Solitary thyroid metastasis from colon cancer: a rare case report
L Nicosia1, S Alessi2, M Proh3, E Grosso3, M Ansarin3, A Vingiani4, E Pisa4 and E De Fiori2
1Scuola di Specializzazione in Radiodiagnostica, Università degli Studi di Milano, Milano, Italy
2Divisione di Radiologia, Istituto Europeo di Oncologia, Milano, Italy
3Divisione di Otorinolaringoiatria e Chirurgia Cervico Facciale Istituto Europeo di Oncologia, Milano, Italy
4Divisione di Anatomia Patologica, Istituto Europeo di Oncologia, Milano, Italy
Correspondence to: L Nicosia. Email: lucanicosia88@gmail.com
Abstract
Malignant metastases to the thyroid are rare and are even rarer from a colorectal primary. As these metastases are often asymptomatic, they are usually discovered incidentally on imaging performed as follow-up for the primary tumour. In this report, we present a case of metastatic sigmoid adenocarcinoma to the thyroid diagnosed and treated at our institution.
Keywords: thyroid metastasis, radiological follow-up, ultrasound imaging, fine needle aspiration (FNA)
Copyright: © the authors; licensee ecancermedicalscience. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Published: 24/11/2016; Received: 08/09/2016
Summary
The diagnosis of malignant metastases to the thyroid is rare: it is reported in only 1.4–3% of all patients who undergo surgery for suspected thyroid carcinoma [1, 2]; however, the actual incidence may be higher as they have been reported in 1–24% of cases in autopsy studies of cancer patients [1, 3]. In a review by Fadare et al, it was estimated that less than 100 cases of this phenomenon have been reported over the past century [3].
Kidney, breast, and lung tumours are considered the most frequent sources of metastases to the thyroid [4]. Metastasis from colon cancer is clinically rare, representing about 14% of all metastases to the thyroid [5–8]. Among the cases of thyroid metastases from colorectal cancer reported in the literature in the last five decades, only three cases were described as solitary thyroid metastasis without any other visceral metastases, suggesting that they usually occur in association with metastases to other sites [9].
Metastases to the thyroid rarely produce symptoms [2]. In fact, most of these metastases are detected incidentally during clinical and radiological follow-up in patients with a different primary carcinoma [10, 11].
In this report, we present a case of thyroid metastasis discovered incidentally during the follow-up of a patient with colorectal carcinoma, who had previously undergone surgical resection.
Clinical presentation
A 75-year-old gentleman who had undergone sigmoid colectomy for adenocarcinoma of the sigmoid colon (pT3 N0 G2) in 2009 was being followed up with routine computed tomography (CT) scans.
In 2013, the patient was diagnosed with carcinoma of the prostate and received treatment with radiotherapy in 2014.
Follow-up CT in June 2013 also demonstrated metastatic left pulmonary nodules, and the patient subsequently underwent lobectomy of the left upper lobe of lung. Histological analysis confirmed metastatic adenocarcinoma of the colon (CDX2 ). Between November 2013 and March 2014, the patient received four cycles of chemotherapy with Capecitabine.
Follow-up CT scan in September 2015 revealed the presence of a previously undiagnosed nodule in the thyroid gland. The lesion was investigated with positron emission tomography (PET) and ultrasound (US), before proceeding to fine-needle aspiration (FNA). Cytological analysis of the sample from the FNA led to the diagnosis of thyroid metastasis (TIR5) from adenocarcinoma of the sigmoid colon (CDX2 ).
The patient denied dysphagia, dysphonia and aspiration. Clinically, palpation revealed a nodule in the right thyroid lobe but no enlarged cervical nodes.
Nasoendoscopy revealed normal vocal cord mobility and glottic respiratory space.
Investigations/imaging findings
CT scan of September 2015 revealed a 19 mm subtly hypodense nodule in the right thyroid lobe (Figure 1).
The subsequent PET-CT with FDG of November 2015 demonstrated marked uptake in the right thyroid lobe, thus confirming the suspicion raised by the CT findings (Figure 2).
The patient then underwent investigation by US (6–13 MHz high-resolution linear probe) that confirmed the presence of a taller than wide (19 × 14 mm), solid nodule in the right thyroid lobe. This nodule had an incomplete peripheral hypoechoic halo with iso-, hypo-echogenic internal echotexture and demonstrated absent internal vascularity on Doppler interrogation (Figures 3a and b).
The patient was referred for FNA of the lesion, the cytological results of which were suggestive of intrathyroid metastasis from a colonic primary (TIR 5) (Figure 3c). This diagnosis was suggested by the recognition of columnar cancer cells with dark, large, elongated, palisading nuclei on a background of necrotic debris. Immunohistochemistry was strongly positive for cytocheratin 20, a marker of colon carcinoma (Figures 4a and b).
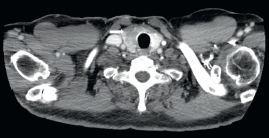
Figure 1. Axial CT scan after injection of contrast agent: 19 mm subtly hypodense nodule in the right thyroid lobe.
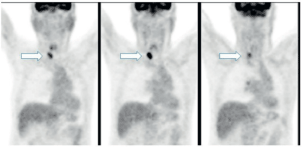
Figure 2. PET-CT: marked uptake in the right lobe of the thyroid gland.
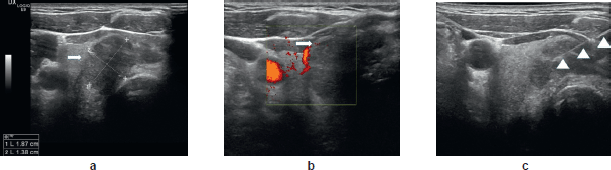
Figure 3. (a) Axial ultrasound image (6–13 MHz probe): a solid nodule measuring 19 × 14mm in the right thyroid lobe characterised by an incomplete peripheral hypoechoic halo and iso-, hypo-echogenic echotexture. (b) Axial ultrasound image with power Doppler: the absence of internal vascularity within the nodule (white arrow). (c) Fine-needle aspiration of the nodule (FNA); the needle (arrowheads) can be seen crossing the target.
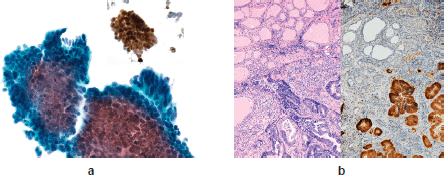
Figures 4. (a and b) Columnar cancer cells with dark, large, elongated, palisading nuclei on a background of necrotic debris. Immunohistochemistry was strongly positive for cytocheratin 20.
Treatment
A multidisciplinary approach to treatment was taken and involved the discussion of the case at a multidisciplinary meeting in which radiologists, head and neck surgeons, general surgeons, radiotherapists, oncologists and endocrinologists participated.
In March 2016, the patient underwent right hemithyroidectomy preserving the parathyroid glands and the recurrent laryngeal nerve. Histology confirmed thyroid metastasis from adenocarcinoma of colonic origin. Immunophenotype of the neoplastic population was positive for CDX-2 and negative for TTF-1 and PSA.
The patient was discharged from the hospital with no indication for radiotherapy or chemotherapy. He is currently undergoing regular clinical and radiological follow-up.
Discussion
Metastasis of malignant tumours to the thyroid gland are uncommon and they have been mainly observed in renal, breast, and lung carcinoma. Cases of metastases from colon rectal cancer, are extremely rare [12, 13]. Typically, metastases to the thyroid are detected as new manifestations of a known primary tumour; however, the primary tumour is sometimes diagnosed following the discovery of metastasis [3].
There are two theories that attempt to explain why metastases to the thyroid are so rare: the first suggests that the rich arterial supply and high vascularity of the thyroid gland prevents tumour cells from remaining fixed in the gland [14, 15]. In the second hypothesis, the high oxygen saturation and high iodine content in the thyroid are credited with preventing the growth of tumour cells from other organs [14, 16].
Thyroid metastases are more frequent in abnormal thyroid glands and are most commonly found concomitantly with goiters or follicular adenomas because of the decreased arterial blood flow, low oxygen level or low iodine content. Hypothyroidism and thyrotoxicosis can occur due to the infiltration of the gland by the malignant mass.
As in our reported case, thyroid metastases can present many years after initial diagnosis, making diagnosis even more difficult [1]. The colorectal metastasis to the thyroid was diagnosed 6 years after surgical resection of the colorectal primary and the patient had no symptoms related to thyroid function. The interval of more than 5 years is long enough to distract the physician’s attention from the previously treated malignant disease. Although a thyroid nodule is an extremely common clinical finding, the new appearance of a thyroid nodule in patients with previous malignant disease warrants prompt cytological evaluation to rule out the possibility of newly developed metastatic disease.
A thyroid nodule arising in a patient with a history of malignancy must be considered to be metastasis until proven otherwise. Fine-needle aspiration (FNA) with cytological evaluation reliably diagnoses primary thyroid neoplasms; this rule also extends to secondary malignancies. Notably, the number of cases with metastatic carcinoma to the thyroid seems to have increased [11]; this increase may be related to a concomitant increase in the number of FNA studies being performed.
Management of thyroid metastases should depend on the individual case. There is no clear consensus; however, some previous studies recommend a thyroid lobectomy and/or isthmectomy in the case of solitary thyroid metastasis and a total thyroidectomy in the case of bilateral metastases. Survival results of thyroidectomy depend on the primary tumour [17, 18].
Radiotherapy and chemotherapy are often reserved as palliative care for patients with widespread disease or in those with comorbidities that preclude surgical intervention [19]. The prognosis varies in relation to the grade of malignancy of the primary lesion; in general, renal cell carcinoma is of low grade malignancy, while lung and gastrointestinal carcinoma are often associated with spread to other organs with unfavourable prognosis [14].
The possibility of tumour metastases to the thyroid gland, although very rare, should be kept in mind when treating patients with a history of cancer elsewhere, especially in the case of a rapidly growing thyroid mass, dysphonia, and cough [20]. As in our case report, the discovery of the thyroid metastasis is often an incidental finding during follow-up imaging.
Conclusion
We presented a rare case of thyroid metastasis from sigmoid carcinoma, a possibility that should be kept in mind whenever thyroid changes, clinical or radiological, are present in a patient with history of carcinoma elsewhere. In any patient with a known history of previous carcinoma, the appearance of a new thyroid mass should be regarded as being potentially metastatic. A thorough investigation for metastases to other organs should also be performed.
References
1. Amenduni T, Carbone A and Bruno R (2014) Precocious and isolated thyroid metastasis of colorectal adenocarcinoma and incidental thyroid papillary microcarcinoma Endocrine 47 969–970 DOI: 10.1007/s12020-014-0258-2 PMID: 24718846
2. Iguchi T, Matsuoka J, and Sato S, et al (2007) F-18 FDG PET demonstration of a thyroid metastasis in a patient with colon cancer Clin Nucl Med 32 361–362 DOI: 10.1097/01.rlu.0000259625.74256.01 PMID: 17452862
3. Fadare O, Parkash V and Fiedler ON et al Tumor-to-tumor metastasis to a thyroid follicular adenoma as the initial presentation of a colonic adenocarcinoma Pathol Int 55 574–579 PMID: 16143033
4. Giuffrida D, Ferraù F and Pappalardo A, et al (2003) Metastasis to the thyroid gland: a case report and review of the literature 560–563
5. Moghaddam PA, Cornejo KM and Khan A (2013) Metastatic carcinoma to the thyroid gland: a single institution 20-year experience and review of the literature Endocr Pathol 24 116–124 DOI: 10.1007/s12022-013-9257-8 PMID: 23872914
6. Cichoń S, Anielski R and Konturek A, et al Metastases to the thyroid gland: Seventeen cases operated on in a single clinical center Langenbeck’s Arch Surg 391 581–587 DOI: 10.1007/s00423-006-0081-1
7. Dequanter D, Lothaire P, and Larsimont D, et al (2004)Andry, métastases intrathyroïdiennes: série de 11 cas, 205–208
8. Atmani A, Valleix D, and Blaise S, et al (2002) Métastases intrathyroïdiennes des cancers du rein: à propos de deux cas Thyroid metastasis from kidney carcinomas: report of two cases 127 532–534
9. Weizer AZ, Raj GV, and O’Connell M, et al (2005) Complications after percutaneous radiofrequency ablation of renal tumors Urology 66 1176–1180 DOI: 10.1016/j.urology.2005.06.125 PMID: 16360436
10. Cohen MS, Arslan N, and Dehdashti F, et al (2001) Risk of malignancy in thyroid incidentalomas identified by fluorodeoxyglucose-positron emission tomography Surgery 130 941–946 DOI: 10.1067/msy.2001.118265 PMID: 11742321
11. Ménégaux F, Chigot JP (2001) Les métastases thyroïdiennes 981–984
12. Nakhjavani MK, Gharib H, and Goellner JR, et al (1997) Metastasis to the thyroid gland: a report of 43 cases Cancer 79 574–578 MID: 9028370
13. Poon D, Toh HC, and Sim CS et al (2004) Two case reports of metastases from colon carcinoma to the thyroid Ann Acad Med Singapore 33 100–102 http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L38478120\nhttp://sfx.library.uu.nl/utrecht?sid=EMBASE&issn=03044602&id=doi:&atitle=Two Case Reports of Metastases from Colon Carcinoma to the Thyroid&stitle=Ann. Acad. Med. Singapor
14. Nakamura K, Nozawa K, and Aoyagi Y, et al (2011) A case report of thyroid gland metastasis associated with lung metastasis from colon cancer Tumori 97 229–232 http://www.embase.com/search/results?subaction=viewrecord&from=export&id=L361839101\nhttp://www.tumorionline.it/allegati/00667_2011_02/fulltext/17-Nakamura(229-232).pdf\nhttp://sfx.ub.rug.nl:9003/sfx_local?sid=EMBASE&issn=03008916&id=doi:&atitle=A case r
15. Wychulis AR (1964) Of August 1964 metastasis of carcinoma to the thyroid gland Surgery 160
16. Willis RA (1931) Metastatic tumours in the thyreoid gland Am J Pathol, 7 187–208 http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2062637&tool=pmcentrez&rendertype=abstract
17. Kim TY, Kim WB, and Gong G, et al (2005) Metastasis to the thyroid diagnosed by fine-needle aspiration biopsy Clin Endocrinol (Oxf) 62 236–241 DOI: 10.1111/j.1365-2265.2005.02206.x
18. Calzolari F, Sartori PV, and Talarico C, et al (2008) Surgical treatment of intrathyroid metastases: preliminary results of a multicentric study Anticancer Res 28 2885–2888 PMID: 19031929
19. Wood K, Vini L, and Harmer C (2004) Metastases to the thyroid gland: the Royal Marsden experience Eur J Surg Oncol 30 583–588 DOI: 10.1016/j.ejso.2004.03.012 PMID: 15256229
20. Chung AY, Tran TB, and Brumund KY et al (2012) Bouvet, metastases to the thyroid: a review of the literature from the last decade Thyroid 22 258–268 DOI: 10.1089/thy.2010.0154 PMID: 22313412






