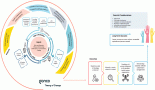
The high burden of non-communicable diseases and communicable diseases in Africa characterised by late presentation and diagnosis makes the need for palliative care a priority from the point of diagnosis to death and through bereavement. Palliative care is an intervention that requires a multidisciplinary team to address the multifaceted needs of the patient and family. Thus, its development takes a broad approach that involves engaging all key stakeholders ranging from policy makers, care providers, educators, the public, patients, and families. The main focus of stakeholder engagement should address some core interventions geared towards improving knowledge and awareness, strengthening skills and attitudes about palliative care. These interventions include educating health and allied healthcare professionals on the palliative care-related problems of patients and best practices for care, explaining palliative care as a clinical and holistic discipline and demonstrating its effectiveness, the need to include palliative care into national policies, strategic plans, training curriculums of healthcare professionals and the engagement of patients, families, and communities.
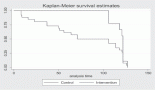
Interventions from a five-year programme that was aimed at strengthening the health system of Namibia through the integration of palliative care for people living with HIV and AIDS and cancer in Namibia are shared. This article illustrates how a country can implement the World Health Organisation’s public health strategy for developing palliative care services, which recommends four pillars: government policy, education, drug availability, and implementation.