)30626-6 PMID: 31582355
11. Sirohi B (2014) Cancer care delivery in India at the grassroot level: improve outcomes Indian J Med Paediatr Oncol 35(3) 187–191 https://doi.org/10.4103/0971-5851.142030 PMID: 25336787 PMCID: 4202612
12. Kuroda H, Takahashi Y, and Shirai S, et al (2021) Survival benefit of immune checkpoint inhibitor monotherapy in patients with non-small cell lung cancer recurrence after completely pulmonary resection Ann Transl Med 9(15) 1225 https://doi.org/10.21037/atm-21-1492 PMID: 34532362 PMCID: 8421933
13. Pala L, Sala I, and Oriecuia C, et al (2022) Association of anticancer immune checkpoint inhibitors with patient-reported outcomes assessed in randomized clinical trials: a systematic review and meta-analysis JAMA Netw Open 5(8) e2226252 https://doi.org/10.1001/jamanetworkopen.2022.26252 PMID: 35972744 PMCID: 9382448
14. Rizzo A, Mollica V, and Santoni M, et al (2022) Impact of clinicopathological features on survival in patients treated with first-line immune checkpoint inhibitors plus tyrosine kinase inhibitors for renal cell carcinoma: a meta-analysis of randomized clinical trials Eur Urol Focus 8(2) 514–521 https://doi.org/10.1016/j.euf.2021.03.001
15. Andrews A (2015) Treating with checkpoint inhibitors-figure $1 million per patient Am Health Drug Benefits 8 9 PMID: 26380599 PMCID: 4570079
16. Verma V, Sprave T, and Haque W, et al (2018) A systematic review of the cost and cost-effectiveness studies of immune checkpoint inhibitors J Immunother Cancer 6(1) 128 https://doi.org/10.1186/s40425-018-0442-7 PMID: 30470252 PMCID: 6251215
17. Ding H, Xin W, and Tong Y, et al (2020) Cost effectiveness of immune checkpoint inhibitors for treatment of non-small cell lung cancer: a systematic review PLoS One 15(9) e0238536 https://doi.org/10.1371/journal.pone.0238536 PMID: 32877435 PMCID: 7467260
18. New drugs [Internet] [https://cdsco.gov.in/opencms/opencms/en/Drugs/New-Drugs/] Date accessed: 18/03/22
19. Hodi FS, O’Day SJ, and McDermott DF, et al (2010) Improved survival with ipilimumab in patients with metastatic melanoma N Engl J Med 363(8) 711–723 https://doi.org/10.1056/NEJMoa1003466 PMID: 20525992 PMCID: 3549297
20. Caduff C, Booth CM, and Pramesh CS, et al (2019) India’s new health scheme: what does it mean for cancer care? Lancet Oncol 20(6) 757–758 https://doi.org/10.1016/S1470-2045(19)30322-5 PMID: 31162087
21. Oettle H, Neuhaus P, and Hochhaus A, et al (2013) Adjuvant chemotherapy with gemcitabine and long-term outcomes among patients with resected pancreatic cancer: the CONKO-001 randomized trial JAMA 310(14) 1473–1481 https://doi.org/10.1001/jama.2013.279201 PMID: 24104372
22. Roth JA, Fossella F, and Komaki R, et al (1994) A randomized trial comparing perioperative chemotherapy and surgery with surgery alone in resectable stage IIIA non-small-cell lung cancer J Natl Cancer Inst 86(9) 673–680 https://doi.org/10.1093/jnci/86.9.673 PMID: 8158698
23. Ramalingam SS, Vansteenkiste J, and Planchard D, et al (2020) Overall survival with osimertinib in untreated, EGFR-mutated advanced NSCLC N Engl J Med 382(1) 41–50 https://doi.org/10.1056/NEJMoa1913662
24. Haitsma G, Patel H, and Gurumurthy P, et al (2018) Access to anti-cancer drugs in India: is there a need to revise reimbursement policies? Expert Rev Pharmacoecon Outcomes Res 18(3) 289–296 https://doi.org/10.1080/14737167.2018.1444479 PMID: 29466887
25. Gambhir RS, Malhi R, and Khosla S, et al (2019) Out-patient coverage: private sector insurance in India J Family Med Prim Care 8(3) 788–792 https://doi.org/10.4103/jfmpc.jfmpc_101_19 PMID: 31041202 PMCID: 6482741
26. Patil VM, Noronha V, and Joshi A, et al (2019) Low doses in immunotherapy: are they effective? Cancer Res Stat Treat 2(1) 54 https://doi.org/10.4103/CRST.CRST_29_19
27. Kumar A, Noronha V, and Patil V, et al (2020) 1049P Efficacy and safety of low dose immunotherapy in palliative setting of advanced solid tumours Ann Oncol 31 S718 https://doi.org/10.1016/j.annonc.2020.08.1169
28. Zhao JJ, Kumarakulasinghe NB, and Muthu V, et al (2021) Low-dose nivolumab in renal cell carcinoma: a real-world experience Oncology 99(3) 192–202 https://doi.org/10.1159/000512000 PMID: 33440374






